Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM here we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Why is it Important that I Can Access My Sister’s Medical Records in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I am here with a live stream today, where I want to answer your questions if you have a loved one in intensive care. And this is one of the most commonly asked questions for families in intensive care and it’s a question that we get all time. And today’s live stream is about the 10 Questions to Ask if Your Loved One is in an Induced Coma in Intensive Care! Live Stream!
10 Questions to Ask if Your Loved One is in an Induced Coma in Intensive Care! Live Stream!
Good afternoon, good evening, wherever you are. It’s Patrik Hutzel here from intensivecarehotline.com with another livestream today, and I want to welcome you to the livestream.
Might just wait for a few more minutes, a few more seconds, until the people come in. Get yourself a cup of tea, a cup of coffee, a glass of water, and also, you should take some notes if you have a loved one in intensive care and write down some things for your own records, because hopefully you will learn something today that you can take back to ICU, that you can take back to your loved one in ICU that will help you in managing this very difficult situation when you have a loved one in intensive care.
So, again, I want to welcome you and thank you again for coming onto the livestream today. If you have any questions, please type them in the chat pad and I will get to them as we go along. If they’re off-topic, but still related to intensive care, I will answer them at the end of this video.
RECOMMENDED:
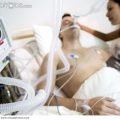
So, in today’s video, I want to talk about the “10 questions you need to ask if you have a loved one in intensive care in an induced coma!” And it’s always a topical issue to talk about. Many patients in intensive care are in an induced coma, especially if they’re on a mechanical ventilator. And one of the main reasons they are in an induced coma is simply to be able to tolerate the induced coma and the breathing tube because it’s very uncomfortable. There are other issues such as for the body to rest so that the body can deal with a critical illness, but obviously there are numerous side effects that are coming from an induced coma as well and I will talk about that in a minute.
So, the other question is, what makes me qualified to talk about this topic today, or what makes me qualified to talk about intensive care or critical care or ICU? Well, I’ve worked in intensive care for over 20 years as a critical care nurse in three different countries. Out of those 20 years, I have worked for over five years as a nurse unit manager in intensive care. For the last eight years, I have been professionally consulting and advocating for families in intensive care all over the world so I’m talking to families on a day-by-day basis all over the world. I’m talking to intensive care units all over the world on a day-by-day basis. I have a team working in the background, working with me that are supporting our clients and their families in achieving the outcomes for our clients. On another note, I also own and operate a service called Intensive Care at Home where we provide intensive care nurses for long-term ventilated and tracheostomy patients at home as a genuine alternative to a long-term intensive care stay. So that’s a little bit about me.
Let’s dive right into today’s topic, so the “10 questions to ask if you have a loved one in an induced coma in intensive care!” So, let’s just start with number one. Why is my loved one in an induced coma? And it’s a question you should be asking and because for intensive care teams, it’s rather obvious or it’s bread and butter for them to put people into induced comas but for you, you should be questioning, why your loved one is in an induced coma?
Again, most of the time they are in an induced coma because they need mechanical ventilation with a breathing tube, I should say, with a breathing tube in the mouth that sits in the throat, and that is incredibly uncomfortable. And due to that discomfort, a patient needs to be induced into a coma so they can tolerate the breathing tube and mechanical ventilation. When you and I breathe in, whilst not being on a ventilator, there is negative pressure in the lungs. If someone is being ventilated and in an induced coma, there’s positive pressure in the lung because the ventilator is doing all the work. That means it’s incredibly uncomfortable. There’s high pressure in the lungs, there’s a tube sitting in your throat. And therefore, an induced coma needs to be started, sedation needs to be started, and opiates, also known as painkillers, need to be started in order to tolerate that.
Other reasons why an induced coma needs to be commenced is often, yes, mechanical ventilation is needed on the one hand, but on the other hand, also a rest period for the body is needed to deal with the critical illness and that sometimes can only be achieved with an induced coma. It should be a last resort, an induced coma and mechanical ventilation, but the reality is that some patients are so sick they need mechanical ventilation, and therefore they need the induced coma.
Next, you do want to ask, what sedatives and opiates are being used? And I’ll break this down. So, number two is, what sedatives are being used? It’s very important for you to know what sedatives are being used. Now, there’s three main sedatives that are being used in intensive care.
Number one is propofol, also known as Diprivan. It’s a white milky substance and it’s quite distinguished when you look at the infusions that are running at your loved one’s bedside, if you see a milky white substance in a small bottle or in a small bag, it’s probably propofol. Propofol is short-acting, which means when you use propofol, patients can be sedated within a few minutes really, seconds. It’s all being used for anesthesia. Main side effect of propofol is hypotension which means patients can go and have a low blood pressure, which might trigger other mechanisms of life support such as inotropes or vasopressors on the other end. And the good news about propofol is that when you stop it, people should wake up pretty quickly, assuming they don’t have any neurological condition.
So that’s propofol, also propofol has been infamously known about being used by the late Michael Jackson, and he used it at home. Now, that’s unbelievable to me, but I just thought I’d throw that in. I believe his doctor has been charged, at least with homicide, which is fair enough because you can only really use propofol for someone that is on a ventilator because people stop breathing and if they stop breathing, they die if they’re not on a ventilator. So, no surprises that the late Michael Jackson didn’t survive a propofol infusion at home. But that’s neither here nor there but I just thought I wanted to throw that in here, more for entertainment purposes than anything. I mean, not that it’s entertaining that Michael Jackson’s passed away, but it’s just unbelievable that Michael Jackson’s doctor prescribed propofol without him being on a ventilator whilst being at home. Unbelievable.
Anyway, next. Other sedatives that are being used, or another mainstream sedative that is being used in intensive care, is midazolam, also known as Versed. Midazolam or Versed is a benzodiazepine and it’s long-acting, meaning it’s often being used for long-term sedation in intensive care. If it’s short-term sedation for a few days, you use propofol often. If you suspect that the induced coma is for a little bit longer, you often use midazolam or Versed. And main side effect of midazolam or Versed, especially when being used for a few more days is, it’s an addictive substance.
A benzodiazepine such as midazolam, other benzodiazepines are lorazepam, Ativan, and temazepam, for example. They can all be addictive in nature. And given that midazolam is being given as an infusion, and I should have said that too, propofol is being given as an infusion too, chances are that once you stop or wean the midazolam, that your loved one goes through a withdrawal process because by now they are addicted to the midazolam or Versed. So, that’s the main side effect of midazolam or Versed. Also, when you stop it, people don’t wake up straight away. If they do wake up, again, they might go through withdrawal, they might be confused, and they might be agitated. All sorts of things.
Suggested Links:
Next, another sedative that is being used more and more in the last 15 years in ICU is Precedex, also known as dexmedetomidine. Precedex, apparently you only need Precedex and you don’t need pain relief on top of that so it can be used as a sedative and as pain relief. I tend not to agree with that. I don’t think that Precedex is working all that well on pain. It definitely has a sedative effect. It works for some patients. From my experience, it doesn’t work for others for whatever reason, but it is a common sedative/opiate being used in intensive care in the last few years.
Another sedative that I have seen being used on and off is clonidine, also known as Catapres. Clonidine is more being used in the later stages of an induced coma, often when people come out of an induced coma. It’s also being used to manage withdrawals. It’s probably less potent than the other sedatives but it still has a sedative effect, and it is being used quite frequently in intensive care still.
Now, number three. When someone is in an induced coma, most of the time they’re getting the sedatives that I just talked about but they’re also getting opiates. Opiates also known as strong painkillers. Opiates being used in intensive care are, generally speaking, morphine, fentanyl, remifentanil, Dilaudid, and oxycodone. They are most of the intravenous opiates that are being used. Again, coming back to mechanical ventilation, whilst having a breathing tube in the throat plus the positive pressure, is very uncomfortable, very painful. You need to be sedated. You need to have the opiates. Again, the main challenge with morphine, fentanyl, Dilaudid, remifentanil, and oxycodone is they are addictive in nature if you use them too long. People are going through a withdrawal process. Similar to the midazolam, it needs to be weaned off gradually.
Also, counterintuitively, all opiates that I just mentioned have respiratory depression as the main side effect. Whereas one of the main side effects, which is, again, counterproductive to weaning someone off the ventilator. It can be a vicious cycle using substances like opiates that have respiratory depression as a side effect and then you’re trying to wean someone off a ventilator and they are respiratory depressed, not a good combination. Therefore, the sooner you can switch off the opiates, the better, and work towards weaning off the ventilator. And finally, extubation, also known as removal of the breathing tube or removal of the endotracheal tube.
Next, number four. How long should your loved one be in an induced coma? Well, what a great question to ask. It really depends. So let me give you some examples. Okay. Let’s just say someone is coming back to ICU after post open-heart surgery. They had bypass grafts, they had a valve repair, valve replacement. Whatever they had, whatever the case may be. Usually, patients should be in an induced coma for a few hours, making sure they’re hemodynamically stable. Making sure they’re not bleeding, making sure they can be weaned off the ventilator, and then they should be out of the induced coma. That’s one example.
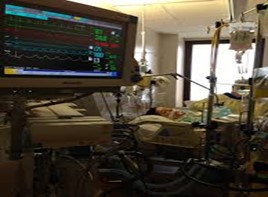
Take another example, someone coming in after, God forbid, after a motor vehicle accident with multiple trauma, they need ventilation. They have rib fractures, they might have a pneumothorax, might have leg fractures, all sorts of things. So, they might wait for surgery and therefore they might need to be in an induced coma for a few days, potentially even be for a few weeks. Now, if they’re predicting that an induced coma might be needed for a few weeks, we would recommend an early tracheostomy, if possible, at all. But there are different scenarios for how long an induced coma needs to be used depending on the critical illness process.
What we’re seeing at the moment obviously, with COVID, patients go into intensive care often with COVID pneumonia, then it might develop into COVID ARDS (acute respiratory distress syndrome). Then they might need to be proned and if they need to be proned, they often also need to be paralyzed, which then, again, prolongs the need for an induced coma. So, it’s not one size fits all, unfortunately, and it very much depends on a case-by-case basis. It very much depends on the need for the induced coma according to a critical illness. And that also brings me back to what should be used? If someone is being paralyzed, they might need midazolam and propofol, and they might need strong doses of morphine or fentanyl. If someone has a significant head injury, again, I have seen propofol and midazolam being used depending on what intracranial pressures are doing, if they’re very high. So, there’s no one size fits all, unfortunately, and it very much depends on a case-by-case basis.
Next, number five. I also mentioned a minute ago, paralysis, and it is almost like a separate issue. So, sometimes you induce people into a coma for mechanical ventilation, for the breathing tube, but sometimes you can give them high doses of propofol, high doses of midazolam, high doses of morphine or fentanyl or any of the other opiates, and they’re still breathing against the ventilator. Sometimes patients are still not synchronizing with the ventilator and then you need to paralyze them. And I’ll explain more about the paralyzing process in a minute.
Also, they might need to be proned, as I just mentioned a minute ago. If they’re getting proned, most of the time they’re getting paralyzed because if someone is being proned on a ventilator with a breathing tube, it’s very, very uncomfortable. So, sedatives might not be enough, and they might still breathe against the ventilator, they might still move. And you can’t really have people breathe against the ventilator or move if they’re being proned, therefore, they do need paralysis. Now, what does that mean? It’s basically muscle relaxants being used as an intravenous infusion or intravenous boluses. They’re also used in anesthetics in the operating room or in theatres to relax people completely while they’re having surgery and it is used in ICU as well. Again, this should be, like an induced coma, it should be an absolute short-term measure and it should be used sparingly. Unfortunately, since COVID, patients went into ICU and needed proning, probably a lot more patients needed paralysis, chemical paralysis, I should say. It’s a chemical restraint, really, if anything.
Recommended:
The other thing that’s important to know is that if your loved one is chemically restrained with muscle relaxants like, there are several out there, vecuronium, rocuronium, cisatracurium, atracurium, there’s a number of them out there. In case you come across those names, they’re most likely muscle relaxants that paralyze the patient.
Now, also, if your loved one does need paralysis, it’s very important that your loved one is being induced into an induced coma first and not the other way around. It’s also being very important that they are on a ventilator. So, picture this, someone is not on a ventilator, someone is not in an induced coma and they’re getting chemically restrained like a paralyzing agent. They would stop breathing, they would stop moving, but their brain would still be working. That would be a terrible predicament to be in. Therefore, sedation first, mechanical ventilation next, or the other way around, and then the paralyzing agent, making sure that your loved one can’t feel that they are paralyzed. The induced coma needs to be first.
Problem with paralysis, similar to an induced coma, is simply the longer someone is in an induced coma and the longer someone is in paralysis, the longer it takes them to wake up, the longer it takes them to build up their strength again, the longer it takes them to start moving again. Things like paralysis and induced coma need to be minimized as much as possible.
Next, number six. I want to talk about synchronization with a ventilator, and I mentioned it briefly before, but I do want to talk about it as a separate issue. So, you need to ask, is your loved one synchronizing with the ventilator? So, what do I mean by that? So, when someone is starting to be ventilated in intensive care, or in the operating room as well, they’re usually being fully ventilated, which means all the work is done by the ventilator. They’re getting a set rate, let’s just say for argument’s sake, 20 breaths per minute, with a set volume 400 mls per breath, with a PEEP (positive end-expiratory pressure), with a pressure support, it’s quite controlled, which is why I said controlled mode. But that can lead to your loved one not synchronizing with the ventilator. It could lead to your loved one fighting against the ventilator.
And let’s just say a loved one has a pneumonia, they need to rest the lungs. They need to let the ventilator do the work and let the ventilator rest the lungs. Give the patient the PEEP, the pressure support, and so forth so the lungs can rest and heal. Together probably with antibiotics, assuming it’s a bacterial pneumonia. And often what you will hear is, “Oh, we tried to wake your loved one up and it didn’t work, he was fighting against the ventilator. He or she was fighting against the ventilator, we had to re-sedate.” And that’s what I mean with synchronization with the ventilator.
It’s quite a common occurrence that when a patient in intensive care should be coming off a ventilator and the ICU team thinks it’s time to try and wean them off the ventilator, the first steps are often not going as planned. You take sedation off, they’re waking up. They often, well, they can’t talk. They don’t know what’s happened. They literally have no idea what’s happened in their environment. They would be scared. They can’t ask questions. Can you imagine how scary this can be? And of course, then they’re fighting against the ventilator. They want the breathing tube out. And they sometimes don’t understand, even though the nurses and doctors are talking to them, and they still can’t make sense of what happened because they literally can’t remember anything. So, you would then re-sedate the patient again and then you need to go through the whole rigmarole again. Try and wake them up, and that’s a bit of an art rather than a science. It often takes a few attempts.
Now, there are some patients that come out of an induced coma straight away, it’s very straightforward, you can extubate them. But a lot of patients, especially the longer the induced coma goes on, can be quite confused, can be agitated, and that often results in them not synchronizing with a ventilator and it’s a bit of back and forth.
Next, I was quickly hinting earlier, number seven, about the proning aspect. So does your loved one need proning while in an induced coma? Well, again, if your loved one does need proning in an induced coma, there’s also a good chance they need very, very high levels of sedation, very high levels of opiates. They’re more likely not needing paralysis as well for your loved one to be able to tolerate the proning. The same can happen if there is a lot of pain prevalent. For example, again, after traumas, after car accidents, motor vehicle accidents, there can be the need for a lot of sedation and there can be a need for paralysis as well, just simply because the pain is so high. But the pain is so much, so great, that high doses of sedation and opiates need to be given and your loved one may still be fighting against the ventilator because they’re in too much pain. So then, higher and higher doses of sedation are needed and then paralysis might be considered as well.
Next, number eight. You might have heard of sedation and opiate boluses. So, what do I mean by that? Let’s just say, for argument’s sake, your loved one is on 10 milligrams an hour of propofol, and one milligram an hour of morphine after, let’s just say, after open-heart surgery for simplicity. And they’re too awake, they still need to be ventilated because they might be unstable, they might be bleeding, they might have ECG (electrocardiogram) rhythm disturbances, their heart may not be beating in a regular rhythm. There could be all sorts of issues going on after open-heart surgery.
And therefore, in order to delay waking up whilst the intensive care team is dealing with maybe bleeding, with instability, hemodynamic instability, and so forth, they need to be given boluses. So, what that means is, rather than increasing the propofol to 15 milligrams an hour and the morphine to 2 milligrams an hour, you might just give them a milligram bolus of morphine, you might just give them a 20-milligram bolus of propofol, and then take it from there. I should also say, instead of saying 10 milligrams an hour of propofol, I should have said a hundred milligrams an hour of propofol. 10 milligrams an hour of propofol is not a lot, it’s just a minimum dose really. So, the minimum dose really, for an adult, would almost be at least a hundred milligrams an hour. But boluses are used quite frequently so not to increase the base rate and just maybe give a bolus here and there to minimize the base rate, but still deal with issues at hand such as agitation or any pain that is going on.
Next, I did hint at that earlier, but I want to talk about it more now, you should be asking, is my loved one addicted to the midazolam, Versed, or to opiates? Now, that is a big issue. We are advocating to use propofol predominantly and minimize the use of opiates such as fentanyl, morphine, Dilaudid, hydromorph, oxycodone, or remifentanil because they’re so addictive in nature. Propofol is not addictive, but especially the midazolam can be very addictive and so can the opiates. So therefore, you don’t need the added-on complexity of going through a withdrawal process when you want to wake your loved one, or when you want to get your loved one out of an induced coma.
Suggested Links:

So, there are challenges around using addictive substances while in an induced coma, because what happens often is when patients eventually come out of an induced coma, they can be confused, they can be agitated, they can be delirious, they can be even half a psychosis, depending on the length of the induced coma. So therefore, you want to minimize the addictive substances as much as you can, to not run into problems when it comes to waking up. There are so many examples that I could give you, and I’m sure other intensive care staff can give you those examples too, where patients are being confused, delirious, agitated, potentially psychotic, when they come out of an induced coma and it’s just another layer of complexity that no one needs. Therefore, you need to minimize the sedatives and opiates right from the start if you can, and there are situations where you can’t, of course. But in the ideal world, if you can, reduce it as much as you can.
Now, so those are my 10 questions that you need to ask. I also want to throw in two other quick points that I think are relevant to the induced coma. So, when someone is coming out of induced coma, or even during an induced coma, it’s critically important to keep doing physical therapy or physiotherapy. Moving of arms, hands, legs, keeping the joints moving because the deconditioning, when someone is in an induced coma, is happening rapidly. It happens within a few days. It’s almost like people have to learn to start walking again after the induced coma because of all the side effects from the sedatives and the opiates. So therefore, early physical therapy is very important and even if it’s only passive range of motion of the limbs, arms, and legs, very, very important to start doing that right from the get-go to diminish the level of deconditioning that is happening.
Now, another quick bonus here is I have made numerous, countless videos about tracheostomy in intensive care. Coming out of an induced coma should definitely not lead to a tracheostomy. But obviously, it can happen that if your loved one can’t come out of the induced coma, if your loved one can’t come off the ventilator, that they may need a tracheostomy down the line. The cutoff usually is 10 to 14 days in an induced coma. And if your loved one can’t come out of the induced coma and they can’t be weaned off a ventilator, a tracheostomy is needing to be considered.
Other inquiries we’re having quite frequently is because, as I mentioned earlier, we’re also providing intensive care at home services. We often have people that come to us and say, “Oh, look, my mom, my dad, my spouse, whatever, is in an induced coma in intensive care. Can we go home with intensive care at home?” Now, depending on where you’re at in your research, Intensive Care at Home is predominantly for long-term intensive care patients. Now that’s not to say you can’t take a patient home in an induced coma with a breathing tube, but it is very risky and so far, we have shied away from it just simply, we are very busy in providing services to long-term intensive care patients with a tracheostomy and a breathing tube, or sometimes with non-invasive ventilation BIPAP (bilevel positive airway pressure) /CPAP (continuous positive airway pressure). But for someone in an induced coma in intensive care, it’s often too early to look at Intensive Care at Home. But nevertheless, if you are interested, go and check out intensivecareathome.com for more information.
So, I am conscious of the time. I usually don’t go for much more than half an hour on these videos, just simply to condense information for you so that you have information available to you at rapid speed and you can run with it and implement very quickly. So, if there are no other questions, I want to wrap this up.
Recommended:
Oh, Mandy has a question. Mandy says, “My 76-year-old dad is in ICU with COVID pneumonia. They started him on propofol and on morphine. They think he will be in an induced coma for a while. Should they be changing his sedation?” That is a great question, Mandy. To answer that one, look, if your dad is needing an induced coma, which he may, well for over a week, I would say, switch him from propofol to small doses of midazolam. It might just be a smoother ride. There are less side effects on a hemodynamic level, especially if he’s getting proned, you didn’t mention that. But if he’s getting proned, for example, the better choice might be to use midazolam and not to use the propofol because, again, propofol, main side effect is hypotension or low blood pressure. Therefore, your dad might need some inotropes on the other end. So yes, potentially, if prolonged induced coma, the intensive care team may want to look at midazolam rather than propofol and keep going with the morphine. I hope that helps, Mandy.
So, if there are no other questions, I want to thank you for watching this video. I want to thank you for all your support. I also want to thank you for coming onto the video, to the livestream, and thank you for your questions.
Now, if you have a loved one in intensive care, go to intensivecarehotline.com. Check out our case studies and call us on one of the numbers on the top of our website for help.
RECOMMENDED:
Now, if you like this video, give it a thumbs up, click the notification bell, subscribe to my YouTube channel for regular updates and also regular livestreams for families in intensive care, and comment below what questions and insights that you have from this video.
I want to thank you once again for coming onto this call and I will talk to you next week.
I will do another livestream next Saturday evening in the U.S., Sunday morning here in Australia, and it is unfortunately in the middle of the night in the U.K., but it’ll be around 7:00 PM Eastern Standard Time next Saturday.
Take care for now and thanks once again.
This is Patrik Hutzel from intensivecarehotline.com and I will talk to you in a few days.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!