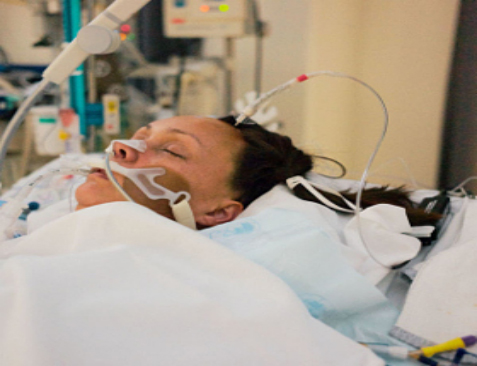
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Mom Died in ICU Because of Medical Negligence. Can I File Criminal Charges to the ICU Team?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Bea, as part of my 1:1 consulting and advocacy service! Bea’s mom died in ICU because of the ICU team’s medical negligence and Bea is asking why the ICU team is withholding clinical information in her mom’s medical record?
My Mom Died in ICU Because of Medical Negligence. Why Does the ICU Team Withhold Information in my Mom’s Medical Record?
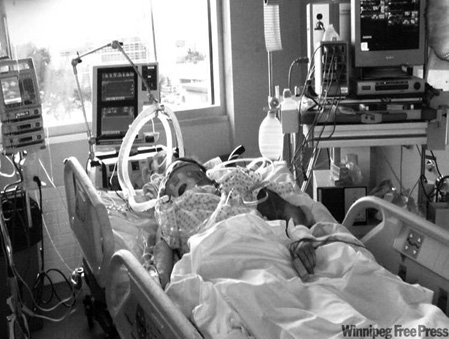
“You can also check out previous 1:1 consulting and advocacy sessions with me and Bea here.”
Patrik: Never? Right. What time of the day did your mother pass away? Daytime? Nighttime?
Bea: Daytime.
Patrik: Oh Daytime, okay. Were you there at the time or were you absent?
Bea: Sorry but I can barely hear you.
Patrik: Oh sorry. What I’ll do is you need to give me about half an hour. You need to give me about half an hour and I’ll call you right back. I’m sorry. I’ll call you right back in about half an hour, three quarters of an hour.
Bea: Ok.
Patrik: I’m sorry. I’ll call you right back. Thanks, thanks. Bye.
RECOMMENDED:
Bea: Hello.
Patrik: Hi Bea. It’s Patrik here from-
Bea: Hey.
Patrik: Hi.
Bea: Okay, hold on. Let me put my headphone on, okay?
Patrik: Yeah.
Bea: Okay. Now, is it okay?
Patrik: Now, I’m back inside. Sorry, I had to run some errands that I couldn’t postpone. Keep in mind, for me it’s 1:00 PM, so it’s all good.
Bea: Yeah.
Patrik: Now, I’ve got about another three-quarters of an hour now and then we can see where we’re going from here. Now, just to quickly summarize from my perspective, right? There have been no surprises. I’ve seen these similar situations over and over again. I know for you this is absolutely outrageous, and it is outrageous, don’t get me wrong.
Patrik: But I have seen those situations over and over again. It’s great that somebody within the hospital is doing some of the work for you already. That’s remarkable, that’s fantastic. Where I think we can help down the line, once I understand your situation 100%, is really a review in medical records. That’s where we can help because we could take this to medical negligence and potentially a murder claim.
RECOMMENDED:
Bea: Yes.
Patrik: Right? And-
Bea: We didn’t like to do a lawsuit first because-
Patrik: Yeah, sure. Yeah, yeah, sure but yeah.
Bea: Let me tell you, let me tell you. The nurse I told you about, had gone to a homicide detective. The detective was asking her, “Where are the family members?” Because I did not file any police report yet. Then I would press charges against certain people.
Patrik: Yeah. But, you see, you can only probably press those charges once you had a good look at the medical records.
Bea: Right.
Patrik: Right? So, what do I mean by that? I’ll give you an example, right? To illustrate that for you. So, for example, many years ago … Well not many, probably about five years ago, I was in a similar situation in ICU when I was a clinician, right? The doctors asked me to stop life support on a patient, okay? And I refused, okay?
Patrik: So, the reason I refused, not only on moral and ethical grounds but also I said to them, “Look, the family’s not agreeing with stopping life support. If I stop life support, I might get sued by the family.”
RECOMMENDED:
Bea: Oh. So, the family actually can sue the nurse who unplugged that?
Patrik: No, no. The doctors asked me to pull the plug. The doctors. And I refused because I knew the family wasn’t ready for that. And I said to the hospital at the time, “Well, I’m not doing that. You can send somebody else to do that, but I’m not doing it because I’m not killing somebody. That could be murder.”
Bea: Yes.
Patrik: Right? So, what I think, one of your missing links at the moment is to find out who were the people who were actually following the orders? That’s one of your missing links. And you will get that from the medical records.
RECOMMENDED:
Bea: Yes. But I do know some people. I know that nurse who was on duty.
Patrik: Yeah, yeah. Yeah, but you have to get the full medical records. It sounds to me like you’ve only got a small amount of what you need.
Bea: Yeah. So, I think the medical record, I’m going to wait until the attorney going to order it, probably next week.
Patrik: Okay. But keep in mind … You see, it’s good that you’ve got an attorney involved but an attorney is not a medical specialist. They can’t review your medical records to the extent that we could review them because we are clinicians.
Bea: They need to hire somebody who does.
Patrik: That’s right, but they need to hire somebody like us who knows intensive care inside out. We’re constantly reviewing medical records as part of lawsuits.
Bea: Yeah, that’s why we might hire you. I will tell him about you.
Patrik: Yeah. Because we do that. That’s part of the services we provide.
Bea: Yeah, that’s great. I will pay for you to review it for me as an extra. Because you’re not in the Texas. I wish you are here.
Patrik: That’s all right but doesn’t matter because intensive care, as far as I’m concerned, it’s the same everywhere. Yes, the funding is slightly different in the different countries, but the politics and the drugs given, it’s all the same. All the same.
Bea: By the way, regardless, I think I would like to have you look at the record-
RECOMMENDED:
Patrik: I think it’s inevitable.
Bea: I would like to. Because when you read the record, you will be able to give me very knowledgeable feedback and notation.
Patrik: Absolutely.
Bea: Even the part that this, they’re trying to evil painting me, you will be able to find that and unplug some items. I definitely would do that.
Patrik: Yeah. It’s not that many medical records. We’ve reviewed months’ worth of medical records in ICU. You’ve got three days’ worth, so we could do that fairly quickly.
Bea: Well, here’s the thing, I don’t have the ICU portion of it. I never got that part because that was not even in the record when I requested. What I have is mostly from the day she was accepted until the day she was put in the ICU.
Patrik: Yeah. It sounds like they are withholding critical information. That’s what it sounds like to me.
Bea: So, what I have is that portion, but those portions not even including the nurse record. Because they monitored. Every day they put in new notes in there.
Patrik: Right, right. You see-
Bea: I don’t have that.
Patrik: Yeah. Do you think they know that you’ll potentially file a lawsuit? They know that, and that’s why they’re withholding critical information. They want to-
RECOMMENDED:
Bea: I don’t think they knew. I think they’re very afraid, fearful, of that nurse-
Patrik: Oh, they would be.
Bea: Because she got all over the place without me because she could not find me.
Patrik: Absolutely.
Bea: And so far, it has been like eight months passed. I am not making any complaints. I have not filed a lawsuit. I haven’t done anything. I think they probably very easy on that part. I think-
Patrik: Right, right.
Bea: I haven’t even make a complaint to some of the nurses and doctors I will. Which is I am right now doing it. Just before talking to you, I’m actually seeing a complaint that my lawyer provided to me to the Department of Public Health.
Patrik: Yeah.
Bea: Amanda thinks I need to do that, so I have. I thought it was very interesting. They have a summary here. I think it’s very proper. It says my mother had pulmonary edema, needed oxygen when she was in the hospital. But on such, such day, she would lay flat in her bed not getting oxygen for four hours over before she went into cardiac arrest.
Bea: This was all witnessed by an assistant nurse who has agreed to speak to the Department of Public Health.
Patrik: Right.
Bea: The nurse repeatedly told the station on duty that my mother’s nasal cannula was off and she needed oxygen. But they ignored her and for whatever reason, did not get my mother oxygen or check on her. My mother was really well but declared brain dead later.
RECOMMENDED:
Patrik: Right. Let me ask you another question. Have you heard of the term DNR?
Bea: No.
Patrik: Right. DNR stands-
Bea: What is DNR?
Patrik: Yeah, DNR. So, you know what I’m referring to that do not resuscitate.
Bea: Do not resuscitate, what’s that mean?
Patrik: Yeah. In case of a cardiac arrest, in case a heart stops, they would not resuscitate if a patient has been issued with a valid DNR do not resuscitate order. So, in case the heart stops, basically the hospital would be passive and let a patient die. So, my question to you is, do you know whether your mother had a DNR a do not resuscitate order? Do you know that?
Bea: I don’t know.
Patrik: Right? Was that ever a point of discussion while your mother was in the hospital or in ICU?
Bea: Nobody discussed that to me.
Patrik: Okay. And that’s why you need the medical records. I have the suspicion that your mother had the DNR, right? That you didn’t agree to, but they had on the records. And that could’ve been part of your mother’s death. It could have.
Patrik: I’m not saying it is, but there’s a high likelihood there is and you need to find out through the medical records.
Bea: So, meaning if they have the DNR they have to get approval from the family member?
Patrik: Very much so. But they often don’t. They often don’t, they just issue a DNR. They sort of mentioned while passing by to families, “Oh yeah, what do you want? If your mother’s heart stops? Do you want us to jump on her chest? Crack her ribs?” So, they really paint a negative picture, to begin with without actually properly consenting you what it means and what you want and all of that.
Bea: Okay.
Patrik: It’s a good chance that they said it. So, that’s why the medical records would be crucial for you. How long ago did you get the records that you have now? How long ago did you get them? Just recently, or?
Bea: I got it in November.
Patrik: Oh, oh so, right at the time?
Bea: I got it on 22nd, right after they put her out. So, there are some notes not even there.
Patrik: Yeah, yeah. There’s notes missing. There’s notes missing.
RECOMMENDED:
Bea: Let me take a look. I have the record right here. I want to take a look at that part. See if actually have something regarding DNR.
Patrik: Have a look.
Bea: Okay, so it would be the one that. . I even have that. I have those things that they actually punch in the computer but not the notes. But I have the patient … Even on November 21, that’s the day before.
Patrik: It would be extremely-
Bea: What we have here, they have a lab test looking pretty good. Albumin is 100. Okay, I want to question before I forget.
Patrik: Yeah, yeah.
Bea: My mother needing dialysis. But she was supposed to be due on the 19th and had an order on it. But she was already dead and sent to ICU. We gained blood pressure, but slowly. Her body was so cold, she is not even sure she’s recovered or not.
Bea: Now, the technician came in, insist that the doctor order perform the dialysis on my mother. I refused. I told him, “I can’t believe you’re doing that. This patient is dead. Just gained conscious within an hour. You can’t do any dialysis on her. You may put her heart in triple danger.” So, I tried very hard to stop them when she’s dead.
Bea: But they put record and they indicate I was trying to stop them from performing dialysis on her.
Patrik: So, they are-
Bea: That’s very crucial.
Patrik: They are accusing you, is that what you’re saying?
Bea: Oh, yes.
Patrik: Right.
Bea: They are accusing me that I did not allow them to put to do dialysis on her. That’s ridiculous.
Patrik: Well, I’ll tell you what then, if that was documented that they’re blaming you for not allowing them to do dialysis. Then there is a sense that your mother didn’t have a DNR. Because sometimes the DNR includes not doing dialysis.
RECOMMENDED:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: So, that almost to me says she may not have had a DNR. What I don’t understand, if they said your mother was brain dead, why was she brain dead? Where was the brain damage? Why did she have brain damage potentially? Can you-
Bea: Because on the … Okay. Now let’s see this. The results of November 21st. He has a treatment and saw some diagnosis, assessment, and plan. It says first of all, what number one is pulmonary edema. Acute hypo … What? H-Y-P-O-X-I-C?
Patrik: Do you know, do you remember whether you, do you remember whether your mother had a chest drain?
Bea: She had a chest x-ray, yes.
Patrik: No, no, no, a chest drain. A drain in her chest. Do you remember that?
Bea: No. She had no drain.
Patrik: Right? Okay. I’m not making any sense at the moment out of this. But you know-
Bea: Yes.
Patrik: How many pages of medical records do you have at the moment?
Bea: Probably I would say maybe 70.
Patrik: 70?
Bea: Do you want me to mail you them?
RECOMMENDED:
Patrik: Yeah. You know what you can do if you can … So, you have them in paper form?
Bea: I can mail it to you.
Patrik: Yeah. You know what you can do, no, no much easier. Take pictures with your mobile phone and email them to me.
Bea: That’s too much. Too many.
Patrik: Well, I look, I don’t know. I take pictures all the time of records and stuff.
Bea: That’s way too many pages. Too many. Too many.
RECOMMENDED:
Patrik: Okay, all right. Up to you. Up to you.
Bea: But here’s the thing. I don’t understand this, acute respiratory failure. You probably when you see it you know.
Patrik: I would have to see, that’s all right. Carry on, carry on.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!