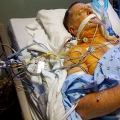
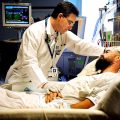
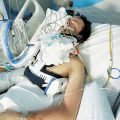
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Far Is My Sister from Coming off the Ventilator?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Joyce, as part of my 1:1 consulting and advocacy service! Joyce’s sister is still on a ventilator and now with a chest tube. Joyce asks where do they start from weaning her sister off the ventilator.
Where Do We Start from Weaning Our Sister Off the Ventilator?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Joyce here.”
Joyce: Okay.
Patrik: You really need to listen to that. There’s a gentleman who was, he must’ve been 60 or 62 at that time when he ended up on a ventilator in 2013. It’s a long time ago. Ended up on a ventilator for a year, for a year. He came over eventually. He’s now in his mid-80s. He’s living life.
Joyce: So, you think my sister can get off the ventilator? We have hope, right? We were better than we were a couple of months ago.
Patrik: You see, right now, you remember. I do remember, it was our second Zoom, I did say to you, I know I can help you but I don’t have a quick fix. And I still don’t have a quick fix. Yes, I believe your sister can come off that ventilator. I believe that. But it’ll take time. It won’t happen if she can’t mobilized.
Joyce: Okay. Right now, I think the biggest thing is get the range of motion. That, I can do.
Patrik: Yes, yes.
Joyce: Get the range of motion going. I want the range of motion going and she’s still on pressure support, then I will add, “Hey, prop her up all the way in the bed.” No one’s really going to pick her up and take her right? But they can move the bed up. They could sit her up all the way up, right?
RECOMMENDED:
Patrik: Yup, starting point. Absolutely. It’s a starting point.
Joyce: I think it’s a bed.. Then, meanwhile now that you’re telling me this is negligence, I will get the record because I thought this was just part of the thing.
Patrik: Look, a pressure sore must … In nursing school, this is probably the first thing you learn in nursing school, how to prevent pressure sores.
Joyce: And you think this could’ve been prevented?
Patrik: Totally. That’s the first thing you learn in nursing school, how to prevent pressure sores.
Joyce: Do you think the hospital is so protected or do you think I can really go after them?
Patrik: I’m not a lawyer. What I will say to you is this. We are reviewing medical records all the time. What people do with them, I can’t tell you. I am reading some blogs of medical negligence lawyers. I’m reading some blogs. There are some very good blogs out there. I can send you to a couple. Those medical negligence lawyers wouldn’t be in business if nobody was coming to them.
Recommended:
Joyce: I just feel like the pandemic, I don’t know if they have like such a shield because of it. But I’m going to look into it.
Patrik: Look, all I can tell you-
Joyce: I’m going to get the record. You and I will look at the records. If you feel like I have a case and we can highlight certain things, then I’ll go to the next step. But I won’t get anybody get away with harming my sister. You know me. I’m a pit bull. I’ll figure it out.
Patrik: The risk of a pressure sore in ICU in particular is real. But then again, this is where good nursing comes in. It must never happen. For example, let’s just say your sister wasn’t on an air mattress in ICU and I don’t know whether-
Joyce: She was on an air mattress.
Patrik: She was?
Joyce: Yes, she was.
Patrik: So, how can a pressure sore happen if she was on an air mattress? That is-
Joyce: She was, for sure she was.
Patrik: Sure, sure. But then, if that’s the case, maybe your theory, what you said earlier that they haven’t moved her is accurate. I can’t believe that. But maybe-
Joyce: She went in November. It was the spike of the century. She was in the ICU on sedation. Like, sedated. Remember, I think they over-sedated her for 45 days.
Patrik: Yup.
Joyce: I really don’t think they moved her.
Patrik: They would have to move her. For example, if she opens bowels, they would have to turn her, clean her up. They would’ve to change linen.
Joyce: Okay. So then, can this happen naturally?
Patrik: No, not really. Because-
Joyce: Something happened that she had these extensive nasty, sores.
Patrik: I think it’s-
Joyce: It was already long before. I don’t know what to tell you.
Recommended:
Patrik: I think its negligence. And the reason I’m saying its negligence is we have clients at home that are bed-bound for months and even years, and they don’t get pressure sores.
Joyce: Okay. I’m so pissed now.
Patrik: I’ve looked after patients in ICU, that we’re in ICU for months and they didn’t have a pressure sore.
Joyce: Can my sister be more susceptible because she has diabetes?
Patrik: Absolutely, yes. Yes, absolutely. But then again, you have a high incidence of people with diabetes in ICU in the first place, and this shouldn’t happen,
Joyce: You know what, Patrik? I’m so pissed now. You just got me so mad. Okay, that’s fine. I’m going to look into it. But it’s like, because her bed sores are holding this up from the start.
Patrik: Absolutely. What stops them from putting the bag in?
Joyce: They cannot. They said they’re so extensive, they cannot. I even had to have a surgeon in this hospital do more debridement. It’s really, really bad. They’re really, really, really bad. Like I guess, they’re really bad. I don’t want to look at them. I don’t think I’m … I can’t. If that’s one part I just cannot swallow, it’s really that.
Patrik: Is she in pain because of it?
Joyce: I can only imagine.
Patrik: Is she getting pain relief?
Joyce: I tell them, that if they do wound care, they should give her something. But this hospital is very conservative about pain medication. The other one drugged her up. This one, not so much.
Patrik: Ask her if she’s in pain.
Joyce: I mean, I asked her. Sometimes, she’ll say no. You could see when she’s relaxed, she’s not. When she’s pain, she can nod yes. But she nods no sometimes. And when she nods yes, she gets pain medication. But I don’t think I’m going to go and ask her if she … Just to circle on one issue that you brought back to me, you said bring up the fact, if she wants to continue, I don’t think anybody who’s in that position’s going to say, I want to continue. Do you have patients that say yes? I just want to circle back because that’s a very sensitive topic with my family because-
Patrik: Very sensitive.
Suggested links:
Joyce: I can go both ways and say, “Look, guys. How long will we let her suffer?” We were reunited until recently where they’re saying, “Absolutely not. We will not do that.” The line on the sand just kept going, pushed back more, and more, and more, and more. It was great, and now we’re getting in a very gray area because we’re getting immune to her looking like this, and we’re not so black and white anymore. I’m not either. I can’t tell you that I’m going to make that decision. And my dad will absolutely, 1000% will never do comfort care, one billion percent. He said, “Let God decide. I will not do it.” My question is, if he will not do it, is it even worth to speak to him about it?
Patrik: It really depends what you as a family would want and-
Joyce: He won’t do it. He won’t do it. 100%. And I don’t want to do it. I don’t want to talk about it because I’m the one that keeps bringing her up, and everybody shuts me down. So, forget it. What am I going to tell my sister. I can’t-
Patrik: Yeah. That’s the problem. Nobody wants to kill their loved one, or whatever it is. So, I get that.
Joyce: If you’re telling me there’s a chance, then I’ll go all the way.
Patrik: There is a chance. They way to look at this from my perspective is if there’s life, there’s hope. As long as you can accept your sister won’t be the same …
Joyce: But I don’t know. Can she be half the same? I mean, I don’t know. Maybe she could.
Patrik: Maybe she could. Listen-
Joyce: Why do people say that she can’t be the same? It drives me insane because-
Patrik: Because they don’t know. They don’t know.
Recommended:
Joyce: I’m not saying she’s going to be happy and jolly that drives fine. But she can look me in the eye and still give me what I need with her eyes. So for me, that’s enough. I guess, I don’t really care. I really don’t care who she is. I love her the way she is. So, I don’t really care what people say.
Patrik: Of course.
Joyce: If I can give her the love and joy, I can pick it up. But my goodness, Patrik. It’s so much.
Patrik: It’s very, very complex. It’s very, very complex. What’s acceptable for you as a family, what’s acceptable for her, how long is a piece of string?
Joyce: That’s the problem. How long can we let her live like this? This is like you’re saying, a couple of weeks, a couple of months, a couple of years. I don’t know.
Patrik: A couples of years.
Joyce: I don’t want to say, a couple of years. Don’t say that.
Patrik: No, I know. I hear you. But the reality is we have people live on ventilators at home that report a very good quality of life, that’s acceptable for them.
Joyce: But they’re not walking. Are they walking?
Patrik: They’re not walking, nope. All of them would be wheelchair bound, bed bound.
Joyce: They are.
Patrik: The reason I couldn’t … This morning, well for me, this morning, the reason I couldn’t do, was it 4:30?
Joyce: Yeah.
Patrik: I couldn’t do 4:30 today, I ended up going to a client myself. With Intensive Care at Home, we had no staff this morning. So, I had to do a couple of hours myself this morning which is fine. A 50-year-old woman with motor neuron disease, she’s been living on a ventilator now for nearly two years. She lives at home with her family. She’s got an eight-year-old daughter. She always has a smile on her face.
Joyce: But she’s not using her hands or her feet?
Patrik: She can talk with a computer, with eye gaze.
Joyce: Okay.
Patrik: She’s got a very supportive husband. It’s such a wonderful environment there. But it depends on-
Joyce: She can’t talk, because she can’t have a talking tracheostomy because she’s literally getting air.
Patrik: She’s getting a ventilator, that’s why she can’t be off the ventilator, not even for a minute.
Joyce: Therefore, she can’t get the talking tracheostomy.
Patrik: No. She can’t talk. But she can use a computer with eye gaze. But it takes ages for her to type a word.
Recommended:
Joyce: Oh, my God. What does she do all day?
Patrik: She can use the computer. She’s got her family around her. She’s got a team of nurses around her. They’re a wonderful family, Joyce. I know it sounds horrible, but that’s the world that I’ve lived in for decades, you know?
Joyce: I know. No, listen. I never thought I would meet a good person like you in my life. Ever since I’ve been in this situation, all of a sudden, this becomes … I never thought I would ever speak about this stuff, ever. This is not in my radar ever.
Patrik: No. Of course, not. Of course, not.
Joyce: I googled you and I’m like, “Oh. I can’t believe I’m googling this.”
Patrik: Yup. No. It is a reality. Its quality of life is very subjective, very subjective. What if your sister can go home on a ventilator, she can be with your family, kids come to play, kids come-
Patrik: There might be a solution with a health insurance. I wouldn’t categorically say no.
Joyce: I just don’t want her on a ventilator.
Patrik: Yeah, sure.
Joyce: Like you’re saying, the 80 needs to go down to 10. That’s eight points. Possibly, we can do this in a couple of weeks.
Patrik: Possibly.
Joyce: We need to push the range of motion 100% and we need to push that bed to be a little bit like a chair to try … and I’m really going to push that. But I need someone who believes in that. I’m going to find that person tomorrow. I’m going to find that person.
Patrik: Listen to this interview that I sent you on WhatsApp. Listen to this, please.
Joyce: Okay.
Patrik: This girl should give you some ideas as much as I hopefully can give you some ideas. There is something else. Have a look at the ventilator picture again. Let’s just say, the pressure support goes down to 10, can you see the volume which is, what is it, 300 and something?
Joyce: 378, right?
Patrik: Yeah. So, those volumes need to stay the same.
Joyce: I thought the volume needs to be a 600 one? Didn’t you tell me that?
Patrik: What’s your sister’s weight?
Joyce: Nobody’s even telling me. I don’t even know.
Patrik: Any rough idea?
Joyce: Now? Maybe like a 150. I don’t know.
Patrik: Okay. Hang on, hang on.
Joyce: I don’t know.
Patrik: Okay. Let’s just take 150 pounds. That just means, you get-
Joyce: She was 180, 190. So, I don’t know. I don’t even know, maybe 170. I have no idea.
Patrik: Okay. Let’s just say for simplicity-
Joyce: I really have no idea. Maybe 130. I’ve no idea how much she weighs.
Patrik: Okay. Let’s just say for simplicity, 150, which is 70 kilograms, because I’m a metric person.
Joyce: Maybe she’s skinnier than that.
Patrik: Right, okay. Let’s just say 70 kg for simplicity. The volumes that you see in that picture, the 378 needs to be around weight. Its weight based. The volumes need to be around 400. It’s about okay. But the problem is, let’s just say you drop down the 18 to 10, these volumes would probably drop to 150, and that would be too low. Are you following?
Joyce: Right. How do we get that number up? Only by elevating her?
Patrik: Strengthening her breathing, physical therapy, strengthening her upper body, strengthening-
Suggested links:
Joyce: I don’t know why are they not advocating?
Patrik: Joyce, the frustrating that I’m having as well by doing this, by looking at ICUs, shocking. Shocking. I work in a different system. All I see is, “Let LTAC deal with it.” Then, once patients go to LTAC, it’s going from bad to worse.
Joyce: I know. I know that’s why I want her off the ventilator before anything else happens.
Patrik: And they’re not doing what they’re supposed to be doing to get her off that ventilator.
Joyce: There is a respiratory special hospital that actually my sister … She was in the same position and, she’s actually off the ventilator by going to this respiratory hospital. There is an option for that, but I don’t want to get there. I just want her off the vent. Then, I’ll move on to the next thing, because then once she’s off the ventilator, I have a lot more options down the line without this vent. I have to get this vent out of my life and then, whatever comes after, I’ll deal with it. I got to get her out of it. Okay, so physical therapy and get her sitting up. I’m going to really advocate that for tomorrow. I just hope I know what I’m doing because the problem is, they’re going to listen to me.
RECOMMENDED:
Patrik: Unfortunately, what I could see across the board is it’d probably fall on deaf ears because they’re not doing it. But you got to keep doing what is right.
Joyce: I’m going to really get on the doctor and really fight for it. Because they keep canceling physical therapy because they said she’s not participating and the nurses are doing range of motion. They’re not doing it.
Patrik: All right. Who is in-charge medically? Who’s making the decisions medically? Pulmonologist?
Joyce: No, she has a main doctor and then, she has a pulmonologist, and then she has infectious disease. But the main person is the doctor or the pulmonologist. Either one of those I believe can write an order for a physical therapy. So, I’ll stay on top of it tomorrow and get on top of it. I just feel like I’m not being listened to. But when I’m going to be in their face tomorrow, I’ll get the doctor to come on the phone and order it like, right now.
Patrik: Right. Maybe just for you to illustrate why I sort of keep coming back to the mobilization, so because the system that I work in, there are no LTACs, so you had to get patients off ventilation and ICU. There was no other choice.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!