Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How to Advocate for My Wife So She Can Get the Best Care & Treatment in ICU? Help!
You can check out last week’s question by clicking on the link here.
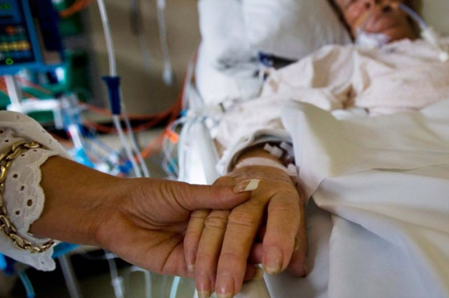
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Julia, as part of my 1:1 consulting and advocacy. Julia’s mother is in ICU and she is asking how she can prevent the ICU team from withdrawing life support for her mom.
How Can I Prevent the ICU Team from Withdrawing Life Support for My Mom?
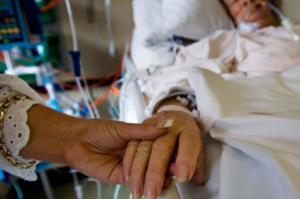
Patrik: Hi Julia! Patrik here from Intensive Care Hotline.
Julia: Hi Patrik! I have gone across your videos and website and I thought of asking you because my mom is still fighting for her life in ICU. I believe that her brain is intact but they want to withdraw life support for her. What do I do?
Patrik: This is not the first time that I’m helping families with that situation and like I always mentioned, everything in a hospital has a policy, whether they’re mopping the floor, whether they’re washing the windows, whether they’re cleaning the desk, everything has a policy. And now, they’re telling you basically, “Oh, well, ending your mom’s life. Well, just do it because we feel like it.” That has a policy, too, of course.
They have a hospital policy around withdrawal of treatment, and that hospital policy will most likely say that you need to be either consulted or you need to give consent. The hospital policies vary slightly from what the law says. Please bear in mind, I am not a lawyer by any means. I’m a clinician. I’m a clinician first and foremost. However, I’ve been in that area long enough that I have a basic understanding of the rules and regulations.
Julia: Is that something that the lawyer would write into their script or is that something I can just email let’s say tonight.
Patrik: I would not wait for the lawyer. I would email them tonight, so they know you mean business.
Julia: Yeah. And who would I email actually?
RECOMMENDED:
Patrik: Hospital CEO. If you have the email from ICU consultant, email it to them, but I would go right to the top, because whilst I think you have enough time to turn this around, I wouldn’t waste any time.
Julia: So, the actual CEO. I’ve got the complaints officer as well.
Patrik: Yeah. I tell you why I wouldn’t bank on the complaints officer. Look, you can email it to both. The complaints officer will be dealing with a lot of complaints, and they are employed by the hospital. They will do what the hospital wants them to do. The hospital CEO, yes, is an employee of the hospital too, but because this is a very serious situation, you can’t be messing around with people that are dealing with 200 complaints.
Julia: Yeah. My only concern is, is there any chance that I can send this tonight and backtrack the time they’ve given us, the extra compassionate leave they’ve given us, the compassionate time?
Patrik: No, I wouldn’t worry about that. If that is an issue, you unfortunately would have to go to the court tomorrow. They will consider within very short period of time.
Julia: But I shouldn’t be worried about them changing …
Patrik: I’ll tell you what you should not be worried about. You should not be worried about backlash from the hospital. You absolutely should not, and I’ll tell you why. I’ve done this. This is not the first time that I’m helping families with that end. Yes, I can understand how intimidating they are, I get it. I’ve worked in the system long enough. I get it. They can be very intimidating, but that should not concern you, because if you give in, if you give them an inch, they will take a mile. They need to know that you mean business because this is life or death.
Julia: So, I have to ring up and ask for the CEO’s email address?
Patrik: Yes, you may.
Julia: Okay. I would say, “Dear, such and such, I’d like to request the withdrawal of treatment policies and to include my mom’s details and what’s been happening.” Or just keep it short and brief?
Patrik: The more information the CEO has, the better it is. But you need not to over explain yourself that you want your mom to live. I would keep it to the point. If the CEO wants to find out what’s happening, he will reach out to one of the doctors.
Julia: So I’ll just say I would like the policy …
Patrik: Well, I can help you craft the email.
Julia: Okay.
Patrik: It’s more about you can keep it sort of as friendly as possible, but if I was you, I would be outraged. You probably are, but you’re probably not showing it. I would let them know that you are outraged by what is happening here. I would go as far, and I know that people don’t want to ruffle feathers and I’m all for making friends when you can. I would go as far that by doing what they’re doing, I would go as far as using stronger language. And by that, I mean I would call them out on that this could be perceived as murder. At a bare minimum, it could be perceived as euthanasia, and euthanasia is illegal. Are you familiar with the term euthanasia?
Julia: Yes, I am.
Patrik: Right. One of the reasons for me to leave the system eventually was simply I just believe that we were euthanizing people in ICU and I just couldn’t be part of it anymore. I just couldn’t be part of it anymore.
Julia: It’s really too strong of a word.
Suggested Links:
Patrik: I would go in with that, because they don’t see anything wrong with what they’re doing. They don’t because they’re doing it all day every day. That’s how desensitized they are. And COVID has probably heightened that people get desensitized. But coming more to the practical steps, we can talk about what language to use a bit later, but let’s just look at the rules and regulations. (A), there is the hospital policy. I sent you some information about access to medical records. (B), I would tell them that by 5:00 tomorrow, you want access to medical records. What I also don’t know at the moment if I had all the clinical information, let’s just say they’re withdrawing life support on Saturday. There is no guarantee that your mom is going to die. There are people where life support is withdrawn, and they survive. I believe your strongest argument in all of this is, your mom’s brain is intact as far you’re aware. They’ve done an MRI scan (Magnetic Resonance Imaging) or a CT scan of the brain, which didn’t show any damage. Is that correct?
Julia: They says she’s got some encephally..
Patrik: Yeah. Encephalopathy.
Julia: Yeah. Now, I was asking whether it’s reversible, irreversible, but he was almost avoiding the question. I just feel because he isn’t waking up after 10 days.
Patrik: It doesn’t mean anything.
Julia: She hasn’t had a stroke or there’s been no seizures, so everything has been stabled in terms of they’re lucky she’s had no other situation go wrong. My sister said, “Look, we’re happy to try different alternative therapies. Look, we’re happy to transfer her to a private hospital and pay for it if we have to.”
Patrik: I was going to come to that. That might be another option. That will definitely get you out of it, but by the same …
Julia: We suggested to the doctor, but he says no, he wouldn’t approve that. We didn’t say this, but I’m thinking if a law draws it up something that say we take the risk out of your hands.
Patrik: I don’t see an issue with that.
Julia: We’re happy to do that. That’s something we probably have to speak to the lawyer.
Patrik: The first thing that you would need to do is ring a private hospital, which would probably be the hospital of your choice.
Julia: Yes, we rang our preferred hospital.
Patrik: Okay, good.
Julia: We have discussed it and they’ve given us a price already.
Patrik: Great. Look, don’t be discouraged by the rhetoric that’s coming from them. We have certainly seen and helped families to go to a private hospital. But I think for now, let’s make sure they’re not going to do what they’re planning to do. Let’s work on that because I think that’s probably something you can control; I think if we follow the right steps. You have a right to access medical records, because I would imagine you haven’t seen. Have you, for example, seen the CT scan (Computerized Tomography) report? Have you seen that?
Julia: Unfortunately, nothing.
Patrik: Right. For example, if he’s avoiding the question, is the encephalopathy reversible or not, well, my response to that would be, well, please show me the CT report. That would be my response to that. Make it transparent. What do you have to hide?
Julia: Yeah. Now, there’s a contact number that says customer relations. That’s something that they’ve used. If I call them, would they give the CEO’s?
Patrik: I think so, because I’ll tell you why. They will give you the CEO’s email address at a bare minimum because the healthcare service needs to be able to take complaints. And if you want to make that complaint to the top CEO, well, that’s your choice. I don’t think they will be refusing to give you the email address, but I’m pretty sure I’ll find out the email address for you.
Recommended:
Julia: Okay. All right. We’ll send that email tonight to get the ball rolling. We’re speaking to the lawyers tomorrow.
Patrik: The hospitals, generally speaking, don’t want to deal with you bringing in a lawyer. I believe that by you saying to them what you’re going to say and saying that you will bring a lawyer in, if they don’t reverse that might be enough. But it’s up to you how you want to manage that.
Julia: Okay. We’re speaking to a lawyer tomorrow, what would you … Walks on this situation, and they’ll give us some suggestions. Then I guess the lawyer might want to send some information out to the hospital I’m presuming
Patrik: Yes. I tell you what often happens. If I, for example, could look at medical records and I would see, okay, your mom is getting this and she’s getting that, I would have a much better understanding what’s happening, how likely is it for your mom to pass away if they stop life support? What are other options? Unfortunately, at the moment, I don’t have enough clinical information to guide you clinically.
Julia: Yeah, that’s okay. With my court application, they’re normally hard to get ahold of, aren’t they?
Patrik: That part, I would absolutely let the lawyer handle it.
Julia: Okay. In terms of the private hospital suggesting that, is that something we would speak to the lawyer? Or is that something I would expect to the hospital straight away? Because the in-charge denied that, because I wouldn’t be doing that. I wouldn’t be accepting. I wouldn’t allow that to happen. Yeah, he probably doesn’t want to take the risk.
Patrik: He probably doesn’t want to take the risk. If you ring up your chosen hospital, you talk to a bed manager. Their job is to fill beds because it’s a private hospital. They will tell you whether they have an ICU bed. If they do have an ICU bed, they will talk to the ICU consultant and ask them if they’re interested, depending on how busy they are, depending in a private hospital that the ICU doctors cannot refuse. Because at the end of the day, the hospital CEO will make the decision.
Julia: Okay. I should do that straight away.
Patrik: I would call up the hospital tomorrow. I would ask for the bed manager if I was you.
Julia: Yeah. And see if there’s a bed available for my mom.
Patrik: Absolutely. Bring her as a private patient.
Julia: If we say that we’ll take the risk out of your hands in a formal letter, is that something that you recommend?
Patrik: You could do that, but I argue that. You could organize a private patient transport and they’re probably prepared to take the risk even.
RECOMMENDED:
Julia: That’s something I would have to call them as far as to …
Patrik: You would have to call them to organize a transport for a critically ill patient.
Julia: Should I do that as soon as in tomorrow morning as well?
Patrik: Yeah. Just to line it all up.
Julia: Yep. Call the bed manager, see if there’s a bed available. They can’t refuse a patient, can they?
Patrik: Look, they can refuse a patient as long as you either have private health insurance or you’re happy to pay for it, assuming they have a bed.
Julia: Yeah. Otherwise, you would have to call another company.
Patrik: Otherwise, you would have to go to another private hospital.
Julia: Yeah. Is there any other hospital you can recommend?
Patrik: Look, I think your chosen hospital is pretty good. It is one of the best private hospitals in the region.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!