Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Will We Know If It’s Time To Stop Life Support For My Sister On A Ventilator?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Cathy, as part of my 1:1 consulting and advocacy service! Cathy’s dad is critically ill in ICU but eventually passed away. Cathy is asking what dying in dignity means to the ICU team who pushes withdrawal of treatment.
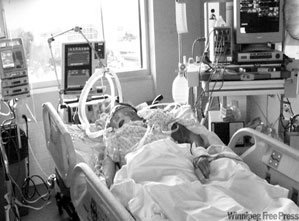
What Does Dying In Dignity Mean To The ICU Team Who Pushes Withdrawal of Treatment?
Patrik: Hello Cathy! How are you?
Cathy: Oh thank you Patrik.
Patrik: Okay Cathy, I’m sorry about what happened to your dad.
Cathy: Yes. But I’ll tell you part about how it happened.
Patrik: Right.
Cathy: Because he passed away at home.
Patrik: Oh, okay.
Cathy: With me holding his hand.
Patrik: Right.
Cathy: And it did not… it almost didn’t happen because… I can’t remember the last time I talked to you so-
Patrik: November. Would have been November.
Cathy: Okay. So, because he was doing…he was breathing spontaneously… Again he was not conscious. He… not interacting with you in that… it was anyone in that way. But because he was breathing spontaneously on his own, on the ventilator, they thought that he would… they could wean him.
Patrik: Right.
RECOMMENDED:
Cathy: So I did that and I was like look, because I kept getting these weird answers because I’m like, can you wean someone if they’re not conscious? If they can’t tell you how they’re feeling, even though they’re breathing spontaneously but they’re not responding, can you wean them? And they just never answered the question.
Patrik: Yep.
Cathy: And it’s clear to me now that the answer is no. And I told them, I said look, when you figure out that he’s not going to wean that meant it was three days, he’s coming home. I don’t know how many times I have to tell you people that I’m trying to do this in a way that’s consistent with my faith. If you disconnect the ventilator I consider that to be killing him because all of his organs were still working. That’s what was totally throwing me. I mean he wasn’t taking any vasopressors or anything like that. No blood pressure medicine, nothing, everything was working, he just wasn’t responding. And they couldn’t say that he was brain dead because when you put him in that spontaneous mode he could breathe on his own. I know volumes weren’t very good but he was still so breathing on his own. So, of course, because his insurance company… he had good insurance, was going to pay 28 days. They kind of led me along until..
Patrik: Yes
Cathy: So that was another wasted three weeks. But he fought that off. And then I was able… and then they tried to lock the place down. I was like no, he’s getting out of here. I don’t really care. I mean, the thing about all the worst part of all of this were the people in the medical establishment that I had to deal with.
Patrik: Yes.
Cathy: They were so rude and nasty and not listening to what you’re saying. I tried to explain to them… I said, when I started this with I put all my heart and specific scripture, it talked about how he breathes life into us and we become a living soul. So life is just not about the fact that he’s not acting to me in the flesh. His spirit is still doing something. For whatever reason God controls the situation here. And I’m supposed to maintain that and when he calls him from the spirit world, there’s not going to be anything any of us can do. And that’s when he’s… that’s when he’s meant to go. And they just so need that.
Suggested links:
Cathy: And then he had to go back. And so we went… he spent a couple more days in the hospital. I got him home two and a half weeks after. Then he was having problems with his oxygen levels, went back, and he was… seemed to be getting better. And then he just started crashing and his stomach… he could… he was aspirating all of the tube feedings and they took him off the tube feedings. So started happening and, it was just confusing me because the next weekend they were like, oh if only he had gotten better. I think they’re trying to do this and at the same time they’re telling me, oh this is the end.
Cathy: … then they were trying to give him this other test. And I’m like, “I already told you all, we’re not doing any tests. We’ve already determined that he’s gotten to a point we don’t want him bothered to that point. His oxygen levels weren’t good, try to fix that, then he can come back.” And I’d gotten into it with the doctor because he… Because I guess they wanted me to say, “We’ll cut the ventilator off.” And I’m like, “I don’t know how many times I have to tell you all this, I’m not going to do that. And I understand that you think that he’s brain dead.” I said, no, I told him, I said, “I know that you can’t declare him brain-dead and it’s frustrating, but I can’t help it that he’s still breathing on his own. And I’m not trying to keep him here.”
Recommended:
Cathy: I said, “If there’s something that happens to him, I know that he’s prone to infections because of the tracheostomy and because he got a bit sore in the hospital, I understand all of that. Your job is to tell me if medically there’s something that can be done. And then he gets stabilized, then he goes home. I’m not here for you to try to fix my dad. We’re at the point where that’s up to God, but I still have a responsibility to bring him in, to see if there’s something we could do.” And he just… And I told him, that I once told the doctor, “Brain dead is not dead. I don’t believe in you guys, so you can give that speech someone else.” My dad, so he would respond through his heart rate to people being in here. Because my dad-
Patrik: Of course.
Cathy: He was not going to a nursing home, he wasn’t going to an assisted living, he did not like people in his house. So when someone would come to service the ventilator, his heart rate would just, he would just get annoyed if they were here for too long. And nothing happened because my dad knew that was family. And I’m like, “These people are not dead.” I said, “There are two components of life. Again, that’s consistent with my faith. And how many times I have to tell you this. If he has an infection, can you cure it? If not, he can go home. We don’t need to stay in here and deal with this.”
Cathy: So he was just very upset about that. And he said something to me and I said… Oh, he was kind of annoyed because I was like, “Well, he can go back home. I’ve been taking care of him for two months. And he needed to just go back home.” And he said, “Well, as a doctor…” Oh this is what happened. He started aspirating and then he cut off my dad’s food and water because he was aspirating. And I was like-
Patrik: Yes, I remember you saying that in the ER.
Cathy: Yeah.
Patrik: Yes.
Cathy: And so I said, “Fine, if this is the end, he can go home.” And he’s like, “I need to talk to your sister.” And I’m like, “Why do you need to talk to my sister?” I said, “First of all, this is a decision for the family to make. Your role is to tell me medically what is going on. And then we as a family, make that decision. And how that happens, doesn’t have anything to do with you. What is wrong with you? What is wrong…”
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Cathy: I mean, I said, “If you’re telling me this is in, you’re not going to give him any food and water…” I’m like, “One minute you’re telling me the pneumonia is getting better and the next minute you’re getting worse, but you don’t know why.” I said, “He can come home.” And I said, “This has been my position from the beginning. Nothing from the start when all this happened. It has not changed. And you all just…” I was like, “I don’t know if you want to get his organs, not happening. I don’t know what your issue is that you can…” “Well, people just don’t do this, people just don’t give up their lives.”
Cathy: I said, “But I’ve been doing it”. And I shouldn’t have… And I was like, “It’s not your concern.” It was the hardest thing, because again, my father was very,. I’ve realized from this experience, he was, and a lot of older people are like this too, it’s like, you are not taking control. It’s like my dad had full confidence that my sister and I would make the right decisions. I never had a problem with managing his money or anything like that. But he wasn’t going to sign a paper that kind of gave up his rights. And yeah, he wasn’t going to do… He was like, “I know you’re going to do what’s right.” He said, “But I’m not signing any paper doing that. I’m going to maintain my right to myself the entire time.” And I totally understand that.
Cathy: And it’s like, these laws, because it was like pulling teeth from them because I didn’t have power of attorney, but I was still next of kin. And it’s like they were trying to use it as an excuse not to say anything. And I had to dig to get anything out of them. And I’m like, “You’re trying to make decisions that are not decisions for you to make. And you can’t even do what your job is supposed to be, which is diagnose and tell me whether you can treat or not. Why are you wasting my time? You’re crossing the line.” And he just was… So that happened on a Friday. Then Saturday I came in, my dad’s stomach was just a balloon, just started ballooning up. But then I came in on Sunday and they took him down for a brain scan.
Cathy: I’m like, “If you’re saying this is the end…” And we sat down and had this long conversation, this conversation about, “Well, this is happening, his stomach is swelling up, but because you don’t want to do tests, you don’t want to do anything invasive, we can’t figure out what’s going on.” And I’m like, “Yeah, because I told you, we’re going to accept what the decision that God makes. And these are signs that we’re winding up. And as I said, he can go home.” And even after I said all of that, even after I said, “I’m going to do this in a way that’s consistent with my faith.” Even though the insurance company, you’re not paying for a 24 hour nurse, I took on that expense and that responsibility to be his nurse and then hire other people to come in and help me when I needed to work a little bit. This nurse practitioner still stood up there and said, “And if as you need for us to make this happen, medically, we can do that for you.”
Patrik: That’s horrible. That’s horrible. Isn’t it?
Cathy: I was like, “This is worse than dealing with what is going on with my dad. And I just can’t… And the other nurse, the charge nurse was just in tears after I kind of got into it with the doctor. And he’s like, “You bring up so many valid.” I was like, “This whole medical industry thing that you all have gotten going on is evil because you are just overstepping your bounds and you’re making this worse than it has to be.” Then my sister was like, “It’s going to be too hard on him if you take him home, and you have to come there when he passes on.” “Okay, fine. So he can stay here, I’ll just stay here with him.” And all midnight they just ignored him. There was a point when his oxygen was tanking. I was like, “Oh, so we’re just going to sit here and ignore that the oxygen is just tanking right now.” So I know how to use the ventilator, so I’m changing settings and I’m telling them to come in and they’re just ignoring him.
Recommended:
Cathy: And I called my sister back and I said, “I cannot do this.” I said, “I cannot. Even if I’m sitting here, this is not going to happen in this place where people were just going to sit here and ignore that this was happening. And then call me in the morning and say, ‘Oh, your dad passed last night.'” I’m like, “I’m not doing it.” And I was just balling over the phone. And my sister was like, “If you think you can handle it, then just take him home.” And so I got him home Monday. He stabilized. All of his oxygen up or whatever, he stabilized. And then right when we were supposed to talk on that Tuesday, because I was just going to ask you because they were confusing me about, “This is the end,” but you’re still taking him for tests.
Patrik: Yeah, yeah.
Cathy: And when I not do that. And I was like, “Is it really the end? What is going on?” That’s what I’m going to talk to you about like, “Is this really the end?” My father hasn’t had any even water in two days, but God was very clear. And around 5:30, his heart rate just started dropping, oxygen started dropping. I called the EMTs just to call them. And they’re like, “Yeah, there’s nothing else that we can do unless you want to take him to the hospital.” I’m like, “No, he’s not going to the hospital. There’s no reason.” And 9:30 that night he passed. And I can definitively say that when he passed, there was a toll difference between that and what I experienced when he was on the ventilator. When he was on the ventilator, whether he chose not to wake up, whether God was talking to him in the spirit world and he was trying to convince him, ” don’t want to go back there,” or whatever, he was not dead.
Recommended links:
Cathy: Even though he wasn’t responding to your voice, he would respond to stimuli. He was not dead. And cutting off that ventilator would have been killing him. And I told him, I said, “When God takes him, he will be on this ventilator and it’s not going to help at all.” And that’s exactly what happened. And so the next, which happened 9:30, and I kind of took my time, spent time with him. All these things that they do in hospitals and I’m like, “If you could do that, you’re not family.” And they don’t want you to do that. And then I call the police the day, they came, and they were just like… Because I had a whole ICU up in here and they were like, “Oh my goodness, we have never seen anything this organized.”
Patrik: Wow.
Cathy: They were just like, “We have just never seen anything like this. This is so clean. You just really took care of your dad.” And I’m like, “Why would you bring someone home if you’re not going to take care of them.” And all of them, and the police officer came in and he’s like, “Why didn’t you call us when this happened?” I was like, “Look, someone died. From what I’ve been told, when someone dies, it’s not an emergency. Everybody in my dad was sick and everybody knows it. He said, “But if this is the process that I have to go through to have kept hospice from coming in here, trying to make the case, that it’s time for them to help my dad go along and shoot him with morphine, that’s what we’re going to do.” So yeah, that’s how it ended, but the whole process, the medical establishment, it just needs to go off of a cliff. I don’t know what they’re doing, it’s like torturing people.
Patrik: Oh, yeah. Can I just-
Cathy: yes.
Patrik: Thank you so much, first of all, for sharing all of this, this is very, very valuable. One thing that struck me is, and it would have struck you as well, but I just want to sort of dive a little bit deeper there. You mentioned the nurse practitioner mentioned to you, “Oh, yeah. If you don’t want to do this, we can take care of this medically,” or something along those lines. I mean, basically what they’re implying is, “Well, we can kill your father softly,” such a thing. And that’s euthanasia.
Cathy: Yes. Yes.
Patrik: That’s how desensitized they are.
Cathy: Yes. And you just cannot have, you just can’t be in that environment. And it’s like you just wanted to stay there, because the only reason I can think that they took him down for the brain scan… And I’m like, “There’s no reason to take him down for a brain scan. I know how this works. If you turn the ventilator off, my dad starts breathing on his own.” Before he passed, the last hour before he passed, he was breathing on his own. And then when he passed, he stopped. I was like, “I don’t know why you keep doing all of these tests. He’s not brain dead, according to your definition. He’s not.” But it’s just like they just wanted to keep them there so they could kill them. I’m like, “This is sick.”
Suggested links:
Patrik: And to do another test to make money. I mean, that’s a relevant question, isn’t it?
Cathy: Yeah. And that was a frustrating thing for me. It’s like, “I’ve told you all over and over again, I’m my dad’s 24-hour nurse. His place is at home. I still have an obligation because this question about…” I knew that my dad hated doctors. He wanted to do everything naturally, all of that, but what he didn’t… But what happened, the position that I was in, or my sister and I were in is when he wouldn’t make clear. And I tried to talk to him about it. He never made clear, “Okay, if you’re on a ventilator or that type of life support, what you want us to do?” He just never made that clear. So I had to just rely on, he raised us as people of faith, what did my faith tell me? And it was, “Look, if all these organs are working, he’s not taking any drugs. I still have his there for a reason and it’s not time for him to go yet. So you need to do everything you need to do to maintain that.”
Cathy: And you don’t allow them to define for you, what type of life is worth keeping. You don’t kill him. And this was the lesson in it to me is, you just can’t listen to these people. And I said, “A lot of people just aren’t aware of it because you don’t stick through it until the end to see the difference.” You can never convince me about someone being brain dead in that situation, because I saw how my father was reacting, not reacting, on the ventilator, and I saw when he passed. And those were two totally different states. And his passing was not the same as when he was on that ventilator. And for whatever reason that God kept him here for those five months, six, seven months, is not really for me to know, but it was for me to continue to be faithful to his word.
RECOMMENDED:
Cathy: And so that’s why I have a lot of peace about it, even though I … As to be expected, I have my breakdowns throughout the day. Just, it’s odd, not walking around and he’s there and all of that. But my message just to anyone that will listen is, these people, these hospitals, this medical establishment, they’re just about killing you. They don’t have any empathy for you. It doesn’t matter how you lay it out, they don’t listen. And as I said to them from the beginning, I never wavered in what I wanted you to do. And that’s what I told her. I said, “I have hired you to do a job, and you’re overstepping your bounds. I said, “You’re trying to tell me what I’m supposed to think about the situation, and it’s just not for you to do. And if I say that I’m going to take care of my father, you don’t need to worry about how that happens. As long as I’m doing the best that I can to take care of him. He’s not staying here. I don’t want him staying here.”
Cathy: And as I tell anybody, it’s like, “If I can figure out having zero knowledge of ventilators and figure out how to do it and keep my dad here and figure out how to have people in to help me.” I was like, “It’s not easy. It’s not going to be easy, but you’ll have peace about it in the end that you did what was right in the sight of God. And you did what was right by them because those people don’t care.
Patrik: No, no.
Cathy: They don’t care.
Patrik: No. I’m sure the whole discussion launched or instigated from your end around what you believe is right for your dad fell on completely deaf ears.
Cathy: Yes. Yes.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!