Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Why Am I Being Pressured by the ICU Team to Agree to Withdrawal of Treatment for My Mom in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Isabel, as part of my 1:1 consulting and advocacy service! Isabel’s mom is critically ill in ICU and she is asking what is considered as maximum life support for her mom.
What is Considered as Maximum Life Support in the Case of My Mom in ICU?
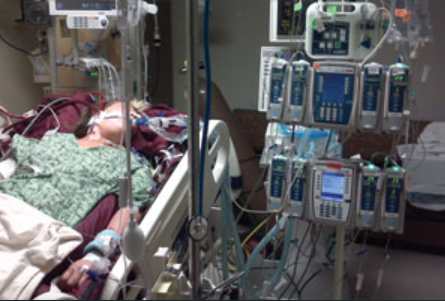
“You can also check out previous 1:1 consulting and advocacy sessions with me and Isabel here.”
Patrik: Has she had blood transfusions in recent days?
Leon: No, not that I know of.
Patrik: Okay. All right. Do you want to try ringing them again?
Isabel: Yeah, I’m trying them right now.
Patrik: Yeah. Yeah.
Leon: What is your take on Ivermectin?
Patrik: Look, I’ll tell you what my take on Ivermectin is. I don’t know enough about the drug, but what I do see as a bigger picture, is there are pharmaceutical interests that go way beyond what might be in the best interest of a patient. And you can interpret that in any way you want, what I just said.
Isabel: (Phone ringing) Hello…
Patrik: But what I do believe is that the system, to a degree, is corrupted.
Isabel: Okay, thank you.
Patrik: Because there are people who want Ivermectin, including some within the medical community, and it would be illegal for them to give it. Right? I have no take on Ivermectin one way or another, but my take on it is, well, if some people within the medical community want it and it’s illegal for them to give it. Why is that?
Leon: Yeah. Yeah. A lot of cases here happen, people are going to court for their family.
Isabel: Hello?
Leon: Yes. Hello?
David: ICU. This is David.
Isabel: Hi, David. This is Isabel again.
David: Hey Isabel. How’s it going?
Isabel: I’m just following up on my mother. I’ve just got a family friend here. He’s just kind of trying to help us understand kind of the numbers that you shared with us. Let me see if I can get him.
RECOMMENDED:
Patrik: Hey, David. My name is Patrik. How are you?
David: I’m doing well. How about yourself?
Patrik: Very good, thank you. David, I’m just trying to help Isabel and Leon to help them understand. I’m a critical care nurse by background myself, and they’ve sort of called me earlier and said, “Hey, look, this is what we’re dealing with our mom. Can you help us interpret some of the things that are happening?” Can you share a little bit more? I believe she’s on 100% FIO2 (fraction of inspired oxygen) and gases are really poor? I’m a critical care nurse by background, and I’m just trying to help Leon and Isabel to understand what’s exactly happening. And they were telling me earlier that their mom is on 100% FIO2 with really poor arterial blood gases. Is that what’s happening?
David: Yes. So, on the ventilator, she’s on 100%. And then the nitric oxide, she’s on four.
Patrik: Right.
David: With that, her last ABG (arterial blood gas) I believe was at 9:00 PM, and her arterial oxygen is continuing to trend down. I don’t have the number in front of me. I believe it was… 50? Oh, we’re doing another blood gas currently.
Patrik: Right.
David: And then the saturation, the one that’s on our bedside monitor is reading 70, seven zero.
Patrik: Oh, my goodness. Okay. Okay. And is she on pressors?
David: Yes, she is. She’s on three currently. So, she’s on Vasopressin. She’s on Phenylephrine, which is max.
Patrik: Yeah.
David: And she’s on Levo, which is about… I’m on 0.2, so I still have a little bit of leeway with that.
Patrik: Sure. Sure. And her blood pressure is… how low is her blood pressure?
David: Right now, it’s 105 over 45.
Patrik: Right.
David: We just had an episode where her heart rate went up to the 180s, and her blood pressure had just dropped down to the 60s.
Patrik: Oh, my goodness. Okay.
David: Her heart rate started dropping. So right now, y’all called just right after that happened. So right now, we have a lot of people at the bedside currently.
Patrik: Right. Sure.
David: We’re doing that blood gas at this moment.
Patrik: Yeah, no, understood. And you’ve still got, from what Leon and Isabel said, you still got dialysis going or CRRT (continuous renal replacement therapy)?
David: They did conventional dialysis during the day yesterday.
Patrik: Right. But not at the moment?
David: Correct. She’s not on any form of dialysis at the moment. We reconsulted nephrology during this nighttime, and asked if they wanted to restart CRRT, and they said they wanted to re-address in the morning.
Patrik: Right. And I guess with her blood pressure so labile, she probably wouldn’t be able to tolerate that anyway, I would think.
David: Right. I think that was their big concern.
Patrik: Yeah, for sure. And has any other treatment been tried besides the nitric oxide? Has she had Flolan nebulizer, for example?
David: Repeat that one more time for me?
Patrik: What I’ve seen with ARDS (acute respiratory distress syndrome), for example, is people on Flolan nebulizer or epoprostenol.
David: Well for me, I’m just a bedside nurse, so I’m not sure.
Patrik: Sure.
David: That’s not something I’ve seen ordered.
Patrik: Yeah, okay. That’s okay. Okay. So, you’re pretty much at the limit with 100% FIO2, you’re maxing out pressors, not looking great at the moment. That’s what I’m hearing in summary.
David: Correct. With worsening chest x-ray…Excuse me for a minute. My colleague is calling me.
Patrik: It’s okay. Thank you. While we’re waiting there, Leon and Isabel, I don’t have any other questions really at the moment because the two most life-threatening things here are they are maxing out pressors, and I can explain more of that in a minute. And they’re maxing out the oxygen levels on the ventilator. And if they can’t get either under control, your mom might have a few more hours to live, I’m afraid. That’s what I can see.
David: The nurse practitioner had mentioned to the two children about proning, which I think we are still waiting for their decision on that, but there was a concern of cardiac arrest in that event.
Suggested links:
Patrik: Yeah, no, that’s understandable, that you can’t prone her if her blood pressure is labile.
David: Right.
Patrik: Okay. Leon and Isabel, I don’t have any other questions at the moment. I don’t know whether you had any other questions?
Isabel: Oh, no. That’s been a big help. David, thank you so much.
David: Sure, not a problem. I appreciate your call.
Patrik: Thank you so much. Thank you so much, David.
David: Y’all take care.
Isabel: Okay, bye.
David: Okay.
Isabel: Okay. Yeah, I mean, that’s a big help to understand what’s going on.
Patrik: Look, it doesn’t look good at the moment. It probably depends on what’s happening in the next few hours. I think with what you shared before, what I don’t see is that they’re not trying, I don’t see that.
Isabel: Okay.
Patrik: That’s what I don’t see. Everything they’re doing seems to be in line with ARDS. As I said, the only thing that worries me a little bit is he didn’t know anything about epoprostenol. This is a question you could ask the doctor at some point. With proning, it might help the lungs. However, she’s so unstable with her blood pressure that if they were proning her now, she could go into cardiac arrest.
Isabel: Okay.
Patrik: So, with the pressors, just for you to understand that what I mean by pressors, her blood pressure is so low that they need vasopressors to constrict the blood vessels to pump the blood to the heart so that the heart can keep beating. Okay? The minute they stop the pressors, the blood will go into the periphery and the heart won’t have enough blood to pump. Right? I’m not sure whether I’ve expressed that well, but basically vasopressors are considered life support.
Leon: Okay.
Patrik: And if they took them off, her blood pressure would plummet to a level where she would go into cardiac arrest.
Isabel: Oh, okay.
Patrik: And that also then makes sense that she can’t have dialysis at the moment or CRRT. Because if they started her on dialysis or CRRT, they would take blood out of the body, and she’s already got low blood pressure. If they took blood out of the body, she probably would go into cardiac arrest.
Isabel: Oh, I see. Okay.
Patrik: It’s like a no-win situation at the moment.
Leon: So, what do you suggest?
Patrik: What I suggest is… I’ll tell you what I do suggest, I do believe you should see your mom if you want to spend some time with her. That’s what I suggest.
Leon: Okay.
Patrik: Are you allowed to visit?
Leon: I don’t know if we can. I mean, they told us that usually overnight, it’s just one person. But I know once we had barely left, they called us when we already had gotten home, and they told us to… because we’re in a whole other city. That’s the whole other situation. Well, my sister is in our hometown, where we live, and luckily, my dad and I are 45 minutes away from where my mom is.
Patrik: Yeah.
Leon: So, they had said that we can go. I don’t know if we just need to get someone to go down to be able to open the door for us.
Patrik: Right. I would think that in a situation like that, that they should give you access to see her. Hopefully she can turn this situation around. I do believe they’re doing everything they can, but whether she can turn this situation around or not, I think it’s out of your hands. It’s almost out of their hands. All they can do is support her organs and see whether she can turn it around or not.
Leon: Okay. So, let’s just say that if she is able to stabilize…
Patrik: Yep.
Leon: What would be the suggestion?
Patrik: Oh look, if she’s able to stabilize, they can probably eventually reduce her FIO2. They can probably eventually reduce the vasopressors. That would be the best-case scenario.
Leon: And what if they aren’t able to decrease the FIO2 for a while?
Patrik: Yeah. I’ll tell you what will happen if they can’t decrease FIO2. So, at the moment the blood gas reads around 50 PO2. That already suggests that not all of her organs are getting enough oxygen. And if her organs are not getting enough oxygen, and that includes the heart, eventually the heart will stop.
Isabel: After a long time. Right?
Patrik: Oh, I don’t think… no, I wouldn’t think…
Isabel: On the FIO2?
Patrik: That’s what I’m sort of saying. It’s hard to put a timeline on this, but it’s sort of a Catch-22. If they keep going up with the pressor… you’ve got a picture of this. So, if they keep going up with the pressors to maintain a blood pressure that’s compatible with life, but she’s not getting enough oxygen through the lungs, they’re pumping blood around the body that’s not saturated enough with oxygen, which means…
Isabel: I see.
Patrik: Right?
Isabel: That makes sense.
Patrik: Which means eventually it’s a vicious circle. And then there’s the question, even if they keep pumping this for a little bit longer, you could argue that if her oxygen levels in the body are low, and the organs are not getting enough oxygen, could there be, even if she does survive, there could be the question about brain damage, because the brain might not get enough oxygen.
Isabel: Right. Okay.
Patrik: Right? So those are the mechanisms at play at the moment, as far as I can see.
Isabel: Okay. I understand. Leon, do you understand?
Leon: Yeah, I understand.
Isabel: Okay. Yeah, we’ll just see where she’s at and make that trip over there.
Patrik: My suggestion is that if you wanted to see your mom, I think you should do that now.
RECOMMENDED:
Isabel: Yeah. Well, I don’t have any more questions. Leon, do you have any more questions?
Leon: No, I don’t have anymore.
Isabel: Okay. Patrik, thank you so much, so much for clarifying a lot this information.
Patrik: I’m sure we all wish we had better news for you. I’m so sorry.
Isabel: Yeah. Thank you very much.
Patrik: It’s a pleasure. Please call me if you need anything.
Leon: Thank you.
Patrik: It’s a pleasure.
Leon: Okay.
Isabel: Okay.
Leon: Thanks.
Isabel: Thank you.
Patrik: Thank you. Bye.
Isabel: All right. Good bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!