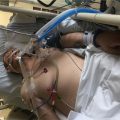
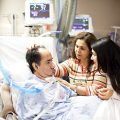
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Long Does it Take for your Loved One to Wake Up After An Induced Coma?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Arthur, as part of my 1:1 consulting and advocacy service! Arthur’s brother is with a tracheostomy and is on a ventilator. Arthur is asking if it’s possible to bring home his critically ill brother through Intensive Care at Home instead of being neglected in ICU.
Is it Possible to Bring Home My Critically Ill brother through Intensive Care at Home Instead of Being Neglected in ICU?
Patrik: Hi Arthur! How are you?
Arthur: Hello Patrik. I’m good. Let me start telling you where my brother is.
Arthur: So, my brother has to be weaned off of the ventilator right? So he’s currently over in a short term rehab. And to me they’re not doing what they’re supposed to be doing. We’ve recorded them, we have our iPads that are for my brother, so we recorded on the treatment that they’re giving him. And we’ve reported them to the state, I’ve gone up there, voiced my concerns and it still hasn’t gotten any better. After telling them several times, and him being treated for pneumonia prior to coming to the rehab. And they claim it’s the hospital, he’s only been there a weekend and two days before he was sent back to the hospital. Right now he’s back over to the hospital and is being treated for the bacterial infection and the pneumonia.
Arthur: But by the time they conveyed that to the rehab, they said they had no record of it. After three days of complaining that my brother couldn’t breathe, they finally sent him back to the hospital. So what I need to get from you is, does your facility offer services, for him to be weaned off the vent at home?
Patrik: Yes.
Arthur: I’ve seen some success stories looking at the information and we’re just trying to figure it all out.
RECOMMENDED:
Patrik: Of course. Can you tell me some timelines? How, are we talking about..
Arthur: As far as the timeline, it was going towards the end of last year. When you mean when he was first, what caused him to get there? Do you mean when and what caused him to be there?
Patrik: Yes. Yes. How long are we talking about? Are we talking about weeks, months?
Arthur: No, it was months. He was diagnosed with COVID pneumonia back in the end of October. Then he was put on a ventilator. And from there, he was on a vent for 60 days. He was taken off of the vent, a week later, then he was sent over to the rehab. Because they said that he was stable enough medically that he can go to the rehab or the weaning off from the vent. And he’s on a low pressure support. He’s only on 18/5. So he’s on the lowest pressure support. And so he was sent to the rehab and then he was started on physical therapy, occupational therapy, and speech therapy. So they did the swallow test and all of that.
Arthur: They told me, once he gets off the vent, he can come home and get the rest of the rehab. But I know like reading your information, it says that you have a success rate of weaning the patients at home. He has a place to come. He can come to my house. I’ll convert my family room into a room for him. I’m just trying to understand the processes of all of it.
Recommended:
Moe: I’m sorry.
Arthur: Sorry, go ahead.
Patrik: Hi.
Moe: Yeah. How are you doing? The others are trying to log on to their phone as well.
Patrik: Right, yeah.
Moe: Our main goal is to get him home so he can get the proper treatment. He is being neglected at the facility, we’ve witnessed it ourselves. He’s afraid to even go to sleep there because he wants to make sure that he’s okay. He knows that he’s not receiving the proper treatment. There’s one nurse to 17 patients. And there’s been times where he was like choking and needed some help and no one was there to suction him. So it’s been very traumatizing.
Arthur: If we didn’t watch him, he would’ve…
Moe: Yeah, we’ve had to call up to the facility to let them know. Hey, you have to go check on him. He’s choking. So we read his lips and he was like, please tell them to hurry, I need help and nothing.
Patrik: Yeah. How long has he been at that particular facility for?
Moe: For about a week and a half.
Arthur: Yes.
Moe: It hasn’t been long. But we had the authorities involved because he was being neglected. And so the authorities did go there and they said, this is normal for this facility. We see this very often. Yeah.
Patrik: Oh my goodness.
Moe: They said, we go here often to check on patients because their families are concerned. So they are known for this neglect. Yeah, So we’re just..
Suggested links:
Patrik: That’s terrible. Are you the medical power of attorney for your brother?
Arthur: So it’s myself… Like my brother is alert, he’s alert, you can hear some words.
Moe: So today we did Face Time him and he’s not…
Arthur: At the hospital.
Moe: … he doesn’t have the voice box for the tracheostomy, but he was able to talk to us.
Arthur: We could hear him.
Patrik: Right, right. But who has made decisions in the past, you know sign, give consent for a trach, or give consent for a transfer to another facility.
Moe: Yeah.
Arthur: Yeah, me.
Moe: Yeah.
Patrik: You, okay. Okay. Now that is important to know that.
Moe: Yeah. The doctor’s go directly with him.
Arthur: Yeah. It’s myself and my other brother, but I’m the one that makes all the decisions.
Recommended:
Patrik: Okay. Right. Right. What’s stopping him from the information that you have? What’s stopping him from getting off the ventilator? Any ideas, besides poor care?
Moe: Let me talk. So he was off of the ventilator for a short period of time…
Patrik: For two days.
Moe: For a short period of time, but then they believe because of the pneumonia, it caused him to go back on it. So he’s going to very low setting there. They want to try and start weaning again once the antibiotic runs its course.
Patrik: Right. I doubt that they can wean with one nurse for 17 patients.
Moe: Right exactly.
Patrik: Exactly.
Moe: Yeah, it’s uncomfortable.
Suggested links:
Patrik: Can you just, tell me a little bit more. So initially ICU for COVID, proning, and trach.
Moe: Right.
Patrik: And what was next after the first ICU stay?
Arthur: They had him on a vent the whole time for the two weeks.
Patrik: Yeah sure.
Patrik: And where did he go next?
Arthur: He went to the rehab facility. So he got the-
Patrik: Last week?
Arthur: Right. Right.
Patrik: He was in ICU up until a week ago?
Arthur: Yeah, well he started out-
Moe: Well not ICU, like he went down to CCU and then like the regular floor, to a step down unit.
Arthur: And then, so during the step down time he was there, they did the temporary trach and a week later they transferred him over to this facility where he was only there a week and a half.
Patrik: Right. Okay. And have they asked you for consent? Have you had a choice or do you feel like you had a choice?
Arthur: No. They’ve basically told us that his insurance would only pay for the facility that they were sending it to. But when I called the insurance company, they sent me 42 different locations basically, but they’re all the same rehab type of situation. I mean, I asked about him being weaned at home. And they said, yes, he can get weaned at home, but you have to find a facility, make sure they take insurance, and then make sure his doctor says- okay.
Patrik: Right. Okay. Excuse me. When you say he has been off the ventilator for two days, how long ago was that?
Arthur: That was like within the last couple of weeks. So maybe…
Patrik: Last couple of weeks.
Moe: Yeah right like two to three weeks.
Recommended:
Patrik: Right. And he’s alert?
Arthur: He’s alert. The only time he’s not, was when they had given him, of course, pain medicine to make him sleep or anxiety medicine.
Moe: Yeah, he’s fully alert. He knows what’s going on. Today he was using his voice to talk.
Patrik: Great.
Arthur: And he’s talking without his voice box. And he’s young. He’s only 32.
Patrik: Good. I was just about to ask how old is your brother, 32?
Arthur: He’s 32 with three babies.
Patrik: Any pre-medical history?
Arthur: None.
Patrik: Just came out of, struck by COVID?
Arthur: Yep, by COVID. He works in healthcare and that’s basically what happened. He was working part-time in healthcare and got sick from, I don’t know if it was a patient or what have you. He got sick and unfortunately, from what I understand, he was always saying, I got to go to work, I can’t call out. He just thought it was this… What happened?
Arthur: So basically he didn’t go to the doctors because he was concerned about working. And they say frontline workers normally are the last to know because they were too busy working, you know? And that’s basically what happened. But other than that my brother has no health issues.
Suggested links:
Patrik: All right. Okay.
Patrik: So do you live with your brother?
Arthur: My brother is living near the rehab. Right now he’s at the hospital. I’m about 30 minutes from there.
Patrik: Right. Okay. Can you visit him or just Face Time?
Arthur: No, it’s just FaceTime.
Moe: They’re not allowing visitors. If they were allowing visitors, it would allow us to come.
Patrik: Sure. Sure. Okay. And have you been able to visit him in hospital before he went to rehab?
Arthur: No.
Patrik: Oh, so you haven’t-
Arthur: Because the hospital’s on red alert.
RECOMMENDED:
Moe: Yeah, both are closed down neither are allowing us to see him. But he did test negative for COVID after testing positive.
Patrik: Sure. Okay. Let’s start with the good news and then let’s look at the not so good news. So the good news is, I mean, he had some time off the ventilator, which means there is light at the end of the tunnel. The not so good news is that, as much as I would like to help you with taking him home through our service Intensive Care at Home, I can’t help you in your location yet. We’re not in your location yet. So I’m not making up things that I can’t promise.
Moe: Right. Where are you located?
Patrik: I am located in Melbourne, Australia out of all places.
Arthur: Oh, they just have two locations.
Patrik: The demand in your place for us is so big. We know we need to go and have our services available there. I’m talking to people like yourself almost every day.
Arthur: Really.
Patrik: It’s unbelievable. I mean, we are very busy here in Australia. But the demand in your place, just because the population is so much bigger than here, it’s just through the roof. But let’s just say, just so that you understand, even if I could help you, even if I could say to you, yep, let’s set up home care, no problem. It would take time. It takes time here. You know if I get an inquiry here, similar to your situation, it would take four, six, eight weeks because it’s such a specialized skill, right? You got to find, you’ve got to have the right equipment, and right staff.
Arthur: Understood.
Patrik: And it’s not as simple as, we’re just hiring ICU nurses for a 24-hour roster in the next four weeks, it takes time.
Arthur: Understood.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!