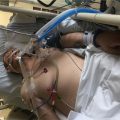
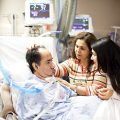
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Paul as part of my 1:1 consulting and advocacy service! Paul wants to know what will happen if his dad will need the tracheostomy for a long time and he is asking if it can be removed still after some time and does people recover from it.
Is it True that if my Dad is with Tracheostomy or Intubated for a Long Time in ICU, it’s Usually a Bad Sign?
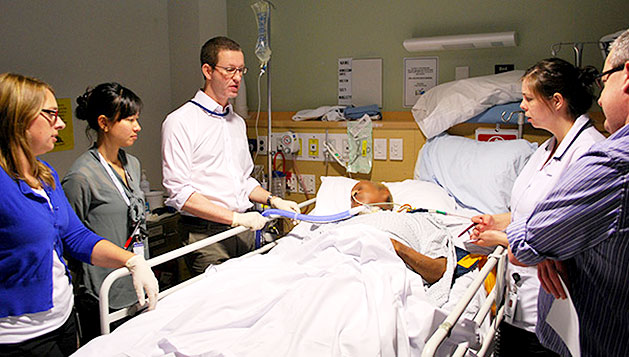
“You can also check out previous 1:1 consulting and advocacy sessions with me and Paul here.”
Patrik: All right, but in some states in the US they go from Florida to Georgia, for example, and they go from New York to other states. It just doesn’t make any sense. People being taken away from their families, which is what they need.
Paul: Yeah. Well, sadly with COVID I can’t visit.
Patrik: Yes.
Paul: What you say is it seems like they’ve done an okay job at the ICU. Everything is progressing as you would expect it to?
Patrik: Definitely. I mean, I’m very pleasantly surprised. Steps, really, or things to look for is definitely the frequency of secretion or the frequency of suctioning.
Paul: It’s pretty often that my father has to suction.
Patrik: But he doesn’t suction through the tracheostomy himself, does he?
RECOMMENDED:
Paul: No, it’s a suction yeah, in the mouth like in the back of the throat. I don’t think he does trach suctioning at all. I think that’s just the nurse who does that.
Patrik: Yeah. Should be, and if that’s what they’re doing twice overnight, that’s nothing. If you were telling me it was two times an hour, I would say, “Okay, all right,” but twice over night that’s just maintenance.
Paul: Okay. Well it sounds like it’s very good. Good news.
Patrik: I’ll give you another example, Paul so you can put that in perspective. Passy-Muir valve, when you put patients on the Passy-Muir for the first time, they manage five minutes, 10 minutes, and they get exhausted. Then maybe the next day they manage half an hour, and they get exhausted. Your dad’s managed up to 16 hours. That’s very, very encouraging. Also, I don’t know whether that when they’re on the Passy-Muir the cuff is down. You know what I mean by that?
Paul: Not really, no. I think that the cuff is the inflatable part of the tube.
Patrik: Yeah. When they put up the Passy-Muir the cuff needs to go down, because otherwise he couldn’t talk, otherwise the vocal cords wouldn’t work. So, they take the cuff down, and I’ve seen people when the cuff goes down, they can’t manage. If your dad can talk and can manage up to 16 hours, that is very, very encouraging.
Paul: Yeah. He doesn’t desaturate either. When I’m speaking to him. I FaceTime, I see his stats on the wall, he maintains heartbeat of 80 or so. His saturation is anywhere between 95 and a 100. If he’s laying prone, it’s usually closer to 99, if he’s up closer to 95.
Patrik: Yeah, and he’s not getting short of breath when he’s talking to you.
Paul: No, not really. I mean, he’s indicated that he’s tired, but not exhausted type of thing.
Patrik: I think he’s allowed to be tired after six weeks.
Paul: Yeah, and he’s not on any type of antibiotics. Oh, I forgot to mention he was treated with broad spectrum antibiotics for the pneumonia. All right, well that’s all very good news. Thank you.
Paul: In the event that he does have to have the tracheostomy for a long time, is it possible to get it out after 60 days?
Patrik: Definitely. I’ve seen people being decannulated after six months.
Paul: Did they recover?
Patrik: Yeah. Well, when I say do they recover, you see what ICU people are good at is we’re very good at knowing what’s happening in ICU, but once the patient leaves ICU, we have very little idea. I have an idea, because we’re also running intensive care at home, so we know what’s happening in the community with some long-term ICU patients. The reality is for people that leave ICU without artificial airway, we have very little insight of what they’re up to. As long as they’re not coming back to ICU, that’s generally speaking a good sign.
Patrik: Yeah, the risk is definitely higher for someone that’s spent a long time on a ventilator, that they might end up again with a tracheostomy, but what you’ve shared with me Paul is very, very encouraging. Very, very encouraging.
Paul: The 60 day, I mean, there’s no hard and fast rule, I get that. I’ve read a couple of places that say, if you’ve had the tracheostomy for more than 60 days, or you’ve been intubated for more than 60 days, it’s usually a very bad sign. It means that you probably will never get off mechanical ventilation or invasive ventilation.
Patrik: I don’t agree with that, Paul. Yes, I agree with one thing that the longer you’ve been on a ventilator the higher the risk that you might need ventilation for a long time to come, but I have seen patients being weaned off the ventilator and a tracheostomy for up to six months. Yeah, you could argue that again the younger someone is the higher the chances they can come off the ventilator, of course.
Paul: Of course, yeah.
Patrik: But I have seen patients in their 80s and in their 90s being weaned off the ventilator over many months and they get decannulated. Does it happen very often? Probably not, but it certainly does happen. Now that you’re telling me there’s no heart issues, no kidney issues?
Paul: No, there’s no other health issues that they’re aware of other than just the pulmonary issues.
Patrik: Yeah.
RECOMMENDED:
Paul: The other thing is, I asked and there’s no evidence of scarring, I guess, from the x-ray, at least that’s what the nurse said.
Patrik: There is no evidence?
Paul: No evidence, yeah.
Patrik: That’s good to hear.
Paul: It’s very good, yeah. So, no fibrosis that they could detect from an x-ray at least. That was when they did the x-ray to see if there was an issue with the silent aspiration.
Patrik: That I see as the biggest problem, your dad would be so thirsty, and the crushed ice is just like extinguishing a fire. I get that. That’s something they need to be careful with, because the micro aspiration could potentially set him back. I know how he feels. I’ve seen so many patients look-
Paul: They did it to him. He’s not particularly thirsty. They were testing swallow.
Patrik: All right, that’s good. If he’s not thirsty, I would take it very slow. Very slow.
Paul: Okay, he’s getting all his nutrition from the NG tube. Well, that’s all very good news. Is it common? When I ask the nurses questions, they try to be very discouraging. One had talked to them about considering hospice at some point, I’m like, “Really? Why would you say something like that?” Another said, “You have to consider the fact that you may never eat again, and you have to think about why you’re living.” These are the things that they told me. So, I was and like, “Why would you tell somebody that?” I get the fact that they’re bringing their own baggage, but statements like that really concern me. From your experience, is that fairly common in ICU for nurses to be like that?
Patrik: I don’t know how much research you’ve done. I don’t know how much you’ve read on my blog. ICU doctors and nurses are negative by default, it’s almost part of their training. It’s almost part of their own insurance. If the doctors or the nurses came to you and said, “Hey, Paul, another three weeks with your dad’s here, and then he’ll be home again,” and it doesn’t happen, you could potentially sue them. So that’s one of the reasons. Their own baggage, definitely one of the other reasons. I guess, your dad would have been probably in a situation where they questioned whether he will survive or not. They questioned it at some point. There’s no doubt about that from what you’re sharing with me.
Patrik: They might picture the scenarios that they’ve seen and they’re probably surprised, but I think part of it is their own baggage and also the training that doctors and nurses go through in terms of, “Oh, don’t make promises that you can’t keep.”
Paul: Yeah, of course.
Patrik: So, but I wouldn’t discourage you just because they’re saying that. It’s just like you said part of their own baggage. It’s a very confronting job as you know. I do believe that some nurses, doctors might even have post-traumatic stress by working many years, maybe decades in ICU. So, it could be all of their own psychological makeup after all this time. I wouldn’t put too much weight on it, because I would go by what’s there and what’s there I argue is very encouraging.
Paul: Okay. Well, thank you. That’s really what I wanted, because I’m not hearing anything from anybody. When I talk to the nurses they seem very either extremely negative, like one told me. Last week, I asked the nurse about how long do you think it would be before we could really consider decannulation. She said, he may never be decannulated. This was, a week ago. My dad was doing pretty good. I’m like, okay. I get that. I get what you’re saying about that’s just what they do. It’s a psychological thing, or it’s how they’re trained, or some combination of all of the above.
Patrik: You mentioned something else that I think is very important. You mentioned they made comments about, why would your dad even want to live, or what’s the reason for him to live? Well, the whole debate in ICU is often about, “Okay, what does that person’s quality of life look like if they make it?” Well, who are you to judge what quality of life is for Paul’s dad?
Paul: Yeah, exactly. Quality of life is a very personal thing.
Patrik: It’s a very person thing, and who’s to judge for any person to get out of ICU, and then maybe go to a hospice, and I’m not saying that’s bad, and then maybe have some time in the hospice with their family, if that’s important to them, that’s important to them. Not for the ICU.
RECOMMENDED:
Paul: Yeah, exactly. I know you have to go, our hour is up here and you’ve really helped me a lot, Patrik. I did have one last question, so for the ABG what should I be looking for? Because I think I’m going to ask when the last test was and what it was.
Patrik: I’ll tell you what I’ll do, Paul, I’ll send you a link with some figures. I’ll send you a link to an article. We’ve got an article on our website about ABG, and you can just look at the figures. I believe the most important figure you’d be looking at is
CO2, the carbon dioxide, and that should be between 35 and 45 millimeter per mercury. As I said, I’ll send you the link. With COPD the baseline CO2 might be a little bit elevated as a baseline. So, if your dads CO2 is 45 to 50, maybe that’s just baseline for him. If it’s 60, that might be a little bit of a concern, but you’ll find that out once they’ve done an ABG.
Paul: Okay, so we want to look at numbers somewhere between 35 and 50.
Patrik: Millimeter per mercury, “mmHg”.
Paul: Yeah, you can send me that link. I would really appreciate.
Patrik: I will send you a link to that, but that would be the next step. It sounds, as I said Paul, it sounds very encouraging. He’s walking. He’s managing the Passy-Muir. If he needs suction twice overnight, and maybe a few times during the day, he’s got a good strong cough, I tell you what the test really is. If the CO2 is stable.
Paul: Hey Patrik, actually that’s my dad. Do you want to hear him real fast? Hear how he sounds.
Patrik: Please.
Paul: Hey dad, how are you doing?
Charles: I’m fine Paul.
Paul: Good. I’m sorry.
Charles: No, I hear you.
Paul: Oh, I’m just talking to somebody about your case. Trying to get some ideas about maybe how to move forward.
Charles: Let me. I’m calling you back.
Paul: No. It’s okay. I’m actually just done real fast. I’m going to drop off here, but I wanted to take your call. Dad, did you hear about the COVID test?
Charles: No.
Paul: They didn’t tell you?
Charles: No.
Paul: It came back positive? I can’t believe they didn’t tell you.
Charles: Positive.
Paul: Yeah. I’m sorry, dad. The good news is that you’re getting great care where you are. Patrik, who I’m speaking to is actually really encouraged about your progress. He’s a former ICU nurse. You want to say hi Patrik.
Patrik: Hi, I was talking to Paul and I’ve been hearing all about your case sir and it sounds very encouraging. It sounds to me like you will have that tracheostomy out in a few days.
Charles: Well thank you. I hope so. I’m really disappointed about the positive COVID test results.
Paul: Well, dad, you’re certainly not COVID positive anymore. You’re just testing positive.
Charles: Yeah, positive.
Patrik: That shouldn’t discourage you.
Paul: Yeah. I was talking to Patrik about you staying on the Optiflow all night. He said that’s a great sign, and that you should probably try to stick with that. It’s better if you sleep with the Optiflow, because it tells the hospital that you’re doing really good.
Charles: Yeah, I think that’s a good plan.
Paul: Yeah.
Charles: Let me call you. Why don’t you finish and call me back?
Paul: Okay, hey Patrik did you have any questions for my dad about his care or anything?
Patrik: How often do the nurses suction you?
Charles: They spend about two hours a day with me, in the morning, in the afternoon.
Paul: But how much of that is suctioning, dad? How much do they actually suction around your valve?
Charles: Well it’s hard to tell. They do it, but it’s not regular, not on a regular basis.
Paul: You said last night they only came in twice, right? The whole night, to suction the mouth?
Charles: Yes, that’s right.
Paul: You’re sure it was only twice, because that’s actually a really good sign. That’s no big deal. That’s what we would normally expect.
Charles: Well that’s because I had trouble with the phlegm in my system. It was clogging.
Paul: That’s to be expected, right Patrik?
Patrik: That’s to be expected. Are you feeling okay without the CPAP? You’re not short of breath since you’ve been off the CPAP?
Paul: Yeah, you know when they put you at night on the CPAP mode, the ventilator.
Charles: Yes.
Paul: Since you’ve been on the new one, the Opti flow, are you out of breath?
Charles: No, I’m okay.
Patrik: That’s very encouraging. During the day, do you know how often they suction around your valve?
Charles: Suction around my what?
Paul: Your valve. How often do they come in and suction around the valve? The tracheostomy tube?
RECOMMENDED:
Charles: I’d say at least once a day.
Patrik: Once a day, that’s nothing.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!