Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question from one of my clients Steven, which are excerpts from a 1:1 phone and email counselling and consulting sessions with me and the question this week is
CASE STUDY: MY DAD’S BEEN IN ICU FOR SEVERAL WEEKS WITH ARDS, CARDIAC ARREST AND DIALYSIS! HE’S GOT A TRACHEOSTOMY, DOES HE HAVE A REALISTIC CHANCE OF SURVIVAL? (PART 2)
You can also look up PART 1 of this 1:1 phone counselling and consulting session here.
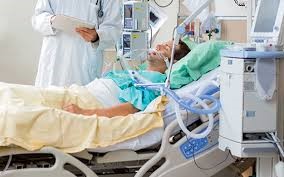
Steven’s father has been in ICU for several weeks now after he suffered from severe ARDS(lung failure), had a cardiac arrest during his time in ICU and now he’s in multiple organ failure with the lungs failing, the heart failing and the kidneys failing. Steven is obviously extremely concerned and he wants to know what decision he should be making about continuing life support for his Dad.
We discuss his Dad’s future quality of life if he survives his stay in ICU and we also look at what’s best for his Dad by looking at the level of suffering his Dad is going through.
Patrik: Patrik speaking, intensivecarehotline.com, how can I help?
Steven: Hi Patrik, it’s Steven.
Patrik: Hi Steven, how are you?
Steven: I’m okay.
Patrik: Yeah, that’s great, I can hear you well.
Steven: Oh, you can hear me well. Okay. So do you want to talk now?
Patrik: I can talk now if you like. It’s up to you.
Steven: Okay. So, yeah look, my father’s condition is still as it is, so he’s still on life support through a ventilator. He had a dialysis yesterday. He did very well, they pulled out 2.4 litres out of him. He’s on intermittent dialysis. They pulled out 2.4 litres…
Patrik: Right.
Steven: … out of him, but he’s still has fairly acidotic in his blood, on his ABG report. He is still in moderate ARDS(=lung failure). And he’s still on the vent …
Patrik: Right, right.
Steven: … so he’s still on that. And he’s still on Fentanyl, which is a pain medication. He was on Propofol earlier, but he’s been taken off of that.
Patrik: Right.
Steven: And so, when I try talking to him, he moves his eyes, but he’s not responsive. I try to tell him to blink his eyes, often sometimes he is, sometimes he’s not. So, what’s …
Patrik: But that sounds way more positive than when we spoke a few days back.
Steven: It’s positive, but he still needs life support …
Patrik: Sure.
Steven: His lungs are really bad. He’s not on vasopressors(=inotropes) anymore, but kidneys are not functioning. He hasn’t produced a drop of urine in 48 hours, so he needs dialysis, and he is incredibly flush because he has a lot of liquids and fluids in him. So, he’s that. So it’s positive in some sense, but also, it’s still not great.
The doctors are not that hopeful that he’ll be able to make it out of the ICU because a lot of the drugs that he needs to just stay stable, the vasopressors(=inotropes) and the Fentanyl and the sedation medicine, Propofol, he can’t get outside of the ICU, so the doctors are of the view that, “Look, he’s going to be …” They don’t know if he’s …
It sounds like … his chest x-ray looked a little bit better than yesterday, so that was something good that they said. He did the dialysis and they needed to use blood pressure medicine to keep his blood pressure up during the dialysis. The dialysis was very successful, they took 2.4 litres out on… so that’s that.
So, yeah look, I mean that’s the status now.
Related:
Patrik: Yeah. You see, what I can see, just by what you’re telling me is, if he’s off the vasopressors(=inotropes), that means his heart is strong enough to cope with whatever is happening at the moment, right. That’s one thing that I can see with him being off the vasopressors(=inotropes). If they’re taking off 2.4 litres within 24 hours, and again, he’s staying off the vasopressor, that to me, is a sign that his heart is coping with whatever is happening.
Obviously, with the ARDS(=lung failure) and statistics rate still not being clear, that is certainly an ongoing concern, but at the same time, if somebody is off vasopressorS(=inotropes) in ICU, it’s clearly a good sign. It’s also a good sign that they’re weaning off the Propofol, right.
I mean, all he’s o n now is …
Steven: Yes, sorry, sorry. Weaning what?
Patrik: The Propofol. Did you say he’s off the Propofol?
Steven: Yup.
Patrik: Right. That’s all …
Steven: Yeah. He’s off the Propofol.
Patrik: Yeah.
Steven: Yup.
Patrik: So, that’s … You know, yes, he’s on life support, but he is on the ventilator and he is on the dialysis machine. There’s no other life support. Yes, they are major forms of life support, but what’s their concern if they continue treating?
Steven: I don’t know. They will continue treating, but they’re doing another … They’re having us do another session with palliative care …
Patrik: Right.
Steven: … sometime this week, on Friday. And the question becomes really, quality of life, right?
Patrik: Sure.
Related:
Steven: His quality of life will never from where he was before, that’s clear, so that becomes the question that’s going to be discussed. So we still think, from what we’re hearing, I think they’re going to continue the treatment and keep it as is, but they still thinks it’s a low probability that he’ll be able to make it out of the … Forget about getting out of the hospital, just making it out of ICU, they think is low probability.
Patrik: Yeah. Sure, sure. And that … I guess you never know what the outcome is going to be. I guess the question from my perspective, really is, “Do you want to keep trying to get him out of ICU alive?” You know, I guess that’s … You don’t know what his quality of life is going to look like if he makes it to that point. And neither do the doctors, right?
Steven: Yeah.
Patrik: I guess you could approach this whole situation with the goal of getting your dad out of ICU alive. And then see what happens. If you want to continue working towards that goal, then I can certainly support you with that.
Steven: Right. Right. What’s your take on the situation, given what I’ve told you?
Patrik: Yeah. Yeah, yeah. So just remind me quickly, your dad’s been in ICU since September, is that correct? 26th …
Steven: Yeah, he was … End of September, he was admitted, and then he was intubated(=insertion of the breathing tube) October 6th. So, he was intubated February 6th, and then moved to this hospital, which is more of a larger facility with 24-hour care, support, and monitoring. It’s a very good university for critical care.
Patrik: Yeah. Yeah. Look, it’s … Look, I can tell you anything that’s happened in Intensive Care. What I can’t tell you is what … if he gets out of ICU alive, what his quality of life will look like in the future. You know, I don’t have a crystal ball. But what’s my take on the situation?
Steven: Right.
Patrik: If he’s not suffering, and you want him out of ICU, as long as he’s not suffering, then I think, you know, that is something you may want to continue doing. That would be my take.
Steven: How do you know if he’s suffering or not?
Patrik: Okay. Yup.
Recommended:
Steven: Because I tried asking him to blink his eyes a couple of times if he’s in pain, and I asked him to try blinking his eyes hard if he remembers me. He did that. I asked him a series of questions, and then one of the questions I asked was, “Blink your eyes hard if you think you’re in pain.” He did, and I said, “Blink your eyes hard if you are … if you want me to get more pain medicine for you,” and he did. And then I tried asking him again, in front of the nurse, and he didn’t do it this time.
Patrik: Yup. Okay, okay. Look, there’s two things that I can see here, number one is, his brain is intact, even if he’s doing that intermittently, that means his brain is functioning. I guess the other question, and that could be the most important question, what do you think your dad would want if he was in a position to make his own decisions. What do you think he would want?
Steven: You know, he has a medical directive, and the directive says, “If there was no hope for him, then he would want” … he had some specific things, but it’s unclear, given this situation because it appears it’s not a terminal issue right now.
Patrik: No. No. And I can tell …
Steven: It’s a grey issue here.
Patrik: And the thing is, there are no right answers in a situation like that. There are only right answers for you and your family, right? The Intensive Care doctors alway say, “Yeah, we know what’s best. We think it’s in the best interest of your dad,” blah, blah, blah. We know all of that, but at the end of the day, as long as you, as the medical power of attorney, can make a decision that you think is a decision that your dad and the rest of your family would support, then I think that’s what you should be going with, if that makes sense.
Steven: Mm-hmm (affirmative), Mm-hmm (affirmative)- got it. Got it.
Patrik: And the other thing that I can tell you is, one of the things that we’re doing here in Melbourne is we also operate an INTENSIVE CARE AT HOME in-home nursing service, right, and most of what we’re doing there is for long-term intensive care patients. And some of what we’re doing there is palliative care at home, right.
And I’m not saying that is applicable for your dad’s situation, I’m not saying that at all, but what I am saying is that, some patients and some families, they want to spend the last few days, sometimes the last few weeks, sometimes the last few months, in the comfort of their own home. And as I said to you, there is no right or wrong answer, it’s just what you feel is the right decision for you, for your dad, and for your family. That’s what it’ll come down to within in the context of what’s medically possible.
Related: INTENSIVE CARE AT HOME services
Steven: Right.
Patrik: Does that make sense?
Steven: Right. Yup.
Patrik: And if you feel … The only thing that I would say is, if you feel that your dad is unduly suffering to get to an outcome that is uncertain, then you might have to rethink your strategy.
Steven: Right, right.
Patrik: But as long as he’s not unduly suffering …
Steven: How do you know that someone is unduly suffering? That’s the thing.
Patrik: Yup, yup, yup, yup.
So, how do you know if he’s unduly suffering? I think you can clearly see by his body language, really. You know, I mean, he can’t talk. But you can see by his body language, I mean that’s how a nurse or a doctor would judge that, by paying attention to his body language. By the body language, but also, from a nurse or a doctor’s point of view, then looking at how much pain medication is he getting and so forth.
Steven: Right. But he’s on 30 mcg/hr of Fentanyl …
Patrik: An hour. What’s your dad’s weight, roughly?
Steven: He was weighing … Before the whole thing, before he came to the hospital, he’s lost a lot of weight …
Patrik: Yeah, he would have.
Steven: He was weighing around 150, call it, 152.
Patrik: Right.
Steven: Pounds.
Patrik: Pounds. That would be …
Steven: That’s about … Call it, let’s say …
Patrik: 70 kilos?
Steven: Let’s see. Let me see how much …
Patrik: Yeah, we can do …
Steven: Yeah.
Patrik: Yeah. Okay 30 mcg/hr … If he gets 30 micrograms …
Steven: That’s 70 kilos.
Patrik: Yeah, right. If he gets 30 micrograms an hour, for days,
Steven: … and everything. All right, look, I mean, it’s given me a lot to think about. I definitely think a goal was to get him out of the ICU, but his quality of life and whether he’s unduly suffering is a big question mark and everything.
Patrik: Right. And look, I think given that he’s got a tracheostomy, I think chances are relatively low that he’s unduly suffering. I mean, you know, don’t get me wrong, I mean intensive care treatment is one of the worst things somebody can ever go through, but having a tracheostomy is making that a lot easier compared to a breathing tube, and you would have noticed the difference by now.
Steven: Yeah. Yeah.
Patrik: You know, what I can do is, I can’t give you the right answer, what I can do is I can guide you because I’ve seen it over and over again. You know, miracles do happen. They do happen. They happen rarely, but they do happen, and at the end of the day, it comes down to what you think is right from a family perspective. That’s what it comes down to, I believe.
Recommended:
Steven: Mm-hmm (affirmative), Mm-hmm (affirmative)-
Patrik: And you should trust what you and your family want. You should trust that. I think that’s your biggest wisdom because the doctors don’t know your dad. The doctors don’t know your family, I don’t know … but you have that wisdom. What your family is prepared to put up with, and what your dad would be prepared to put up with. That is your wisdom.
Steven: Right. Right. Okay. So, look, what do you think is next?
Patrik: I can also dial into the family meetings you have with the doctors, if you want me to do that, talk to the doctors, talk to the nurses, if you want me to do that. I can talk to any other family members, if you want me to that to explain your dad’s situation to them also.
Steven: Okay. All right, I’ll send you a message. Let me sleep on it tonight and then we’ll take it from there. We have a family meeting with the doctors and the nurse in charge on Friday 2pm, can you be there over the phone?
Patrik: Yeah. Sure, Friday 2pm works fine for me.
Steven: Okay?
Patrik: Absolutely.
Steven: Okay.
Patrik: All right.
Steven: All right. I’ll be in touch tomorrow!
Patrik: Take care, have a good night.
Steven: Okay. Good night.
Patrik: Good night. Bye, bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!


