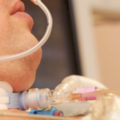
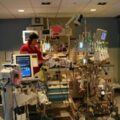
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can I Prevent the ICU Team from Withdrawing Life Support for My Mom?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Julia, as part of my 1:1 consulting and advocacy. Julia’s mother is critically ill in ICU and she is asking why is it important to get access to her mom’s medical records.
Why Is it Important to Get Access to My Mom’s Medical Records in ICU?

Julia: Yep. Call the bed manager, see if there’s a bed available. They can’t refuse a patient, can they?
Patrik: Look, they can refuse a patient as long as you either have private health insurance or you’re happy to pay for it, assuming they have a bed.
Julia: Yeah. Otherwise, you would have to call another company.
Patrik: Otherwise, you would have to go to another private hospital.
Julia: Yeah. Is there any other hospital you can recommend?
Patrik: Yes, most ICU doctors may have worked together in the same hospital for specialization or residency.
Julia: Yeah.
Patrik: But still, there’s a different dynamic as to where they practice now.
Julia: Okay. I’ll do that, but would I mention that to the letter to the CEO or that’s something I’ll get the lawyer to …
Patrik: I would keep it with the CEO. I would keep it strictly very short, and I would keep it to what I believe is a big injustice.
Julia: Yeah. And then let the lawyers handle.
Patrik: Let the lawyers handle the rest.
Julia: Would I say things in the letter like, “We will get the media involved?”
Patrik: Not yet. Most of the time, the hospitals will seek an agreement. What they do is they’re trying to push you. They’re trying to see whether they can get away with it. If they can get away with it, that’s it. The media, probably not yet.
Julia: Yeah. With the medical records, who would I direct that to?
Patrik: I would direct it to the CEO.
Julia: Oh, so I’ll put it all in one email?
Patrik: Yes, Put it all in one email.
Julia: Yeah. Okay. Look, just want to say it’s been great speaking to you. We’ll have plenty of scotches and Coke, and pizza one day. I really appreciate everything you’re doing. So, what else should I be asking?
RECOMMENDED:
Patrik: You see, one thing that I would recommend you do is ask them, “Why are you so in a rush to end my mom’s life? What’s the hurry in this?”
Julia: What he says is he thinks any other future treatment is futile.
Patrik: Okay. Turn that around and say that’s his perception. The words you use going forward matter greatly. What you can say with regards to that is, you can say, that is your perception. I don’t think that my mom’s further treatment is futile. We think that she will wake up. So, start talking about perceptions. Take the heat out of what he says it’s futile. Well, that’s your perception, that’s not my perception.
Julia: Yeah. Okay. I’ll email the CEO about the policies and that we need all medical records by tomorrow. Yeah. This doctor will ring me tomorrow and ask the neurologist. I’ll just say, “Look, I need more time, because you only gave me a day and a half.”
Patrik: Absolutely. If you feel like he’s too pushy, I would push back and I would start using stronger language.
Julia: So, I will tell him to put everything, what he says, into writing or no?
Patrik: Look, I think putting it in writing will be important, because he could deny a phone call potentially, unless you have a witness there. Unless you call him and you have another family member or myself there.
Julia: Do you represent people for family meetings?
Patrik: Oh, absolutely.
Julia: So, you would come to the hospital?
Patrik: I can come into the hospital. I can be there. We can also talk to them via the phone.
Julia: Oh, thank you so much. If he speaks to me, he’ll say, “Have the attending neurologist.” I’ll say, “No, I need more time.” If he says, “Well, we need to make this decision quickly.” I’ll say, “Well look, can you put that in writing?” Should I say that? “Can you put that in writing for me?” Or just leave that?
Suggested Links:
Patrik: I would leave it. If I was you, I would push it back to him and I would really challenge him on the euthanasia part and on the murder part. I would really start doing that, and I would also push him on hospital policies, state law, and your lawyer should know all about that.
Julia: Okay. Even when I speak to, obviously, the CEO that I’ll remind him about the euthanasia?
Patrik: I would absolutely do that. Because the problem in hospitals is they don’t see anything wrong with that.
Julia: Yeah. The families would rather accept it because they don’t know the difference. All right. Okay, so we do that.
Patrik: And look, as I said, I’m not a lawyer, but your lawyer will tell you that you need to document everything.
Julia: But then as long as we’ve got on the front foot an email, and if we don’t get no response, then obviously that shows, “Well, hang on a minute, there’s something going on.” That will put pressure on him.
Patrik: Absolutely. Generally speaking, a hospital does not want you to bring in a lawyer. Often it is enough for you to say, “Hey look, if this doesn’t get resolved, I will seek legal advice.” That’s often enough for them to start talking and sort of open the door for a different resolution.
Julia: Yeah.
Patrik: Now, can you say that any discussion you, or your mom, or your sibling would have had with your mom in the past that if a situation like this arises that she would want to have everything done?
Julia: And we’ve had two family meetings and we’ve been so strong in saying that. The nurse manager was in there, the head nurse, and the social worker was in there. They’re all in there witnessing and they know how strong we were. We said, “We’ll try everything.” She said she’s a happy, relaxed person and she’s taught us to be positive and she wants everything. We’re really clear with that. We’ve got photos on her things. We’ve brought in note pads to play great music. We’ve done above and beyond to … They know we’ve got photos on the wall, and we’ve been very clear with everyone that she’s not someone that gives up, and she would be disappointed in us if she didn’t do everything in her power. We had meeting and there’s five people. They’re fully aware.
Patrik: Okay, good.
Julia: Obviously, the nurse manager of the nurses, social workers, they’ve been very supportive and great.
Patrik: It’s the doctors driving it.
Julia: Yeah.
Patrik: Did they acknowledge that this would be your mom’s wishes?
Julia: Yeah, they did. They said, “No, that’s fine. We understand.” Look, I must admit they’ve done all the tests. They’ve told us, they’ve rang us up on a regular basis in informing. The problem has been that we have seen different doctors speak to us in five weeks.
Patrik: Right.
Julia: And one doctor sometimes said, “You should get a tracheostomy for your mom.” That’s all we want to do so far. We’ll do it straight away.”
Patrik: Exactly.
Julia: Then another doctor a few days later said, “No, we shouldn’t do it.” And he said seven different doctors will tell you different stories. And I feel like saying, “Well, okay, if you’re telling me seven different doctors are telling different stories, then why should one person decide on my mom?”
Patrik: If I was you, I would put that in the email tomorrow that you want the tracheostomy as well. I would put that in my note.
Julia: You want the tracheostomy in play?
Patrik:eah. I would put that in the email. So, they know you’ve done your research. They know you have done your research for options to prolong your mom’s life.
Julia: Should I also say that “Look, we’re informed by my mom’s doctor that tracheostomy would be done?”
Patrik: Absolutely.
Julia: Nothing was done over that weekend, but now this Monday, the family were told it wouldn’t be done. We’re a bit confused by the mixed messaging. We’ve had more than 10 different doctors, but should I include all that?
Patrik: Absolutely.
Julia: And this is all addressed to the CEO? Should we mention doctor’s name?
Recommended:
Patrik: Yep. Absolutely.
Julia: Now, there was a doctor that told us a week ago. She said, “Look, I worked in the UK and people were waking up two, three, four weeks months later. I wouldn’t be worried about your mom waking up.” I don’t want to get in trouble, but should I just mention that your own doctors told us that they’ve seen patients wake up several weeks later?
Patrik: I think you should. If I was to go in a meeting with you, I would say that very same thing.
Julia: Yeah.
Patrik: I think you should.
Julia: Yeah, but I’ll say, “Look, we’ve spoken to over 10 doctors there over the last five weeks.” I don’t know all their names I’ll say, but I do know most of their names. Yeah. All right. You said do the letter. You said you can help me draft the letter. Is it something I should do tonight?
Patrik: Look, I think the sooner you can get the ball rolling, the better. I do believe that when the CEO starts his day tomorrow, I do believe that email needs to sit in his inbox or as quickly as possible. And you don’t need to write a novel. You just need to keep it to the point. I think the gravity of the situation is okay. You need to bring your point across with short sentences, so they know, “Hang on a second, there’s something seriously wrong here.”
Julia: o, I coud say this could be considered as murder or euthanasia.
Patrik: would use those words. I really would, because they are not words people use lightly, of course. But I do believe they understand that you mean business and that your perception is very different compared to their perception. I have found that unfortunately those words can be very powerful.
Julia: Yeah.
Patrik: cause then you don’t need to tell them that you might go to the media. It’s already implying that.
Julia: Yeah. Policies of withdrawal of treatment. The doctors about the tracheotomy, the different doctors we’ve spoken to, and also those strong words.
Patrik: Yeah. Here is another thing that I quickly want to need to spend a couple of minutes on that. You might have seen that in my emails. I’ve talked about DNR policy. Now, let’s just quickly talk about that because that could really be something that could work in your favor.
DNR stands for do not resuscitate. Another term for it is NFR, which stands for not for resuscitation. What that means is some patients in hospital, especially in ICU, might be NFR, not for resuscitation, or DNR, do not resuscitate. What that means is if your mom’s heart was to stop and she’s a DNR, they wouldn’t resuscitate her. Now, why do I bring this up? Now that they’ve decided they want to stop life support, most likely they would have signed a DNR form without you knowing.
Julia: Yes.
Patrik: I’m almost 100% certain that this is what’s happened, which is why it’s so important for you to get access to the medical records because you will find it in the medical records. Now, if they have signed a DNR form or documented somewhere that she’s a DNR, they are breaching another policy, which they can make that decision for DNR, but the bare minimum they have to do is they have to inform you. By the sounds of things, they haven’t informed you, have they?
Julia: Well, no. They’ve been very strong to say that we want resuscitation at any stage.
Patrik: nce they’ve given you access to the medical records, you will see all of that, right?
Julia: Is it something I’ll send through to you?
Patrik: Yes. Ideally yes. We can look at the medical records.
Julia: Look, I’ll go for another extended time because I think I will need you.
Patrik: Look, I tell you what I expect once you’ve started talking about medical records. I expect them to try and delay. I expect them to say, “Oh, you can’t have access to the medical records, because it’s too difficult. We have to talk to blah-blah-blah.” That’s what I expect.
Julia: What would I respond to that if they said that?
RECOMMENDED:
Patrik: I tell you how you respond to that. The Medical Health Records Act is clearly saying that you have a right to have access to medical records. You can just paste that link in your email. If she comes back and says, “Well, I can’t give you access to the medical records because of rah-rah-rah.” Well, you go back …
Julia: What if she says, “Oh, I’ll give it to you soon.”
Patrik: Look, if she comes back with something, if she comes back to you and says, “Hey, I can’t do it today, but I’ll make sure it’s ready tomorrow, I think that’s okay.”
Julia: Yeah. But they’ve got to give it time to view those.
Patrik: Not necessarily, and I’ll tell you why. Most of it would be online now. In this day and age, they should just send you a link to a website with a username and a password, and you should have access to the medical records.
Julia: I guess what I’m trying to say is if we ask for the … Yeah, okay, that’s fine.
Patrik: I don’t know what they’re doing there at the moment. Whether they have everything online or whether they still do paper based, I really don’t know. But most ICUs now, it’s all paperless. It’s all in the cloud. They should just send you a link to a website with the username and a password and it’s all there.
Julia: Okay.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!