Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the first question from Eliza in last week’s episode was
The doctors in the ICU are urging us to sign a DNR form. What can I do to turn this around?
You can check out last week’s question by clicking on the link here.
In this week’s two-part episode of “YOUR QUESTIONS ANSWERED“, I want to answer the questions from one my clients ELIZA as part of my 1:1 consulting and advocacy service!
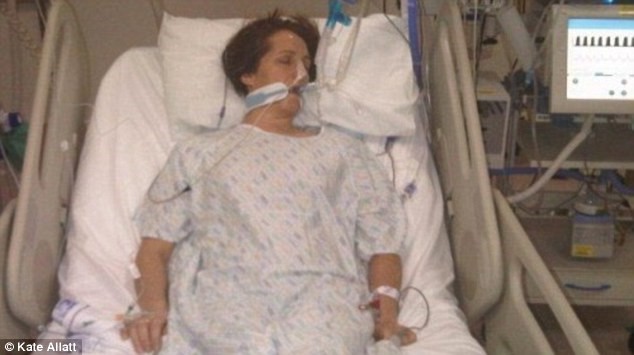
Eliza has her mother transferred in the Intensive Care Unit due to Liver Failure. Her mother was eventually diagnosed with Renal Failure treated with dialysis. Additionally, she had fluid in her lungs and was put in a ventilator.
The ICU is telling me that my mom no longer has any hope of surviving? Can a DNR take effect without my decision?
Eliza: Mm-hmm (affirming).
Patrik: Right. Was that part of their plan when they were doing the trache? Was that part of?
Eliza: Yes.
Patrik: Right. Okay. So that plan has fallen through. Okay. I’m glad I’ve asked the question. Here is where it probably gets interesting for you. Let’s just say the trache would have succeeded. They would have succeeded with doing the tracheostomy. She wasn’t bleeding. They would have shipped her out to long term acute care. And I can tell you from experience, they’re not shipping out people to long term acute care if there’s no hope of survival. Okay. So they’re now going from trying to do a trache, which they obviously didn’t succeed for now.
Now they’re going from, potentially going to transfer her to long term acute care and within 48 hours, they’re saying she’s dying.
Related article:
Eliza: Yeah.
Patrik: There’s a mismatch as far as I’m concerned. There’s a mismatch in communication. Why would they do a tracheostomy and then plan to send her to long term acute care? Well, the tracheostomy failed. Okay, we acknowledge that for now. Then all of a sudden, they’re saying there’s no hope and she’s going to die. So, the question to me then would be, what has changed besides the bleeding of the tracheostomy obviously making it very difficult for them to perform that trache? I understand that.
So how can she go from potentially getting a tracheostomy, going to another facility and then all of a sudden, they’re saying well, we’ve got take her off.
Eliza: Right.
Patrik: There’s no correlation as far as I’m concerned and also from my clinical experience. You know what I’m saying?
Eliza: Yeah.
Patrik: I would never claim in a million years that I can save her life. That would be foolish for me to make that claim. But what I can do, definitely, is help you maximize the chance for survival, especially in the short term. Maybe she needs another few blood transfusions and maybe they need to try then again for the trache.
Eliza: They said that she can never get a tracheostomy.
Patrik: I question that. Let me ask you this, when they did the tracheostomy, did they do a trachea surgically or percutaneously? Am I making sense here?
Eliza: You’re making sense, but I don’t know what it means. I know she went into surgery.
Recommended:
Patrik: Okay. She went into surgery. Okay, okay. Then it must have been a surgical. I’ll tell you where I’m going with this. A lot of ICU’s in this day and age, they do their traches in the ICU and it’s called a percutaneous tracheotomy, which is not a surgical one. They’re basically just punching a hole in the neck and it’s a very quick procedure, can be done within half an hour or 45 minutes in this day and age.
The risk for bleeding is there, especially in liver failure when coagulation and blood results are off. The risk is there, don’t get me wrong. But, sometimes it’s also a matter of maximizing the coagulation in the blood beforehand. And that’s a question that I would ask, have they optimized her coagulation status. Do you know what I mean by coagulation ?
Eliza: No.
Patrik: Right. Sorry. Coagulation basically … when you take blood results, there are coagulation results and that would be APTT, INR and that would indicate how quickly somebody is bleeding, or how thin the blood is. I don’t want to get too technical here or too medical, but the reality is, you can optimize that, especially before performing a procedure and I’m wondering whether they’ve done that or not.
Whether they tried to optimize that before doing the trache. Those are all the sorts of question we would need to ask. You see, there is no, at the moment, what I can see is they’re putting an artificial timeline on this and saying, tomorrow she needs to be taken off. There’s nobody in the world who can force you to make that decision. If they are-
Eliza: Well, they told me that if I don’t, then they can make the decision-
Recommended and more information about tracheostomy:
Patrik: No, no, no, no, no no no no. And that’s where we can help. That’s where we can help. We’ve helped so many families, I don’t know how many case studies you’ve read on our website. We’ve helped so many families in similar situation where, the next step really from my end would be, we would have to … number one, I could set you up with a series of questions to stop them from doing that. And number two, we could together, on a three-way call, we could talk to the doctors.
Have you had a family meeting, like a formal meeting with them?
Recommended:
Eliza: I’ve had three or four.
Patrik: Okay. And they’ve always been sort of formal, in a room. Tell me a little bit-
Eliza: Yeah.
Patrik: Okay. How many people were there? You. Who else was there?
Eliza: Yeah. Me and my sister, my aunt, my grandmother and my best friend.
Find more information about family meetings:
Patrik: Okay. And who was there…. Right. And who was there from the hospital?
Eliza: The palaeontologist and a nurse practitioner.
Patrik: Just two people from the hospital?
Eliza: The first time, the first two times. Then the third time, it was a doctor, well a specialist, and two practitioners and a palaeontologist.
Patrik: Right. Who were those practitioners? Were they ICU specialists? Or do you know?
Eliza: I’m not sure.
Patrik: Okay. When was the last meeting you had?
Eliza: Yesterday.
Patrik: Yesterday. Okay. And pretty much yesterday they told you about, yesterday they told you about that today sort of decision making time. Is that where they left it?
Eliza: Yeah.
Patrik: Right. Okay. Well, number one, there’s a couple of things there really. You don’t need to respond to that pressure. I can assure you that they can’t just take your mother off life support without your consent. That would be murder. They often position those situations like as if they were in a position to make those decisions, but they can’t. Seriously, if they took her off the ventilator tomorrow without your consent, that’s murder.
Eliza: I kind of already gave it to them because how she said it again today, yesterday, she said we need to know something by the morning.
Patrik: No, no, no.
Eliza: So this morning, here they come and they’re like, “Well, if you guys don’t plan, then we’re going to go ahead and do it today.”
Patrik: No, no, no. No. No.
Eliza: Unless you give us a day and time. That’s what they told us.
Recommended:
Patrik: No, no. You’re just responding to something they’re imposing on you. Just stop responding to that. Right. On what grounds? There is no law that permits them to take your mother off the ventilator Again, I can only … I can’t stress that enough. If they did that, they’re committing murder. Yes, what they are trying to do is, they’re trying to put artificial pressure on you because they want the ICU bed. That’s what they’re doing.
Eliza: I said well I didn’t know you guys could do that without my consent. She said we kind of can when we feel it’s going to be more hurt to the patient.
Patrik: No, no, no.
Eliza: More harm than good.
Patrik: No. So what we need to do there actually really is the next step. Number one … two things that we do right. The first step would be; I will set you up with some questions that you can ask. But, number two, we can also get on the phone to the doctors. Or when you have the next meeting with them, I can be there over the phone with you. Then we will stop them from doing that. They can’t do that. And I will help you with that. Most likely, they’re breaching the law. They’re breaching their own hospital policies. They’re breaching a number of things.
Also, what we don’t know at this stage is, your mother is pretty sick. There’s no doubt about that. But, what we don’t know at this point in time is, have they done everything within their power? If they stopped dialysis, they haven’t done everything within their power.
Recommended:
Eliza: Right.
Patrik: Right.
Eliza: Yeah, that’s what I was thinking.
Patrik: Absolutely. Absolutely. So, your current reality really is like, they’re telling you things they want to do. You’re not in agreement with it. And the roadblocks really are, they are wanting to pretty much kill your mother and you’re not agreeing with it.
Eliza: Right.
Patrik: That’s the reality. At the moment, just remove yourself from the pressure that you’re on. Just remove yourself from that for a moment. You are just responding to an unreasonable request from the hospital. That’s all it is. You’re responding to an unreasonable request from the hospital. And the reality is, at the moment you are responding the way they want you to respond and we need to change it. All we’re doing is we’re changing the situation. That’s all it is.
We are changing a potential life or death situation. That’s all we do. Up until probably until you’ve spoken to me, you thought it would not be possible, but all we’re doing is we’re changing a situation. That’s all we do. Okay. You’ve really got to step back from responding to that pressure.
Recommended:
Eliza: I’ve tried, but they keep coming. They don’t stop.
Patrik: It doesn’t matter what they do. You see, in a situation like that, it’s never what you’ve been told. It’s never what you’ve been told that determines the outcome. It’s always how you respond that determines the outcome. What they tell you is not important. How you respond is important. If they came to you and said, “Oh, Eliza, would you jump off this bridge tomorrow?” You wouldn’t jump off the bridge would you? So it’s not-
Eliza: No. I’ve been telling them I don’t want her off of the ventilator.
Find more information about asserting for the patient:
Patrik: Sure. And that’s good. That’s good that you’ve done that. Now what we need to do next is … what you haven’t done yet is you haven’t argued on a clinical level. What I mean by that is, I’ve seen those situations hundreds of times. And I know that number one, they haven’t maximized their therapy options. Number two, it’s just a knee jerk reaction from them. They’ve tried one thing. It didn’t work. So now what?
They need the ICU bed, so their way forward is to, unfortunately, try and kill your mother. We will stop them from doing that because we will ask them questions and we will argue on a level that they can’t ignore. You haven’t argued on a clinical level because you can’t at the moment. You need the clinical insight. And you also need the insight from a hospital or from an ICU environment.
Eliza: Mm-hmm (affirming). Yeah.
Eliza: Okay. Okay. Well, the number to call you back … I’m going to go back in the hospital and discuss these options with my family.
Patrik: Yeah.
Eliza: 0K.
Patrik: Yeah.
Recommended:
Eliza: Correct.
Patrik: Okay, Eliza, I can be available any time over the weekend. I can be in the next family meeting you’re in over the phone or in person! I would love to continue to help you with this because I think this is a life or death situation and I can help you buy time that will give your mother the time she will need, and also you will need as a family to give her that time. Part of my 1:1 consulting and advocacy is to get results for families in Intensive Care! All the hospital wants to do is, they want to empty that bed and they don’t care how they do it. You are just responding to pressure, that’s all. You need to change your response. That’s all it is.
Eliza: Right. Okay. Well, you’re available tonight too?
Patrik: I am.
Eliza: I just want to.
Patrik: Yeah, absolutely. Absolutely.
Eliza: Okay. I’m going to go discuss this with them and I’ll be sure and call you back.
Patrik: Okay. I will send you the options now in an email.
Eliza: Okay, please.
Patrik: Okay. Thank you so much Eliza. Thank you. Bye bye.
Eliza: All right bye.
“This is the last part of consultation with ELIZA. Thank you very much for being a part of the previous series of 1:1 consulting and advocacy sessions. We hope you find our upcoming episodes informative and empowering also.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



