Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
HOW TO ASSESS GLASGOW COMA SCALE (GCS) IN ADULTS AND CHILDREN?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Peter, as part of my 1:1 consulting and advocacy service! Peter’s mom is in ICU with a tracheostomy and he declined the DNR order of the ICU team. Peter is asking if he needs to worry about the repercussion of his decision.
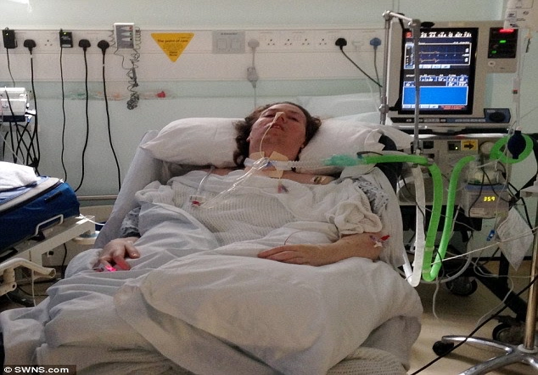
My Mom is in ICU with a Tracheostomy and I declined the DNR order of the ICU Team. Should I Worry about the Repercussion of my Decision?
Patrik: Hi, it’s Patrik from intensive care hotline.
Peter: Hi Patrik. This is Peter. How are you?
Patrik: I’m well and you?
Peter: Good.
RECOMMENDED:
Patrik: Anyway, can you tell me again why your mom is in ICU?
Peter: Ok. Firstly, I really appreciate the information you have in intensivecarehotline.com and for being an advocate for us families in intensive care. I find your website really helpful in giving us information with the best possible approach and how we can get control and power over the ICU team for the sake of our loved ones.
Patrik: Oh, thank you. I am more than happy to be of service.
Peter: Anyway, my mom has been admitted to ICU because primarily she complained of shortness of breath, which turned out that she had lots of fluids in her lungs according to the ER doctors. My mom’s diagnosed with stomach cancer actually. And one of the doctors is talking to her saying, “Well, this is not a good quality of life.” And my mom has said she wants to keep fighting, just that she’s lost-
Patrik: Right. Can I just ask a few questions for my own clarity so I can really help you the best way that I can? Are you the medical power of attorney for your mom?
Peter: My sister is. But we’re in agreement, we work hand in hand together.
Patrik: Okay. And I missed that bit, how long has your mom been in ICU now? Or you said she’s in and out but just-
Peter: About a month. Yeah, yeah. This most recent episode, about one month.
Patrik: About one month. And is she on a ventilator at the moment?
Peter: Yes, she’s on a ventilator.
Patrik: Oh okay, with a breathing tube in her mouth or with a tracheostomy?
Peter: A tracheostomy.
Patrik: Okay.
Peter: Just give a second. Hold on one second, sorry. I’m actually at the hospital, I just have to suction her. Two minutes and I’ll be right back.
RECOMMENDED:
Patrik: You have to suction her?
Peter: Yeah, the nurse is not here and her mouth is-
Patrik: That’s terrible.
Peter: Yeah. Hold on one second. I apologize. Hold on.
Peter: Sorry about that. I’m okay now. She’s fine.
Patrik: Yeah, sure. So are you telling me you are doing some of the work that the nurses should be doing? That’s terrible.
Peter: Yeah, the thing is, you know how it is, they’re in and out, they’re with other patients and they’re not going to be here 24/7.
Patrik: Well, on the one hand, I know how it is. I worked in intensive care for 20 years. On the other hand, I’m embarrassed as a nurse … I’m embarrassed.
Peter: Yeah, my girlfriend works at an ICU in Nashville Cancer Institute, one of the big ones in Tennessee here, so she’s given me one or two things. But I love to talk to you because she doesn’t know everything, she’s not as experienced as you. But yeah, the nurses are not always here, they have to be other patients in. I don’t want to be that annoying family member who’s-
Patrik: Well, I can tell you that if you want to get results for your mom you might have to become that annoying family member.
Peter: That’s why I reached out to you.
Patrik: Right, you know. But anyway, let’s just keep focusing on the clinical things for now so we can hopefully get a plan together. So she’s ventilated at the moment and is she ventilated with a tracheostomy?
Peter: Yes, sir. She’s got a tracheostomy. So she’s on the ventilator, she’s on a tracheostomy.
Patrik: Okay. And how long ago did they do that tracheostomy?
Peter: Tracheostomy was done … So we brought her in to the ER and when she came in through the ER they kept the intimidation tactics, they waited till she stopped breathing. Because what happened was she had a lot of fluid in her lungs and after we … I think it was done about a month ago, the thing was done about a month ago. The procedure, from the ER. We came into the ER and you know …
RECOMMENDED:
Patrik: And then they did the … Okay.
Peter: They did it.
Patrik: And what’s your biggest challenge at the moment? Is the biggest challenge that she’s not waking up, is the biggest challenges the-
Peter: No, she’s up. She’s very alert now actually. The thing is every time we come here she’s alert, she’s actually doing … If I walk through the hall and I go to the restroom she’s doing way better, and I don’t mean this in a bad way, she’s doing way better than everybody else I see in a different room.
Patrik: Okay, good. No, that’s good, that’s important information to have. That’s very important information to have.
Patrik: But they, nevertheless, want to make your mom DNR, is that what they want to do?
Peter: Correct. Exactly. The doctor’s like well … The doctor tried to discourage her this morning, like well, you know, there’s nothing else we can do, there’s nothing else we can do, this is not a good quality of life, try to talk to her about the quality of life and stuff. And you know, this is not a good quality of life.
RECOMMENDED:
Patrik: He’s trying to talk to her about quality of life, is that what you’re saying?
Peter: Exactly. He’s trying to talk to her about quality of life and say, well there’s nothing else we can do.
Patrik: Yeah, stop him from doing that. Stop him from doing that. Tell him off. That’s what I’m saying, you may have to become that annoying family member.
Peter: Yes, and I’m willing to do that. And you know the funny thing about this hospital is, I can even give you the name on Skype. This is not the first time. When we came here before, I think it’s their culture, some nurses were trying to … We’re not abusing my mom, my mom has said she wants to fight. Some nurses were trying to convince my mom to … Like manipulative tactics. Like saying stuff like, you know, I hope, you know … Pretty much insinuating that the family is keeping her here outside her will. And I attended one of the meetings and the meeting was like, they’re like well she’s pretty much trying to insinuate she wants to go to hospice and me kind of shut them up, I’m like no, that’s not true, my mom has said she wants to fight, and I have to speak up. Now that I spoke up after that meeting the charge nurse was like, yeah, you did the right thing. Because again, they’re trying to force our hand and play … The doctor came in this morning and played… Sorry, I hope I’m not rambling. Long story short. Just tried to tell her, this is not a good quality of life, you’re never going to walk again, you’re never going to-
Patrik: Stop them. Yeah, stop them from doing that. You are not in control of what they do but you are in control of how you respond. And your response to that is stopping it. It’s as simple as that. Don’t blame what other people do, but take responsibility for your response.
RECOMMENDED:
Peter: Right.
Patrik: Right. That’s why I’m … We can blame the weather all day long, we can blame other people all day long for things that happen or don’t happen in our lives, it doesn’t matter. All that matters is your response. You need to take 100% responsibility for your response and your response is, “stop it.” It’s as simple as that. End of story. There’s no … That’s why I’m saying, you may have to become that nagging family member. You may have to.
Peter: Could that backfire to where they like … Because right now she’s on some antibiotics because she has an infection and her white blood cells at 16. Can that backfire to where if I tell them-
Patrik: Yeah, you’re worried about repercussions.
Peter: Yeah. As an example, they could be selective about the type of antibiotic they give her, they could play some type of tactic to where, you know …
Patrik: Of course. And that’s a valid question. I guess that’s where I could come in in terms of guiding you and making sure they are doing the right things. That’s part of what we do in terms of advocacy and consulting. The other thing that I can tell you from experience, if you become that annoying family member they will be rolling their eyes, don’t get me wrong, I’m not saying it’s going to be easy, that’s not what I’m saying. They will be rolling their eyes, but I can tell you from experience if you are persistent in your message, it will stop eventually. It’ll stop eventually and at first, they will probably say, oh, what are you on all about and they will roll their eyes, but it doesn’t matter really. Again, I think it’s a general problem in life, far too concerned about what other people think about us. I think that’s a general problem in life from my perspective and often we shouldn’t give a toss about what other people think.
Peter: Absolutely.
Patrik: This is about your mom. It’s not about what they’re thinking … Look, and this is one of the reasons why I’m doing what I’m doing. What you’re describing in terms of what the doctors say, what the nurses say. I was in the system myself and I was sick of it and that’s one of the reasons why I’m doing what I’m doing. Because I didn’t want to be part of that. I just didn’t. And the culture in ICU across the board, it’s not unique to your hospital there. It’s just the way you are describing it and the way I describe it on my blog. There are some good ones out there, don’t get me wrong, but they’re far and few in between.
Peter: Why do you do that? It’s like you’re here to save people’s lives, but then they intimidate you. You know.
Patrik: That’s exactly right. What’s the purpose of being a doctor, being a nurse, if your work is that … What’s the word? Is that ingrained in the politics and in the hospital system? That’s basically dictating how people should behave. It’s just, unfortunately, the industry has become like … What’s the word? It’s like an assembly line now. People come in, you tick certain boxes and if they don’t get better, throw them out … And if they don’t get better in a time that’s a convenience for the ICU we kick them out on the other end by doing things like DNR or by withdrawing life support. It’s terrible.
RECOMMENDED:
Peter: So what are we doing here? Is it possible to get a ventilator, because we want to leave this environment? Is it possible to get her with a ventilator and the LTAC but in a skilled nursing facility? Is there a ventilator in a skilled nursing facility?
Patrik: Potentially. So what are the options besides basically a DNR have they given you? Have they given you any other options?
Peter: No other options. They say she’s not getting better and that’s it. So we want to leave this environment.
Patrik: Right, right. How much research have you done … The reason I’m asking this is most families, when they come to us in a situation like that their problem is either the end of life issue, what your problem is at the moment in terms of DNR or, on the other hand, the other issue they’re facing often is that the ICU wants to send their family member to LTAC or to a skilled nursing facility. So that has not been an option?
Peter: I don’t know if the insurance approved or not. I’ll have to ask the social worker on Monday. I know we’re looking at … The thing is she’s on a ventilator. So I don’t know if … They were trying to get out the ventilator today but her Arterial Blood Gases wasn’t good. So I don’t know if they’re going to be able to send her on a ventilator to an LTAC or a skilled nursing facility because I don’t think the insurance approved for an LTAC but I think insurance may approve for a skilled nursing facility. The challenge is, in a skilled nursing facility, do they have a ventilator, which I don’t think they do.
Patrik: Yeah, yeah. Look, either one, skilled nursing facility or LTAC is pretty challenging for a ventilated patient. I’m not recommending LTAC or skilled nursing facility but what I am saying is, in a situation like that, nine times out of 10. I actually see ICUs trying to push patients to LTAC or a skilled nursing facility. That’s why I’m a little bit surprised to hear that-
RECOMMENDED:
Peter: They are. Usually, they are but it sounds like with the doctor’s speech this morning, we didn’t appreciate that as a family.
Patrik: Yeah, of course. How old is your mom?
Peter: 63.
Patrik: That’s very young.
Peter: Yeah.
Patrik: That’s very young. Okay. So the first advice that I can give you is do not give in. Just ignore and tell them to stop talking about the things that you don’t want to talk about. That’s the first thing. The other thing that I would like to know is if I was to see a picture of your moms ventilator if I was to see a monitor of your moms monitor if I was to see a gas result for example, if I was to see some blood results, you mentioned white cell counts and whatnot, I can give you a better understanding of where your mom is at, I can give you a better understanding of how close, for example, is your mom to be coming off the ventilator. So it’s one thing to say oh, she won’t have any quality of life, she won’t come off the ventilator, but it’s another thing to verify that.
Peter: Yes, I can send that to you.
Patrik: Right, right. Because the reason I’m saying that is, let’s just say your mom is in a ventilation mode that is close to her coming off the ventilator. That would give you a very … That would give you a strong argument for not doing a DNR, for example. It would also give you a strong argument for continuing treatment. Because I can’t … Your biggest challenge or the biggest challenge for families in intensive care in a situation like that is that you simply don’t know what you don’t know. That’s your biggest challenge. And it sounds to me like you’ve done a lot of research already, however, the nitty-gritty is in the detail. The devil is in the detail. And for example, if your mom is breathing in a ventilation mode where she could come off the ventilator, well, maybe they just need to wean her off for another week and then she’s off the ventilator. That would take one layer of complexity away.
RECOMMENDED:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Peter: Yeah.
Patrik: Has anybody mentioned that your mom could come off the ventilator or is close to coming off.
Peter: Yes, they tried this morning. She was just on the ventilator two days ago. They tried to take her off today but she didn’t do good as far as results. So they made an attempt to take her off and we were like wow, they’re taking her off so quickly. But then they put her back on because she didn’t do well.
Patrik: Okay, and was that the first time they’ve done that?
Peter: This is the second time. They tried yesterday and then they tried today.
RECOMMENDED:
Patrik: And within that four week cycle since she had the tracheostomy she’s never been off the ventilator not even for five minutes?
Peter: Oh she was. She got off. So what happened was she’s back in the ICU. She came into the ICU, got off the ventilator, did well, went to-
Patrik: Sorry, you’re dropping out.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
Related Articles:
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care