Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s PatrikHutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Loved ones in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Is the ICU Team Allowing My Brother to Die by Giving Him Heavy Sedation? Help!
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions that we get quite frequentlyas part of my 1:1 consulting and advocacy service!
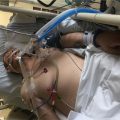
TRACHEOSTOMY IN KIDS (Part 2)

A tracheostomy may be permanent, long-term or short-term, depending on the needs of your child. Your child will have regular medical appointments, and the removal of the tracheostomy tube will be planned once the medical team is confident that your child can breathe well without it.
Before it is determined that your child no longer require tracheostomy tube, your child’s doctor may conduct trials to determine how your child tolerate breathing through the nose and mouth again. These trials are usually done via two methods: weaning or capping. Often times, capping will be conducted at the end of a weaning trial to ensure your child is ready to return to breathing through the upper respiratory tract.
WEANING

This process can be conducted various ways, although the most common is to begin by using a Passy-Muir Speaking Valve (PMV) if your child is not already using one. The PMV requires your child to exhale through the nose/mouth while still allowing them to inhale via the tracheostomy tube.
In this sense, your child can breathe only partially through the tube which serves as a good determinant in assessing if your child may be ready to be decannulated. Although not always, if your child is unable to tolerate the PMV during prolonged use throughout the day, it is unlikely your child is not ready to be decannulated.
In some cases, weaning from tracheostomy tube may also include down-sizing; which means your child’s current tracheostomy tube size is exchanged to a smaller size. Essentially, the space your child have to breathe through the tracheostomy is made smaller, usually requiring more respiration activity through the nose and mouth.
Since airflow follows the “path of least resistance,” by making the tube size smaller, air should more easily low through the nose and mouth after down-sizing. Although not always, if your child is unable to tolerate down-sizing of your tracheostomy tube, it is unlikely your child will be decannulated.
Down-sizing may be conducted in combination with PMV utilization and/or capping trials during the weaning process.
CAPPING TRIALS
Capping trials refers to times when a “cap” is placed over the tracheostomy tube opening to close off airflow via the tube. In doing so, the tube no longer acts as a means of airflow, allowing respiration entirely through the nose and mouth.
Capping trials may be started using a particular schedule, asking your child to wear the cap for specified amounts of time. If this is well tolerated, your child will be asked to wear the cap 24/7 for a period of a few to several days. If 24/7 capping is well tolerated, this is a good indication the tracheostomy tube is no longer needed and decannulation can be planned.
Although capping trials provide a good sense of how your child will tolerate breathing without the tracheostomy tube, it is important to remember that breathing will be easier following decannulation. If the cap is not well tolerated, and no particular upper airway obstruction is noted. It may be that the tube itself is creating too much obstruction to airflow and you may be down-sized as a result. By placing a smaller tube, and replacing a cap, this will allow for improved airflow around the tube and likely, better tolerance for the capping.
Criteria for decannulation, your child should:
- Not be dependent on a ventilator.
- Be alert and responsive and swallow reflex needs to be present so that your loved one is not aspirating secretions, sputum, gastric content or food.
- Not require frequent suctioning for tracheal secretions.
- Be able to cough and clean his/ her tracheal secretions.
- Have cardiovascular and hemodynamic stability.
- Have no new lung infiltrates on chest x-ray.
- Have their tracheostomy tube downsized and should not have breathing difficulty in the presence of this tube.
- Have the tube should be occluded (with a trach plug/cap) for twelve hours during the day with close monitoring by the nursing staff with no evidence of respiratory difficulty or requiring of suctioning of the trach tube.
- Tolerate the steps in item # 8 above, their trach is plugged for twenty four hours and they are monitored for respiratory difficulty or suction requirement.
TUBE REMOVAL
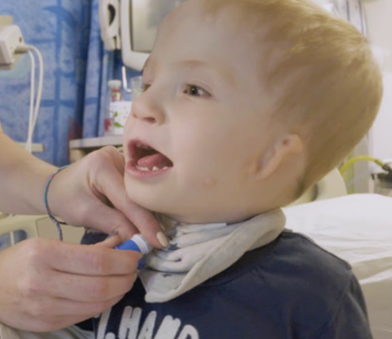
If the child has no difficulties with the overnight capping trial, then the tracheostomy tube is removed the following day by the ENT team. The stoma is covered with a small occlusive dressing.
Observation continues for another 24 to 48 hours to make sure that the child is able to breathe comfortably without the trach tube when awake and asleep, and is able to cough and clear respiratory secretions adequately.
To help ensure quick healing of the trach site, it is very important to apply pressure to the site whenever your child coughs, talks, swallows and laughs. Without adequate pressure to the site, air will continue to leak from the wound, serving to keep it open instead of allowing it to heal.
As the tracheotomy site will continue to drain for a while, it is important to keep clean, dry dressings in place until the wound site has completely healed.
CLOSING THE STOMA
A child’s stoma will start to close without the tracheostomy tube in place. This opening without a tracheostomy tube is called a tracheocutaneous (TC) fistula, which means an open tract between the skin and trachea.
The TC fistula should be kept covered with a small bandage until it is fully closed to protect the child’s airway from foreign objects or particles in the air. The opening should be carefully cleaned and inspected daily. The bandage should be replaced daily or more frequently if it becomes saturated with secretions.
Some TC fistulas close completely on their own, while some remain open. Until the opening fully closes, it is not safe for the child to go swimming because water can go through the opening into the airway.
If the TC fistula fails to close on its own, surgery can be done to remove the tract. Surgical closure of the TC fistula would be considered if the tract is still open one year after decannulation in a young child. In the older child with a larger airway, surgical closure can be done sooner.
FAILURE TO REMOVE TRACHOSTOMY TUBE
Whenever weaning off ventilation and removal of tracheostomy in Intensive Care fails or is prolonged, INTENSIVE CARE AT HOME is a viable and genuine option, creating a win-win situation for all parties involved by
• Getting Patients out of Intensive Care into a holistic Patient and family friendly environment by having 24/7 ICU nurses come to your home
• Improving Patients and families quality of life and in some instances quality of end of life
We also have some case studies here so you can see how we have provided INTENSIVE CARE AT HOME services to Patients with tracheostomies.
The first case study is where we looked after a 15 month old toddler with tracheostomy at home. The toddler eventually had the tracheostomy removed, therefore it ties right in with our topic. Here is a link to it
REFERENCES:
1. Tracheostomy
https://www.rch.org.au/kidsinfo/fact_sheets/Tracheostomy_information_for_parents/
2. Decannulation and Tracheostomy
https://www.chop.edu/treatments/decannulation-and-tracheostomy
3. Decannulation
https://www.hopkinsmedicine.org/tracheostomy/living/decannulation.html
4. TRACHEOSTOMY CARE
https://www.practicalslpinfo.com/tracheostomy-care–decannulation.html
5. Image credit to: Candidacy for Passy Muir® Valve Placement in Infants and Young Children: The Airway Assessment
https://www.passy-muir.com/wp-content/uploads/2019/04/ped_patientl.jpg
6. INTENSIVE CARE AT HOME SERVICES FOR A 15 MONTH OLD TODDLER, ANOTHER “WIN-WIN” SITUATION AND SUCCESS STORY
7. Image credit to: Decannulation for Children with tracheostomies
https://i.ytimg.com/vi/YYBS35ji6pg/maxresdefault.jpg
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!