Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
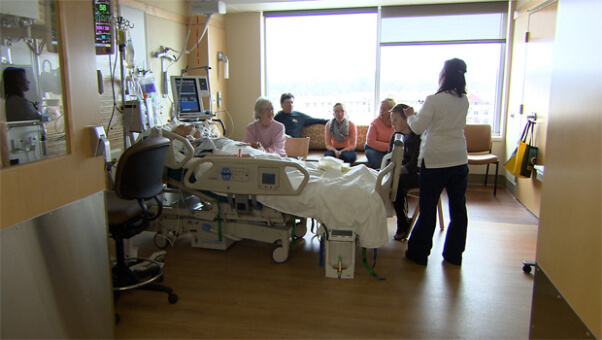
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM , where we instantly improve the lives of Families of critically ill Patients in Intensive Care, so that you can have PEACE OF MIND, real power, real control and so that you can influence decision making FAST, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of YOUR QUESTIONS ANSWERED and in last week’s episode I answered another question from one of our readers and the question of the last three episodes was
“My Mum has been in ICU for three weeks now and she is on ECMO for ARDS! Will she survive?”(PART 1), (PART 2) and (PART 3)
As Ellie’s Mum continues to be in Intensive Care for many weeks, Ellie had many questions so therefore we stayed in contact and it became a three part series where you can look up PART 1 here, PART 2 here and PART 3 here
Ellie has also been featured in our PODCAST in an interview that you can check out here.
In this week’s episode of YOUR QUESTIONS ANSWERED I want to answer another question from one of our readers and this week the question is
“My father has been admitted to Intensive Care with a brain clot. He therefore had surgery on his head around one month back, performed by neurosurgeons and he’s still unconscious. HELP!”
Hi Patrik,
My name is Aatish and my father has been in Intensive care for 32 days. To start with on 24th May his right side was unmovable so we admitted him to hospital on 25th May. Then hospital staff did his CT scan & MRI of his brain in which they found two blood clots.
He therefore had surgery on his head around one month back, performed by neurosurgeons and he’s still unconscious.
Now the Intensive Care team is saying that there has been a lack of oxygen supply to his brain, which is causing him to be unconscious. According to the Intensive Care team, they appear to be at a loss and they are saying there is no medication, no medicine that can help him in this situation!
Therefore me and my family are anxious to wait and watch whether he will recover or not. The Intensive Care team is not giving us any assurance whether he will recover and wake up or not.
I just wanted to ask what you think can be done in his case, whether there is any medication or something else which will help my father to recover?
My father is 67 years of age and he has a history of high Blood pressure for which he is already taking medications and he has Diabetes as well.
The exact MRI report is outlined below:
Subacute right frontal and posterior parieto-occipital SDH with max thickness of approx 7mm without significant mass-effect.
A large left fronto-parieto-ocipital acute on chronic SDH is seen with max thickness of approx 2.6 cm with mass effect on the adjacent brain parenchyma with midline shift to left of approx 0.9 cm.
Then neurosurgery (Craniotomy) was done on 26th May. Before going to surgery & after surgery, my father was conscious but as he started getting convulsions, sedation was given to him & since then he has not been conscious.
After surgery his CT scan was done on 28th May & on 31st May which has shown that both left side & right side clots were successfully removed.
Then on 31st May his Tracheostomy was done.
Meanwhile he has undergone many complications like having swelling to his kidneys, continuous fever, lack of urine output, lose bowel motions, complete body swelling due to non body movement.
The Doctors have done all possible tests meanwhile like checking infection in blood, stool test, cough test, etc.
Now his kidney swelling is getting worse, his creatinine is rising even though his urine output is still 100ml/hour.
On 21st June again we have done an MRI of his brain which shows nothing new.
The exact report is mentioned below:
– Post-operative status
– Subdural collections over right cerebral & left frontal convexities & right cerebellar convexity. There are likely to represents sequelae to trauma.
– Areas of gliosis in bilateral thalami.
– Haemorrhagic contusions in left parietal & bilateral frontal parenchyma.
– Haemosiderin staining over bilateral cerebral & cerebellar convexities.
– Diffuse axonal injuries in corpus callosum.
– Mild dilatation of the lateral ventricles.
– Subacute ischemic change in bilateral frontal & parirto- occipital parenchyma.
Possibility of global ischemic insult is likely.
Now on Monday the 23rd June the Doctor has done tapping & has removed approx 100 ml of liquid & again today i.e. 25th June tapping has been done & they have removed 2-3 cc liquid & Doctor had said that again on coming saturday they will do tapping.
Request you to kindly advise as what should be our next step.
Thanks & Regards,
Aatish
Hi Aatish,
Thank you for clarifying your query and sending all the details through.
I am also very sorry to hear what your father, you and your family are currently going through, as you would be experiencing one of the biggest challenges in your lifetime!
And we are here to help. We can’t cure your father and we can guide you in the right direction about what the next steps for you and your family might be so that you and your Family have PEACE OF MIND, control, power and influence.
There are a number of things that you need to consider in your father’s case.
The first thing that springs to mind is that the CT/MRI reports shows
– Subdural collections over right cerebral & left frontal convexities & right cerebellar convexity. There are likely to represents sequelae to trauma.
– – Subacute ischemic change in bilateral frontal & parirto- occipital parenchyma.
– Possibility of global ischemic insult is likely.
You also mention a midline shift of 6 mm. I can also see that his initial diagnosis was set out as an “acute on chronic SDH(Subdural Haematoma)”, suggesting that a bleed had been there prior to your father being admitted to hospital.
The CT/MRI reports don’t show glowing results in light of the fact that “subacute ischemic change” and the possibility of “global ischemic insult” is likely to cause your father not “waking up”.
Again, in combination with a midline shift of 6 mm it’s not a good position to start off with.
However, it’s not quite clear to me why the midline shift hasn’t resolved as yet, as midline shifts can either disappear completely or at least move in the right direction after the initial problems of having high intracranial pressures have been resolved.
The biggest challenge however why your father hasn’t woken up is that the initial SDH(Subdural Haematoma) has most likely caused the “global ischemic insult”. Such an ischemic insult can be irreversible.
As a rule of thumb, the brain can only go for 3 minutes without oxygen supply, therefore any time > 3 minutes without oxygen can cause irreversible brain damage.
Check out this article for further clarification
Even though the Neurosurgeons removed the blood clots, the time for your father’s brain without oxygen may have been more than 3 minutes, therefore the irreversible brain damage could be a real possibility.
Those are the facts and the clinical realities as they stand right now and those are the facts and clinical realities as they are documented on paper.
I will address the other clinical issues such as kidney failure, infections, loose stools etc… later.
The fact and the truth of the matter is that on the one hand you are dealing with your father not “waking up” and not showing any signs of improvement as far as his neurological condition goes.
And once again, the CT/MRI as well as his current state isn’t suggesting that anything is going to change anytime soon.
However, despite the clinical results and the current clinical realities, my experience in more than 15 years Intensive Care nursing in three different countries have shown me that head/brain injuries and/or strokes take time to “wake up” and it’s not linear and “waking up” is not an event and it’s a process.
Whether your father will “wake up” or not I can’t tell, however given that after one month he is still in Intensive Care and given that you haven’t mentioned that neither the Intensive Care team nor the neurosurgical team want to give up, there must be hope.
I also want to quickly advise on the recent case of Michael Schuhmacher(the famous formula one world champion) who had been in Intensive Care for basically six months after a severe and traumatic head injury and only now went on to rehabilitation, so they haven’t given up hope on him either.
On the other hand, you and your Family need to think about and then decide what you want for your father, how much longer you want to wait and you also want to think through some scenarios for the future, such as what if he isn’t waking up, what if he is deteriorating further or what if he’s only slightly improving.
You also should ask yourself how your father has dealt with health challenges, setbacks and adversity in the past? Do you and your Family think that he will make a recovery? Do you and your family think that he has a real chance of recovery?
Answer those questions for yourself, don’t worry too much about what’s written on paper and what the Intensive Care team says, you probably know the answer already.
Many Families of critically ill Patients in Intensive Care often get too caught up in “experts” opinions such as the Intensive Care team and they often forget or neglect one of their deepest sources of wisdom which is their gut feeling and the knowledge they have about their loved one.
Do just that and you will have PEACE OF MIND, control, power and influence. If you don’t listen to yourself and if you are putting too much weight on what the Intensive Care team says you will have no PEACE OF MIND, control, power and influence.
As far as other issues go, such as the continuous fever, lack of urine output, lose motions, complete body swelling due to non body movement etc… those are the unfortunate side effects of being in Intensive Care for prolonged periods. I would assume your father is being fed either via a PEG or a Nasogastric tube and often loose motions are a side effect.
Body swelling can be a side effect of the kidney failure and the non- movement.
You and your Family need to think about and then decide what you want for your father.
Recommended resources:
Also, it’s very important that your father is getting stimulated and it’s very important that your father is getting good nursing care such as
– Having regular washes and showers
– Getting out of bed regularly in a chair(there is no reason why he can’t get out of bed)
– Having some natural daylight and fresh air
– Having his favourite music play
– Getting good and regular mouth care
– Playing his favourite music
– Having regular and experienced nursing staff looking after him
And whatever else you think is good for your father!
Also, have you thought about home care as a possibility for your father? If he’s not “waking up”, taking your father home, with specialised services might be a good opportunity. There are specialised Intensive Home Care services in India, check out http://healthcareathomeindia.com/. If you are reading this and your loved one is in a similar situation in Australia you might want to consider home care as well, check out INTENSIVECAREATHOME.COM.AU
Moreover, check out these two articles about kidney failure and kidney dialysis here
Also, I had a lady from Ireland enquire about her father recently in an almost similar case and I urge you to check out the answer I gave to her question here, as you will get answers and insights there as well. I even recorded an interview with her.
Here are the links to her question and the interview.
I really hope that helps Aatish.
Please let me know if you have any other questions!
Thank you& Kind Regards
Patrik Hutzel
How can you have PEACE OF MIND, control, power and influence whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 “killer” tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Thank you for tuning into this week’s episode of YOUR QUESTIONS ANSWERED and I’ll see you again in another update next week!
Make sure you also check out our BLOG section for more tips and strategies or send me an email to [email protected] with your questions!
Also check out our Products section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 consulting!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
Related Articles
- What is an induced coma and why is my critically ill loved one in an induced coma
- How long can a breathing tube or an endotracheal tube can stay in
- The 10 COMMANDMENTS for PEACE OF MIND, control, power and influence if your loved one is critically ill in Intensive Care
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take
- My 25 year old wife has been in ICU for one month with Tracheostomy and is still in an induced coma
- The questions you need to ask the most senior doctor in Intensive Care, if your loved one is critically ill in Intensive Care