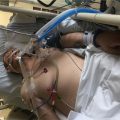
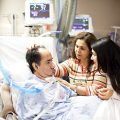
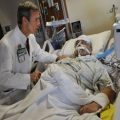
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I want to answer questions from one of my clients Isaac, as part of my 1:1 consulting and advocacy service! Isaac’s dad is ventilated in ICU. Isaac is asking if they have the legal right to access the medical records of his dad.
Do We Have the Legal Right To Access the Medical Records Of My Ventilated Dad in ICU?
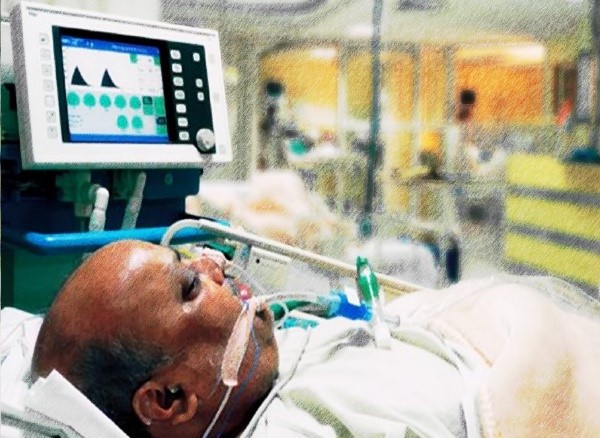
“You can also check out previous 1:1 consulting and advocacy sessions with me and Isaac here.”
Patrik: The Precedex would get his blood pressure down. No question.
Isaac: For sure, huh? Yeah, I told the doctor that too. I said, “Well, why do you guys have him on Precedex during the day if you guys have him off completely.” “Oh, he wasn’t sleeping.” I said, “He doesn’t sleep during the day just during the nighttime.”
Isaac: I said, “Well, why don’t we stop the Precedex right now and see how his blood pressure goes?” “No, we want him comfortable.” I go, “He looks comfortable to me.” But, they didn’t stop it. I said, “Well, you guys have been saying he can’t go through the surgery unless his blood pressure goes up, why don’t we turn off the Precedex if it’s not really necessary during the day. Why are we giving it to him,” I told them. “Oh, just to keep him stable,” and then I asked her, “Well, doctor,” I’ll have to ask her like it was her idea because then, they don’t like hearing that. I told her, “Well, don’t you think it can lower his blood pressure?” “Well yeah, it can.” I say, “Well, you have been saying the blood pressure’s too low that you don’t want to do the tracheostomy so maybe we should turn it off?” “Oh, we’ll look into that but right now we’ll just keep him comfortable.” I don’t know.
RECOMMENDED:
Patrik: If I was you, I would also ask for the medical records.
Isaac: Yeah.
Patrik: The reason I would ask for the medical records if I was you is simply, if I was you, I would want to see what medications is he on. I wouldn’t be surprised if they’ve got something else for sedation and they’re not telling you. I’ve been doing this long enough to know that most ICUs are only telling half of the story. If you don’t know what questions to ask and if you don’t know what to look for, they’re only telling you half of the story.
Isaac: Oh, yeah, there was another bottle hanging. I told him, “What is that?” They said it’s something for his protein. I said, “Protein?” “They say yes, for the body.”
Patrik: I would-
Isaac: I was going to take a picture the other day.
Patrik: I would do that. I wo just ask later. Then-
Patrik: And-
Isaac: Uh-huh (affirmative)?
Patrik: In this day in age, they should be just sending you a link to a website with a username and a password. You know?
Isaac: Yeah, very easy.
Patrik: Very easy. Don’t get me wrong. Not all hospitals have electronic records yet, but most have nowadays. You know?
Isaac: Yeah. Then, so I shouldn’t sign for both at once? Now they don’t want to do the tracheostomy until I do both of them. And I was like, “Well what are you guys waiting for? I never signed for the percutaneous endoscopic gastrostomy (PEG) tube. Well, let’s just do the tracheostomy.” “But it’s not good for him to be on the ventilator for too long.” I said, “I agree. That’s why I signed this a couple of days ago.”
Patrik: That’s why I’m sort of, are they blackmailing you? Are they trying to blackmail you to consent to a percutaneous endoscopic gastrostomy (PEG) tube whilst in the meantime they should be doing the tracheostomy. I think they need to do the tracheostomy full stop.
Isaac: Yeah, I agree and I told them that. I told them, “Well, I haven’t signed for a percutaneous endoscopic gastrostomy (PEG) tube so let’s just do the tracheostomy and we’ll go there.” They’re like, “Well, why would you want to put your dad through double surgery and more of a chance of double sedation and double risk? Why don’t you do it at two-in-one?” I said, “Because I don’t know if he needs a feeding tube right now if he’s already feeding through the nose so that’s not the problem at this point. Well, we’ll deal with this then.” They said, “But you might be putting too much trauma on him.” What do you think?
Patrik: No. No, I disagree with all of that. I disagree with all of that. What they’re not telling you is, once he’s got a percutaneous endoscopic gastrostomy (PEG) tube and a tracheostomy, they will be pushing you out to LTAC. If he only has a tracheostomy, they can’t push you out to LTAC or it’s more difficult. Again, from my experience, Isaac, patients can live with a nasogastric tube for months.
Isaac: Well, they can?
Patrik: There’s no reason why people can’t have a nasogastric tube for months. The other thing is this. The other issue is this. When someone has a percutaneous endoscopic gastrostomy (PEG) tube, it’s almost like a permanent thing. People are getting very complacent. Then, they will not try hard enough to get your dad eating again because it’s got this permanency around it.
Isaac: Yeah.
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
Patrik: Right? It makes people very complacent. All I see-
Isaac: But, then I told my dad. He said, “What’s going on with his eyebrows?” I said, “That’s your doctor. Remember I told you … Because, they come and try to talk to him when I’m not there too. I said, “Remember, if they ask for the percutaneous endoscopic gastrostomy (PEG) tube, no.” He shook his head like no. I said, “The tracheostomy, I signed,” and he said, “Yes.”
Isaac: Then, I tried to explain to him why and he said, “They’re going to try to shift you off to LTAC or to a newer facility. He shook his head like, no. I said, “You might need the percutaneous endoscopic gastrostomy (PEG) tube later but right now, we’re just going to keep you feeding through the nose and he pointed his nose and said, “Yes.”
Isaac: Right now, he was looking at me and the doctor like, why they don’t want to do it? and then I said, “Dad, I don’t want to put the feeding tube in your stomach if you don’t need it.” He shook his head like, no. Don’t do it if I’m feeding right now.
Patrik: Exactly. You should be pushing for a tracheostomy.
Isaac: Okay. Just tell them then, the family doesn’t agree. I don’t have to sign nothing, right?
Patrik: You have to sign nothing. I would sign for the tracheostomy though. I would sign for the tracheostomy, but I would-
Isaac: Yes.
Patrik: I would also-
Isaac: I did that three days ago.
Patrik: Right. I would also push for the medical records because I do believe there is stuff in the medical records that they are not sharing with you. There’s stuff happening that they’re not sharing with you.
Isaac: Okay so I’m going onto medical records and that family just wants to do the tracheostomy. I already signed for it. I don’t know why they don’t just do the tracheostomy.
Patrik: Yeah, there’s no reason. There’s no reason. Don’t have them blackmail you. They only want both things, but he should have a tracheostomy now. How many days has it been now since he’s been ventilated for?
Isaac: For four weeks and six days.
Patrik: Yeah, no, it’s way overdue. Tracheostomy is way overdue.
Isaac: Yeah. They told me that and I said, “Well, I already signed. I don’t know what you guys are waiting for.” They said, “Because we want to do the percutaneous endoscopic gastrostomy (PEG) tube as one.” I said, “I told you I don’t want to do that.”
Patrik: That’s blackmailing. That’s blackmailing.
Isaac: Yeah. Yeah, so I’m just going to tell her no, the family doesn’t want to do it. We don’t want to do it. We’re going to do that later. They keep telling me, “Oh, we can’t do that with the tracheostomy, with the feeding tube.” I told him I’ve heard what they do in many places with the tracheostomy, with the feeding tube in the nose. I don’t understand why you’re saying that.
Patrik: Yeah.
Recommended:
Isaac: How long can he have the feeding tube in his nose for?
Patrik: For months unless they might have to change it once. I’ll tell you what the biggest risk is, for the feeding tube in the nose. There are some risks attached to it. That’s number one, a pressure sore in the nose. And number two, if your dad is more alert, it’s easy to pull out the nasogastric tube.
Isaac: Yeah.
Patrik: Because it can be uncomfortable. It can be uncomfortable.
Isaac: Yes.
Patrik: But, other than that, there’s really no risk. The biggest risk that you are facing with a percutaneous endoscopic gastrostomy (PEG) tube is to go to LTAC quickly and the other risk is it’s got a permanency to it. It’s got a permanency to it that’s just not healthy. If he does have a nasogastric tube, people will keep trying to get him eating again. It’s not going to happen when he has-
Isaac: Yeah.
Patrik: You know?
Isaac: Yeah.
Patrik: You can see that.
Isaac: Okay. Yes, so I’m just going to tell them “Sorry, we do not want to do a percutaneous endoscopic gastrostomy (PEG) tube and let’s do the tracheostomy”.
Patrik: Exactly.
Isaac: What if they keep saying, “Oh, no. We’re not going to do the tracheostomy without a percutaneous endoscopic gastrostomy (PEG) tube.”
Patrik: Well then, I would keep saying then-
Isaac: Who do I talk to or-
Patrik: Yup, then I would say if I was you, I would say, “You’re not acting in the best interest of him.”
Isaac: Okay.
Patrik: Right. They’re not acting in the best interest of him. I’ll send you an article in a minute. I’ll send you an article on when a tracheostomy should be done. It should be done after a couple of weeks.
Isaac: Yeah. That’s what I told them. I signed and then I’m ready for the tracheostomy but-
Patrik: Yeah, they’re not-
Isaac: I told them I signed. Don’t wait. Just do the tracheostomy.
Patrik: Absolutely. Absolutely. That tracheostomy needs to happen.
Isaac: Okay. For sure. Okay. Then, I’m going to request for the medical records.
Patrik: Absolutely.
Suggested Links:
Isaac: As soon as I get them, I’ll send them over to you.
Patrik: Absolutely. Yup.
Isaac: Okay so I’ll give you call tomorrow?
Patrik: Yup, when-
Isaac: I’ll tell you what they say.
Patrik: Sure. Sure. Be in touch.
Isaac: All right. Thank you so much. I appreciate it.
RECOMMENDED:
Patrik: It’s a pleasure. Thank you, Isaac. You’re welcome. Take care for now. Thank you.
Isaac: You too. Bye-bye.
Patrik: Bye. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!