Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
The ICU Team is Giving My Mom Too Many Sedatives & Now She Has ICU Psychosis! Help!
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I am here with a live stream today, where I want to answer your questions if you have a loved one in intensive care. And this is one of the most commonly asked questions for families in intensive care and it’s a question that we get all time. And today’s live stream is about the 10 Questions to Ask if Your Loved One has a Traumatic Brain Injury in Intensive Care! Live Stream!
10 Questions to Ask if Your Loved One has a Traumatic Brain Injury in Intensive Care! Live Stream!
Welcome to another livestream from intensivecarehotline.com. My name is Patrik Hutzel, and I will guide you to today’s livestream.
Today’s livestream is about, “10 questions you need to ask if your loved one is in intensive care with a traumatic brain injury!”
Thank you for joining this livestream today. Before we go into the 10 things, I just want to quickly talk about a couple of housekeeping issues. If you have any questions, just type them on the chat pad. If you can keep them to the topic, that would be great. If you have any other questions related to having a family member in intensive care, maybe type them at the end of this presentation so that we can stick to the topic to begin with, because I believe that’s why you’re probably here to want to know about traumatic brain injuries in intensive care.
RECOMMENDED:
Next, you may want to wonder what makes me qualified to talk about this topic. I am an intensive care nurse by background. I have worked in intensive care for over 20 years in three different countries. Part of my nursing career in intensive care included, me working as a nurse unit manager for over five years and having been in charge of two intensive care units in total. Then, I’m also professionally consulting and advocating for families in intensive care and have been doing so since 2013. I’m talking to families in intensive care all over the world every day. And I am participating in family meetings in intensive care, often over the phone via Zoom, via Skype, all modern technology, including the phone. I’m talking to doctors, nurses, and families in intensive care all day, every day, all around the world. Other things that we are doing here is also, we are running an organization, Intensive Care at Home, where we look after predominantly long-term ventilated patients in the home.
But without further ado, let’s dive into today’s topic because I believe that’s why you are here.
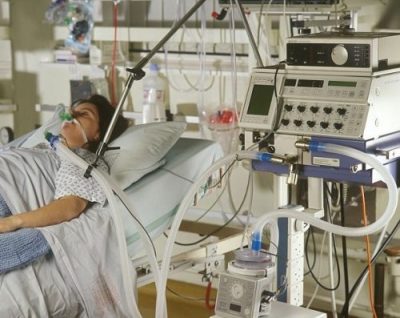
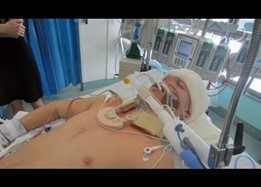
So, 10 things you need to know and 10 questions you need to ask when you have a loved one in intensive care with the TBI, TBI standing for Traumatic Brain Injury. So, traumatic brain injuries in intensive care can happen after a number of issues including but not limited to car accidents, people falling off roofs, after altercations, after fights, gunshots, stabbings, you name it. The first thing you need to probably know is when someone does come into intensive care with a traumatic brain injury. Usually, they have gone through detailed and intensive diagnostics on admission through the emergency room. They would’ve had a detailed CT (Computed Tomography) scan of the brain, maybe an MRI (Magnetic Resonance Imaging) scan of the brain. And that obviously then, often determines the next steps.
Now, also when I talk about a traumatic brain injury in intensive care, I also talk about most of those patients would be ventilated. Often if they have a traumatic brain injury, their Glasgow Coma Scale drops often to a 3. They need to be induced into a coma and need to go on a ventilator. Depending on the extent of the traumatic brain injury, patients might go to the theatre, to the operating room straight away, and have their skull opened. Maybe to decompress a bleed, insert an ICP, an intracranial pressure monitor. Sometimes patients have their whole skull removed, which is called a craniectomy only to decompress the brain so that the brain and the pressure goes down by removing parts of the skull. And the goal is when you remove a part of the skull, is to put that part back down the line when things are more settled and that is called cranioplasty.
But one of the most important things in those situations that needs to happen is to monitor ICP (Intracranial Pressure). ICP should be between 5 and 15 millimeter per mercury. Anything above 15 to 20 millimeter per mercury could potentially cause brain damage because if the pressure in the brain is too high, there’s not enough oxygen going to the brain.
It also needs to take into consideration with the CPP, which is called the cranial perfusion pressure. To give you a simple algorithm here, the mean arterial blood pressure or the mean blood pressure minus the intracranial pressure gives you the CPP, the cranial perfusion pressure. So, let’s make this an example. If the mean blood pressure is 80 and you have an ICP (Intracranial Pressure) of 20, And you deduct 80 minus 20, you get 60. 60 millimeter per mercury CPP (Cranial Perfusion Pressure), is the minimum the brain needs to have enough oxygen supplied to the brain.
So, it is very important in those situations that ICP and CPP are closely, closely monitored. If, for example, the mean arterial blood pressure is too low or the mean blood pressure is too low and you’re not achieving a cranial perfusion pressure of a minimum of 60, you often need to get the blood pressure up and you can achieve that potentially with fluids, but also often with inotropes or vasopressors. So, as you can already see, it’s a fairly complex arena, fairly complex issue to look at. And that is something that needs to be monitored very, very closely almost by the minute. That’s why you have an intensive care nurse at the bedside, one-to-one, 24 hours a day, to monitor this very, very closely. Because similar toward hypoxic brain injury, if the CPP is below 60 millimeter per mercury for prolonged periods, a patient can sustain irreversible brain damage. So, that gets ICP and CPP explained.
If your ICP is too high, you can do a number of things. As I mentioned, you can manage CPP potentially with inotropes and fluids. But if your ICP is too high, you can manage that in a number of ways. You can manage it, when an ICP goes in, there’s also often an EVD attached, an extra ventricular drain, that can drain CSF, which is basically the cerebral spinal fluids.
Now, when you drain EVD, your intracranial pressure should go down. But there’s also the assumption that the more you drain, the more CSF will be produced, and the more pressures go up. There is a suggestion that this potentially causes a vicious cycle. Therefore, there are other ways to manage high ICPs as well, and that can be with sedation, paralysis, or also hypertonic saline. If you’re giving hypertonic saline to get down to reduce ICPs (Intracranial Pressures), the saline draws out extra fluids out of the brain, and therefore reduces the ICP.
Another way to manage high ICPs, or high intracranial pressures, is mannitol. Mannitol is a diuretic that has come out of fashion a little bit from what I understand now. But I’ve certainly seen it used in ICU for high intracranial pressures.
So just recapping what we’ve talked about so far, ICU admission with traumatic brain injury. Initially, patients go through the ER or emergency room, emergency department has detailed diagnostics including but not limited to a brain CT scan. They often then go on to the operating room to have the brain decompressed, ICPs monitor being inserted. A craniectomy might happen to remove parts of the skull to reduce the pressure or to have a hemorrhage or a bleed stopped. There are a number of reasons why patients go for a brain surgery after a TBI.
Next, they have an ICP monitor inserted and an EVD inserted, an extra ventricular drain. They have then ICP and CPP very, very closely monitored to make sure that there is enough oxygen going to the brain. When someone has an ICP and an EVD, also often the CSF which is again the brain and spinal fluid need to be checked daily because there’s a high risk for an infection. You certainly don’t want the infection in the brain and therefore, the CSF needs to be checked almost daily for an infection.
Next, once things are more stable, your loved one might have an MRI scan. Going for an MRI scan is not an easy undertaking. Many questions need to be answered before someone goes for an MRI scan because there are many pitfalls. It takes a lot of preparation. It’s very complex sending someone to an MRI scanner, especially if they’re in intensive care and are unstable.
Suggested Links:
So also, I want to quickly talk about when someone is in an induced coma, and they’re paralyzed as well, and why they’re paralyzed especially when it comes to traumatic brain injuries. So again, there is obviously a lot of pain involved, or there can be a lot of pain involved. So, sedation and opiates are a must in traumatic brain injuries as most patients are ventilated. And they’re often fighting against the ventilator because it’s so uncomfortable, plus they can’t be oriented because of the brain injury. So, they need to go into a deep induced coma. Often, they end up on high doses of fentanyl or morphine for pain. They end up on high doses of midazolam or Versed, sometimes propofol, and sometimes a combination of all of that. With the propofol, propofol has a side effect of hypotension, which means low blood pressure. From what I explained to you earlier, that CPP needs to be maintained by achieving a certain mean blood pressure. The propofol could be counteracting that. Therefore, often midazolam or Versed is used as a drug of choice for sedation to not reduce the blood pressure even further.
Again, if patients are having still high ICPs and low CPPs while they’re in an induced coma, and high doses of sedation and opiates are used, then they need to be paralyzed on top of that to basically reduce any movement and reduce any high ICPs and CPPs.
Next, other suggestions for traumatic brain injuries are to keep the room dark, and not disturb the patient too much. Some units I’ve worked in, they use the PEEP (Positive End-Expiratory Pressure) of 0. PEEP is from the ventilator. It puts pressure on the lungs, which could potentially put pressure on the brain. Some units are still doing that. Other units use a PEEP as normal, which is a minimum PEEP of 5.
So, next is that a Glasgow Coma Score needs to be measured hourly. If you don’t know what a Glasgow Coma Score is, basically, what’s also known as GCS. The maximum Glasgow Coma Score, it’s a neurological assessment tool, which is very important to be used when someone is unconscious. So, you hear me talking, I’ve got a Glasgow Coma Scale of 15, that’s the maximum score. It means someone is oriented. They can talk, they have their eyes open, they can move, they’re compos mentis. The minimum score for a Glasgow Coma Scale or GCS is a 3, that means people don’t move, they don’t respond to pain, they don’t open their eyes, there’s no response at all. You could also argue they are in a vegetative state, but the more correct term is really to put a number on the Glasgow Coma Scale. So, if you don’t know what Glasgow Coma Score is, Google that after we finish here, after this livestream. Type in Glasgow Coma Scale. It’s really important that you familiarize yourself with it if you have a loved one in intensive care with a traumatic brain injury. It also helps to guide you with what their functional capacity potentially is down the line.
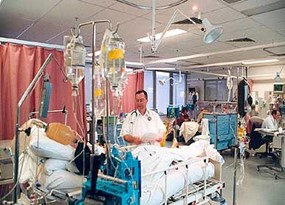
Next, pupil reaction. So again, after traumatic brain injury, the pupils need to be checked with a torch, making sure they look equal, they are reactive to light. Many patients in intensive care after a traumatic brain injury, you might see sluggish pupils. You might see them sluggishly reacting to light. You might see them not reacting to light at all. There could be a number of ways that pupils react. And if pupils, for example, don’t react to light at all, and they’re unequal in size, again that is a sign that there is significant brain damage. It could also be a sign that if they’re not reacting to light and they really pinpoint, that a patient might be brain dead. Sometimes, pupils are also dilated, and not dilated and not reacting to light, that could also be a sign of brain dead.
So, many questions need to be asked and answered when it comes to traumatic brain injuries. I will say this, there is a big difference between brain damage and brain death. If someone is brain dead, in most countries, they’re also legally dead, even though other organs such as heart, lungs, kidneys, and liver might still work. So yes, you got to be mindful of that. But I guess normally what happens if someone is considered brain dead, the intensive care team will talk to you sooner than later because there are other implications such as there could be a discussion to be had about organ donation and so forth.
I did talk about a craniectomy earlier and I want to hone in on that very briefly, that if someone again is having a traumatic brain injury and is having parts of their skull removed, you can sometimes see the brain pulsating. And you can see the brain sort of moving outwards a little bit, again, depending on how high the pressures are in the long run. And then the goal is obviously to put the skull back eventually. Most of the time, they’re using a plastic skull and it’s called a cranioplasty for that very reason. So, it’s not your own skull that goes back. It’s actually plastic, but that’s what’s being done often. When someone has a craniectomy, and has parts of their skull removed, they also often wear a helmet temporarily to protect them from any impact.
Next, I also want to talk about minimizing the risk for seizures. So, a lot of patients in intensive care after traumatic brain injury are at high risk of seizures. And you will find that if you look at the medication list for someone who’s in intensive care with a traumatic brain injury, they have Keppra or a phenytoin, phenytoin also known as Dilantin, as a first-line medication to minimize the risk of seizures.
You will see, or you can see that if patients are not overly sedated, there is definitely a higher risk for seizures to be caused. And seizures again can also cause more brain damage. Because again, you have similar to a low CPP, you have minimum oxygen flow into the brain, at least temporarily. And also, if someone is having seizures, even though they might be on phenytoin or Keppra, you could also manage that with midazolam. Midazolam works well in seizures, but then you’re sedating someone even more. Having said that, anti-seizure medications such as Keppra, or phenytoin or Dilantin also have a sedative effect.
Recommended:
Then, I also know a lot of you want to know about prognosis. Now, I do want to talk about prognosis, and I do want to talk about a quality of life going forward in a situation like that. Before I go into that into more detail, I want to sort of set the scene about outlooks, and about outcomes, and about prognosis. Because it is really difficult in intensive care to provide a clear prognosis in situations with traumatic brain injuries.
Often, traumatic brain injuries end up with a prolonged intensive care admission, which means until you’ve got ICP settled and until you’ve got the medications right, and until people have time to get the brain swelling down, should have talked about brain swelling as well. Also, should be quickly talking about midline shift. The brain is compartmentalized into two sections, left and right hemispheres of the brain. And when pressures are high, you might see the brain shifting from the left to the right. And that can quite literally be deadly, which is why it’s another reason to do a craniectomy as I explained. And that it’s another reason why you got to check ICPs and see CPPs really, really closely. And it’s also called a herniation of the brain if there’s a midline shift. So, if the midline shifts left to right because of brain pressures, that can really cause death.
Then, what I’ve seen as well, and that’s probably where I want to give you a little bit of a warning here. What I’ve seen as well is that sometimes the prognosis is so bad that ICUs want to rush to withdraw treatment and also want to donate organs. Many patients with traumatic brain injuries are young or can be young, and there is potentially interest to harvest some organs for organ donation.
If I was you as a family, I would not rush into any organ donation. I would not rush or consent to withdrawal of treatment just because there is a perceived poor prognosis. The brain is very difficult to predict. And what I do know is that some patients do recover, but it takes a long time. ICUs often don’t want to give people the time for that recovery. It’s very expensive, people take up beds in ICU, they take up resources that could be used for other patients, the outcome is uncertain. So, almost a traumatic brain injury can be considered as the “worst case scenario” for the ICU because it’s uncertain and it could end up in a long-term stay in ICU.
So then, if patients can’t come off the ventilator as part of their prognosis, as part of their progress or lack thereof in ICU and they can’t come off the ventilator, they need heavy sedation, heavy opiates, potentially paralysis, and they often need a tracheostomy. And if they need a tracheostomy, sometimes sedation can be lowered pretty quickly, which may or may not help with CPPs and ICPs. Because again, a breathing tube in the mouth is also very uncomfortable whereas a tracheostomy is much more comfortable.
Then, what you will often see that patients in intensive care after a traumatic brain injury can be incredibly volatile to look after in terms of, I don’t mean them to be volatile on a personal level, I mean them to be volatile on a clinical level. Everything can be all over the place, blood pressure, ICPs, CPPs, and other organs might be failing as part of their disease process. And that’s why it’s so difficult to predict what the next steps are.
But as time goes on, you might see that people will improve, and then you might see that people may not wake up and that it takes a long time for them to show any signs of improvement. If they do wake up once ICP has been removed, once EVD has been removed, once the brain injury has stabilized to a point where all medications have been optimized and the brain swelling has gone down, there’s no more midline shift, and so forth. And then they still might have a Glasgow Coma Scale of only 3, which means they’re in a vegetative state. And then you wonder, how long does it take for them to wake up? Will they wake up at all? And often, nobody has a crystal ball for that. What I will say is this, it depends on where you stand in terms of your religious beliefs, spiritual beliefs, cultural beliefs, what you think is the right step for your loved one. Do they have an advanced care plan? Have they talked about what they would want if they ever were in a situation like that?

Those are all questions that need to be asked, and they need to be asked and answered on your level, not so much on the intensive care team’s level. It is up to you to determine the future for your loved one. Intensive care team might want to stop life support. They might want to get palliative care involved. If you consider that as an option, think about it. Talk to them. But if you want your loved one to live, and if you want to give them a fighting chance, then you got to keep pushing on and try and get them out of intensive care as the next step and see whether they can go onto a neurology rehab and so forth. There are no right or wrong answers in this situation. It’s really a preference for you and your family, depending on the wishes for your loved one.
Other things that can happen in situations like that, temperature sometimes can be very high. As part of the brain also regulates the temperature and patients might end up with a high fever. They might end up getting cooled. They might end up on a cooling mattress or on a cooling blanket to manage that as well.
Suggested Links:
So also, once your loved one is out of intensive care, or even if they can’t get out of intensive care but they’re more stable and they’re off inotropes, vasopressors. They’ve got the ICP removed, ICU stopped measuring the CPP, and they have a tracheostomy. You also may want to think about options such as Intensive Care at Home where long-term intensive care patients can improve their quality of life at home. Especially if they’re on a ventilator with a tracheostomy, you definitely should consider that as an option. And you can find more information there at intensivecareathome.com.
I usually always have those livestreams run for about 30 minutes because I think I’m very conscious of your time, conscious of my time as well. So, I try to condense the information into as little time as possible. And I’ve almost gone through all of my points now, and I really want to open up the floor for any questions. You can type them on the chat pad, and I’ll be happily answering them.
While I’m waiting for your questions, just want to quickly hone in again. This is a very complex issue and it’s also a very contentious issue. I can’t tell you how many families that I’ve seen in intensive care where the intensive care team wants to withdraw life support and families are opting against it. And there are these big debates going on, is it “in the best interest” for someone to continue treatment or is it not “in the best interest” for someone to have life support withdrawn? So, there’s no right or wrong answer. It really depends on what works for you and for your family. It really depends on, is there an advanced care plan and so forth?
So, that’s where I sort of want to wrap it up. Other topics that are coming up next week possibly is I have the same topic, “10 questions that you need to ask about hypoxic brain injury in ICU”. If your loved one has a hypoxic brain injury in ICU, I would do a livestream about that next week or the week after. Maybe want to do a livestream next week about intensive care at home. Again, if you look back through my livestreams, I’m doing different livestreams sometimes for Intensive Care at Home, and sometimes for families in intensive care like today. It really depends on what I want to talk about or what you are telling me you want to talk about or what you are telling me you want to hear about.
So, if there are no questions, I’m going to wrap this up very shortly. I want to thank you for coming onto the call. If you have a loved one in intensive care, you should check out intensivecareathome.com. Call us on one of the numbers on the top of the website or send us an email to [email protected].
Now, I do also offer one-on-one consulting advocacy for families in intensive care. Me and my team, we look at medical records. I talk to doctors and nurses directly, and participate in any meetings you have with the doctors. That’s all part of what I’m doing.
Now, I’ve got a question here. Mama Tried says, “Hi, my loved one’s pupils are reacting, he’s still sedated, and had sepsis. Is this the same thing as TBI?” No, it doesn’t sound to me like this is the same thing as a TBI. Did your loved one have any trauma to the brain? Did your loved one have a car accident with a head injury? Did your loved one fall off a roof? Was he in a fight, had the head punched, any of that?
While I’m waiting for your answer, so go to intensivecarehotline.com, where you can find more information about the services we are providing, which includes but is not limited to working with families in intensive care, one-on-one participating in family meetings, talking to doctors and nurses, almost providing like a second opinion and insights for you.
If you like this video, give it a thumbs up, please subscribe to my YouTube channel, and click the notification bell, and comment below what you want to see next and what insights you have.
Now, Mama Tried says, “It’s possibly meningitis.” Meningitis doesn’t qualify as a traumatic brain injury, assuming that meningitis is not secondary to a traumatic brain injury. So, can you rule out that your loved one had trauma to the brain, again by maybe being in a car accident, motorbike accident, falling off a roof, or having trauma done to the head maybe by a third party? Can you rule that out? Where’s the meningitis coming from? Do you know?
While I’m waiting for your response, also type underneath this video what topics you want to see so I can make a video about the topics that you want to see.
Recommended:
Then, Mama Tried says, “No trauma.” So then if it’s no trauma, then it’s not a traumatic brain injury. However, there are some similarities between meningitis and traumatic brain injury, because at the end of the day, it still impacts on the brain.
Again, Mama Tried says, “Points to viral meningitis”, sure. What can happen with the meningitis that is similar to a traumatic brain injury, patients can still have an EVD, and they can still have the brain pressure monitored. That is sort of similar. They can have seizures similar to what I mentioned before, but it would be a separate issue. You got to talk to the neurologist about the meningitis and how they’re treating it. Probably would be on some antivirals but have a look whether your loved one has an EVD in situ and an ICP, an intracranial pressure monitor, as well.
Well, thank you so much again for coming onto the call and for giving me your time.
Please also like this video, and again, subscribe to my YouTube channel.
I want to thank you for all your support.
There’s another message from Mama Tried and she says, “Brain waves are good. No seizures, no stroke.” That’s good. That’s excellent. That’s really excellent.
I’m going to wrap this up now.
Again, go to intensivecarehotline.com and call us on one of the numbers on the top of the website if you need further help. Again, we can participate in family meetings with the intensive care team and so forth and talk to the doctors and nurses directly.
We can review medical records and so forth.
RECOMMENDED:
Thanks again. I’m going to close this off now.
Thanks for watching.
This is Patrik Hutzel from intensivecarehotline.com and I will talk to you in a few days and in another livestream next week around the same time.
Take care.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!