Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
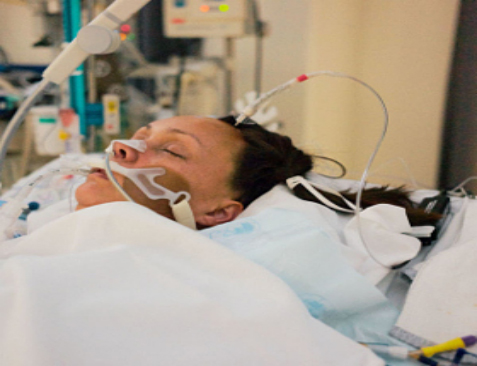
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tara, as part of my 1:1 consulting and advocacy service! Tara’s mother was admitted with a leg infection only and Tara is asking why her Mom is ventilated now with a tracheostomy and cannot be weaned.
My Mom was Admitted with Leg infection Only But How Come She is Ventilated Now in ICU and Cannot Be Weaned?
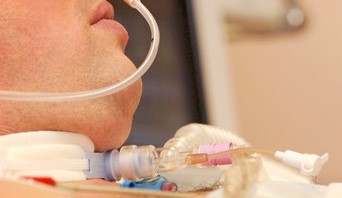
Tara: Hello?
Patrik: Hello. Is this Tara?
Tara: Yeah.
Patrik: Hi Tara, it’s Patrik here from Intensive Care Hotline.
Tara: Yeah.
Patrik: How are you?
Tara: How are you?
Patrik: I’m very well, thank you. How are you?
Tara: Good.
Patrik: You have a family member in intensive care.
Tara: What was that? Yes.
Patrik: Right
Tara: Unfortunately I have another call coming in and it’s beeping. Let me just see who it is. I can’t even read it but that’s alright, hopefully they’ll hang up.
Patrik: Right.
Tara: There we go. Okay.
Patrik: Right and you can hear me well? The connection is good?
Tara: Yeah.
Patrik: Yeah, I can hear you well too.
Tara: Yeah. .Yeah.
RECOMMENDED:
Patrik: So the way I operate is I always have 15 minutes of my free time. We can go through your situation, see how far it takes us. Anything beyond the free 15 minutes, I have options available against a fee. Obviously, I have paid consulting and advocacy options available.
Tara: That’s fine.
Patrik: If you want to tell me what you’re dealing with, then I can tell you how we can help.
Tara: Well, it’s my mother and she’s having difficulty getting weaned off the ventilator she’s been on. She had a tracheostomy done three weeks ago now.
Patrik: Right.
Tara: And pretty much the respiratory therapist has basically said he can no longer even work with her.
Patrik: Right.
Tara: Because the last time he tried to start the weaning it only lasted seconds and the alarm started going off.
RECOMMENDED:
Patrik: Okay. How long has your mom been ventilated for?
Tara: Well, she had the tracheostomy three weeks ago and so two weeks before that was… Or a week and half, I guess, was the full tube so we’re looking at five weeks now.
Patrik: Okay and at the moment, is she still in ICU or is she in a LTAC?
Tara: Well, she’s in critical care recovery unit of a hospital.
Patrik: Sure, sure. Any talk about going to LTAC? Do you know what I mean by that?
Tara: Not at all.
Patrik: Okay. So what happens often is when patients are in ICU and they receive a tracheostomy and they can’t be weaned off the ventilator, they often end up in LTAC, which stands for Long Term Acute Care facility.
Tara: Oh, it’s like a nursing home?
Patrik: Well, it’s a euphemism for nursing home.
Tara: Right. Yeah.
Patrik: It’s a nicer word.
Tara: Yeah that is. Then they have talked about that. Right. That is unfortunately, we have to make a decision whether to send her there or just to give up.
Patrik: I hear what you are saying but one of the biggest challenges in a situation like that, is you will need to change your vocabulary and by that I mean, you’re saying that you will have to make a decision and I tell you that you don’t have to do anything. It all comes down to asking the right questions and it all comes down… At the moment, your biggest challenge is that you don’t know what you don’t know. The way they’re framing this to you is, you have to make a decision. That’s not accurate. Right. It sometimes can take time to wean somebody off the ventilator and just because it hasn’t happened now after three weeks, after a tracheostomy, doesn’t mean it’s not going to happen. What they are implying however, is that they can’t do it and they can’t do it… And more importantly, what they’re not telling you that they can’t do it in a time frame that is convenient for them.
RECOMMENDED:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Tara: Okay, well, pretty much I agree. I mean… I’m starting to have my doubts that she can even be weaned but. .
Patrik: Why did your mom end up on the ventilator in the first place?
Tara: Well, she has a lot of problems. She went in the hospital for cellulitis. She had cellulitis in her legs and a urinary tract infection so she was septic. So they started her with a bunch of fluids and then they said she wasn’t able to control her secretions. I think every time they wanted to try get the secretions, her blood pressure was dropping and that’s when they decided they had to intubate.
Patrik: Okay.
Tara: And then, go ahead.
Patrik: Any other significant pre-medical history?
Tara: Yeah. She has Parkinson’s. She has COPD.
Patrik: Oh, I see.
Tara: Yeah.
Patrik: How bad is the Parkinson’s?
Tara: Well they call it end stage but I can’t really figure that out because technically you don’t die from Parkinson’s.
Patrik: When you’re talking to your mom, does she recognise you?
Tara: No. She is now, not even woke up in three weeks because her CO2 is so high.
Patrik: Okay.
Tara: And that was the other thing we were looking at, was trying to… There’s a machine called the Alung but it’s still in trial stages and it’s basically like a dialysis for the blood and it takes the CO2 out.
Patrik: Yeah, yeah, yeah.
Tara: Yeah, but we were having trouble getting hold of them, however my brother’s working on that part of it.
Patrik: She’s on that machine?
Tara: No. No, we would like to if we could. . .
Patrik: Okay.
Tara: Find one near us that would accept it because it’s has been approved in Canada, but as far as I know, it’s not approved in the United States yet.
Patrik: No, that machine is approved in the United States. It’s also called… Have you heard of ECMO?
RECOMMENDED:
Tara: Yes.
Patrik: Right. Look I can send you a list of ECMO centres all around the world, there’s plenty of ECMO centres in the U.S.
Tara: In America, though?
Patrik: Oh, yes. I can send you a list when we come off this call. There’s plenty.
Tara: But what I’m not sure whether they would accept her.
Patrik: I’ll tell you what the challenge might be, the hospital where she is currently at, they might not have that ECMO because it’s usually… Every sort of big city… I don’t know where you are exactly but every big city has at least one ECMO centre, at least.
Tara: Yeah, yeah.
Patrik: Okay.
Tara: I asked about it and they said she didn’t qualify for it. But they don’t even have it there.
Patrik: Exactly, exactly. What would they know? I can tell you over the years. I looked after many, many patients on ECMO if CO2 is an issue.
Tara: That seems to be the biggest issue right now because she won’t wake up.
Patrik: Right.
Tara: And if she doesn’t wake up then she can’t actively participate in the weaning process, which makes it even more difficult.
Patrik: And are they still sedating her? Do you know what I mean by that?
Tara: No, I didn’t hear you. What was that?
Patrik: Are they still giving her any sedation? Do you know what I mean by that?
Tara: No, no. No sedation.
RECOMMENDED:
Patrik: Okay, okay. And no pain medicine either?
Tara: No.
Patrik: Okay. What are you trying to achieve? What outcome do you want to get in this?
Tara: Well, we would hope that we could reverse it and she could maybe come home with a tracheostomy. I’ve done a little bit of research on that too and if our only problem was controlling secretions, they make just a button, and so you don’t even have to have the full tracheostomy. So, the button allows access to go in and suck the secretions out but you can talk and eat as normal.
Patrik: Yeah, sure but that’s only if she was off the ventilator.
Tara: Right, but that’s what is so infuriating about this whole thing is that I don’t think she even needed to be on it. Because she wasn’t having any problems eating or swallowing before this. They only said she needed it because she wasn’t being able to control her secretions. It was exacerbated because she was septic and they were pumping her full of fluids and not taking anything off.
Patrik: Right. Does she have a weak heart?
Tara: It’s not the greatest but it was under control.
Patrik: How old is your mom?
Tara: What was that? How old? Seventy-eight.
Patrik: Seventy, that’s not very old.
Tara: Well, she’s not a spring chicken. She had a lot of issues going in. We understood all that but I just feel like this whole thing got… It went really quickly, it just escalated. And like I said, she went in with a leg infection and now five, six weeks later she’s on death’s door with a breathing tube stuck down her throat. Well, she was walking when she went into the emergency room… Walking, talking, eating, swallowing and everything.
Patrik: Absolutely.
Tara: And now they’re saying she can’t breathe because she’s been on… Because it’s been so long that she’s on this thing that her lungs have become weaker.
Patrik: Yeah, yeah. And every day where they’re not being proactive of weaning her off the ventilator. It’s a big risk that it’s getting worse, not better. I’ll tell you how we can help in a situation like that. Number one, I really understand the situation and it’s not good enough to say they don’t have the machine available or they can’t remove the CO2. That is not good enough because it sounds to me like that’s the biggest problem. Right? The other thing, the other problem that I can see, there is certain things you can do when you have somebody on the ventilator to get CO2 down. I would like to know whether they are doing that or not.
RECOMMENDED:
Tara: Yeah. They said they could but for one, they’re afraid. They don’t want to give her too much oxygen because then you change the pH and become acidic, so that’s not good. And they said, if they do try take the CO2 out, they’re afraid it’s just going to come right back.
Patrik: You see giving more oxygen is not getting CO2 down. There’s other things they need to do. If you look at the ventilator, for example, there’s twenty numbers on the ventilator and there’s a few of those numbers that you can adjust and then potentially get CO2 down. Do you know how high your mom’s CO2 is? Have you got a number?
Tara: A hundred and one.
Patrik: A hundred and one?
Tara: Yeah, the other day. Yeah.
Patrik: All right. That’s really high. Okay. And it’s been like that for many days?
Tara: Well apparently, but here’s the thing they’ve only tested it twice since she’s been in there. So we don’t really know.
Patrik: Right, right, right. And let me ask you one more question. Are they getting your mom out of bed? Are they mobilising her?
RECOMMENDED:
Tara: They’ve tried to. They have therapist that comes in, do a range of motion and they tried getting her, sitting her up but she is completely asleep so they’d see she wasn’t tolerating that.
Patrik: Okay.
Tara: That’s why I kept saying if they could get her awake so she could participate in her therapy and stuff more.
Patrik: Yes. Absolutely. Who is in charge of her overall care? Is this the pulmonologist? Is this an intensive care specialist?
Tara: There are two doctors. Yeah. One doctor is in charge of the whole patient and then there’s a doctor, the pulmonologist.
Patrik: Okay. Because it is important for you to find out who is taking responsibility. Are you getting regular updates?
Tara: Yes, I’m there every day.
Patrik: You’re there every day?
Tara: Almost every day.
Patrik: Right, right. And they’re talking to you? They’re not avoiding you?
Tara: No. No, but it’s very hard when they make their rounds. They come through and I realise, they saw a lot of patients and all that but really you try and ask as many questions as you can. Then it’s as if they’re allotted and as soon as they walk out the door you think of ten more. It’s a little bit difficult but no, they seem to be very nice and they’re not avoiding me.
Patrik: Okay, okay. Now that’s good. That’s good. And any talk about potentially not continuing treatment? Any talk about DNR? Do you know what I mean by DNR?
Tara: Yes. Do not resuscitate.
Patrik: Yes.
Tara: Yeah.
Patrik: Any talk about that?
Tara: They haven’t asked to have her status changed but they’ve asked me what we would do. And I said, if we ever run out of complete options then I do not want her to go to a nursing home or whatever you want to call it. Therefore, we were talking about end of life hazards.
Patrik: But at the moment, is she in full resuscitation?
Tara: She is. She is full resuscitate. Yeah.
RECOMMENDED:
Patrik: Okay, okay, okay. As I’ve said the one way to remove the CO2 would be to look at ventilation settings. You do not decrease CO2 by increasing oxygen. It’s not happening. There’s other things they need to do. And the other option would be definitely ECMO. Right. Whereabouts are you? You’re in Vermont?
Tara: Yes.
Patrik: And where in Vermont?
Tara: Rutland.
Patrik: Oh, in Rutland. That’s up at. .
Tara: Rutland. Yes. Northeast
Patrik: Up at the lakes, isn’t it?
Tara: Yes.
RECOMMENDED:
Tara: I guess. I’m sorry, what we would be planning on doing and so, one thought my brother and I had, was if she wanted to end her life we would like to bring her home.
Patrik: Yes.
Tara: And number two, the other reason I am interested in your services was to see if you could do anymore at home that were not getting in the hospital.
Patrik: Yeah, yeah, yeah. For sure. For sure.
Tara: So that’s why I reached out to you.
Patrik: I see, I see. Yeah. Look, we take patients home on ventilation and tracheostomy, we’ve certainly done that and it’s part of what we do. The other question is, do you know whether she’s on any other forms of life support besides the ventilation? Do you know that?
Tara: No.
Patrik: Are you sure?
Tara: No.
Patrik: She’s not on any Vasopressor? She’s not on any medication that’s supporting her blood pressure?
Tara: Oh. I’m going to have to look into it. She’s always been on a blood pressure medication. I don’t know what they’re giving her right now. We went over it in the beginning and now I can’t remember. I know they cut a lot of her meds out and were just giving her the basics. I know they’re giving her three Parkinson’s medications but I can’t remember if they’re still doing the blood pressure medication.
Patrik: Okay. Because if they do, that would be prohibitive of taking her home. Because that’s why I’m asking, if they do give her blood pressure medication it’s considered life support and that would be prohibitive to take her home at this point in time.
RECOMMENDED:
Tara: Would be perfectly, what?
Patrik: It wouldn’t be doable to take her home.
Tara: Doable?
Patrik: Yes.
Tara: Oh. Because of blood pressure medication?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!