Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to showcase how I can answer many questions in a short period of time when helping clients directly over the phone or via Skype.
I therefore showcase another conversation with one of my clients Steve in a 1:1 phone/Skype counselling and consulting session.
This is another great case study where I can leverage your time, get down to your most pressing questions and most pressing issues very quickly and therefore help you to get the outcomes that you want, need and deserve for your critically ill loved one.
I can show you very quickly how you can improve the care and treatment for your Mom, your Dad, your husband, your wife, your brother, your sister, your niece, your nephew, your Aunt, your uncle or your grandmother or grandfather!
It all comes down to asking the right questions and it all comes down shining the light on the things that you don’t know and looking for a solution that Intensive Care teams often hide away from you!
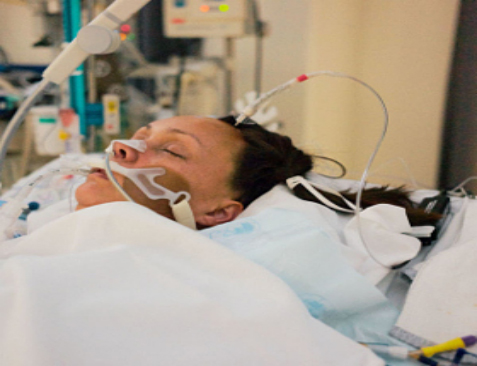
CASE STUDY: My Mom is ventilated in Intensive Care with a breathing tube and in an induced coma! She has COPD, will she need a tracheostomy?
Patrik: What’s your mother’s current situation?
Steve: She came in with a spot of pneumonia on her lungs. She has COPD. They put her on a bypass. Yes, she was on that overnight and the next day, she had not really gotten any better from that. They wanted to intubate her and they said, she would probably on it for three to four days. Today is day nine and she continues to fail the waking up process, I guess. Well she wakes up, but her heart rate goes up and they get worried. During this, they changed the ventilator to CPAP mode. They don’t start the weaning process or that’s as far as they go on the weaning process because they’re worried about her heart rate.
However, she has a history of anxiety. She is very anxious and gets agitated easily and you know she’s coming off of the Propofol, she’s coming off sedation to realize that, she’s got that tube down her throat. The breathing is laboured that’s why her heart rate and stuff is going up, but they don’t want to give her anything too close to the time for anxiety as they do that process because they don’t want to get a false reading, remove the tube and have have to re-intubate her. At this point they’re telling me that, she has osteoarthritis which she manages that pain at home with oxycodone.
They’ve been giving her fentanyl here. Right now, they’re currently doing the sedation vacation, in about 20 minutes I think they’re going to see about doing the CPAP mode, which is one of the reasons I wanted to call. Also, because they’re talking about by Monday, the only other option is to get the tracheostomy to have the ventilator hooked up through that. I just had questions like… I also purchased “The 5 Mistakes you are unconsciously making if your critically ill loved one is in an induced coma and is not “waking up”!
Patrik: Yes, thank you!
Steve: I’ll worry about that soon but one of the things I’m wondering about is, when she’s coming down like that, when she is off of the sedation and they are trying to see how she does on the CPAP. She’s kind of anxious and they’re asking her to do commands and stuff. Do you think I am making her more anxious if I am there, letting her hear my voice and telling her that I’m there in the room?
Patrik: No.
Steve: Asking her to do those things also?
Patrik: No I don’t think so.
Steve: You think she’d be doing that?
Patrik: -I don’t think so.
Steve: Like I should hold back?
Patrik: No, I don’t think you should be holding back. I think it’s very important for anybody in intensive care who’s coming out of an induced coma, or who still is in an induced coma, to have somebody around that’s simply familiar. Yes, absolutely. I think it’s very important-
Steve: What about playing music, should I have music playing that she likes?
Patrik: Absolutely, if-
Steve: During that period?
Patrik: -if you think that is something she would be doing at home, that’s comforting her. Absolutely yes.
Steve: Okay.
Patrik: Anything that you think is helping your mother in terms of feeling more familiar with her surroundings. Keep in mind, she’s in a foreign environment and she’s battling a critical illness. I think anything that you can do to help her go in through this, whether that’s your presence or whether that’s playing music. I think that’s only a benefit-
Steve: Can I ask you this?
Patrik: Yes.
Steve: They’ve been adamant here about the nine to 10 day mark on the ventilator, is really, that as long as you want to do it unless you’re going to– at that point you needed to go to the tracheostomy. My friend’s grandmother was in a medically induced coma also, they kept wanting to take her off of it. She was on it for four weeks and her daughter kept saying, let’s just try one more day for her to get her strength back. But she was in there for– she had heart failure and then had surgery.
I understand that they’re different, they’re in there for different things but if the concern is her lying in the bed and her oesophagus starting to get erosion from the tube. I don’t see how that’s any different one way or the other. Is it more common for COPD patients to have a lesser time on the ventilator than a heart patient?
Patrik: Not necessarily. Now when you’re saying your friend’s grandmother, did you say she was on a breathing tube for four weeks?
Steve: Correct.
Patrik: Right.
Steve: They were saying, we want to go ahead and give her the tracheostomy. Go ahead.
Related articles/videos:
Patrik: Here’s the thing, one of the major benefits of a tracheostomy is that it can seem to lower the sedation very quickly, I would say. Somebody who’s on a breathing tube for four weeks would receive a fair amount of sedation, whether that’s propofol, fentanyl or any other sedatives.
Steve: Right.
Patrik: That is one of the main benefits of a tracheostomy, it can pretty much-
Steve: We’re talking beyond that.
Patrik: -reduce the sedation as soon as the tracheostomy has been done. The sedatives have a number of side effects, right? Or undesired side effects, I should say. From my perspective, having a tracheostomy done has a lot of benefits. Probably more benefits than negatives.
Steve: Right. Although she’ll have to go to a nursing home, it’ll be a year. On Monday if I apply for in-home health care for her, the waiting list is roughly a year in my area.
Patrik: Right.
Steve: That worries me.
Patrik: Absolutely. You see, the goal of a tracheostomy should not be for your mother to go a nursing home. The goal of a tracheostomy really, should be to support and even speed up the process of getting her off the ventilator.
Steve: I see, but what they’re telling me is, she would be here after that surgery about a week at the most. Then there’s an interim place called ‘Select’, where she would go where they would do that weaning but, it only last two weeks at that place. They attempt to wean her for two weeks. Afterwards, the only option would be a nursing care facility until I was able to get things set up to take her home, which they’re saying in this area that you got a year before that’s going to happen.
Patrik: Right. That would be fairly lengthy conversation to have in terms of what’s next after tracheostomy. What other medical issues is your mother having besides the COPD? Is she having any other? Major medical issues?
Steve: She has osteoarthritis.
Patrik: Osteoarthritis. Yes, anything else?
Steve: Yes. Those are the big ones, high blood pressure, she suffers from high blood pressure.
Patrik: Right. Okay. The goal would always be-
Steve: And something called, I think it’s hyperlipidaemia.
Patrik: Hyperlipidaemia. Yes, the goal would always be to get somebody off the ventilator, right? Without the tracheostomy, that would always be the goal. If that can be facilitated in one way or another, that should always be role. Right?
Steve: Do you think that it’s– go ahead, I’m sorry.
Patrik: The goal should always be put a tracheostomy in or get your mother off the ventilator without the tracheostomy. That would be a really good goal. Then get her out of intensive care. If that’s not achievable at the moment, then doing a tracheostomy and getting her off the ventilator. I don’t quite understand why they’re telling you if she has a tracheostomy they can only wean her for a couple of weeks in this other facility and then she would have to go on to a nursing home, or maybe getting her home. That’s a very bleak scenario as far as I’m concerned.
Anybody with a tracheostomy, just like with a breathing tube, the goal should always be to get them off life support. The goal with a tracheostomy, of getting her off life support would be to aid that process if anything, because you can reduce sedation very quickly. It’s easier to mobilize your mother out of bed. That sort of stuff. I’m not quite sure why they’re sort of not pointing towards that.
Steve: Right. Should I be after the– or for the tracheostomy or after, if I should be looking in a different hospital for that?
Patrik: That would be my first feeling with-
Steve: Do I have to go through the doctor here in order to have that set up or can I call another hospital?
Patrik: They might get a little bit defensive if you are trying to steer this into another direction but I, just by what you are telling me I assume you always have to– we almost have to steer this in another direction. The other thing that’s often happening in hospitals is simply, you don’t know how pushed they are. If they’re not pushed for beds, you don’t know what interest they might have in putting a tracheostomy in terms of co-payments they are getting extending– there is always that financial side involved as well. But usually the main concern is that they are pushed for the beds they probably have.
Steve: Do you know, can I call a hospital directly myself and ask about having her switched because initially before, when they wanted to put her on the ventilator and she was on the bypass, I told the doctor I’d like to have her to move to another hospital that’s in a bigger city that’s nearby. He said, “Sure no problem, I’ll start making that phone call now.” He came back in and said that they contacted him and said we wouldn’t be doing anything for her that you’re not doing there. They didn’t accept her. We tried another one and again they didn’t accept her.
Patrik: I think one of the challenges is, how big is the interest of the hospital to really help you in that respect. I couldn’t tell you that at the top of my head but there is always that question. What interest do they have to do X, Y and Z or not do X, Y and Z that’s something. I couldn’t tell you over the phone. Another part of how we might be able to help you is, we would certainly be very happy in having a chat to the hospital too and find out what’s really happening. Why are they talking about only giving her two week time window to get her off the tracheostomy if she has one and then she has to go on to a nursing home.
That to me doesn’t make any sense at all. It’s as if the goal should always be get somebody off the tracheostomy and the ventilator. That should always be the goal.
Steve: Yes.
Patrik: The outlook should not be to do a tracheostomy, give her a two week time period to get her off the ventilator if that doesn’t work, she’s got to go to a nursing home. That to me doesn’t sound like a desirable therapeutic goal, if that makes sense.
Steve: No. Yes. They keep telling me that they don’t think she can breathe without the machine. If she hasn’t been able to for this many days that they’re not sure how successful it will be to do the tracheostomy but how do you know if you don’t try?
Patrik: That’s exactly right. And I don’t know how much time you spent on our website to sort of look what other people ask or what common scenarios are in those situations. The reality is that sometimes people with the tracheostomy, they might come off the ventilator within days, within weeks or sometimes within months. And in rare instances not at all. But the reality is that most patients do come off the ventilator. And the tracheostomy yes, absolutely.
Steve: Even with COPD?
Patrik: Absolutely. The other thing again, and you might have seen that, if you have read a number of articles, or watched some videos on our website-
Steve: I haven’t.
Patrik: No, no that’s okay. Or some of the videos, ICU teams and the doctors in particular tend to be always negative. Always.
Steve: Yes.
Patrik: That’s one of the biggest challenge that families are dealing with. They’re always negative. They’re not telling you the bigger picture and that’s a shame really. Here is what we can do for you if that’s of interest, we would definitely be very happy to talking to them to find out what’s really happening. For example, if I had to chat to one of the doctors and just simply asking them.
You mentioned before she’s on CPAP, what other settings is she on, besides CPAP? How much PEEP is she on? What’s her pressure support? What’s her tidal volume like? What’s her blood gasses like? Have they started to get her out of bed? What are they doing in terms of physical therapy? There’s a whole range of things where we would have a very good idea of how close is she really to number one, get of the ventilator. Number two, needing a tracheostomy. That sort of stuff. Where we could really help you to sort of ascertain of, “Hang on guys, are you really trying everything that you can to get this lady of the ventilator?”
Steve: Sure. What number would they call?
Patrik: It would be this number, but– or at the same time we can contact them. But that’s something we can definitely help you with. And it’s also a matter of holding them accountable. I think they are only telling you half of the story.
Steve: Okay.
Patrik: They’re only telling you half of the story. What also happens often is, you mentioned that if your mother has a tracheostomy, she’s got a two week time window to go to this other facility and then wean her off the ventilator. Now, again that to me sounds to a degree almost unrealistic. She might well come off the ventilator within two weeks, even with the COPD. But she might need three weeks, she might need two months. And that is certainly an achievable goal. I can send you a link to an interview that I did a while back with a gentleman who was on a ventilator for 12 months. And he managed to come off. He was a gentleman, he just turned 80. Right, eight, zero. There’s no-
Related interview:
Steve: My mom’s 70.
Patrik: Right, so that’s a benefit. There’s no one size fits all in those situations and then that’s what they often try to do. They’re trying to press people into a pathway that doesn’t necessarily exist. People don’t follow the same pathway. People are different. They’re individuals.
Steve: I can have you call them or you would rather they call you?
Patrik: It doesn’t really matter, I can contact them or they contact me. One way or another we will hold them accountable for their actions or inactions! I would imagine that the other thing that I’m [chuckles] when they’ve told you that they’ve contacted them at the hospital, and they’re telling you that the hospital wouldn’t take your mother. Again, I’m almost questioning, have they done that?
Steve: Did they actually do that?
Patrik: Yes.
Steve: How would I find that out? By calling that other hospital?
Patrik: Most likely. Most likely.
Steve: What department would I be wanting to call?
Patrik: Most likely intensive care. If she’s on a ventilator-
Steve: Okay.
Patrik: If she’s on the ventilator and she doesn’t have a tracheostomy, she would have to be admitted to intensive care in another hospital. You see-
Steve: They could actually still move her before the tracheostomy?
Patrik: They could. They could, they could. You see, from the hospital-
Steve: That’s a lot of stuff to move.
Patrik: -it would be but that’s what’s ambulance service are doing. That’s not-
Steve: Right, right.
Patrik: -I don’t see that as a major obstacle really.
Steve: Yes, okay.
Patrik: Right? From a hospital’s perspective, it’s really a matter of, on one hand, they might want to keep the bed occupied because of obviously the payment they’re getting. On the other hand, if they are too pushed for beds because they’ve got other Patients waiting for beds. Right? Then they might want to discharge her. And you might see as time goes on they might change the story because of that. Because of their pressure in terms of what’s going on on their end.
Steve: Right.
Patrik: Right? From my perspective and from my experience, a tracheostomy would help. However, that sort of pathway they’re showing you in terms of, “Yes there will be a two-week window and if she can’t get off the ventilator within that two-week window, she’s got to a nursing home.” I’m almost saying, “Excuse me, that’s not how you want to treat anybody.”
Steve: Right.
Patrik: Right?
Steve: I agree.
Patrik: You know.
Steve: Probably you’d be hearing that from somebody else.
Patrik: That’s exactly right.
Steve: You need to hear-
Patrik: That’s exactly right. I would also be curious to know, they’re telling you this other facility, she can go there and she has a two week time window. I’m almost curious to know, “Okay, what’s this other facility saying about this?” How specialized are they to get her off the ventilator?
Steve: I think that’s like, that’s one of the things they do there.
Patrik: Right.
Steve: But, that two-week period seems awful short. They’re supposed to come in on Monday to make an assessment-
Patrik: Right.
Steve: -that’s the way we had that setup.
Patrik: Right. And again, that would be part of what we can help you with in terms of talking to them. We can talk to whoever you want us to in order to help your mother’s situation.
Steve: Do I need to setup like an actual time for you to speak with them? Or I said-
Patrik: Here is usually what we tend to do, and again, there’s no one size fits all it’s majorly structuring anything around what you need and the outcomes you want to achieve.
Steve: Yes, right.
Patrik: In some situations, we might say, “Look, it does make sense to work with you over the next week or over the next three or four days.” Or whatever time frame we put on this. But we speak to whoever you want us to and help you get the outcomes that you want. That’s what you engaged us for! And if I can talk to the doctor that’s usually when we can help you and your family the most! IWe can also talk to another facility and find out what they can do for your mother and if they can help you get the outcomes that you want!
Steve: Where they were sending her after she gets the tracheostomy? You could talk to them and all that stuff?
Patrik: Absolutely.
Steve: Okay, all right.
Patrik: The other thing that we can help you with, and that would be down the line. Again, I really need to stress here that goals should always be to get somebody off the ventilator. I’m not even sure why they’re sort of painting this negative scenario. If in the worst case scenario, if your mother can’t come off the ventilator and off the tracheostomy, another service that we are providing, and again that would be long term and down the line, we are providing a service INTENSIVE CARE AT HOME. Right? We provide services at home for somebody on long-term ventilation with tracheostomy. But that’s-
Steve: You do?
Patrik: -yes, we do. But that’s not-
Steve: Okay.
Patrik: -that would be the worst case scenario.
Steve: But is that something that’s covered by her insurance?
Patrik: Most likely. Most likely. We would have to find that out. But the reality is that coming off the ventilator should be number one priority and if your mother can’t come off the ventilator and you want her at home you can use our service INTENSIVE CARE AT HOME!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE quickly when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
Related Articles:



