Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Brother has COPD and Went into Cardiac Arrest. Is He At High Risk needing a Lung Transplant?
You can check out last week’s question by clicking on the link here.
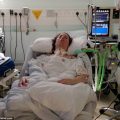
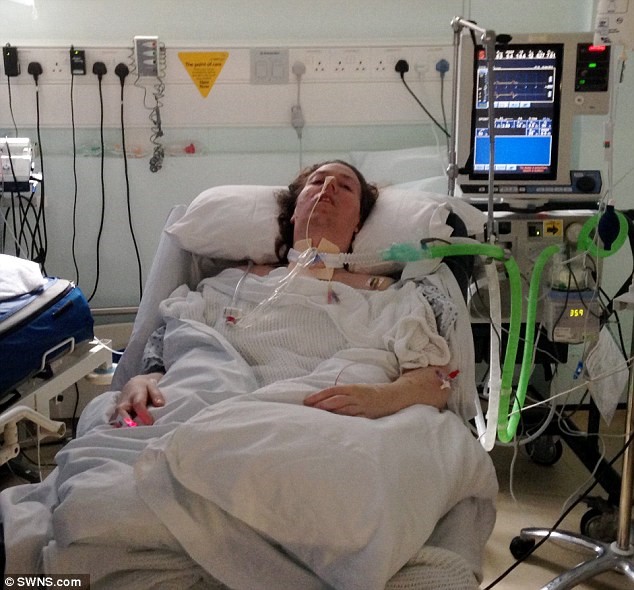
In this week’s episode of the INTENSIVE CARE HOTLINE Podcast I want to share the experience from one of my clients Carlos as part of my 1:1 consulting and advocacy service! Carlos’ mom had a cardiac arrest because of disconnected breathing tube due to negligence. The doctors told that her mom won’t make it but Carlos sought the help of Patrik of intensivecarehotline.com and was very happy that her mother was on full recovery now.
“People that are interested or listening at your website, they should know that it’s not about money or anything. It’s just getting the correct help, and you’re not going to get it from the hospitals because they’re on their own side. I’m glad that I did move forward and became your client. It was just wonderful”. – Carlos
INTENSIVE CARE HOTLINE PODCAST: My Mom Went on Cardiac Arrest Due to Negligence and the Doctors said that She Won’t Make It! Help!
You can listen to the podcast here or read the transcript below
Patrik: Hello, and welcome to the INTENSIVECAREHOTLINE.COM podcast. INTENSIVE CARE HOTLINE helps families of critically ill patients in intensive care to make informed decisions, get peace of mind, control, power, and influence. In today’s podcast, I want to interview one of our clients, Carlos. Hi, Carlos. How are you?
Carlos: Hello. I’m doing good, Patrik. Thank you.
Patrik: That’s great. Thank you, Carlos, for making time for this interview. I really, really appreciate it. Carlos. You first contacted me in August last year. At the time of this recording, it’s February 2019. You first contacted me in August 2018. I don’t want to do the talking because you have so much to share with our listeners. I know our listeners will benefit from your mother’s story. Carlos, if you can talk about your mom’s situation that would be really helpful.
Recommended:
Carlos: Okay. June 30th of 2018, my mom, she was complaining about stomach pain. She actually drove herself to the hospital. She was real healthy other than she has insomnia. When she went into the hospital, automatically they said, “Oh, we have to do emergency surgery. We have to remove your whole gallbladder.” My mom, she was real worried because she was already breathing not in a solid 100%. She had a little bit of breathing problems. She was doing treatment for asthma, but she didn’t have asthma, so she was worried about going through surgery. Sure enough, right after surgery, she got placement of the breathing tube down her throat, not a tracheostomy but the one that goes into her mouth.
Patrik: Yeah, a breathing tube, endotracheal tube.
Carlos: Yeah, and I think the hospital where she first went to, they didn’t really know how to deal with her, so they sent her out to another hospital, in Chicago, Illinois. She seemed to be recovering, doing pretty good, but they ended up having to put the trach through her throat. As soon as that happened, she started to recover a little bit. Go ahead, I’m sorry.
Patrik: Yeah, and I do remember because I just looked through all of our email exchange before the interview. I’ve seen that. I do remember when you first contacted me, she was, I believe, in ICU at the time or in LTAC. I can’t remember, but the short of it is that she was restrained, I believe. Then she probably disconnected her ventilator and ended up in a cardiac arrest. Is that correct?
Carlos: Yeah, that’s what happened. Now the doctors were not giving me true information. One doctor said there was only three minutes that he came into the room, and another doctor said he responded to my mother and that it was more like 11 minutes. When they brought her back, she was out for, I believe now through the history of the wreckage, that it was about eight minutes that she was without oxygen. She went into cardiac arrest. When they brought her back, it took a few hours. She started going into having seizures. Her whole body was just shaking real bad. Her arms were getting thrown up in the air. I do remember it was scary, but I sent you some of those videos so you could see what my mom was going through.
Patrik: Yes.
Recommended:
Carlos: I remember two days later, the neurologist from that hospital called me up, and she said, “I have to give you this news. Your mom is not going to make it. She’s not going to pull through this.” She was out, sedated where that was it. We weren’t going to see her. She was just asleep, like coma.
Patrik: Yeah. There have been many concerning parts in all of this, but the most concerning part to me was when you first contacted me. Basically, you mentioned that your mom was restrained, and because of that obviously she was agitated, because of that her ventilator became disconnected. She went into a respiratory arrest. She went into a cardiac arrest, and then potentially sustained a brain damage. That, to me, is gross negligence. How can you restrain a patient and then not watch them? If you restrain someone, then you need to have a nurse next to them at all times.
Carlos: Yeah, and in that facility, there was about nine nurses on duty around that time.
Patrik: Right, and just remind me, Carlos. When the cardiac arrest happened, was that in ICU or was that in a long-term acute care facility?
Carlos: That was in the LTAC.
Patrik: In the LTAC, right.
Carlos: She had got out of ICU and was in the regular rooms, but they had put her in the farthest room available. She had nobody really watching over her. When we would go in there to visit her, the patient next door to her, her alarm was going off. We counted 12 minutes. The people don’t respond. They weren’t responding to any of their patients.
Patrik: Yeah. No, that is so sad. I do remember then at the time, you sent me some videos from your mom. The videos you sent me, she had some seizure, some jerking movement. That is usually a sign for hypoxic brain injury which is what you’ve been told, as well, that your mom sustained a hypoxic brain injury. A few months have gone by and maybe can you elaborate on your mom’s journey since then?
Recommended:
Carlos: Yeah. Since then, she’s been into four different hospitals. It’s been real hard because I live 100 miles away from where they placed her. It was getting really hard to go and visit her. We noticed, too, when we weren’t there, the nurses, they don’t really care that she would be dirty. Sometimes she would be shaking real bad, and they forgot to give her medications. When you’re there visiting, right away they’re running around doing everything to try to impress you. If a lot of these hospitals just did their job correctly, a lot of things would turn out better.
Patrik: Yeah, for sure. I think that’s pretty much what you observed when the incident happened. If they had done their job properly, they would have noticed your mom becoming disconnected from the ventilator. Again, unfortunately I have no other words, but I believe that’s gross negligence.
Carlos: Right. Even some of the doctors in the beginning when I had told them that I had contacted you for medical consulting, I remember you talked to them once or twice.
Patrik: That’s right.
Carlos: Once they talked to you, Patrik, they were listening to an outsider, but when they talked to you, they were impressed right away. I remember the medications, when I gave you the list of all the medications, and you had me question them on certain ones, that’s when she started getting better, especially the last part where you told me about the humidified air.
Patrik: Yes.
Carlos: That’s what brought her back. The last hospital she was at, once she came into this new LTAC, remember I was scared of sending her there?
Patrik: Right.
Carlos: I tried to do all I can to keep her at the other place. Well, once she got here, she started to improve a lot. These people really started doing their job. Other than the therapy, they don’t help with the therapy, but that’s an insurance problem. That’s what I found out. That’s why they’re not helping her with moving her mobile and stuff like that because it’s insurance. They’re trying to say that she’s not responding to it, which is not true.
Patrik: Right, right. That’s something I do remember we talked about along the way. Whenever somebody needs to come off the ventilator that mobilising her is key. It’s absolute key to mobilise.
Recommended:
Carlos: Yeah. We started exercising her leg, my wife and my sister. Some of my aunts would go visit her and be lifting her legs real high. We got her a stress ball, and I told her, “Squeeze it all day. When there’s nobody here and you’re mad, squeeze this thing.” Now she’s using her cell phone to text us and send messages.
Patrik: Wow.
Carlos: She wanted to make that video thanking you so I said, “Okay. Well, let me get the camera out.” She knew exactly what to say.
Patrik: Right. That’s amazing. You mentioned earlier you had one of the doctors tell you your mom wouldn’t survive this. What were your thoughts at the time about this? What did you do with that message at the time when the doctors told you your mom wouldn’t pull through?
Carlos: When I got that message, I was with my wife, my sister, and my niece, and my son, which is her grandson. We were going to go visit her, and she called me and gave me that message. I was thinking, “How can I tell the rest? How can I give them a message that their grandma’s not going to make it or my mom?” Something inside … That’s the day I contacted you, Patrik, when she gave me that news that my mom wasn’t going to make it. That’s the day when I had contacted you because I said I don’t know that. I don’t feel that she’s going to go through all this and die, you know?
Patrik: Yeah. That’s why it’s so important, number one, to get perspective on a situation like that but also follow your own gut instinct. I’m sure it’s not only that you had other information through our website, but it’s also probably your gut feeling was telling you, “No. I’m not accepting this.”
Carlos: Right.
Patrik: You weren’t giving up, but even after that, even after that, I do remember the doctors told you that with a brain injury she wouldn’t recover. Even if she did survive, she wouldn’t be able to talk, to walk. Now when I saw the video last week, I was dumbstruck.
Carlos: Yeah. They told me that she wouldn’t recover. She wasn’t going to have her memory, and she wouldn’t even remember who I was.
Recommended:
Patrik: Now we need to let the listeners know. Your mom is talking now.
Carlos: Oh, yeah. She’s talking. She still has that little bit of shaking. That’s going to take some time. It may be wrong, but I even think once we get her home, we’re going to try to … What I was looking up is even maybe oxygenating drinks and therapy for your brain. That type of music that you play over and over and it just gets your brain working. I did a little bit of that with her, and she likes it. I know there’s hope for her to actually make a full recovery one day.
Patrik: Right. How did she start talking again? Was the speech therapy involved? Is that something that you and your family encouraged her to do? How did she get to that point?
Carlos: Yeah. Actually, the new place where we’re at, they put her in that newer valve. I forget what it’s called.
Patrik: The speaking valve.
Carlos: Yeah, the speaking valve. She was making some robotic sounds. She started laughing. She said, “That’s not me.” We started laughing. I said, “Mom, anything we hear coming out of your mouth right now sounds beautiful.” She started laughing. “I sound like a monster.” She knows it just cleared up. Her lungs started clearing up a little better. I know that when she has that valve in, she gets dry air into her lungs, so she knows. At night, she asks the nurses to take it out so she can have that humidified air.
Patrik: Yes, and what about mobilisation? Is your mom getting out of bed regularly now?
Carlos: No, no. They’re not helping her pretty much at all, so it’s all my family doing it. I got to try to talk with the insurance because they’re trying to say that my mom doesn’t respond to therapy. I know that’s a lie. She walked herself in that hospital, and she told me herself she wants to walk out.
Patrik: Yeah, that’s good to have a goal. It’s so good to have a goal. The last video that you’ve shown me, she was off the ventilator, just on the trach mask. Is she having time on the ventilator at all, or is she off the ventilator now completely?
Carlos: No, she’s off the ventilator completely. She’s just on an oxygen flow.
Recommended:
- What if you could reverse the Intensive Care team wanting to “pull the plug” or “withdraw treatment”
Patrik: That’s fantastic. I can see the improvement. I know you can see. She went basically from cardiac arrest to not waking up. Now she’s talking. She’s off the ventilator. The next step probably is to get her mobilised.
Carlos: Yeah, right.
Patrik: Another thing that I know our listeners would want to know is you mentioned you’ve been in four hospital now. We have helped some clients to change hospitals, but it can be very tedious. I’m sure it can be very tedious changing hospitals. What was your experience with changing hospitals? Was that difficult? What would your advice around that be?
Carlos: Well, I didn’t know how to do it the first time, and I wish I did because I could have got her out. Before she went into cardiac arrest, she was begging me to get her out of that hospital. She didn’t like it. She didn’t like the things that were going on there. The nurses, she said were real mean, and I didn’t know how to do it because I never learned. You think that you just trust the nurses and doctors to tell you what to do, but I found out I had to just talk with the main caretaker, the social worker.
Patrik: The social worker, yeah.
Carlos: Yeah, so once I talked with the social worker, she said, “Oh, okay, you want your mom moved. We advise that you leave her here, but if that’s what you want to do, then here’s these options. We can have her moved by tonight.” I said, “Okay, that’s what I want to do.” That’s why we moved from one place to the other. It was just because I just didn’t feel safe, her being there no more.
Recommended:
Patrik: Yeah. When you moved her, I do remember in the beginning you moved her from one place to another, but that was also the same hospital group. Did you step outside of that hospital group?
Carlos: Yeah. I wanted her to go to another facility and they didn’t want to. They pushed it. They had a social worker call me. The doctor came all the way from Beverly Hills in a golfing suit to come and talk to me to tell me to go to this one. They tried to keep my mom in the same circle of the hospital because they were worried about lawsuits or something like that. They wanted to keep her in their care. Sometimes that’s not the best thing for your loved one.
Patrik: No, not at all. I do remember in the beginning you had to travel 100 miles, like you said. It was a matter of proximity for you, as well. You wanted her as close to your home probably as possible.
Carlos: Right, yes. That’s been real hard for my family. My sister lived with my mom, so I basically would go pick her up and then we would travel together. My wife would go. Sometimes my kids would go, but it was costing so much money. I tried to do it as long as I can without people realising how much we’re spending, but I think I must have spent like 8 or $9000 in the last four or five months that she’s been in that hospital. That’s just fuel cost and my family eating lightly one lunch a day.
Patrik: Yeah. It’s very sad when things like that happen, and it’s very easy to give up, especially with all the obstacles that you’re facing. A lot of families have to travel unfortunately because sometimes those things don’t happen at the end of their doorstep. It is very costly. Nevertheless, the biggest lesson I would imagine is probably not to give up and continuing to pursue what you want against the odds because that’s basically what your mother was facing. She was facing a recovery against many, many odds. She defied those odds, really.
Carlos: Oh, yeah. She did. The doctor that told me my mom wasn’t going to make it, the main doctor chose her to come and tell me that my mom was pretty much going to make a full recovery, so she had to change her whole news and come and tell me three or four weeks later that from one bad news to the good news, that my mom was on the way to make a full recovery.
Recommended:
Patrik: That’s so fantastic. That is so fantastic. At the moment, Carlos, your mom is still in a long-term acute care facility. Is that correct?
Carlos: Yeah, she’s still in there because she still has a trach in her throat. She still has that shakiness, so right now they’re trying to wean her off to get the trach completely taken out. Then we’re probably going to have to do therapy at home to mobilise her, help her exercise. If we had her closer to us, we could do it a lot, intense and longer, but like I said, it’s too far. Now I’m only being able to go once a week. I communicate with my mom a lot on the phone, but she gets real sad when we’re not there.
Patrik: I can imagine. I can imagine. From my experience and perspective, the mobilisation part is huge because it sounds to me like your mom has basically been bedbound since July or August.
Carlos: Seven months now.
Patrik: Yeah, and it will be difficult for her to start walking again. It’s not going to be impossible, but the longer they don’t mobilise, the more difficult it gets.
Carlos: Yeah. Actually, my mom, she’s doing her own exercise. She doesn’t wait for the therapy to come in. She’s lifting her legs three or four inches off of the bed, one at a time. She turns her body. She lifts her arms up real high in the sky till she gets tired. Like I said, she has a stress ball. She’s squeezing it, so she’s doing her own therapy. She’s determined to walk out of that place and prove everybody there wrong.
Patrik: Absolutely, absolutely. Yeah, as I said, the mobilisation part needs to be next. You are saying that it’s an insurance issue that the insurance is not paying for that part? Is that what you’re saying?
Carlos: Yeah, so that’s what they’re doing. They’re just coming in and asking her to lift her hand a few times and lift the other arm two or three times. Then they walk out. I called the social worker, and she said, “Well, basically it’s the insurance.” They’re not paying for full therapy, which I don’t understand why they wouldn’t. My mom walked herself into the hospital.
Patrik: Exactly, exactly.
Carlos: We didn’t bring her in in a wheelchair.
Recommended:
Patrik: That’s right. One thing you can look at, Carlos, is your mom must have a care plan. The doctors and the nurses must have documented a care plan. I can’t imagine that mobilisation would not be part of that care plan. Walking is an activity of daily living that needs to be part of that. What you could do is you could ask for the care plan. Once you see the documentation of goals of care, one of the goals of care would be mobilisation. You could go back to the insurance and you could say, “Hey. This is part of the goals of care. It needs to be funded.” It’s also like imagine your mom can go home walking. It would also save cost for the insurance down the line. If she can’t walk, she may need home care. It’s probably making the argument along those lines in terms of long-term outcomes.
Carlos: Yeah.
Patrik: The other thing that I do remember from last year and from the conversations we’ve had, I believe your mom is about 56 or 57 years of age. Is that correct?
Carlos: Now she’s 62. She turned 62. She had her birthday there in the hospital.
Patrik: Oh, okay. That’s great. That’s very young. People live until 80, 90. It’s very young. It’s not that age should ever be a determining factor, I believe, whether you should continue treating someone or not, but it just shows anything is possible.
Carlos: Right, exactly.
Patrik: Carlos, was there anything else that you would like to add? Was there anything that you think was important as well that we haven’t talked about?
Carlos: Well, you know what? I feel that I got a lot of the confidence talking to the doctors and stuff with your help, so a lot of other people that are interested or listening at your website, they should know that it’s not about money or anything. It’s just getting the correct help, and you’re not going to get it from the hospitals because they’re on their own side. They are for themselves. A lot of times they know what to do, but they’re not going to do certain things unless you ask or you know about it. I’m glad that I did move forward and became your client. It was just wonderful.
Patrik: Thank you for those kind words. I can only emphasise the biggest challenge for families in intensive care is simply that they don’t know what they don’t know.
Carlos: Right, exactly.
Patrik: That’s the biggest. Once you have a clinical person on your side that can talk to the doctors, negotiate with the doctors it’s a game-changer, I believe.
Carlos: Yeah.
Patrik: It’s a game-changer, but look Carlos, I really appreciate you taking the time out of your busy schedule to share this with our listeners.
Carlos: Okay, thank you. Thank you so much.
Recommended:
Patrik: Thank you so much again for taking time out of your day. This is the INTENSIVECAREHOTLINE.COM podcast, and I want to thank Carlos once again. Go and check out our case studies at INTENSIVECAREHOTLINE.COM and where you can also get one-on-one consulting and advocacy if you have a loved one in intensive care. Thanks again, Carlos, and we’ll talk soon.
Carlos: Thank you.
Patrik: Take care. Bye-bye.
Carlos: Bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!