Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the first question from Paula in last week’s episode was
SEEMS LIKE THE ICU DOCTORS WANT TO PUT MY DAUGHTER TO DNR! CAN THEY DO THAT WITHOUT MY CONSENT?
You can check out last week’s question by clicking on the link here.
In this week’s two-part episode of “YOUR QUESTIONS ANSWERED“, I want to answer the questions from one my clients ELIZA as part of my 1:1 consulting and advocacy service!
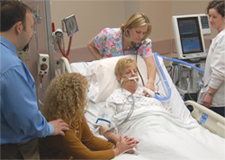
Eliza has her mother transferred in the Intensive Care Unit due to Liver Failure. Her mother was eventually diagnosed with Renal Failure treated with dialysis. Additionally, she had fluid in her lungs and was put in a ventilator.
The doctors in the ICU are urging us to sign a DNR form. What can I do to turn this around?
Eliza: Hello?
Patrik: Hi, is this Eliza (Affirming)?
Eliza: Uh huh.
Patrik: Hi Ashley, it’s Patrick here from https://intensivecarehotline.com/ How are you?
Eliza: I’m okay, how are you?
Patrik: Very good, thank you. So this is really to help you with your situation. You have a family member in intensive care, is that correct?
Eliza: Yeah.
Patrik: I just want to listen, I just want to listen to what your situation is and then I can advise you how I can help you.
Eliza: Okay. Well the situation is, my mother is in ICU. She has cirrhosis of the liver.
Patrik: Right, right.
Eliza: And she’s had that, well, she was diagnosed about a year and a half ago.
Patrik: Right.
Eliza: She’s just had some severe edemas.
Patrik: Right.
Eliza: Once the doctor had seen the edema, he sent her straight to the ER. And they took her to another ICU and she had fluid in her lungs. And then they said of course the kidneys are starting to fail, so they put her on dialysis. Then they tried to do a tracheostomy but she kept bleeding so they took the trache out.
Find more recommended information about tracheostomy:
Patrik: Yup.
Eliza: Yeah. And now they’re saying there’s nothing else they can do.
Patrik: Right, right.
Eliza: Her vitals and stuff seem to be good. It’s just, I’m not sure what to do. I’ve seen a ventilator, but not a “real” ventilator.
Patrik: Yeah, yeah. Absolutely. Tell me a few time lines. How many days has she been in ICU for?
Eliza: She’s been in the ICU since the 10th, so 19 days ago.
Patrik: Okay. Right. And she was ventilated from day one?
Eliza: Yes.
Patrik: Okay.
Eliza: When she went to the ER, she was fine. The second day she was in the ER, she started having trouble breathing. The third day, they sent her to a different hospital. She went to ICU. They put her on the ventilator immediately.
Patrik: Right. Okay. How old is your mom?
Eliza: 55.
Patrik: Oh my goodness. That’s very young. Oh my goodness okay. How much research have you done in terms of, is this the first time you’ve come across our website? Have you subscribed to our free newsletter? How much research have you done to this point?
Eliza: I’ve used Google. I’ve just been Googling.
Patrik: Right, right.
Eliza: So I’ve been looking at this for about a few days now.
Patrik: A few days.
Eliza: Because they’re saying there’s nothing else they can do.
Recommended:
Patrik: Yeah, yeah.
Eliza: So they’re making us make a decision.
Patrik: Yeah.
Eliza: But they said either they’re going to take her off, or we have to decide when to take her off.
Patrik: Right, right. And I’ll come to that in a moment. Are you the medical power of attorney?
Eliza: I’m not the TOA (Transfer of Authority), but I’m the oldest daughter, so I’m the one making all the choices.
Patrik: Okay. Yeah. No, no, that’s fine. Now, irrespective of what you said right now, that they would make a decision to take her off or you would potentially make a decision to take her off, let me ask you another question. What is the ideal outcome you would like? No matter what people say, what is the ideal outcome you would like for your mom?
Eliza: The outcome, of course I would … they told me that the most that she, if things were to turn around, she could possibly live another 90 days. I would be grateful for that, but not if she’s on a ventilator.
Patrik: Right.
Eliza: But they’re basically making us. Either they’re going to take her off today, or we have to take her off.
Patrik: Right.
Eliza: By tomorrow.
Patrik: Right. Are you … right. Have you heard of the term DNR (Do Not Resuscitate)?
Recommended information and related article about DNR/NFR:
Eliza: Yeah, they also keep bringing that up.
Patrik: Okay.
Eliza: Do not resuscitate.
Patrik: Okay. Has that been agreed upon?
Eliza: No. They want us to do the DNR.
Patrik: But you have not.
Eliza: But she wasn’t for code.
Patrik: Okay. And you have not agreed to that?
Eliza: No.
Patrik: Okay. You know what it means? Like, if somebody is on-
Eliza: Right. Go ahead.
Patrik: Basically what it means is, if your mother’s heart was to stop today, they would not do CPR. That’s basically what it means. But you are saying there is no DNR in place? That’s what you are saying.
Eliza: Right.
Patrik: Okay, okay. Yeah, okay. Do you feel like, to this point, they’ve done everything within their power?
Eliza: What?
Patrik: Do you feel like, up to this point, the ICU team has done everything within their power to help your mom? Or do you feel like they haven’t tried everything that’s available to them? What’s your feeling around that?
Eliza: I just feel that it’s not enough time because she keeps having these different procedures that’s making her weak and they keep making the argument that she’s not being respondent, but she’s moves around and tries to open her eyes, but then she’ll get sedated for another surgery.
Related information that empowers you as a relative of an ICU patient:
Patrik: What type of surgery? What surgeries did she-
Eliza: Well, first they went down in her lungs-
Patrik: Oh, a bronchoscopy. Yeah.
Eliza: Then, they put the trache in.
Patrik: Oh, so she’s got-
Eliza: Then they took the trache out.
Patrik: Yeah, yeah, because she was bleeding.
Eliza: Right.
Patrik: Is she getting blood products?
Eliza: I know she’s had one transfusion.
Patrik: Right. Just one?
Eliza: Mm-hmm (affirming).
Patrik: Okay. Do you feel, at the moment, do you feel under pressure in making a decision? Do you feel under pressure?
Eliza: Definitely.
Recommended:
Patrik: Okay, okay. Okay. The reason why I asked a moment ago, what’s the ideal outcome, no matter what the situation looks like at the moment, you should always look at the ideal outcome. Now why is this important? It is important because yes, your mother is very sick. There’s no doubt about that, especially now that you’re saying to me she’s moving right.
Is she, for example, opening eyes?
Eliza: She has opened her eyes all the way three times. But lately, she’s been trying. You can see her blinking. When we talk to her, she’ll start blinking and moving. But, she opened them once again today for the third time.
Patrik: Okay. If you grab your mother’s hand and you ask her to squeeze your hand, would she do that?
Eliza: No. She squeezed it on her own, but not when we asked her to.
Patrik: Okay. Okay. But she’s definitely moving her arms and probably also her feet.
Eliza: Yeah. She’s moved her feet once that we know of, but she will move her arms up and then they’ll go back down.
Patrik: Right, right.
GLASCOW COMA SCALE
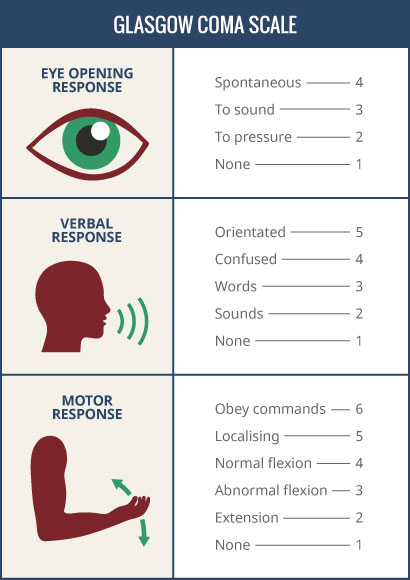
Eliza: I don’t know if she’s reaching maybe for the tube or what, but she’s definitely moving her arms.
Patrik: Okay. What about, do you know whether at the moment, she is in an induced coma? Do you know whether she’s on any medications that’s keeping her asleep?
Eliza: Well, they say when they sedate her, because of her liver issues, it’s going to take longer for her to get up.
Patrik: Correct. I agree with that. But, the question still remains, do you know whether she’s getting anything at the moment or not?
Eliza: If she’s getting sedated? I think they are not as of yesterday.
Patrik: Are not.
Eliza: It’s on and off.
Patrik: Right, right. So basically what you’re then suggesting is, your mother is not awake and that is a natural coma then because she’s not on any sedation. It’s a natural situation at the moment.
Recommended:
- 1:1 phone and email counselling and consulting with Patrik
- Join our Membership for families in Intensive Care INTENSIVECARESUPPORT.ORG
Eliza: Right, because of the liver.
Patrik: Yeah, because of the liver. No, no that makes sense. Okay. So then the next question is, has a liver transplant been mentioned for example?
Eliza: Has what been mentioned?
Patrik: A liver transplant?
Eliza: They said that she can’t get it because of her kidneys.
Patrik: Hmm. The kidney failure, is that new? Has that only happened since she’s been in ICU or was the kidney failure a condition that existed before ICU admission?
Eliza: It happened when she was in ICU three months ago, but they said it was going towards kidney failure, but they ended up, I don’t know the word, restoring, but it didn’t get to the point of dialysis.
Patrik: Okay. As of now, is your mother on the dialysis machine? At the moment, is she on the dialysis machine?
Eliza: No.
Patrik: No, she’s not. And why have they stopped it?
Eliza: They took her off about the same day they took the trache out. They said it was possibly making her sicker.
Patrik: How many days ago was that again with the trache? How many days ago?
Eliza: Two days ago.
Find more information about dialysis:
Patrik: Two days ago. Okay. Right. Have you discussed a situation like that with your mother before, like if it ever came to this point what she would want?
Eliza: No.
Patrik: No. It hasn’t been a point of discussion.
Eliza: No.
Patrik: Okay. That’s okay. Look, what we can definitely do, from our end is, you seem to have a very good basic understanding of what’s happening there. But let me ask you another question, then we’ll talk briefly about liver transplant, but has liver transplant ever been a point of discussion before this ICU admission? Has that ever been explored as an option?
Eliza: I asked her doctor last time she was in ICU and he said that she was not to that point. But I guess you have to be so sick to get one and she wasn’t there yet.
Patrik: Right. Now she decompensated very quickly.
Eliza: Right. And she was just fine. She just went because she had the swelling.
Patrik: Yeah, yeah.
Eliza: Edema.
Patrik: No, understood. Who is the primary decision maker at the moment? Is the ICU?
Eliza: It’s me.
Patrik: Sorry?
Eliza: It’s me.
Patrik: Yeah, no, no. I understand that. Who’s the primary decision maker on a medical level? Who’s in charge of the medical care at the moment? Is it an intensive care doctor? Is it a liver specialist?
Eliza: It’s … I’m thinking it’s the ICU doctor, but they all … he said that they’re all agreeing that there’s nothing else that they can do.
Patrik: Right.
Eliza: But they didn’t start saying that until she couldn’t get the trache. I feel like they don’t want people on the ventilator long.
Patrik: Yeah.
Eliza: I almost feel like they’re kicking us out, making us pull the plug on her.
Patrik: Yeah. Well, I tell you what, if you had contacted me four days ago with the situation, I would have told you the trache, if she could have tolerated the trache and she wouldn’t have bled, they probably would have tried to ship her out to a long term acute care. Do you know what I mean by that?
Recommended:
Eliza: Mm-hmm (affirming).
Patrik: Right. Was that part of their plan when they were doing the trache? Was that part of?
Eliza: Yes.
Look out for the next consulting and advocacy session with Eliza, next week!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!