Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question and CASE STUDY last week was Part 1 of
You can check out last week’s episode by clicking on the link here.
This was another great case study where you can see how I can help a very concerned and very distressed client how to quickly make sense in a situation where the Intensive Care team hasn’t been open transparent with her and her family!
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another question from one of our clients which is an excerpt from an email counselling and consulting session with me and the question this week is
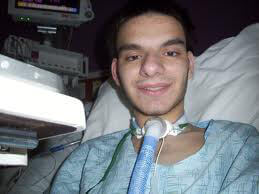
My 32 year old son has an anoxic brain injury with a tracheostomy and I want him to “wake up”! Now they are giving him more sedatives, help!
Hi Patrik,
my 32 year old son was suffocated and lost oxygen resulting in anoxic brain injury.
He was in the coma from Thursday 7th of this month, the doctors said : no hope of recovery since day one and that he would remain in a vegetative state.
On the 15th they did the tracheostomy and since than I saw some improvements because he started to move his legs, his arms and his head and at times opening his eyes but he has not been trying to talk yet.
He’s still intermittently ventilated overnight but he’s off the ventilator during the day.
This morning I went to visit and the nurse told me that they gave him sedatives to control his movements because he almost fell off the bed.
His oxygen level this morning was about 85%. Normally it’s around 95% -100% My question is if the sedative is going to interfere with his attempt to wake up or recover. Please let me know anything you can as soon as possible thank you so much.
Many thanks
Avanka
Here is my response!
Hi Avanka,
Thank you for being a client and use the email counselling and consulting service.
You see Avanka, it looks like your son has fallen prey to the Intensive Care teams negativity. Most families who come to us at INTENSIVECAREHOTLINE.COM have the number one complaint that Intensive Care teams or “the doctors” are negative!
This negativity is probably even worse when it comes to head and brain injuries. Why?
Because unlike any other organ, the brain can’t be controlled.
Any other organ, whether the lungs, the heart, the kidneys or the liver can be temporarily controlled and function replaced by mechanical ventilation, ECMO, kidney dialysis etc…
The brain function cannot be controlled and not be replaced at this stage, even though I believe this might be a possibility in the future!
The problem with head and brain injuries is simply that it probably has the most uncertain outcomes out of all admissions into Intensive Care for the reasons that I just mentioned.
Therefore, unless you and the doctors will give your son time, you simply don’t know the outcome!
Related article/video:
My experience has shown me that the best outcomes in head and brain injuries come over time.
This time is often not granted by Intensive Care teams and by the doctors because of what’s happening “BEHIND THE SCENES” in Intensive Care!
The reality is that you are looking for a solution for your son and the Intensive Care team is looking for a solution for their Intensive Care Unit.
What’s a solution for you?
To get the best possible care and treatment for your son and most of all, he will need time and positivity to recover!
This will take time, resources, effort, nurturing and a lot of patience!
Therefore, time is the best healer!
I have seen some Patients with severe head and brain injuries-including anoxic brain injuries- being in Intensive Care for many weeks and sometimes many months and the more resources, time, patience, efforts and nurturing you give to these Patients the better the outcomes!
Some of those Patients stayed in Intensive Care for up to 6 months and they left ICU alive and went on to rehabilitation.
Why did they stay in ICU for up to 6 months? Because they had lots of issues such as ongoing high brain pressures that needed to be managed and they also needed Haemodialysis for kidney failure etc…
So much is dependent on the culture in an Intensive Care Unit and unfortunately most Intensive Care Units are negative and want to “pull the plug” as early as possible! Sad but true!
Some of those Patients I have seen have been in induced comas for many weeks and yet they recovered.
Related article/video:
To answer your original question, they shouldn’t have re-sedated your son just because he was starting to move his legs and arms!
Those are actually good signs and they show progress!
I would almost argue that with the Intensive Care team being so negative that they almost want to supress any positive signs in order to make management of your son easier for them!
For example, if they keep giving sedatives even though your son is showing signs of movement and improvement it also makes it more likely for your son needing the overnight ventilation.
The goal for your son should be to be more awake, getting out of bed and stimulate him so that you and the Intensive Care team can get an idea what his level of functioning is going to be!
You are not going to get that by sedating him.
It’s also concerning that your son’s oxygen levels have dropped. Again, side effects of getting sedatives is respiratory depression and therefore he may have shown minimal breathing efforts due to the sedatives.
Again, as next steps, your son needs to be off sedatives, he needs to be stimulated, he needs to have Physical Therapy, he needs time, nurturing and positivity!
Then he can hopefully get off the ventilator and maybe even have the tracheostomy removed eventually.
Your goal for now should be to get your son out of Intensive Care and off the ventilator and then on to neuro rehabilitation!
Next, the best resource besides my 1:1 phone or email counselling, consulting and advocacy is this resource here
It sounds like you are a good advocate for your son and it sounds like you are not giving up anytime soon!
But you also need to know and understand what’s happening “BEHIND THE SCENES” in Intensive Care and you need to know and understand why the Intensive Care team is negative, why they are doing the things they are doing and why they are saying the things they are saying!
Again Avanka, you are looking for a solution for your son and the Intensive Care team is looking for a solution for their Intensive Care Unit!
Their worst possible scenario from an Intensive Care perspective is that your son will be occupying an Intensive Care bed for many weeks or even months to come.
Therefore they keep giving you negative “doom and gloom” speech so that they can have their way eventually and if you are like 99% of the families of critically ill Patients in Intensive Care you will give up and you will give into the “perceived power” and the “perceived authority” of the Intensive Care team!
The fact of the matter is that if you do that, you and your son will be another “casualty” of the Intensive Care team.
Therefore you need to go against the grain and you need to speak up and keep fighting for your son!
What’s the solution the Intensive Care team is looking for?
Well, again their worst possible scenario is that your son will be occupying an Intensive Care bed for the next few weeks or even months!
Intensive Care beds are scarce, expensive and “in-demand” resources!
Therefore, somebody else is already knocking at your son’s ICU bed that me a more profitable and/or more interesting case for the Intensive Care Unit.
For example, all Intensive Care Units do medical research and it’s a revenue driver for them. If your son is not enrolled into a medical research study, the Intensive Care team may not have an interest in giving your son the best possible treatment and care!
They may prefer looking after 70 year old Mr Smith after open heart surgery because he’s been enrolled into a medical research study.
That’s why it’s so important to know and understand that Intensive Care is often not “what you see is what you get”!
The best way to know and understand what’s happening in Intensive Care “BEHIND THE SCENES” and then use that knowledge to start managing the Intensive Care team is this Ebook here
This Ebook will give you a deep understanding of how Intensive Care Units operate “BEHIND THE SCENES” and how they position your son’s diagnosis, prognosis, care and treatment!
Your job as your son’s advocate is to position your son’s diagnosis, prognosis as well as his care and treatment in a positive light, because if you don’t the Intensive Care team will do it for you with an outcome that you won’t like!
You need to stay in control of your son’s fate and destiny!
Again, I can help you in positioning your son’s diagnosis, prognosis, as well as his care and treatment here with my 1:1 counselling and consulting so that you can get the outcomes for your son that you want, need and deserve!
Last but not least, please make sure that you also have a look at INTENSIVE CARE AT HOME.
INTENSIVE CARE AT HOME is a home care service providing tracheostomy and ventilator care at home as a genuine alternative to a long-term stay in Intensive Care!
I hope this helps!
Your friend
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



