Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question in this series of questions from our client Robert and the question last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another question from one of our clients and readers
My Dad had a severe head injury 47 days ago and he’s still not “waking up”! He’s still in Intensive Care, what are the next steps?
This is an excerpt from an email counselling and consulting session with me and one of my clients Antonia
Hi Patrik,
on the 21st Sept 2016 my dad was hit by a car while cycling. He has not been conscious since after the hit.
Around one hour and a half after the hit he has been operated and a huge hematoma (front right) has been evacuated from his brain and the place of explosion was clipped. There were three/four other trauma places from the head injury. The skull was not broken. And no other body traumas were detected.
Since the operation dad has been in a coma even though he has now been off all sedatives and opiates (=pain killers) for many weeks.
They also did a craniectomy (=partial removal of the skull) to ease the brain pressures when he went for brain surgery.
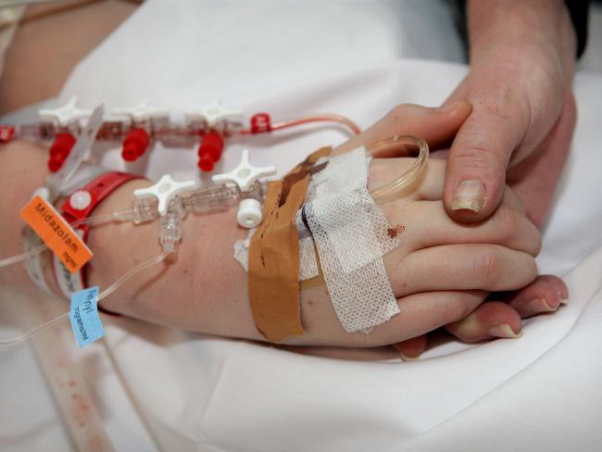
However, with the time currently he breathes alone (through tracheostomy and he is fed via Nasogastric tube through the nose. His organs were not damaged and currently function sufficiently in the given circumstances. He is moving his jaw, seems to have swallowing functions, does mimics (when provoked by pain). In recent weeks he does more arm and leg movements and there are attempts to open eyelids.
In several of these attempts he opens the eyes fully for a few seconds but without conscious response behind. There are some movements in the arms and hands (more expressed with the left arm/hand) primarily when exposed to some pain and recently with the left arm voluntary movements as well. This is an observation from the series of Physiotherapy during which movements of all the joints to full capacity is done. Physiotherapy is organised 2/3 x per day currently.
Imaging:
Till current date there are in total 6 CT scans imaging done:
– 21 Sept – Full body & Head
– 26 Sept, 28 Sept, 5 Oct – Head
– 13 Oct – Head
– 27 Oct – Head
– 31 Oct – Head
MRI has not been done yet but mentioned to be in the plans for next week perhaps.
Medications:
herewith his medical treatment per dosage and hour of intake: Amikine 1g, Ulcoprol 2x40g; Nootropil 6+6+0; Vit C 2×500, Depakine 1×400, Fraxiparine 2×0,4, CaGluc 2×1, Dilceren 1-2mg/h
Laboratory: please see attached. Most of it I believe looks OK
As of the 13th October CT scan of the brain, it was reported to us that it is visible that there is an improvement and further on in the one from 27th October.
It was reported to us that the scanner of 27 October also shows the risk for developed hydrocephalus. The subsequent scan of the brain from 31 Oct monitored this risk and showed that for the time being it is not a hydrocephalus.
However I did a consultation with an external doctor and he advised a tap test which now I am trying to convince the unit to be done in order to exclude NPH hydrocephalus as well.
Three weeks ago the brain activity was measured via BIS Brain Monitoring System which shows results in a scale from 25/30 to 100 (100 being the brain of an active conscious person). Dad’s brain activity was measured to be 96.
The overall doctor’s opinion is that these measures and scanners’ results should correspond to a conscious brain. Unfortunately clinically this is not the case.
Dad is 72 years old in a very good health condition before the accident. Very fit and active, intelligent person (mountain hiking, skiing, cycling daily, dynamic and intellectually challenging work etc.). He had never had medical interventions apart from a light hernia two years ago and a regularly monitored and successfully controlled hypertension.
The neurosurgeon wants to plant back the bone flap which according to external doctors is not necessary right now and exposes this person to unnecessary risk of sedation while we are trying to wake him up.
I am quite new to this extraordinary life circumstances and I feel guidance is crucial which I am missing.
I am not receiving such from the doctors and the ICU either.
It seems to me that a coordinated programme for recovery is necessary among the intensive care unit, neurologists/ neurosurgeons and physio.
On the contrary the unit is only taking care of the bare minimum, I am organising the Physio – otherwise nothing is done I am fighting with skin wounds, the neurosurgeon seems to be interested only in closing the bone flap. Everybody is negative or acts with apathy. My dad will not have the chance to recover like that. And my efforts from day one are huge but in vain as am not given as frequent access to him as I would like to. It is a vicious circle.
I am native Bulgarian who lives in Brussels, Belgium. My Dad lives in Bulgaria and the accident happened there. The operation and current hospital are in Sofia – Hospital xxxxx.
The overall problem in the local health system is the post-operation recovery. And we, the family are so committed to do everything possible to bring our beloved father and husband to a place where he will receive one of the best chances for recovery.
I am exploring options to move him to Germany or Belgium to a dedicated rehab clinic. I don’t know if I am doing it right and I am not aware how the transportation could be organised but the neurosurgeon here in Bulgaria says Dad could be transported since he is breathing alone.
If you have any advice for the current situation please do not hesitate.
Apologies for the long letter. I am very confused and not aware what info may be of use thus I write everything.
I soon have to be back to work and I dread the moment when I need to organise my dad’s recovery from a distance.
I thank you very much in advance for all your time and advice in any direction. It is much appreciated.
Best wishes and thank you
Antonia
Recommended:
Dear Antonia,
thank you for being a client and thank you for using my email counselling and consulting service, I appreciate it.
Thank you for explaining and detailing your Dad’s situation.
I’m very sorry to hear about the predicament you and your family are currently experiencing.
Let’s quickly look at the positives.
The “only” injury your Dad has is the brain injury. That’s a very significant injury there is no question around that.
He’s also safe in respect to him breathing with a tracheostomy spontaneously without the help of a ventilator.
That means he has a safe airway and he’s able to breathe by himself.
This also confirms that most of his other organs are stable, including the lungs.
What’s also positive- even though you have mentioned that the ICU team is negative- your Dad is still alive after 47 days in a coma. Many ICU teams would have already tried to “withdraw treatment” after a few days of not “waking up”.
Those are the positives.
Recommended:
A lot of my clients are facing somewhat similar but different situations in the sense that ICU teams are negative from day one and are trying to coerce families to agree to “withdraw treatment” after only a few days.
The challenges are that you need to look at getting your Dad out of this negative environment ASAP, because as you have correctly pointed out, he needs to make progress and they are not doing it for him. It’s also good that he’s getting Physiotherapy 2-3 times a day.
Again, there are many Intensive Care Units where he wouldn’t get Physiotherapy 2-3 times/day!
But I also understand and know from experience that the Intensive Care team will act with more and more apathy the longer your Dad will not “wake up”.
That’s why it’s so important for you and your family to stay positive and also give the situation some meaning.
Related articles/videos
I understand that your time is limited especially since you need to get back to Brussels.
That must be very frustrating for you and your family.
I think getting him to another country, potentially Germany for Neuro Rehab, would be a positive step if you can logistically manage to get it organised
Many Rehab centres in Germany are specialised to do Neuro Rehab.
Furthermore, whilst I know that it’s frustrating to watch your Dad like this, the tests are positive and it looks like the brain has some sort of functionality according to the BIS Brain Monitoring System.
You see Antonia, what’s really important to understand is that anybody after a severe head or brain injury will need time to recover.
How much time do people need to recover after significant head and brain injuries?
Lots of time, often weeks and months.
From my experience, you can’t rush these things and even though the Intensive Care team is negative, they haven’t suggested to stop treating him.
That’s a positive!
I have worked in many Intensive Care Units where a “withdrawal of treatment” and/or “limitations of treatment” have been pushed way too early without giving Patients the chance for a meaningful recovery!
Therefore, give it more time.
Especially with the BIS brain monitoring system showing a positive result, your Dad will need time and your main job at present is to give him that time.
You may also want to have a look at this resource here for more guidance
Given that I have also worked with many Patients in the community who are either on life support with ventilation and/or tracheostomy, you shouldn’t give up, because your Dad might be able to go home with the right care and support structure.
The lab/pathology results look fine I can’t see anything of concern there.
Overall guidance is crucial in all of this and I can see why you feel it’s missing.
Here are your next steps to stay in control of the situation
- Your Dad needs to continue doing Physiotherapy 2-3 times /day to keep his muscle tones up and to keep getting stimulated
- Do not buy into any negativity, know that a recovery is possible and that it may take time
- Do not engage into “quality of life” discussions. You and your family are the only ones who know and understand what your Dad accepts for quality of life and hopefully he will come to the point where he can decide himself
- Do try and find options for Neuro Rehab
- Give the situation some meaning! Only you and your family know what meaning you can give this. Giving a difficult situation like this meaning will help you to put up with all the difficulties and challenges
- Also, given that your Dad has been very active previously should also be encouraging to you that he can recover from this
- Don’t let the Intensive Care team get away with only taking care of the bare minimum, demand the best and keep asking for it! You will only get what you ask for!
- Also, in terms of medications, he’s not on a lot of medications and it also suggests that his main problem is the brain
- It’s also a good sign that you haven’t mentioned any seizure activity. Many Patients with significant head and brain traumata often have seizures, even though he’s on anti-seizure medicine (Depakine)
- I agree to not do surgery for now and to not put the flap back on, it’s not priority for now
- With the Physiotherapy, you have not shared that they are mobilising your Dad and get him out of bed, but I would highly encourage to get your Dad out of bed into a recliner chair so that he gets stimulated
Wishing you and your family all the best
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!