Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Paul as part of my 1:1 consulting and advocacy service! Paul is worried that his dad’s oral secretions may hinder his progress to recovery and he is asking about the ways to be done so that his dad may not aspirate on it.
My Dad is in ICU with Tracheostomy and Has Lots of Secretions. Is it True that the Biggest Risk for Him is Aspiration?
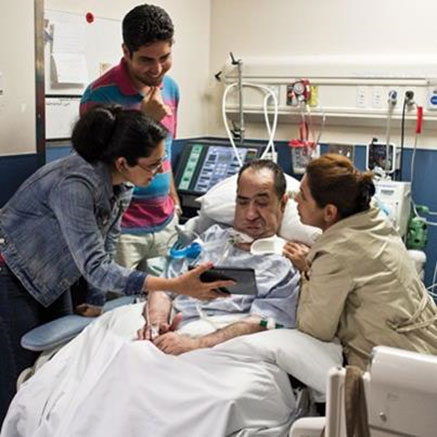
“You can also check out previous 1:1 consulting and advocacy sessions with me and Paul here.”
Charles: Suction around my what?
Paul: Your valve. How often do they come in and suction around the valve? The tracheostomy tube?
Charles: I’d say at least once a day.
Patrik: Once a day, that’s nothing.
Paul: Would you say maybe once or twice a day, like the morning nurse and the evening nurse both do it, or is it just the morning nurse.
Charles: Well come to think of it. The person who does it is a therapist. We have a therapist that comes in. She comes in once a day, so it’s probably not done more than once, I’m thinking. That’s a great question.
Patrik: Do you cough frequently? Do you have a cough frequently?
RECOMMENDED:
Charles: I do when I lie on my back. I get all of this phlegm circulating in my throat and in my mouth. This is what they had to suction last night twice. What am I using Paul?
Paul: The Optiflow.
Charles: Optiflow yes. When I’m standing straight, or during the day I don’t have any problem at all, but when I retire, or go to sleep all this phlegm and mucus circulates around my throat and mouth, and I get clogged up. So, I’m sitting up straight tonight hopefully I can go to sleep. I’m sitting up straight.
Paul: Okay.
Patrik: With the phlegm, can you cough it up? Can you cough it up yourself, or do you need help with the nurses getting rid of that?
Charles: I can cough it up.
Patrik: Great.
Charles: I have a device here that says suction it.
Patrik: Great.
Paul: Yeah, it’s like a little just suction basic.
Patrik: Yeah. I really think Paul, there should be no reason if the dye test is positive. If he can manage the dye test, and arterial blood gas, the CO2 is normal, I mean it’s almost a miracle to me that I can hear your dad so clearly. I mean, you’ve got the phone next to you.
Paul: Yeah.
Patrik: Right. I mean, I can hear him clearly.
Paul: Yeah. You’re on speaker by the way dad. Sorry, if didn’t you figure it out.
Patrik: Right. I mean, for someone with a Passy-Muir valve he’s got a very strong voice. Somebody that’s exhausted, or can’t breathe, can’t talk. I mean, I can hear you that clearly. That’s very encouraging.
Paul: We can hear you cough too. So, yeah there you go. That’s good though. The coughing is good, because it means his cough reflexes are good, right?
Patrik: Absolutely. That’s why I’m asking can he cough up the phlegm. I think what’s really important as well, going forward, Paul is if he can do the walking every day, that brings him back the strengths, including coughing, breathing. The mobilization part is important, very important.
Charles: I don’t walk every day.
Paul: Yeah. You walked 150 feet today, right? When you changed rooms.
Charles: Yes.
Paul: Yeah. My dad walked 150 feet. That’s like what, 50 meters or so?
Patrik: That’s fantastic.
Paul: Yeah, dad you’re doing good. All things considered.
Charles: I’m trying. I just don’t want to go through another night like I did last time.
Paul: Yeah, but dad stay on that Optiflow if you can right. That’s one of the tools that they use to see how long you can stay on that. To see if you’re ready for getting that ventilator removed. They typically want to see about 72 hours how well you do on that. Right now you’re at about 36, because you’ve been off of it since yesterday morning at 6:00 AM, and it’s about 5 o’clock now.
Charles: Yeah, okay no problem.
Paul: You’re not tired though, right?
Charles: I’m tired from not sleeping last night.
Paul: Yeah, but you’re not physically exhausted.
Charles: No.
Paul: Just sleepy?
Charles: Yeah. I’ll do all right. I just hope I can sleep sitting up like this. I just like sleeping on a chair.
Paul: Yeah, it’s like sleeping in a recliner.
Charles: Yeah, I hope I do that.
Paul: Yeah, if they have to clear your secretions they can go ahead and do that. That’s not a problem. That’s what they’re there for dad.
Charles: I want you to finish your conversation with Patrik.
Paul: Okay. I’ll call you right back in five minutes.
Charles: Patrik, thank you for your help. I appreciate it.
Paul: Yeah. Thank you, Patrik. Did you have any other questions for him?
Patrik: No. Very nice to talk to you. I think you’re halfway there. It sounds like from what Paul shared with me, and just by listening to you it sounds to me like you’re very strong considering what you’ve been through, and that is very encouraging. That’s very, very encouraging.
Charles: I appreciate that. You know you feel down so much of the time, and to hear a positive word like he just expressed makes me feel a lot better. Thank you Patrik.
Patrik: No, thank you.
Charles: I’ll talk to you later Paul.
Patrik: Pleasure talking to you.
Charles: Bye.
Paul: Hey, dad you don’t get too tired talking on the Passy-Muir? When you talk, since they put the talking valve in, the Passy-Muir, you don’t get too exhausted when you talk on that. Like we talked for an hour and it’s fine, right?
Charles: Yes.
Paul: Okay. Yeah.
Patrik: That’s great. That’s great.
Paul: All right, dad, I’ll call you in just a few minutes. Okay?
Charles: Okay.
Paul: Love you.
RECOMMENDED:
Patrik: That’s good Paul. That is really amazing. I can hear, basically, I looked after patients with a tracheostomy trying to talk, and you could barely hear them at the bedside. I can hear your dad talk through a phone via Zoom. I think that’s very encouraging.
Paul: Yeah. His voice. I mean, it’s raspy, but it’s the same. It’s the same volume it always is. It’s not like I have a hard time hearing him.
Patrik: I can hear his cognitive state is good. Again, that is often a big issue when patients come out of prolonged critical illness. They can be delirious. They can be confused. That means with his cognition intact, he can comply with whatever they are requesting from him.
Paul: Sure.
Patrik: That’s a bonus for him. That one of the biggest risks that I can see is the aspiration part. They got to be careful with ice water, got to be careful with that. If he’s got a good strong cough, he should be able to get there eventually.
Paul: Good. Well, you heard it. His cough is pretty good. It had a lot of secretion in it, so.
Patrik: Absolutely.
Paul: All right, well I’ll encourage him.
Patrik: I really hope it’s going well. I think the signs are there that it’s going well.
Paul: Okay, good. Well that’s all I needed to know. Thank you. We’ve gone over an hour. I very much appreciate.
Patrik: Pleasure.
Paul: Go ahead. I’m sorry.
Patrik: Very heartwarming for me too, because a lot of people come to us when it’s often too late. Like we’ve had some COVID cases lately where people come when it’s too late and it’s very heartwarming for me to see that there’s people recovering.
Paul: Yeah. Well, I’m glad. I’m sorry for those other people though. That’s real sad. It’s so tragic. I wish people would do more to stop it. I wish my dad would have. I asked him actually not to travel. That’s why I gave him an oximeter, thermometer, some extra gloves, make sure you use hand sanitizer. I think older people they forget things. They forget to sanitize every time you handle money or something that.
Patrik: Yeah, when you now go into the super market I almost feel it’s finally, like in a hospital, you are having the hand sanitize us everywhere. So, when I now go to the supermarket and I see, “Yep, that’s what hospitals are like.” That’s why people in hospitals are generally much safer or at least the workers, not all the time, but compared to when you go to the supermarket now.
Paul: Exactly.
Patrik: All right, I’ll send you this link, Paul, to the ABG.
RECOMMENDED:
Paul: Okay. Thank you so much Patrik.
Patrik: Thank you so much. All the best, Paul. Thank you so much.
Paul: Okay. I’ll send you an email to let you know how it resolves. Okay.
Patrik: That would be great. I would like to know.
RECOMMENDED:
Paul: Okay. Thank you.
Patrik: Thank you Paul. Bye.
Paul: Bye-bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!