Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Mom is in ICU with Seizures and is Not Waking up. Is it Because of Her Sedation?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ryan as part of my 1:1 consulting and advocacy service! Ryan’s mom has been ventilated with sedation but has already discontinued sedation for 4 days and now he is asking why his mom is still not waking up.
Mom Has Been off Sedation for Four days But Why is My Mom Not Waking up. Please Help!
Hi Patrik,
Thanks for the reply and your time, only found you the other day. This is a long story as to what happened to my mom from August 8th till November.
So on August 8th, she had back surgery which was successful as she was on the verge of being unable to walk if the surgery is not done.
On the 14th August, it was planned to put a stent in the heart too.
On the 17th August she was in the ward recovering and the right leg was having blood flow problems. It turned out that the puncture site in the groin got infected which then needs open leg surgery.
RECOMMENDED:
On the 21st August, the surgeon did not think she would make it. She survived the first 24 hr after.
On 23rd of August, she was vomiting early in the morning and turned pale white. The surgeon rang me up saying she needs surgery on the small intestines because there was no blood flow to 10cm and was then cut out.
She came back intubated, it was planned only for 4 days then they extubated her. Well in the end, the ICU did not feel confident about the extubation. So it was suggested to put a Tracheostomy on the 28th of August.
Recommended:
From that day, the main ICU doctors, both of them, who are looking after my mom, went on 5 weeks holiday. Getting Bench warmer ICU Doctors who were very non proactive to trying to solve the problem on getting her off the ventilator.
Since The 28th August she had 5 different doctors. The main ICU doctor has been 75% on the case but very non proactive and the rest have just followed his lead.
Suggested links:
On The 4th Sept she was on dialysis as the kidneys are acute and only 40% working and since then from Sept on, she has been on Propofol anywhere from 5 to sometime 15 on the IV unit machine and Fentanyl has ranged from 5 to 8 units the machine for a long time now.
Then a new ICU doctor took over and tried cutting off both. The Propofol is stopped but he is having problems with the fentanyl as she is getting agitated and not responding to commands so they put her back on to the Fentanyl at 2 units.
She is passing black stool and now she started passing bright red blood from large intestines which I think now she has IBD (Inflammatory Bowel Disease) or ulcers. I said from day 1 she was no good on opioid drugs.
Kind Regards
Ryan

Hi Ryan,
Thank you Ryan for explaining your Mom’s situation. Your mom has been through a lot and I know that you want only but the best for her condition. This is usually the challenge that the families are facing when their loved one is critically ill in the ICU.
Most of the time, families will only take and follow whatever it is that the doctors are telling them. But that should not be the case. You have the power to be in charge and take control of how you want your mom to end up. And that is, for her to LIVE and RECOVER.
Recommended:
Firstly, your mom had a successful back surgery, for the reason of possibly becoming disabled if left untreated. Back surgery is an option if conservative treatments haven’t worked and the pain is persistent and disabling. Back surgery often more predictably relieves associated pain or numbness that goes down one or both arms or legs.
These symptoms often are caused by compressed nerves in your spine. Nerves may become compressed for a variety of reasons, including:
- Disk problems. Bulging or ruptured (herniated) disks — the rubbery cushions separating the bones of your spine — can sometimes press too tightly against a spinal nerve and affect its function.
- Overgrowth of bone. Osteoarthritis can result in bone spurs on your spine. This excess bone most commonly affects the hinge joints on the back part of the spinal column and can narrow the amount of space available for nerves to pass through openings in your spine.
Then, they have placed a stent in your mom’s heart, but the question is, why would your mom need it in the first place?
WHAT IS A HEART STENT AND WHY WOULD YOUR MOM NEED IT?
Stents are used to reduce symptoms in patients with obstructive artery disease who suffer chest pain/tightness or shortness of breath that your mom might be experiencing with exercise or during periods of strong emotions. Stents may be used instead of bypass surgery in some selected patients.
Stents are essentially required to open blocked blood vessels unable to deliver blood to the organs of the body. A stent is a small mesh tube that is inserted into the artery to remove the blockage and is left there permanently to keep the blood flow steady. According to the medical rules, a stent is required to widen the blocked artery when there is at least 70% of blockage detected.
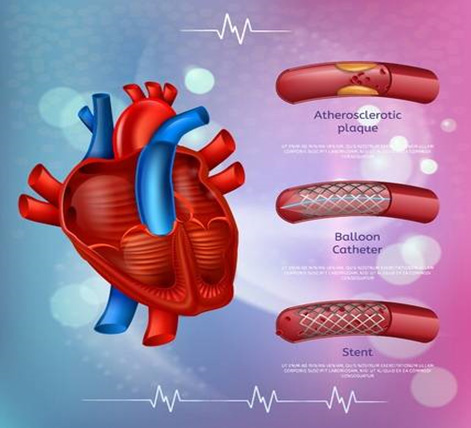
WHAT IS THE STENTING PROCEDURE?
Stents are placed during a coronary angiogram. A small tube called a balloon catheter is inserted into the femoral artery in the groin, where I believe is the puncture site for your mom, or the radial artery (arm), and advanced toward the heart to the very top of the aorta. After the blockage is identified, a wire is placed into the coronary artery to the site of the blockage and the stent is loaded on to the wire. The stent is expanded to the size of the artery and may be expanded by inflating a balloon within the stent. Then the wires are removed along with the catheter, while the stent stays in the artery permanently.
WHAT HAPPENS AFTER THE PROCEDURE?
Recovery from an angioplasty and stent implantation is usually fast. Most patients can resume normal activities 24 hours after the procedure. Some people experience bruising, which will disappear in a few days. It would be wrong to say that there will not be any risk associated with heart stents, but such risks arise in case of lack of care and this could be the reason why your mom developed blood flow problems at the right leg 3 days past the heart stent placement. Due to a heightened risk of clotting after stenting, treatment with Aspirin and antiplatelet drugs (also called anti-clotting drugs) is required such as Clopidogrel (Plavix). Consequently, it turned out that the puncture site in the groin got infected which then needs open leg surgery and this must be really difficult for you and your mom.
Vigilant monitoring of your mom after heart stenting is fundamental for early identification and management of complications. Nurses and doctors who are able to promptly identify complications are in the optimal position to prompt critical action and prevent your mom to undergo open leg surgery because of this. Heart stents are completely safe for the right patient with proper procedure of insertion and good after-care.
Then, the doctors now have become negative telling that your mom won’t make it? But they were wrong. Your mom is fighting for her life up till this time and YOU as hr son should stay positive to counteract whatever negativity these people are throwing at you and I can definitely teach you how to do that!
Related links:
Days passed and your mom’s condition became worse and therefore she needed to undergo another surgery because part of her small intestine became necrotic and that they have to cut it out.
What could have led to this condition anyway? Have you asked the doctors about it? Have they cared telling you the reason behind it? The biggest challenge for families in intensive care is that, you don’t know what you don’t know. You should learn how to have a voice and to ask the right questions!
She came back intubated, opted for extubation, but the doctors are not confident about it and so they resorted to putting a tracheostomy on your mom, still ventilated for how many days and you are unsure when will your mom be removed off the ventilator because your doctors are being laid-back of your mom’s current condition.
There are certain parameters to know how your mom can be weaned off from the respiratory support. There is a routine management for that which includes, results of arterial blood gases, current chest x-ray, your mom being fully awake and her hemodynamic stability.
Recommended:
Then came Sept 5th where your mom had to be on dialysis because her kidneys are unable to function at full capacity and you mentioned that she was on sedation with Propofol and Fentanyl for a long time already. There was a trial study about critically ill patients that concluded, that patients on a “sedation control group” developed a degree of renal impairment apart from the “awake intervention group.” Thus, sedation may injure organs other than the brain. The doctors should have taken precautions with sedation knowing that your mom developed kidney failure.
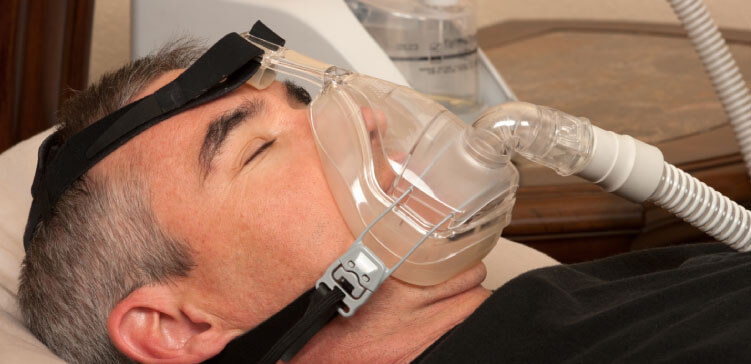
But why is your mom on sedation primarily? Because she needs to be in an induced coma to get the benefit of full ventilation therapy when she still has the breathing tube in. Imagine a tube down your throat would be very uncomfortable for you and so in order for your mom to cope, she needs to be sedated.
But when they shifted her to tracheostomy for ventilation, the doctors should have weaned then ceased the sedation because tracheostomy is much easier to tolerate. If your mom has been on in induced coma for a long time, waking up might be delayed because it might take some time to wash out all of the drugs off her system.
If your Mom can’t come off the ventilator and tracheostomy and is therefore facing a prolonged ICU stay, look for genuine alternatives such as INTENSIVE CARE AT HOME.
INTENSIVE CARE AT HOME sends ICU/PICU nurses into the home 24/7 and provides an intensive care substitution service, providing a much better quality of life for Patients and their families whilst reducing the cost of an ICU bed by 50% whilst freeing up in-demand ICU/PICU beds!
A win-win situation!
Recommended:
And so, a new doctor came into the picture and tried to cut both the Propofol and Fentanyl, but your mom is having withdrawal symptoms so they resumed back Fentanyl. Weaning off the sedation, it should be gradual as your mom is prone to withdrawal especially for Fentanyl, usually, clonidine will help minimize symptoms of withdrawal.
Lastly, your mom developed gastrointestinal (GI) bleeding, categorized both, melena and hematochezia. Melena refers to black stools, while hematochezia refers to fresh, red blood in your mom’s stool. Hematochezia usually comes from the colon, while melena usually comes from a higher point in your GI tract.
Both melena and hematochezia are symptoms, not actual conditions. Many conditions can cause either type of bleeding but this condition of your mom is serious and should be treated immediately by the doctors as this is life threatening.
Often, GI bleeding, melena or hematochezia are treated with proton pump inhibitors (PPIs) such as Pantoprazole (Omeprazole) infusions.
Furthermore, a gastroscopy may be necessary to identify the source of bleeding or a colonoscopy may be necessary if the bleed is in the lower GI tract.
To such extent, if the GI bleed is causing a significant drop in hemoglobin blood transfusions are required.
If GI bleeds are prolonged, feeds are being stopped and TPN (total parenteral nutrition also known as intravenous nutrition) is required via central line or PICC line.
RECOMMENDED:
It’s very difficult for you seeing your mom to be inside the ICU and in critical condition feeling that treatment is not working in her favor. That as time passes by, her condition is getting worse. You seem to have your hands tied, you know deep inside you, you have to do something, you feel you’ve got to do something but the challenge is, you don’t know how.
We definitely know what you feel and we are here to help as advocates for families in intensive care. When it comes to such issues, it’s best if you call me on one of the numbers on the top of the website so I can talk you through it step by step and let your mom have the best and appropriate treatment she could get and overcome this challenge in your lives.
Regards,
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
REFERENCES:
- Back surgery: When is it a good idea?
https://www.mayoclinic.org/back-surgery/art-20048274
- Why Would You Need A Stent In Your Heart?
https://www.epainassist.com/test-and-procedures/stents-in-your-heart
- Who Needs Stents and Why?
- What Causes the Need for Kidney Dialysis?
https://healthfully.com/216473-what-causes-the-need-for-kidney-dialysis.html
- Sedation and renal impairment in critically ill patients: a post hoc analysis of a randomized trial
https://link.springer.com/article/10.1186/cc10218
- What’s the Difference Between Hematochezia and Melena?
https://www.healthline.com/health/hematochezia-vs-melena
- Role of endoscopy in acute gastrointestinal bleeding in real clinical practice: An evidence-based review
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6379746/