Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How to Avoid Reintubation after Extubation! Quick Tip for Families in Intensive Care!
You can check out last week’s question by clicking on the link here.
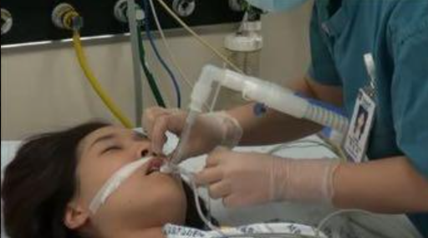
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Nestor, as part of my 1:1 consulting and advocacy. Nestor’s wife is intubated in ICU and he is asking why the doctors won’t try to wean his wife off the ventilator first before they do tracheostomy.
Why Won’t They Try Weaning My Wife Off the Ventilator Before They Do Tracheostomy?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Nestor here.”
Nestor: Hi Patrik!
Patrik: Hi Nestor! How are you and your wife?
Nestor: All right. Things have changed since then. I mean as far as the MRIs results though, I guess my most pressing issue now is, they’ve come back around, and they want me to do the trach and they’re pushing LTAC (long-term acute care) and the PEG (percutaneous endoscopic gastrostomy) and the trach at the same time. I told them no. They’re saying that LTAC is the best place for her and basically they said, “If you don’t go to LTAC, then you don’t really have a whole lot of options. You need to go to a nursing home or home.”
Patrik: Yeah. So I think there is a way forward Nestor. So, it sounds to me like the tracheostomy might be inevitable.
Nestor: Right.
Patrik: However, I think I might have mentioned that on one of our last calls, you can consent to a trach, but don’t consent to a PEG.
Nestor: Right.
Patrik: Why is that? I have not seen LTACs that take patients without a PEG. The LTACs have to have both. They have to have patients with PEG and trach. If you don’t consent to a PEG, they can’t send her out and that will buy you time.
Right. Now, be prepared. They’ll probably jump up and down and say, “Oh you must have a PEG” and blah, blah, blah. From my experience Nestor, I’ve seen patients with nasogastric tubes for up to six months.
RECOMMENDED:
Nestor: Right. That’s what I asked them. They gave me the whole spiel about, “Well, she can get infections and everything.” I’m like, “You can get infections with anything.”
Patrik: Absolutely. And bear in mind, A PEG tube is a small operation. A nasogastric tube is not an operation. You put it in, you insert it into the nose. A nurse can do it. I’ve inserted many nasogastric tubes over the years. It’s not a surgical procedure. So, don’t be pressured by them.
You will see over time that when you stand your ground, they will give in. You will see that over time. They’re doing what they’re doing with everybody else, putting pressure on them and assuming that eventually they will give in. So you just at the beginning of them getting to know you, that you’re not giving in.
Nestor: Mm-hmm. Right. The doctor came and the first day she asked me, because I told them, I said, “Well, let’s just discuss the trach,” I said. She said, “When would you like to do it?” Because I asked her about weaning her off of the ventilator, and she said, “Well she’s not going to be strong enough to breathe without the ventilator.” Be now, she’s saying she’s trying to out-breathe the ventilator. And I said, “Well, okay.” I said, “Give me a couple of days. Let me discuss it with my team and then I will have this decision. They’ll give advice on what I need to do.”
Then the second doctor asked me, “Who are you working with?”
Nestor: “Who are you working with? Who are you getting advice from?” I’m like, “That’s not really important. What’s important is the discussion that we’re having right now.” So, I thought that was interesting.
Patrik: Yes. They would be curious to find that out. Look, just remind me, how many days has your wife now been in ICU for?
Nestor: 11 days.
Patrik: In total?
Nestor: Yeah.
Patrik: Okay. So there is one advantage with a trach. The advantage with the trach is, they should be able to take her off the ventilator. Sorry. They should be able to take her off sedation quickly. She’s still on sedation?
Nestor: Well, they’ve taken off, but when she tries to out-breathe the ventilator, they sedate her a little bit.
Patrik: Right. I see. I see. But I’m just looking through your emails. It says propofol has been discontinued.
Nestor: Right. But I looked last night, and I think they gave her a little bit of it.
Patrik: Right, right.
Nestor: So, they’ll stop and then they’ll start back.
Patrik: They’ll start again.
Nestor: Because like she’s coughing, but they said that’s a reflex. They were doing suctioning and her legs turned inward and they said that’s kind of like a neuro reflex as well.
Patrik: Yes. Well, it’s a good sign that she’s coughing. But here are the advantages of a trach. So, you’re saying she’s breathing against the ventilator or over the ventilator?
Nestor: Mm-hmm.
Suggested Links:
Patrik: Some of that, it’s not guaranteed, but some of that could be simply she is feeling uncomfortable with the breathing tube in the mouth. It’s very uncomfortable. Whereas the trach, generally speaking, is so much easier to tolerate. Have you seen a trach?
Nestor: Oh, yes. I’ve seen a trach.
Patrik: So, one of the main reasons you put someone in an induced coma, it’s not the only reason, but one of the main reasons you put someone in an induced coma when they end up with a breathing tube is simply the discomfort of the breathing tube. So, when someone has a trach, that discomfort is almost going away. So that is the main advantage.
However, here is another thing. It’s day 11 now. One of the concerns is that I’m pretty sure I mentioned that to you in the beginning, day 10 to day 14 of ventilation with a breathing tube and you can’t come off the ventilator, one needs to consider a trach, which is where we’re at now. So, I can understand why they’re considering it. I totally get that.
The question is still to me, before you do a trach, my question is, have they done everything beyond the shadow of a doubt to try and avoid the trach and get her off the ventilator?
Nestor: Did you look at the settings of the ventilator, the pictures that I sent you the other day?
Patrik: Yeah.
Nestor: I asked them if they would try weaning her off the ventilator before just doing a check. And she says, “We could try that, but she probably won’t be able to breathe by herself.” Basically, she was just saying they won’t try to do anything. They want to go straight to the trach.
Patrik: I get that. You know why they want to go straight to the trach? They want to go straight to the trach because then in their mind, they can send your wife to LTAC.
Now, it’s almost like an art taking someone off a ventilator. It takes experience, it takes practice, it takes not giving up just, because it doesn’t work for the first time. So, picture this. Let’s just run through the best-case scenario and let’s just run through the worst-case scenario so you can understand where I’m coming from.
So, best case scenario would be, okay, they can take your wife off the ventilator, take the breathing tube out, and then in a few days they should be able to send her to a hospital ward, hospital floor and off she goes. That would be the best-case scenario. That might also take a little bit of time, or it may never happen because of the hypoxic brain injury. She may never be awake enough to have the breathing tube removed, i.e. which would push her to a trach, okay?
Nestor: Mm-hmm.
Patrik: Worst case scenario is, she’s not waking up. She can’t come off the ventilator. She needs the trach. By you then avoiding the PEG, they have to keep her. She won’t be going to an LTAC.
Now, an LTAC, some LTACs… Or no, let’s put it the other way. The “LTACs are working to wean long-term ventilated patients off the ventilator.” That’s sort of the umbrella that the LTACs are coming under. My experience is that they’re very poor at weaning patients off the ventilator. There is the odd LTAC that’s pretty good. Don’t get me wrong, but they are far and few in between. Patients going from a sort of bad situation in ICU to a worse situation in LTAC, at the moment in ICU, she would have one nurse to two patients at the most, sometimes probably even one to one. In LTAC, that will go down to 1 to 4, potentially 1 to 5, maybe 1 to 8, or even 1 to 10 overnight, right? So, you get the picture?
Nestor: Mm-hmm.
Patrik: In ICU, you have ventilator-competent staff, like nurses, doctors, respiratory therapists. If she goes to LTAC, and I hate to say it, the staff there are barely ventilator competent. That’s what they’re not telling you. What they’re telling you is framed in a way to discharge your wife to LTAC. Here is another sort of pitfall that we are seeing over and over again.
Let’s just say you would consent to trach and PEG, okay? Your wife is still very vulnerable. If she was to deteriorate in LTAC, let’s just say you consent to all of that, she’s going to LTAC, if she was to deteriorate there, God forbid, she would need to go back into ICU pretty quickly. Now, if that was to happen, there’s no guarantee that your wife will go back to the very same ICU she came from, because they may not have a bed. You may choose her to go to an LTAC that’s in a different location. The next ICU might be closer to the LTAC. So we’ve seen situations where someone goes from ICU to LTAC and within 72 hours they’re back in another ICU, basically, going to three different places within 72 hours. That’s madness.
So, I’m not trying to be negative here. A discharge to LTAC needs to be very carefully thought through. Now for them, it’s a one-size-fits-all. For them, it’s like, “Oh, well someone has a trach, PEG, let’s send them to LTAC” Out of sight, out of mind.
Nestor: Right. Then I think now they’re trying like the scare tactics, because she was like, “Well… ” I said, “So what is the other options. If I don’t do the PEG and she doesn’t go to LTAC, what’s the other options?” And she said, “The nursing home.” And I’m like, “What?”
Patrik: No. No. I would argue they are misleading you there. So for now, all you need to do is, you need to buy time. I don’t mean buying time financially. All you need to do is stand your ground, possibly give her a trach, not a PEG. You can always consent to the PEG down the line. There’s no hurry. There’s no rush.
Nestor: And that’s what I told her.
Recommended:
Patrik: Right. Good. Look, they will try and bully you. Don’t let them. Just by you not consenting to a PEG will probably buy you all the time you need.
Other question, have they mentioned something about that if she stays in ICU for too long, that the insurance won’t pay? Have they mentioned anything like that?
Nestor: No, they haven’t mentioned insurance.
Patrik: Right. Okay.
Patrik: Then we can ignore that. That’s good.
If she goes to LTAC, you’ll be very disappointed. If she stays in ICU, you’ll also be disappointed because they won’t be putting their best foot forward either, because in their mind she should go to LTAC. It’s almost like it’s a no-win situation. By the same token, if she goes to LTAC, it’s going from an undesirable situation to a less desirable situation. Have you looked at LTACs?
Nestor: I haven’t. I basically trusted what you told me.
Patrik: Right. Yeah. Look, have they made any suggestions? Have they told you, “Yeah, she should go?”
Nestor: No.
Patrik: No? Okay.
Nestor:And that’s the thing. They basically, it’s almost scripted. It’s almost like you knew what they were going to do and they did exactly what you said. They push and they’ll take, they’ll have this doctor come and do the same thing, another doctor… It’s like they’re trying to say, “We need to do the PEG. We need to do the trach and we need to send her to LTAC.” And I just told them, “I’m not doing both. I’m not doing the PEG and the trach.” “We can do the trach.”
Then the doctor that told me that… I said, “What are other options besides going to LTAC?” And then she said nursing home or at-home care. I asked her has she ever been to an LTAC facility to see how they operate? And she said, “No.” I said, “Basically, we’re done here. Because you been telling me to send my wife somewhere where you’ve never been and your job is to tell me to go there, but you’ve never been there to see how it operates and you’re a doctor of a palliative care.
Patrik: Yeah. Oh, look, the LTACs are set up to save money, not for clinical need. It’s terrible. But the good news is this, if there is something good here, you still have time. You’ve sought help in the early stages. A lot of people come to us once their loved ones are in LTAC, and then they realize that’s a dead end.
Nestor: Yeah, I saw that.
Patrik: You’re still in a position where you have a degree of control, and they don’t like it.
Nestor: Right. I saw that video, the one you said someone called and they let their loved one get the trach and the PEG and now they wanted something else. And you were like, “Well, you shouldn’t let them do the PEG.”
Patrik: That’s right. Another thing is, as I said, most ICUs that I worked at, we had patients in there for six months weaning them off the ventilator and they had a nasogastric tube. There was no PEG needed. A PEG should be done for someone where you know beyond the shadow of a doubt, they’re not coming off a ventilator. They will need nutrition for the rest of their life. They can’t eat. Your wife is not dead. It’s day 11 today.
Nestor: That’s exactly what the palliative care doctor said. She was like, “She’s probably going to be like this for the rest of her life. She needs the nutrition and she’s not able to breathe on her own.
Patrik: Yeah. What I don’t like about the PEGs is, it has a permanency to it. Day 11 is not permanency. If it was month 11, then it’s a different story. It’s day 11. They are already riding off your wife. That’s terrible.
Nestor: Yeah. They were doing it day four though. That’s how awkward it is. And I told the doctor. I said, “Day four, you were trying to get me to unplug them and because you said she was going to be like this, vegetative state for the rest of her life, but you all knew y’all had her on sedatives and paralyzed.” Basically, she was in a coma, but she was in a medically induced coma primarily, because you gave her propofol, fentanyl, and a paralytic.” I said, “You played on my sympathy.”
And I just told her I had no respect for that. The team is great. I said, “But it comes to me day four and day six. And you know a lot of these are the sedatives. You know that probably the withdrawal from fentanyl and propofol is waking up the body and they want me to focus on the fact that, ‘Look, she had brain injury and she’s probably not going to wake up.’
I said, “But she blinked, she coughed, and her pupils were still reacting to light and her eyes, although they don’t focus on you, if you say something, her eyes open and they follow. They go to the side that you’re standing on.” And I said, “Those are signs to me that the brain is not completely dead, that there’s still some reaction there.”
Patrik: I’m glad you mentioned it, that she’s coughing. When people are brain- dead, they’re no longer coughing, so she’s not brain dead.
Nestor: The coughing is voluntary.
Patrik: No. It’s a reflex.
Nestor: Oh, okay.
RECOMMENDED:
Patrik: Surely, we can all voluntarily cough, but especially in this situation, if she coughs, it’s most likely the reflex, but again that’s a good sign. Are you familiar with the Glasgow Coma Scale?
Nestor: I don’t see a rating on the board that they have in the room, but can you tell me about it?
Patrik: Can you access a computer at the moment?
Nestor: Yeah, I have mine with me.
Patrik: Okay. I will send you a Glasgow coma scale now because it’s so much easier if I can talk you through it over the phone. Just give me one second and I will send it to you. Just give me a tick.
Nestor: Because I like her to be awake enough to where she can get to like a brain rehab facility.
Patrik: That’s probably what she will need.
Nestor: Yeah. We have a neuro rehab here nearby, but they won’t take her unless she’s alert, and able to follow commands. But I know I told them I looked that there was brain hospital somewhere in another place.
Patrik: Right. I’ve just sent you an email now with the headline GCS. It’s coming now. Let me know once you’ve got it. Then I’ve attached a picture there. Let’s look at the picture together because it’s important.
Nestor: Okay.
Patrik: You got it?
Nestor: Glasgow Coma Scale. It’s loading.
Patrik: Yep.
Nestor: Okay, I got it. Okay, I see. Okay. It came up.
Patrik: Right. So let’s just go through them one by one once you’ve got it open.
Nestor: Okay. I’m ready.
Patrik: Can you see eye-opening response?
Nestor: Yes.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!