Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another question from one of our readers and the question this week is
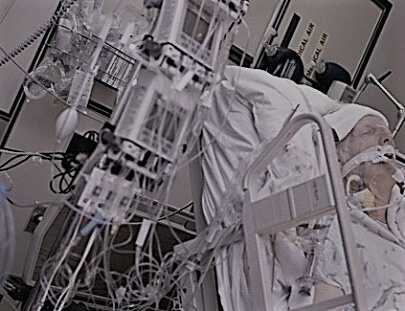
My 57 year old Dad has been in Intensive Care with Cardiomyopathy and Pneumonia for 5 weeks! He’s still in an induced coma and still doesn’t have a tracheostomy, HELP! (PART 11)
This series of questions from Garry are excerpts from numerous 1:1 phone and email counselling and consulting sessions with me over a two month period.
You can access previous parts of the series here Part 1, Part 2, Part 3, Part 4, Part 5, Part 6, PART 7, Part 8, PART 9 and PART 10
Garry and his family went through many challenges while his Dad was in Intensive Care and I felt very privileged helping Garry through this difficult time in his and his Dad’s life!
If you have followed this series of questions, you would have seen that by now, Garry’s Dad’s situation was getting more and more desperate as the ICU really let them down from the start.
By the time Garry got my help it was almost too late, because his Dad had been mistreated for too long and the ICU was reluctant to seek outside help.
This story and this series of questions really serves as a warning to anybody who has a loved one in Intensive Care and it really shows that you can’t afford of not doing your research. Not doing your own research when your loved one is critically ill in Intensive Care could well prove deadly in fact!
If you are in doubt if your loved one is getting the best possible treatment that they could possibly have, please send us an email to [email protected] or simply give us a call on one of the numbers here
Garry writes
Hi Patrik,
hope you are well.
Just a quick update, Dad isn’t doing too good.
His liver is now in failure, he is very jaundiced and the bilirubin count is high.
I suppose the only positive side is that his infection markers are down and his vitals are holding strong. Though, with the liver failure im not sure if that makes any difference now.
His cognitive awareness is very poor. His eyes are open, but little to no response. “lights are on but nobody is home” is how I’d say it. He responds every now and then but then falls back in to that state.
Got nowhere with Medical records, they won’t release them while he is still a patient, asked several different people and all said the same.
Only thing I can think of is the medical director which I’m still working on.
Is there anything they can do for the liver?
It looks like it has come to that time where I have to say whether it’s in my Dad’s “best interest” to continue treatment or not.
He is still on antibiotics, which they have just changed up to see if that helps his liver. He is still on 6 of Dobutamine, 5 of Noradrenaline and 2 of Morphine.
The consultant said that he is suffering now due to prolonged treatment and that he wouldn’t be a candidate for any invasive treatment at this stage, and that we would only be prolonging the inevitable. He asked my thoughts and still said that my Dad would want to fight this to the end but he still gave me the same response “it’s in the best interest of the patient to make him comfortable”!
It seems no amount of preparation has prepared me for this decision that i have to make, what makes it worse is that I have to make it alone…
In your experience working in ICU, do you think (without actually seeing my Dad and his medical records) that we are at that stage now considering: 3.5 months in ICU etc. ? – 2 steps forward 6 steps back and a never ending circle.
Thanks for everything Patrik
Garry
Hi Garry,
I’m so sorry to hear that your Dad isn’t getting better.
One thing they could do for the liver failing is giving Parvolex. Parvolex(also Acetylcysteine) is a drug being used for liver failure. It might be a little bit old fashioned as it has slowly disappeared over the years, but it’s still available.
I’m so disappointed that you don’t have access to the medical records, it sounds like the whole system is very restrictive…
I know that you can get the medical records whenever you want them, you should be asking them what they have to hide?

By now we know that they have lots to hide with everything has been happening or more importantly with everything that hasn’t been happening and that should have happened!
As it relates to the liver failure… Early tracheostomy would have minimised the risk for liver failure due to less need for sedatives and opioids for the induced coma. Those drugs are very potent and get metabolised via liver and kidney. Therefore minimal use of such is critical for long-term outcomes.
Also with liver failure, your Dad’s brain wouldn’t be working 100% as toxic waste often accumulates in the brain. I hope is comfortable at least.
However as I mentioned in our previous conversations over the phone and by email, the words used in ICU by the Intensive Care team “in the best interest” always raise red flags for me.
The Intensive Care team always has an agenda that goes way beyond what’s happening clinically. I have written about this extensively in my blogs and videos!
No amount of preparation, thinking, reading or researching will prepare you for this. It’s the worst possible nightmare and worst possible outcome.
Clinically, it looks like your Dad might be approaching his end of life.
However just because the doctors think or perceive that your Dad is suffering doesn’t cloud your judgement. What do you think? Do you think that your Dad is suffering?
You have been clearly stating your Dad’s wishes that he would fight this to the very end.
This is the most important question in all of this. If you think that your Dad isn’t suffering and you think that they should continue treatment than your wishes and thoughts need to be respected, period!
They have been fluffing around and messing up so much that they want to put an end to it.
This must be so embarrassing for this ICU and the head consultant in particular… Not getting a Cardiologist involved, not referring your Dad to another more specialized ICU where he could have had ECMO, VAD and the potential for heart transplant.
Instead the ICU consultant left your Dad in the worst of all places, in a 3-bed ICU where they wouldn’t ever see any severe cases of Cardiomyopathy.
And again, not doing a tracheostomy for nearly 5 weeks and leaving your Dad in an induced coma unnecessarily is just pure negligence, period!
And yes, 2 and a half months in ICU is a very long time, however what’s “in the best interest” of your Dad should be a 50/50 decision between you and the Intensive Care team. The reality is that there has been no communication, let alone collaboration with you and your Dad from the very start. What was “in the best interest” for your Dad has gone out of the window from the very start and it’s an absolute disgrace!
I’m very frustrated just by the way they have treated your Dad and you. It’s absolutely disgraceful and negligent and I stand by that!
The only question in this situation really is, do you want to put an end to it?
Would your Dad want you to put an end to it, because at this point in time you are the decision maker.
If you and your Dad were having a conversation what do you think he would say? I believe that is what it’ll come down to. It’s fictional but only you know what your Dad would say if you were having a conversation about this situation. Therefore only you know “what’s in the best interest” of your Dad.
By now you have a very good understanding what’s happening clinically, therefore you should really forget about what the consultant has to say and go with your gut feeling. Your gut and intuition never lies.
An end of life situation I always hard and it’s especially hard when you are in the midst of it and you are about to lose a key family member at a young age! It’s the worst possible nightmare!
The way to look at it from my experience is “If I could look back to this situation in ten years time, would I still do the same things and make the same decisions?” Hindsight is a wonderful thing, however time doesn’t permit you to get this wrong.
Related article/video:
And by that I mean your own positioning, your own thinking and your own rationalisations! Are there things that have been unsaid between you and the Intensive Care team? Do you think that if your Dad died tomorrow that you have unfinished business with him or other family members? Do you need more time to think?
Do you think you can look yourself in the eye by what you have and haven’t done in the last few weeks if your Dad died tomorrow?
This is what it comes down to when I say “make informed decisions, have peace of mind, control, power and influence”.
You most likely can’t stop your Dad from dying soon. What you might have control over is the circumstances and the way you are approaching this. Do you need another 24, 48 or 72 hours to spend more time with your Dad or do you need another week? Only you can answer this question!
Do you think it’ll help you as well having more time with your Dad? Again, only you can answer this question!
Recommended:
Will you have a say or will you just be “giving in” to the Intensive Care team?
I have seen many families in Intensive Care who felt extremely guilty when their loved one died in ICU for a number of reasons. You want to have a mental state that helps you moving on from here quickly, come to terms with things and not let you look back in bitterness. Neither you, your Dad or the rest of your family deserves or would want this.
You really need to take the Intensive Care team out of the equation for now. This is about you and your Dad. The Intensive Care team should be able to facilitate the last few days or hours on your terms and what you think is “in the best interest” for you and your Dad!
It’s called a holistic approach, but I would imagine that the Intensive Care team there wouldn’t even know how to spell holistic.
I hope this helps Garry. More than happy to talk if you want to.
Never forget that things happen for a reason in life. I don’t know why the universe is challenging you with this situation, but I’m sure you will find out sooner or later!
Stay strong and stay in control of “what’s in the best interest” for your Dad and for you!
Take care and I can be available pretty much anytime if you want to talk it through.
Look after yourself and wishing you all the best!
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!