Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED”n and in last week’s episode I answered another question from our readers and the question was
How Can We Stop the ICU Team From Pushing My Dad in ICU for a Gastrostomy Tube Insertion?
You can check out last week’s question by clicking on the link here.
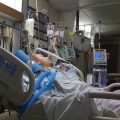
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Isaac, as part of my 1:1 consulting and advocacy service! Isaac’s dad is a long-term ventilated patient in ICU. Isaac is asking what are the risks that his dad might face after a tracheostomy.
What are the Risks that My Dad Might Face After a Tracheostomy in ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Isaac here.”
Patrik: Right. Okay. And-
Isaac: But where do you think the bleeding came from? Because I’m not sure if it’s the cancer that’s causing it. They’re trying to figure out where his bleeding came from.
Patrik: Yeah. The first thing that probably-
Isaac: I just keep telling them, “I don’t want to sign for the percutaneous endoscopic gastrostomy (PEG) tube because that it is not going to help anything else.” They just want to transfer him out. If they transfer him out, he could die.
Patrik: Right. I agree.
Isaac: For sure.
Patrik: I agree. No, I agree with you there.
RECOMMENDED:
Isaac: I even saw when they took him out of ICU to the second floor. I go, “Oh great.” And then every week, the doctor changes and it’s one doctor, she’s on the same page as me. She’s like, “Wait on the percutaneous endoscopic gastrostomy (PEG) tube. I don’t mind. I understand you.” The other one, she started getting aggressive saying, “If you don’t do the percutaneous endoscopic gastrostomy (PEG) tube, I’m going to take out the feeding tube out of his nose.” I said, “Okay, go ahead and take out the feeding tube.” She got upset. She kind of talked to me like that and told me if I don’t do this, do that. I know, eventually, my dad is going to need the feeding tube, I get it, I understand exactly what they’re talking about. But, let’s figure out everything else first. I’m not going to do the percutaneous endoscopic gastrostomy (PEG) tube, if you’re just shipping him out.
Patrik: Well, this is the thing. Your dad, by the sounds of things, might need a percutaneous endoscopic gastrostomy (PEG) tube. But what you can do-
Isaac: He does.
Patrik: – is you can bargain with them. And you can say, “Look, I’m doing a percutaneous endoscopic gastrostomy (PEG) tube if you’re not shipping him out.” You can bargain with them. You know?
Isaac: Yeah.
Patrik: I think-
Isaac: But I think they- Uh-huh?
Patrik: Get it in writing. Get it in writing. Bargain with them. You know?
Isaac: Yeah?
Patrik: It sounds to me like-
Isaac: I could do that, huh?
Patrik: It sounds to me like he’s not moving away from the ventilator at the moment. But by the same token-
Isaac: Yeah.
Patrik: By the same token, in the meantime, they should put in a nasogastric tube. They should. Irrespective of your decision. He still needs feeds right here and then.
Isaac: Yeah.
Patrik: You know?
Isaac: Yeah.
Patrik: That hasn’t changed. He still needs feeds. And by not putting a nasogastric tube in while you are deliberating what to do next, that’s almost negligent.
Isaac: Yeah, you’re right.
Patrik: He needs food. He may not need a lot, but he needs some nutrition.
Isaac: They were saying I guess the nasogastric tube is messing with the cartilage in his nose. What do you think about that?
Patrik: With the cartilage in the nose? What do you mean by that?
Isaac: They say ulcers.
Patrik: Oh, I see. I see, an ulcer, okay. Yeah. Yeah.
Isaac: He had it for over 4 weeks.
Patrik: Yeah, no, I agree. If that is the case, you probably should move to a percutaneous endoscopic gastrostomy (PEG) tube, but that shouldn’t stop you from-
Isaac: Oh. Okay.
Patrik: That shouldn’t stop you from bargaining to keep him in ICU.
Isaac: Yeah. So, how would I get it in writing from the doctor? And then, also telling them, every week, or every doctor changes. So, then it gets to another doctor who just-
Patrik: Yeah. Look, there’s not much-
Isaac: Yeah.
Patrik: There’s not much you can do in terms of the doctors changing. I mean, that’s way beyond your control.
Isaac: Yeah.
Patrik: There’s not much you can do there. It’s-
Isaac: But if one’s trying to say that she’ll keep him here. Then, how does it go about when it changes to the following shift?
Patrik: Sure. Do you know who is the main decision-maker? What I mean by that is, do you know one of those doctors, are they the medical director, for example?
Isaac: Yeah, like the case manager, moreover, his main doctor?
Patrik: Yes, the main doctor. Who’s sort of the-
Isaac: Yeah. She’s the one who wants to ship him out.
Patrik: Right. Okay.
Suggested Links:
Isaac: She’s the one about the whole percutaneous endoscopic gastrostomy (PEG) tube and she says that he can’t be here forever. He needs to be shipped out. But I understand that, you know?
Patrik: Sure. Sure.
Isaac: But I know that’s the plan, is to do the percutaneous endoscopic gastrostomy (PEG) tube, and ship him to subacute.
Patrik: Well, yeah, sure.
Isaac: We’ll still think about that.
Patrik: Right. That subacute-
Isaac: And she’s an aggressive one.
Patrik: Sure.
Isaac: She’s just more like, “It’s time to get him out.”
Patrik: Yeah, yeah. Okay. Okay. What about-
Isaac: The other ones are more reasonable. I know he needs a percutaneous endoscopic gastrostomy (PEG) tube, he really does, you know? But-
Patrik: Sure. Timing.
Isaac: Shipping him out, it’s kind of like, “Wow.”
Patrik: Yeah, it’s timing. It’s all about timing.
Isaac: Yeah, it is timing.
Patrik: What about, with the cardiac arrest yesterday, is he on any vasopressors? Do you know?
Isaac: Is he on any vasopressors, you said?
Patrik: Yes. Yes.
Isaac: Is he on any vasopressors?
Dan: No.
Patrik: Okay, no.
Isaac: He’s on IV fluid, right?
Dan: He was on Dextrose 5% in Water (D5 Water).
Isaac: He’s on D5 Water.
Patrik: What?
Isaac: D5 Water.
Patrik: Okay. And no sedation?
Isaac: And no sedation?
Dan: No, no sedation.
Patrik: Okay. Good.
Isaac: He’s kind of tired. I popped in, I said, “You know who I am dad?” He said, “Yes.”
Patrik: Okay.
Isaac: He’s like that.
Patrik: So, he’s rousable.
Isaac: Yeah-
Patrik: Okay.
Isaac: But he’s kind of sleepy.
Patrik: Yeah. And the kidneys are working?
Isaac: The kidneys are working?
Dan: Yeah.
Patrik: Okay.
Isaac: Yeah, with the blood, what do you think the reason why he has a blood transfusion or low hemoglobin? The doctor said it could be the cancer with it, just not producing enough, or it could be something else. She’s trying to check it. She didn’t want to say one reason.
Patrik: Yes, it could be the cancer, but it could also simply be that he’s got anemia. Have you heard of anemia?
Isaac: Yeah. Anemia, right.
Patrik: Yeah, that he may not produce enough red blood cells. There could be a number of reasons. I would argue that in order to find out why he’s not producing enough red blood cells, probably need a hematologist. A hematologist needs to look at that.
Isaac: Is that the one who withdraw the blood?
Patrik: No, no, no. You need a hematologist to find out why the hemoglobin drops.
Isaac: Okay. Yeah, this is the first time it happened too. That’s why the-
Patrik: Right. Right. And the reason that is so important is, God forbid, if he has to go to subacute, those specialists are not there. So, I think now-
Isaac: Exactly. That’s what I said. That’s exactly what I said.
Patrik: Right. So, now that he’s in ICU, get the specialist in, right?
Isaac: Yeah.
Patrik: Get the specialist to look at him. Now, other question, if he-
Isaac: Can you text me that name for the blood?
Patrik: Oh, the hematologist? You mean that?
Isaac: Yeah.
Patrik: I’ll text that to you, for sure. For sure.
Recommended:
Isaac: Yeah, so I know exactly what to tell.
Patrik: Yeah, yeah. So then, if he has to go to subacute, how far away are those places? Are they around the corner? Are they hours away? What are we talking about?
Isaac: Yeah, that’s what I told her too and she goes, “Yeah,” that she’s going to give me the social worker’s information before I even do the percutaneous endoscopic gastrostomy (PEG) tube, because I told her, “I don’t want to do the percutaneous endoscopic gastrostomy (PEG) tube, and then they’re going to ship him out right away.” I don’t know where he will go so they’ll kind of give me an option of where he was, so I can go see first.
Patrik: Absolutely. Absolutely. Do you know if those places are around the corner, or are they far away? Do you know?
Isaac: No. That’s what I asked her. She said that she’s going to have a social worker call me beforehand because she said she agrees that. The doctor for this week, she’s very understanding. She goes, “You know what? I understand why you don’t want to do the percutaneous endoscopic gastrostomy (PEG) tube.” She’s like, “Go check first and go make sure that it’s close by. Go see if you like it before you even decide to do the percutaneous endoscopic gastrostomy (PEG) tube.” I go, “Yeah, that’s what I want to do.” She goes, “No, I understand exactly.” I told her, “Yeah, you’re understanding, but the main doctor, the case manager doctor, she’s not.
Patrik: Mm-hmm. Okay.
Isaac: Oh, my god.
Patrik: What about the oncologist for the cancer? Is he or she involved?
Isaac: Yeah. But we haven’t done an actual biopsy, but they did test the fluid and came that it is cancer. So, they said in that case, it’s Stage 3 or 4.
Patrik: Right.
Isaac: What was the name for the tracheostomy, that you were asking, because respiratory’s here, so that we can ask.
Patrik: The inner cannula.
Isaac: What?
Patrik: Inner cannula, or inner-
Isaac: Does he have an inner cannula?
Ralph: Yeah.
Isaac: He does have inner cannula?
Ralph: Yeah, he does.
Patrik: Okay. Well, again, if he had a respiratory arrest yesterday, what’s the reason? Do you have access to the medical records?
Isaac: See, that’s a problem. He came here with his driver’s license. We can no longer find it. So, in order for me to get his medical records, they needed my driver’s license to have it along with him but we don’t have any because it’s on file. I checked if they could scan to see if it’s on file and there’s nothing there.
Isaac: Now, I was wondering about the oxygen level went to 73, but then bounces back up to like 94. I don’t- And then it goes off, so I’m not sure if it’s reading correctly.
Ralph: I’ll check.
Isaac: It doesn’t read, right? Yeah, see, it’s like a 95 now? So, that’s what I was kind of worried about. Every time I come, it’s all about the percutaneous endoscopic gastrostomy (PEG) tube. It’s like, so I get upset. You know?
Patrik: Right.
Isaac: I understand, I think he needs the percutaneous endoscopic gastrostomy (PEG) tube at this time, because he had it for a long time, and there are a lot of issues, but I don’t want to just ship him out. I knew when he went to the second floor, I kept going, “Wow, they’re not going to take care of him” because they don’t see, they don’t check the blood pressure and the oxygen levels too much. He’s just not stable, you know?
Patrik: Yeah, yeah. Yep, I get it.
Isaac: And then, that’s probably what happened, it kept dropping and dropping, and then that’s what happened, because when I went, I always ask them, “What’s his blood pressure at? What’s this at? Can you go check in his oxygen level?” “Yeah, yeah, he’s good, his oxygen’s at like 94, 95.” “Oh, okay. Perfect.” I always make sure before I leave, because I know it’s not like ICU, I could see him right now, but there, I can’t. And then, when he code blue I was like, “Wow, I knew.” So, I know- Could imagine when he gets to subacute, it’s probably worse care, right? They don’t see them too much?
Patrik: Oh. At the moment, he would have a 1:1, or 1:2. In subacute, he would have a 1:10. It’s ridiculous.
Isaac: Yeah. That’s why I get nervous about the-
Patrik: It’s ridiculous.
Isaac: Yeah. They were weaning him off the ventilator and he was doing good, but he was doing his breathing trials for a couple of days, but then this happened and now it bring him all the way back.
Patrik: Right. Right. So, it’s going to be disastrous for him going to subacute, just on that level. So, just coming back quickly. And you can, look, I don’t know what happened yesterday. But I can tell you, if he’s got an inner cannula, my biggest concern..So, imagine, he’s going to 1:5 or 1:10 nurse to patient ratio, nobody’s going to change or check that inner cannula regularly. And it’ll block off and he’ll end up with another arrest, you know? It’s just bound to happen.
Isaac: Yeah, for sure.
Patrik: It’s just bound to happen.
Isaac: Yeah, I don’t know that he’ll make it out of that one. That’s what I was telling them.
Patrik: Yeah. It’s just bound to happen.
Isaac: So, they need to change it out, then, right?
Patrik: They need to change it-
Isaac: For how many times?
Patrik: As I said, at least three times a day, at least.
Isaac: Yeah. And what about the one that’s longer?
Patrik: I am not sure what’s the reasoning, what’s the rest part of the tracheostomy, not too long, I don’t know.
Isaac: Yeah.
Suggested Links:
- Quick tip for families in ICU: What are the right steps when weaning off ventilation & tracheostomy?
Patrik: You would need to ask them-
Isaac: Why, huh?
Patrik: Why.
Isaac: Yeah.
Patrik: What about the oncologist? Did the-
Isaac: They never did a biopsy. They just tested the fluids in his lungs, and it came back-
RECOMMENDED:
Patrik: Sure.
Isaac: The fluid came back as cancer, so then they staged it at Stage 4. I was shocked. But everything else in his body’s good. I know his lungs are real bad.
Patrik: What about the oncologist? Are you talking to the oncologist?
The 1:1 consulting session will continue in next week’s episode
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!