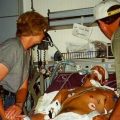
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Mom is Critically Ill in ICU with a Brain Injury. How Can I Reverse the DNR status of my Mom?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Lara, as part of my 1:1 consulting and advocacy service! Lara’s mother is critically ill in ICU with a hemorrhagic stroke and Lara is asking if her mom has pneumonia because of the ICU team’s negligence?
My Mom is Critically Ill in ICU with a Brain Injury. Is it True that my Mom has Pneumonia Due to ICU Team’s Negligence?
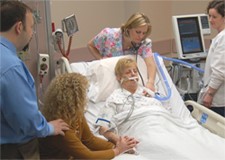
“You can also check out previous 1:1 consulting and advocacy sessions with me and Lara here.”
Lara: No, I’d need to say it to them to be honest this could help me before that they make you feel upset and then you just don’t pay again. But I didn’t want that.
Patrik: And that would be another line of argument for the DNR. So with the DNR, you go back to them and you say, Hey, we’ve discussed this with our mom before this event, what she wants in a situation like that. And she clearly wants to live, she clearly wants to fight, she has a lot to look forward to. And besides, she’s now moving, she’s squeezing my fingers. And the other thing is do you know at the moment with the GCS, do you know how often they’re checking it? Are they checking it every hour? Do you know?
Lara: I know that there’s daily but I don’t know if it’s hour.
Patrik: Okay, probably not every hour because overnight you want to have patients to sleep but during the day they should check that at least two hourly. Because everything got to be checked very regularly because there will be slight ups and downs. But if GCS is nine, I’m pleased to hear that. Now is she coughing? Does she have a cough?
Lara: Yes.
Patrik: Okay. Great.
Lara: Yes. She’s coughing. Does that add the GCS score?
Patrik: No, no. The reason I’m asking is, if she couldn’t cough or can she swallow? Do you know whether she can swallow?
Lara: No, she can’t right now.
Patrik: Okay. You see the reason I’m asking both cough and swallow is, with the cough that’s great. That means, she can clear her airway, if she can’t swallow properly. There is a chance some of here saliva, may go in her lungs and she may end up with a chest infection or pneumonia.
RECOMMENDED:
Lara: Yeah. She has pneumonia now.
Patrik: Do you know where it’s coming from?
Lara: Do you know actually, there was one negligence I found, the bed that they were using was deflating and they had to change it twice. So she was falling back into herself instead of sitting upright, that’s when it was happening.
Patrik: Say that again. What was deflating?
Lara: The bed, so they had a deflating bed. So how can I address that to make it a really serious problem on their side? Do I say gross negligence? I think that’s what caused the infection.
Patrik: Okay. Where I’m not following is, how could a deflated mattress lead to a chest infection? I’m not following there.
Lara: Because she was falling backwards a little bit. So can have some bacteria in it and they were going back into her wind valve.
Patrik: And that what I meant before, if she can’t swallow there’s a chance of… Have you heard of the term aspiration?
Lara: Yes. So they were using aspiration, but then a few times I had to say to the nurse I found what wrong and try and relieve myself.
Patrik: Okay. So, and at the moment they’re still giving antibiotics for the pneumonia.
Lara: Yes. Is there anything that I could say about the depleted bed that would-
Patrik: I think you should because the bigger picture is at the moment, you are fighting them to a degree and you need to throw things at them as much as you can. Because they’re trying to make you feel bad and to a degree, you have to use their weapons, if you will.
Lara: Yes. Yeah, I just need to get to their level, unfortunately.
Patrik: Yes, you have to, but at the same time, for example, are they mobilising her? Are they getting her out of bed?
RECOMMENDED:
Lara: No, they’re not.
Patrik: Why not? Have you asked?
Lara: I think it’s because she’s not really responding.
Patrik: Okay. I’ll tell you something. So imagine somebody with a stroke, they need stimulation, by lying in bed all day. Especially if she’s not opening eyes, she needs to be stimulated. She needs to get out of bed, right? Yes your mother is sick, but that doesn’t stop her from getting in a recliner chair. They’re specialised chairs in ICU. But here’s the other thing, especially with the pneumonia, I don’t know how much you know about a pneumonia.
Patrik: Your mother probably has aspiration pneumonia. But the reality is when somebody has a pneumonia, their lungs need to expand, to get the capacity back. And that’s not happening by lying in bed for a week, that’s happening by actually sitting up and doing some work on the chest. Not only by sitting up, but also by potentially having some physical therapy or physiotherapy. Have they done physiotherapy?
Lara: Yes. But I’m not sure what they did, I know that they touched the eyes and a few things.
Patrik: But no physiotherapy?
Lara: I’m not too sure. I don’t think they have because they only allow us to come between one o’clock, eight o’clock and do everything before hand.
Patrik: That’s ridiculous. Because, that’s like in the stone ages, visiting hours between one and eight. What do they have to hide? That’s really bad that’s, very negative. So, it’s those little things, well, they’re actually not little things, but they’re quite important things in terms of getting your mother to mobilise, doing some physical therapy-
RECOMMENDED:
Lara: Even if she’s not moving at all herself?
Patrik: Yeah, and that’s okay. They can get her out of bed, that’s why they’ve got the nurse there. That’s why they can get a physiotherapist. The nurse has a neighbour, they can ask their neighbour to help them. Don’t let them get away with any excuses. The reality is that… And here’s the other thing, in some units that I’ve worked in, some very good units, patients get mobilised on a ventilator. Your mother doesn’t have any of that, so she’s free to do that, so don’t let them get away with any excuses whatsoever.
Lara: So they mobilise them?
Patrik: Absolutely. I’ll give you another example, especially since she’s not on a ventilator. A good ICU would get her on a shower trolley and would give her a shower. That’s the best recovery doing “normal things.’ Getting out of bed.
Lara: Even though she’s not really, mobile at all?
Patrik: Doesn’t matter.
Lara: But the shower what if the water went down her mouth, would that cause issues?
Patrik: That could be an issue, but again a good ICU nurse would manage that. There is no reason they can’t do that if they can’t do it, it’s usually a matter of laziness, the culture in the unit. Because if they’ve been negative from the start and they’re talking about DNR and they’re talking about stopping the feeds, a shower is the last thing on their mind. But I go in the other direction and I say, hang on a sec this is actually a human who wants to live.
Lara: Yeah, that’s true.
Patrik: A lot of ICU are negative. They are desensitised to what you are going through, again, it’s just a number unfortunately.
RECOMMENDED:
Lara: Yeah, that’s true.
Patrik: It’s very sad.
Lara: We’re impressed in what we got actually.
Patrik: Say that again?
Lara: That’s the impression that we got. They’re obviously used to having a comeback straight away. So even when on the first day when in a really bad way, then she would say it’s not because we don’t have the time and would choose being quite snuffy.
Patrik: Other question, when she’s in bed, are they sitting her up there? Are they trying to stimulate her in bed? Do you think that’s happening?
Lara: I know that they do physiotherapy each day, but I think they might be, they’re checking the eyes and trying the legs.
Patrik: You can do little things like if your mother, for example like to listen to music, if she has-
Lara: We’re doing that, so we take her music, we talk to her, we tell her about all the people that she really like.
Patrik: That’s really important, And that’s why especially in a situation like this, I don’t like the idea at all that you can only go there between one and eight. Because she will need familiar voices around her. The more familiarity she can have the better it is. You might think, she’s not responding but the reality is, the subconscious takes stuff in.
Lara: It does. Yeah.
Patrik: So it’s those little things where you probably could do more than you think you can. And that negativity from the ICU is just not good. Tell me, have you had a formal meeting with them or how have updates been happening? How has that been happening?
RECOMMENDED:
Lara: They don’t actually update us, we have to keep calling them instead. To say, can we speak to somebody and when we call and that if the nurses maybe they’d been told that, there’s no point. Because even they’re like if I call them the answer is the same, there are no attempts for them in reply.
Patrik: So issues like with the feeds that you mentioned or with the DNR that just been mentioned sort of almost casually by when they’re passing by. Is that how it happened or?
Lara: The DNR they said to us right in the beginning and they said, we’re not operating and we’re not going do anything. And we were just all in shock then. So I even forgot about it to be honest, until you said. And the feeds well, yesterday my sister got quite upset. So I think she just didn’t have a response, so that’s why I’d like to.
Patrik: What about other things? Like, do you know whether, she’s got a healthy heart?
Lara: Yeah. Her heart is fine.
Patrik: Kidneys are fine?
Lara: Yeah, her kidneys are fine.
Patrik: Okay. Yeah, am just wondering at the moment, if her heart is fine and if her kidneys are fine. Yes, they’re treating the pneumonia with antibiotics, but I’m actually wondering what’s keeping her in ICU. I haven’t found a reason at the moment, what’s keeping her in ICU?
Lara: The infection, they said because doesn’t fight that.
Patrik: And don’t get me wrong, I think it’s great that she’s in ICU. I think that’s great because I do believe that even though they’re negative, at least she has one in one nursing at the moment. But two things you should find out. Number one, what’s their plan? Have they talked about that?
Lara: Sorry, what was that?
Patrik: Yeah. What’s their plan?
Lara: Okay. All they told us is that they couldn’t operate and they’re going to resuscitate if she stops breathing. So they really said to us. The next thing they said to us was that she’s not responding to the antibiotics.
RECOMMENDED:
Patrik: Has anybody talked about the best case scenario, I mean sounds like they’ve only spoken about the worst case scenario.
Lara: I think my sister did force them and they said, the worst case scenario she doesn’t make it and the best case is that she’s disabled, but we’re fine with that. It’s not their decision to say it.
Patrik: No it’s not.
Lara: Because she has been sending people to look after her.
Patrik: Absolutely. Okay. So, then let’s stay with the best case scenario. The other thing you should be looking for is, if she gets out of ICU, will she be going to Neuro-Rehab? You really need to go in the opposite direction here. They’re talking about stopping feeds, if she’s not going to respond to all of that doom and gloom. You need to go in the other direction, you need to ask when can she go to Neuro-Rehab? I think what’s important in this, in those situations, most of the time the ICU doctors are trying to call the shots.
Patrik: However, there would be a neurologist in the picture. And then the neurologist often have a different opinion from the ICU. So the reality is if your mom leaves ICU, ICU is out of the picture. If your mom leaves ICU, the neurologist will still be in the picture.
Lara: So I might ask them next week if the neurologist has anything to say about her progress has it been made so far.
Patrik: Very much so. And there’s a very, very high chance your mother would have been admitted to hospital under a neurologist. The primary caregiver at the moment would most likely be a neurologist, because it’s a neurological condition.
Lara: I just asked my sister actually. Sorry, and she said that when she was there, she does swallowing gulping action.
Patrik: Right. Okay. She does swallow?
Lara: She said she’s doing an action. I’m sorry. Can I just put you on hold for one second?
Patrik: Yeah, sure.
Lara: Thank you.
RECOMMENDED:
Lara: Hello?
Patrik: Yes.
Lara: I’m sorry Patrik. She just called to confirm. So what she said is that she was coughing up and then while that was happening, she made a swallowing action, specifically her throat, going up and down.
Patrik: That’s great. The other thing that’s really important in those situations as well is, your mother will need time, and you know that already. But the worst case scenario from an Intensive Care perspective is to look after a patient indefinitely with an uncertain outcome. That’s their worst case scenario, your mother needs time to recover from this, I mean she’s critical at the moment, but as time goes on every day she survives, it’s a bonus.
Patrik: It will increase the chance, number one, for her to leave ICU alive and number two, to recover and that’s why this whole mobilisation is going to be so important. She needs to be stimulated, she needs to sit up. That will help her lungs, it will help everything.
Lara: Yeah. That make a lot of sense.
Patrik: It really does. And you need to talk to the neurologist and there’s a good chance that the neurologist will have a different point of view compared to the ICU. I’m not for playing one team against the other, but it is important for you to find out what the neurologist point of view is.
Lara: Yeah. I mean they just say in the beginning, that the bleeding is big so, they wouldn’t be able to operate. But then they also said to us that she would at least survive without it.
RECOMMENDED:
Patrik: Well, it’s been five days now, hasn’t it?
Lara: Yeah, so.
Patrik: Do they measure the pressure in her brain? Do you know whether they’re doing that?
Lara: I’m not too sure.
Patrik: Okay that’s okay.
Lara: Sorry, they did. They did a nerve scan actually and they said that was fine.
Patrik: Okay. But did they put in a drain into her brain to measure the brain pressure. Do you know?
Lara: I think they did.
Patrik: Are they seeing-
Lara: But I need to double check, so basically it was a scan used to measure pressure.
Patrik: Right. Again, they can see that in the scan, but sometimes what they do is they put in a drain and measure the brain pressure consistently.
Lara: Okay.
Patrik: Doesn’t sound to me like it has happened, but-
Lara: It hasn’t.
Patrik: Okay. When they shine light in her eyes with a torch, do you know whether her pupils are reacting to the light? Do you know any of that?
Lara: I don’t think they were.
RECOMMENDED:
Patrik: Okay. You don’t think-
Lara: Then on the first day I asked her if she could see me, and she said yeah.
Patrik: Oh, on the first day she said that?
Lara: Yeah.
Patrik: Your mom?
Lara: Yeah. She did not say but I was using the hand gestures, and she said, with the hand up she could see me.
Patrik: That’s great. It’s really important for you to and that’s what I’m here for really. It’s really important that you put this situation in perspective. If your mom on day one is responding to you, that’s a very good sign. Why is this important? Because I can tell you, I’ve seen patients with strokes over the years, and they’re not responding at all, they may not respond for weeks. So there is a loss, and most stroke cases that end up in ICU there will be a lot of them with the GCS of three, four or five. That’s not the case.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!