Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Do We Know If Our Mom Is Ready For A Tracheostomy In ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Robert as part of my 1:1 consulting and advocacy service! Robert’s wife is in LTAC with a tracheostomy and Robert is asking if Intensive Care at Home can help his wife go home.
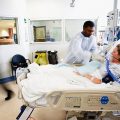
I Am Not Happy with How They Treat My Wife with a Tracheostomy in LTAC. Can Intensive Care at Home Help in Getting My Wife Home?
Patrik: Hi, Robert. How are you?
Robert: Hi! Oh, I’m hanging in there. How are you doing, Patrik?
Patrik: Very well, thank you. Can you hear me?
Robert: Yes. Can you see me?
Patrik: I can hear you, but I can’t see you.
Robert: Weird. Let’s see … Oh, “Start video”. That will help. There we go.
Patrik: That’s better.
Robert: I’m sorry, I didn’t hear what you said. It was crossing.
RECOMMENDED:
Patrik: I said, you’re okay?
Robert: Not really, but I’m trying my best.
Patrik: Yeah. No, absolutely. So your wife’s in LTAC at the moment? Or in intensive care?
Robert: She is in LTAC. I’m not very happy with her treatment there, but especially that they’re not allowing visitors. And she’s having delirium and depressed and I just feel like the not having visitors is making it worse.
Patrik: Oh, it’s terrible! Unfortunately, I’m having these calls every day now.
Robert: Really?
Patrik: People are being locked out of LTAC, out of … It’s horrible. It’s difficult if people can visit, let alone, if they’re locked out. It’s just terrible. Just tell me a little bit, how long has been the whole path from where it started to this point? How many weeks, months?
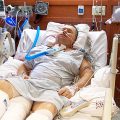
Robert: So she went in about couple of months ago with COVID and then they put her on BiPAP machine. She was on that for two days, and then they intubated her. She was on the ventilator for a week and they really quickly took off her sedatives, really quickly weaned her. And then they ended up taking it out and had to reintubate her, which is worse. And then they put in a tracheostomy tube. My days are all a mess now, but I would guess it’s been about 10 days or so that she’s had trach.
Patrik: As soon as she had the trach, they will try to-
Robert: Probably more than that now. Probably two weeks, because … I’m sorry?
Patrik: As soon as they’ve done the trach, they were sending her out to LTAC?
Robert: Yes.
Patrik: Did you see that coming? Did you know about that? Or did that come out of the blue?
Robert: No, I was told that the trachs were a good way, because that they’re more mobile. If they can allow them to do these breathing trials.
Recommended:
Patrik: If you had to come to me-
Robert: And I’m reading that they’ve had good success with trach.
Patrik: Okay. Oh yeah, trach. I’m not opposed to a trach. What I am opposed to is LTAC, because LTAC is just … Unfortunately, LTAC is a better version of a nursing home.
Robert: Okay.
Patrik: Right? If you had come to me at the point of trach, I would have said, yeah, probably trach, but no to LTAC.
Robert: Interesting. They said that they wouldn’t keep her at the hospital.
Patrik: Look, everything in life is negotiable. Right? We strongly advise against LTAC for a variety of reasons. But LTAC is designed to save money for the health insurances.
Robert: Right.
Suggested links:
Patrik: It’s not about clinical need. How old is your wife?
Robert: 60.
Patrik: And otherwise, previously fit and healthy?
Robert: She has a little bit of asthma, but it’s well-controlled.
Patrik: Okay. Are you the medical power of attorney for your wife?
Robert: We don’t have one. I mean, I’m the insurance person.
Patrik: Have given consent for a trach? Have you signed for a trach?
Robert: I did.
Patrik: Yeah. So you are more or less the medical power of attorney. If they asked you for a signature for the trach … If nobody else agreed to it but yourself, then you must be the medical power of attorney for now.
Robert: They didn’t ask me to sign anything, but they called me and asked me my permission. They had to get somebody else on the line.
Patrik: Yeah, sure. But you had to give verbal consent?
Robert: I did.
Patrik: Yeah. Is there an advanced care directive for your wife?
Robert: No.
Patrik: Okay. But, but you think at this particular point in time she wants everything done?
Robert: I think so, definitely, because she can still get out. Not if she’s going to be insane or mental, like not be with-it. She wouldn’t want that. But otherwise-
Recommended links:
Patrik: Right. Yeah, okay. Are you having face time with her? Can you talk to her?
Robert: A little bit. I talked to the CEO of the LTAC and I was complaining about it, and he said he could maybe try to set it up for twice a day. Of course my wife can’t communicate, other than nod.
Patrik: But she’s awake.
Robert: She’s having ICU delirium and she’s getting agitated.
Patrik: Right.
Robert: She is awake.
Patrik: She is awake. Okay. Look, I know your initial inquiry was-
Robert: Can I get her out of the LTAC?
Patrik: I’m coming to that. I was just about to talk about that. So I know your initial conversation was around intensive care at home. Right? And whilst I can’t help you in your area, but I can certainly share some insights. Intensive care at home is great for the right patient, at the right time. What I don’t know at the moment is, is your wife the right patient? Is it the right time? The reason I bring this up … It all sounds great and, again, we are in this business, but taking your wife home on a ventilator, all doable. It’s all doable, right? But what if your wife is two weeks away from coming off the ventilator, going home without a ventilator? So much easier.
Suggested links:
Robert: Right.
Patrik: Right? So those are all the questions that need to be asked. Questions need to be asked.
Robert: They don’t know. They just say it’s different for everybody. So how would I know?
Patrik: I agree. It is different for everybody. How do you get updates for your wife? Who’s updating you about his condition?
Robert: I have to call the nurse and bug her to talk to me.
Patrik: So, there’s no-one calling you unless you …
Robert: Yep. I asked for the doctor to call me once a day and she has done that, but the nurses, no. I have to call them.
Patrik: So the doctor is calling you once a day?
Robert: Yes. But she doesn’t know much. I asked the doctor like, did my wife do breathing trials today?” And she said, “Well, you’ll have to talk to the pulmonologist.” Like, “Well, the pulmonologist doesn’t call me!”
Patrik: Who is the doctor? What’s her title? Is she not a pulmonologist? Or-
Robert: No. She’s the internal medicine doctor there.
Patrik: Right. Okay. Anybody else talking to you there, like a social worker, case manager? No, nothing?
Robert: I talked with the case manager today, but all that they knew was, they were finding out do we have steps at our house and stuff like that. It doesn’t help me right now.
Suggested links:
Patrik: Sure. No, it doesn’t help you right now. No.
Robert: I spoke with the CEO, I tried to go to visitation in. And I’ve spoken with the charge nurse and I keep trying to advocate. They say that they’re in there all the time, but the nurse … I asked if I could talk with her and it was four-and-a-half hours later and she’s sitting there being depressed. It’s just awful for me.
Patrik: Yeah, of course. How many days ago did she go into LTAC?
Robert: On Wednesday. Few days ago.
Patrik: So, it’s basically days ago.
Robert: Yes.
Patrik: Okay. Is she COVID negative now?
Robert: I don’t know. They said that they thought it was out of a system. So does that mean … ?
Patrik: Yeah, she would be negative, then. Yeah. It would be negative. Okay. So here is how I can help you. Are you living near the city?
Robert: Yes.
Patrik: The reason I’m asking all of these questions is, the closer to the city, the easier it is to get support. Of course. Again, not-
Recommended:
Robert: I’m in a city.
Patrik: Sure. You can talk to nursing agencies in your area and they might be able to pull it off. But, again, the question is, if your wife was to stay another two weeks, another four weeks and she could come off the ventilator, her recovery would look so much different.
Robert: Right.
Patrik: Right? Intensive care at home is really for someone that either can’t come off a ventilator, at all, ever. Or someone that has failed to come off the ventilator, but it has a very good chance of coming off the ventilator eventually. Right? I can’t see that for your wife at the moment with what you’ve shared. It’s too early. I believe it’s too early to say she can’t come off the ventilator. Because if she could come off the ventilator, maybe another four weeks, LTAC is worth the time, you know? That is the questions you need to ask.
Robert: Right. I was thinking about, well, I could transport her to … If I could find another hospital, let’s say three or four hours away that would allow visitation, because there are some in our area that are allowing visitation. The problem is that she became so disoriented when they transferred her from the one to the other that I’m concerned that she’s going to be disoriented again. But right now she is disoriented. What are your thoughts on that?
Patrik: Yeah. That’s a great question, Robert. I don’t know how much research you’ve done. One of my arguments against LTAC is, a critically ill patient doesn’t need a change to another facility. They need consistency of care. And it’s one of my biggest arguments against LTAC. I can’t believe how a critically ill patient can have a care episode interrupted. That is one of the cruelest things I believe that someone can do. Right? You’re right on the-
Robert: I feel so bad I didn’t research this. Oh, God!
Patrik: Right. So, it’s unbelievable. And it’s all done because of money. A critically ill patient needs consistency of care. They need to be surrounded by a team that knows and gets to know the patient. And by going to LTAC, that’s a whole new team. The worst thing in LTAC is not only the disruption of the care episode, it’s also in intensive care you have intensive care nurses and respiratory therapists. You’re going to LTAC and you’re going to a level of care with no intensive care doctors, with no intensive care nurses. From my perspective and from my experience, Robert, that’s like flying an airplane with a cabin crew instead of the pilot.
Recommended:
Robert: She was in a step-down unit. They moved her to a step-down unit. But now I’m feeling so guilty. I-
Patrik: No, you shouldn’t. Look, people don’t know what they don’t know.
Robert: They told me at the hospital they wouldn’t keep her.
Patrik: Look, all hospitals are very good to pretend they operate in a vacuum. So, what I mean by that, if you had done your research and maybe we would have had this conversation two weeks ago, you would have said, “Hey, hang on guys. I have some questions here.” No, it is what it is. You got to deal with what’s given. Where I think I can help you to hopefully improve the situation at all is, I can get on a call with you, with the doctors and find out what’s exactly happening. How realistic is it for your wife to get off that ventilator in the next few weeks? What are they doing to achieve the goals? What are they not doing? I guess that’s where I can definitely help you. And then map out the steps.
Patrik: If your wife had been in LTAC for six months, I would say … and she can’t come off the ventilator, I’d say, yup, let’s look at the intensive care at home. Or let’s look at similar options in your area. Absolutely.
Robert: Right.
Patrik: But it’s too early.
Robert: Okay.
Patrik: Too early.
RECOMMENDED:
Robert: Well, I’m supposed to have a care meeting with them. And so I can certainly ask them. I certainly appreciate your help, but I think that I can certainly ask them those type of questions. Unless you think that you would have questions that I wouldn’t know.
Patrik: Yes. Very much so. But my first advice for families in a situation like that is, if you don’t know what questions to ask, they only tell you half of the story. When someone is in a situation like your wife, there are dozens of things happening simultaneously. I ask clients. I say, “Can you tell me what the ventilator settings are? Even better, can you send me a picture of the ventilator?” And at the moment that’s very difficult. And then they tell me, “Oh yeah, she’s on a 50%. And I say, “Okay, that’s great, but there’s 10 other numbers that are important.” So the devil is absolutely in the detail. Yes, I can send you a list of questions. I can do that. But they tell you something back, but unless you can ask the next question straight away, you will only get half of the picture.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!