Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question last week was
You can check out last week’s episode by clicking on the link here
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another question from one of our clients which are excerpts from email counselling and consulting sessions with me and the question this week is
My husband had open heart surgery with complications! He’s not “waking up”, he needs 100% of oxygen and now he’s bleeding from the stomach, I’m so scared, help! (PART 1)
Other parts of this series of questions you can look up her PART 2, PART 3, PART 4, PART 5 and PART 6
This was another great series of questions where I was able to “hand-hold” a very anxious and distressed client through a very stressful and complex situation.
Katie writes
Hi Patrik,
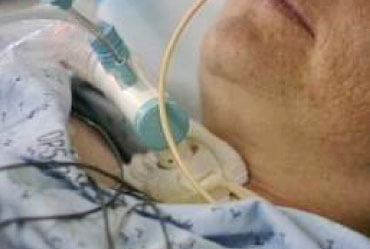
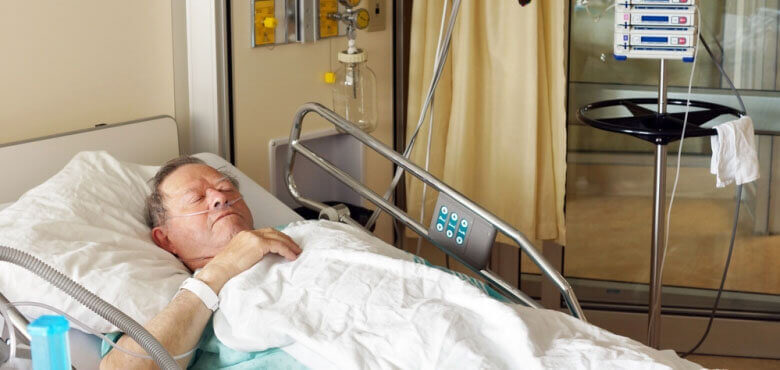
my 70 year old husband had aortic valve replacement(=AVR) yesterday. He is still in Intensive Care with the ventilator supplying Oxygen at 100%…
During the surgery they discovered a hole in his heart between the chambers and that is why his lungs have no Oxygen and therefore he isn’t able to breathe on his own.
All vital signs after surgery are good except the breathing. He has been kept sedated since surgery. The blood is flowing between the two heart chambers and therefore not enough oxygen is getting to the lungs.
One option is to open him up again to repair the hole which they called “severe”…he has told me often that docs have told him he had a hole in his heart from years ago that posed no problems, I guess I am so scared for him. Can you please shed some light to what I should be doing to help my husband?
Thank you so much,
Katie
Here is my response
Hi Katie,
thank you for making contact and sending your questions through and thank you for using my 1:1 email counselling and consulting services!
I’m very sorry to hear that your husband is going through some complications after what often is “straight forward” surgery having an AVR.
I’m also very sorry to hear that your husband can’t come off the ventilator since he’s had the Aortic valve replacement (AVR).
There is a high chance that your husband needed the AVR because of the “hole in the heart”. A “hole in the heart” is usually also defined as a VSD (=Ventricular septal defect).
A lot of literature suggests that a VSD is causing aortic regurgitation, causing aortic valve incompetence, hence the requirement for surgery.
I really don’t understand why they haven’t closed the VSD during the surgery or why they hadn’t identified the VSD as a significant risk factor before your husband was going into surgery for the AVR.
There is a high chance that your husband also has high pressures in his lungs (=pulmonary hypertension) from the VSD that they will most likely treat with Nitric Oxide (NO).
Besides 100% of oxygen is your husband also getting nitric oxide (NO) with the ventilator?
Other treatment options for high pressures in the lungs (=pulmonary hypertension) are Prostacycline (Flolan) nebulizers as well as Sildenafil (Viagra) tablets.
Therefore, before oxygen requirements can go from 100% to <40% on the ventilator, there is a very good chance your husband will need to stay in an induced coma.
For now they will most likely keep him on 100% Oxygen on the ventilator overnight as well as the Nitric Oxide (=NO).
They will keep measuring his PA (=Pulmonary artery pressure) in his lungs and they will wean NO accordingly if his PA pressures come down.
They will also keep monitoring his Arterial blood gases and wean his oxygen accordingly if possible.
Your next steps are to ask the doctors what their plan is to improve the oxygenation to the lungs.
It almost sounds to me like he will need to go back to have surgery and have the VSD closed, because otherwise he won’t be able to come off the ventilator and the breathing tube.
Related articles/videos
The next steps for you really are to get the Intensive Care team as well as the cardiac surgeon to discuss your husband going back to the operating theatre to have the “hole in the heart”(=VSD) closed.
This may well pose high risk, especially since your husband is already on 100% of oxygen after the surgery and potentially on Nitric Oxide (=NO) or Prostacyline (Flolan) nebulizers.
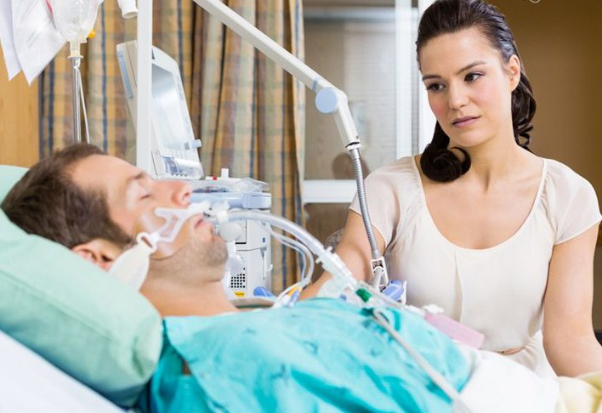
Even though you haven’t mentioned specifically, I’m certain that your husband is also on Vasopressors or Inotropes to help with a potentially low and life threatening low blood pressure.
This poses another significant risk for your husband to have the VSD repaired, as those high levels of life support make it very risky for your husband to have surgery.
Therefore, the next step for the Intensive Care team is to check his heart via an echocardiogram or with a TOE (=transoesophageal echocardiogram) to check out the functionality of the heart and also assess the risk to take him back to surgery.
On the one hand, the sooner they can repair the “hole in the heart”(=VSD= ventricular septal defect), the higher chances are to get your husband out of the induced coma and to get him off the ventilator, on the other hand, if he’s not stable enough, the risk factors to take him back for surgery is huge at this stage.
Therefore, getting your husband more stable, potentially weaning down the 100% oxygen as well as the Nitric Oxide and the Vasopressors (Inotropes) will make a return to the operating theatre/operating room less risky.
Returning back to the operating theatre/operating room is going to increase the risk for other complications to occur such as bleeding, Pneumonia and Atrial fibrillation to mention the most common and also the most dangerous complications after such type of surgery.
The reason Pneumonia and bleeding are so common after open heart surgery is simply that during open heart surgery a Patient is almost always put on a Bypass machine that takes over the function of the heart and the lungs during this type of surgery.
Whilst on a Bypass machine, the lungs are collapsed therefore significantly increasing the risk for a Pneumonia to develop.
Furthermore, whilst on a Bypass machine, blood thinning medicine such as Heparin is given which is increasing the risk for bleeding after surgery.
It sounds to me like there is no other choice but to take your husband back to get the VSD closed, however they need to assess the risk first and get your husband more stable before taking him back for surgery.
From my experience, I would imagine that your husband may stay in Intensive Care for at least one to two weeks from now on given everything that’s been happening.
Let me know what other questions you have and I will guide you.
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!