Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions that we get quite frequently as part of my 1:1 consulting and advocacy service!
After Coming Off the Ventilator, Is There a Chance to Go Again Ventilated?
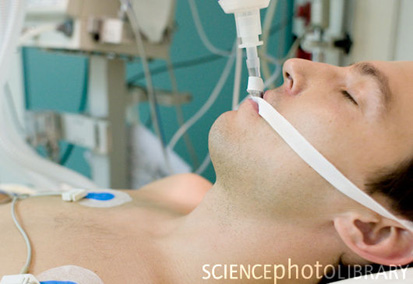
Taking patient off a ventilator is usually a gradual process, often referred to as weaning. There are numerous articles that describe this process in detail, and clear protocols have been developed. Assessment of a patient’s readiness for removal of the endotracheal tube in the ICU is based on:
- ability to maintain a patent upper airway
- ability to cough and clear secretions
- ability to follow 4 simple tasks (ie, open eyes, track with eyes, grasp with hands, and stick out tongue)
- adequate ABG (Arterial Blood Gas)
- sitting up in bed
Reintubation is common following extubation and discontinuation of mechanical ventilation. The extubation failure rate considered acceptable has empirically been set at 10–15%, but avoiding reintubation remains an important clinical goal.
Extubation failure-need for reintubation within 72 h of extubation, is common in intensive care unit (ICU). It can cause increased morbidity, higher costs, higher ICU and hospital length of stay (LOS) and mortality.
Due to the high economic and personal costs of prolonged weaning and extubation failure, it is imperative that the critical care nurse monitor factors such as patient discomfort, fatigue, sweating, work of breathing, mental status, and vital signs during weaning. In addition, measures such as these can be taken prior to the start of a Spontaneous Breathing Trial (SBT) to encourage successful breathing:
- Optimizing muscle strength by providing adequate nutrition, avoiding neuromuscular blockers that paralyze the muscles that are necessary for breathing like cisatracurium or rocuronium , decreasing corticosteroids, and normalizing electrolytes.
- Decreasing respiratory work by placing the patient in an upright position, decreasing respiratory demand and resistance, and increasing compliance.
- Optimizing ventilator drive by reducing or stopping sedative medications.
- Increasing oxygen-carrying capacity by avoiding factors that cause atelectasis or collapse of the lung, correcting anemia and blood gases imbalances.
- Addressing cardiac dysfunction and oxygen-carrying capacity.
- Promoting sputum clearance.
- Mobilization as appropriate. (6)
Related Article:
WHO ARE AT RISK FOR EXTUBATION FAILURE? (3)
- Patients with advanced age
- High severity of illness at ICU admission and extubation
- Preexisting chronic respiratory and cardiovascular disorders
- Unresolved illness
- Development and progression of organ failure during the time from extubation to reintubation
- Prolonged sedation and prolonged induced coma
*Reintubation itself have been proposed as reasons for increased mortality and morbidity*
PARAMETERS USED TO PREDICT EXTUBATION FAILURE CAN BE CATEGORIZED INTO:
- assessing respiratory mechanics
- assessing airway patency and protection
- cardiovascular reserve
*The intensivist needs to identify patients at high risk of extubation failure and be prepared to reinstitute ventilation early to prevent adverse outcomes*
NECESSARY FOR SUCCESFUL EXTUBATION:
- Adequate cough strength
- Minimal secretions
- Alertness
- Stable vital signs
- Acceptable blood gas results and chest x rays
Related article:
FAILED EXTUBATION CONSEQUENCES
To predict “extubation failure” is essential, as both delayed and failed extubation have detrimental consequences such as:
- prolonged ventilation and ICU stay
- need for tracheostomy
- increased cost of treatment and mortality
CAUSES OF EXTUBATION FAILURE
- poor nutrition
- decreased level of consciousness due to persistent effects of sedative and analgesics
- neurological impairment due to primary illness
- respiratory failure which manifests with increased work of breathing, accessory muscle use, hypoxia
- failure to maintain airway patency due to upper airway edema seen in patients with prolonged translaryngeal intubation and evident as stridor
- Excessive secretions, coupled with inadequate muscle strength and glottic incompetence
- Prolonged sedation and induced coma
WHAT IS AN UNPLANNED EXTUBATION?
Endotracheal intubation is always being done in the hospital for patients who have and may have problems with their airway and it is very important to monitor closely these patients to always secure the breathing tube in place to avoid unplanned extubation.
An unplanned extubation occurs when a patient is on mechanical ventilation and their endotracheal tube is removed when it was not supposed to be.
If the patient themselves intentionally removes their own tube, this is known as self-extubation or deliberate unplanned extubation, whereas if the tube is removed by health professionals, or a patient removes it by accident, it is referred to as accidental extubation. (4)
Unplanned extubation can increase the amount of time a patient must remain on mechanical ventilation, the duration of the patient’s hospital stay, and the patient’s medical costs. It is also estimated that 60% of patients who experience an unplanned extubation require re-intubation, which may increase the risk of ventilator-associated pneumonia.
MANAGEMENT OF FAILED EXTUBATION
A reasonable strategy to prevent failed extubation, if anticipated, can be:
- continued ventilation
- treatment of remediable causes of muscle weakness and excessive secretions
- daily assessment for readiness to extubate
Specific therapies can be used only when the cause for failed extubation is known.
- If extubation failure is due to cardiac failure adequate anti-failure with diuretics and vasodilators can be instituted and then extubation attempted.
- Performing tracheostomy is another option; however, the problem of removing artificial airway still remains and tracheostomy has its own complications.
- Only two options seem promising in failed extubation, non-invasive ventilation and prophylactic steroids
Intubation is one of the integral parts of the hospital procedures as it is considered as an emergent life support measure. Being able to successfully remove the breathing tube of your loved one or wean them from a ventilator requires prompt and proper implementation of the successful extubation recommendations to avoid getting your loved one again ventilated. Such circumstance needs that the critical care nurses and the team serve as leaders in the adoption of the above recommendations to ensure that patients receive the highest quality of care during mechanical ventilation, weaning and successful extubation.
REFERENCES:
- Factors Associated With Reintubation in Intensive Care https://www.researchgate.net/publication/11841633_Factors_Associated_With_Reintubation_in_Intensive_Care
- Predictors of Reintubation in Critically Ill Patients http://rc.rcjournal.com/content/59/2/178
- Extubation failure in intensive care unit: Predictors and management https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2760915/#sec1-1title
- Unplanned Extubation https://en.wikipedia.org/wiki/Unplanned_extubation
- Unplanned Extubation in Adult Critical Care: Quality Improvement and Education Payoff https://aacnjournals.org/ccnonline/article-abstract/24/1/32/891/Unplanned-Extubation-in-Adult-Critical-CareQuality?redirectedFrom=fulltext
- Mechanical Ventilation Weaning: An evidence-based review https://journals.lww.com/nursingcriticalcare/Fulltext/2018/11000/Mechanical_ventilation_weaning__An_evidence_based.2.aspx
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!