Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another frequently asked question from our readers and the question last week was
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer another question from one of our readers and the question this week is
My Dad is in Intensive Care on BIPAP for COPD, should he be having a tracheostomy?
This question from Emma is from a 1:1 phone counselling and consulting session with me.
Hi Patrik,
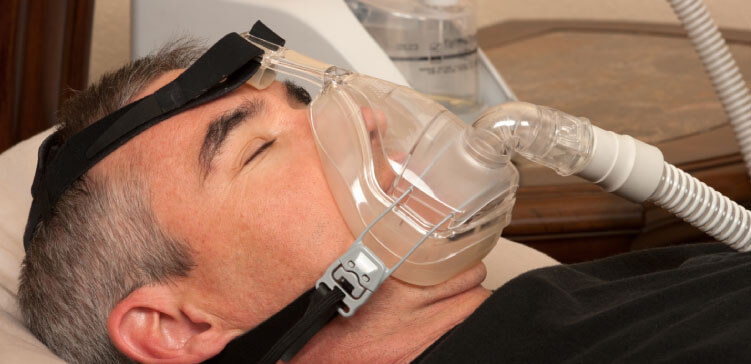
my 87 year old Dad is currently in Intensive Care and has been for the last 4 days. He is on a BIPAP machine with a face mask for high CO2(Carbon dioxide) as he has been suffering from COPD for a few years now.
He has been in good health generally speaking and he has been living independently.
About 12 months ago he has had cardiac surgery for an Aortic valve replacement. He recovered fairly well from that given his age, however his COPD has been causing more and more trouble since.
He’s now at the point where he has been in hospital for about a month, initially two weeks in ICU, where he was on the breathing tube, ventilator and in an induced coma. He managed to get off the ventilator, he was discharged to the ward however, his CO2(Carbon doxide) kept climbing and he got readmitted back to Intensive Care 4 days ago.
As I mentioned, he’s now back on a face mask for BIPAP and they are managing to keep his CO2(Carbon dioxide) down that way.
His CO2 levels are climbing around 75 mmHg off the BIPAP.
He also as a lot of sputum at the moment that he can’t clear himself and the doctors are telling us with a tracheostomy it would be easier to manage the sputum as well.
The Intensive Care team has asked my Dad whether he wanted to have a tracheostomy, as they think that given his COPD and high CO2, he won’t manage to get off the ventilator with a normal breathing tube.
My Dad has already agreed, but I’m having second thoughts and I’m not sure whether a tracheostomy will cause more suffering and just prolong the inevitable.
What do you think?
Many thanks
Emma
Dear Emma,
thank you for your question and thank you for using my 1:1 phone counselling and consulting service!
Your father is in a very unusual situation, given that he’s tolerating the BIPAP and they are now wanting to do a tracheostomy.
The reason I’m saying he’s in an unusual position is that most Patients in Intensive Care go from a breathing tube to a tracheostomy and not from BIPAP(with a face mask) to a tracheostomy.
It’s good that he’s agreeable to have the tracheostomy, however you, your family and your Dad really need to think through whether he wants to go down that path.
I guess what you and your Dad would be looking for is if the tracheostomy will be achieving the goal to going back to a quality of life that is acceptable to your Dad and to the rest of your family.
It’s obvious that your Dad wants to live despite the challenges and setbacks he’s currently going through and he’s obviously prepared to go through the procedure to have a tracheostomy without fully knowing what the outcome is going to be.
Your Dad’s worsening COPD will always push his CO2 up and he would be getting confused, lethargic and sleepy with an ongoing high CO2.
A tracheostomy and intermittent ventilation would be a good management strategy to manage the CO2 effectively and keep it within normal levels.
I understand your concerns that at your Dad’s age of 87 a tracheostomy would just prolong the inevitable.
That may well be the case, however by having a tracheostomy he’s giving it the best shot and you will soon find out if he can improve his situation or if he can’t.
But even if he can’t improve his situation straight away, a tracheostomy will give him more time to recover and improve his CO2 and his breathing. A tracheostomy tends to leave a lot of flexibility around mechanically ventilating your Dad when he needs it and he can stay off it when he doesn’t need it.
Also, if he is currently producing lots of secretions a tracheostomy will help to manage those secretions too by having access to suctioning via the tracheostomy.
Especially when Patients are producing copious amounts of secretions with a weak cough, a tracheostomy is very advantageous to manage secretions effectively through suctioning.
The next question you may want to look into and also discuss with your Dad are issues such as the potential for end of life.
Maybe your Dad already knows that a tracheostomy will just prolong the inevitable, however at the same time he may not be ready to die yet and he wants to have the tracheostomy to have more time.
Also, quality of life is a very subjective experience and what some people might find acceptable as for their quality of life other people simply wouldn’t find it acceptable.
It’s for the individual to decide what’s acceptable for their quality of life and by the same token we simply don’t know what our quality of life may look like after some major health issues and/or critical illness!
The same applies to you and the rest of your family. Do you want to have more time with your Dad? A tracheostomy might facilitate this.
And the good news is that it doesn’t have to be in a sterile, depressing and institutionalized Hospital or ICU.
Once your Dad is having the tracheostomy and needs intermittent or even permanent ventilation to manage his CO2, he could still go home with services like INTENSIVE CARE AT HOME.
A service like INTENSIVE CARE AT HOME is specialized to look after ventilated adults& children with tracheostomies and it provides a genuine alternative to a long-term stay in Intensive Care/ LTAC.
Therefore in this day and age a tracheostomy doesn’t necessarily mean that your Dad will spend a lot of time in ICU as long as you keep looking for the right options and as long as you keep making the right choices and decisions.
Here are also links to a couple of articles and videos that will explain more about tracheostomy in Intensive Care and the options.
Doing a tracheostomy may well be the right thing to do, however you and your Dad also need to know about the risks and benefits.
Generally speaking we get lots of questions about tracheostomy and it’s a subject that we are highly specialized in.
What’s also important to know is that with Patients with COPD, tracheostomy and ventilation we have experience at INTENSIVE CARE AT HOME to successfully make a transition home and improve our Client’s quality of life and/or quality of end of life.
We had a client at INTENSIVE CARE AT HOME who spent a good couple of years at home after they had a prolonged stay in Intensive Care and the gentleman had a tracheostomy, COPD and needed intermittent ventilation.
Him and his family where ever so grateful to have that time at home instead of in Intensive Care and him and his family where very grateful that he could approach his end of life at home instead of Intensive Care.
Maybe your Dad is thinking along those lines.
87 years of age is not an obstacle to have a tracheostomy and then go home even if it means your Dad will need intermittent ventilation.
Again, INTENSIVE CARE AT HOME can make that transition from Intensive Care to home possible for your Dad and for your family.
By the same token, the Intensive Care unit might be in a position to wean your Dad off the ventilator and the tracheostomy if they think it’s achievable.
If they can eventually wean him off the ventilator and the tracheostomy he may be able to “get away” with intermittent BIPAP(=Non-invasive or mask ventilation).
And that can be done at home as well and it’s often mainly a night-time activity. Especially during sleep CO2 keeps rising if not managed appropriately with BIPAP.
Therefore if your Dad chooses to have the tracheostomy, you now have a better understanding of what the options might be down the track.
Also, last but not least, I would like to mention that a tracheostomy is generally not causing any discomfort or pain for Patients, but is obviously a foreign body in a Patient’s neck and I also need to point out that a tracheostomy obviously needs specialised care.
I also believe that if your Dad finds down the line that he’d rather not live with a tracheostomy once he has it, there would still be time to remove it and look at palliative care options.
But for now, just keep looking at the positives and for now my advice would be to support your Dad in his decisions because I’m sure he hasn’t taken those decisions lightly.
Wishing you and your family all the best!
Your friend
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



