Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question last week from my client Graham was
My grandmother is in an induced coma after cardiac arrest! Is she brain dead?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the questions from one my clients RACHEL as part of my 1:1 consulting and advocacy service!
RACHEL has her husband transferred in the Intensive Care after cardiac surgery. Her husband eventually had a cardiac arrest and is not waking up.
My Husband’s alcohol withdrawal and sedation is keeping him unconscious in ICU. Why is he not waking up?
Patrik: … because that, it’s really significant. Do you know what I mean when I say cardiac arrest? Do you understand what I mean by that?
Rachel: No. I asked did he go in cardiac arrest. They said no.
Patrik: Okay, but then you’ve got to ask them why they shocked him. You really got to find out why they shocked him. That’s a make or break question. From my perspective, there is no reason why they would have to do a CT of the brain if he didn’t have a cardiac arrest. There’s no reason unless you mentioned stroke. From what you’ve said so far, there is no indication that there was a stroke. Or is there?
Rachel: Well, they said that, I guess, with the scan that they did, it’s kind of superficial. It doesn’t really give a snapshot of the brain. It just tells you some surface … answered surface questions.
Patrik: Yeah. But why did they do a CT scan in the first place? Is that because he wasn’t waking up? There must have been a reason why they’ve done a CT of his brain.
Rachel: He’s not waking up. The first day after the surgery, he did make communication and said that he loved me and he needed a drink. He didn’t speak it, but he moved his mouth and he squeezed my hand and I had him flutter his eyes if he can hear me. Then, I guess, the next day, because they have him on propofol, they have him libium, did I say that right, lyrium? Let me see.
Patrik: Valium, Valium.
Rachel: I guess it’s not Valium, but it’s … Hold on.
Patrik: Midazolam or Versed?
Rachel: Librium. It’s called Librium.
Patrik: Diprivan.
Rachel: The particular drug they have him on is called Librium.
Patrik: Liquidem?
Rachel: It’s what the doctor said, Librium, L-I-B-R-I-U-M.
Patrik: Yes, it’s similar to Valium but not quite Valium.
Rachel: Because they’re trying say is that he’s going through alcohol withdrawal.
Related article:
Patrik: Okay. I understand. If he’s withdrawing from alcohol he needs to have some form of benzodiazepine and Librium is one of them.
Rachel: Because they didn’t tell me that they’ve had him on medication for the alcohol withdrawal the past few days and now they say that today is the first day that he’s been off of the Librium. Librium is for alcohol withdrawal. But they asked me several times about his drinking and I don’t know if that has a major influence on him and his conscious state because all of the vitals are clear and they’re good, but his neuro isn’t positive in the sense of when I came in the room earlier yesterday I talked with the nurse about lowering the propofol because it’s day eight, and he’s not moving. I mean, he can move his arms and move his legs, but the doctor said that he’s not following commands.
Glascow Coma Scale:
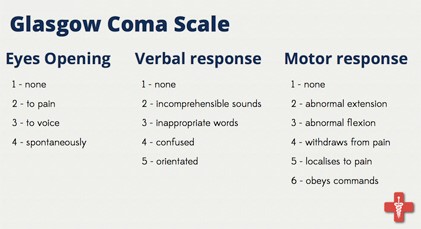
Patrik: Yeah, I understand. I’m following. I do have a few other questions. The surgery was on the 18th. Is that what you said?
Rachel: Pardon me, Sir?
Patrik: The-
Rachel: Oh, the 18th. Yes. The 18th.
Patrik: 18th. Okay. How old is your husband?
Rachel: 69.
Patrik: 69. Okay. Here are a few things that you need to know. After cardiac surgery if all goes well, patients should be out of the induced coma within 48 hours. Okay? Yes, if somebody is withdrawing from alcohol, yes, that could certainly delay waking up. Besides that, not coming out of an induced coma for over a week, there must be other issues, other clinical issues, that you may or may not be aware of.
What I’m saying is there must have been some other things going on clinically, and I’ll name a few so you just … Maybe you’ve heard of them. One could be bleeding. One could be an irregular heart rhythm. You’ve already mentioned the pacemaker. Right?
Recommended and more information about induced coma:
Rachel: Okay, that’s what happened when they shocked him. He was having irregular heart palpitations.
Patrik: Okay. That makes sense. How long has he had the pacemaker for? When did he have the pacemaker?
Rachel: If he had the surgery on the 18th, they waited around four days before implanting it. Oh, last Friday, so on the 22nd he had the pacemaker surgery.
Patrik: Okay. The shocking, was that before or after the pacemaker? Probably before.
Rachel: After. No, it was after.
Patrik: Right.
Rachel: The shocking was on the 24th, Christmas Eve.
Patrik: Okay. When he had the pacemaker, did he go into the operating room for that or did he have that in the unit, in the ICU?
Rachel: No, he went to the operating room.
Recommended:
Patrik: Okay. So it’s a permanent pacemaker?
Rachel: Yes.
Patrik: Okay. If they shocked him after that, that means the pacemaker wasn’t working to begin with. Okay. Yeah, it wasn’t. It wasn’t.
Recommended:
Rachel: But it almost makes me nervous in the sense of why did they shock him because I think they did it because they were scared. I don’t think they shocked him because when I heard them talk with the doctor they seemed a little unsure.
Patrik: I can tell you-
Rachel: Then when they started talking to the doctors, then I heard about they were suctioning him because at first it just made it seem like he just all of a sudden, they had to run in the room because of the cardiac… I mean, because his levels of the heart rhythm were off the beat and the blood pressure was high.
Patrik: Yeah. I can tell you-
Rachel: But when the doctor-
Patrik: It makes me very nervous.
Rachel: When the doctor … When they talked to the doctor, the doctor brushed it off like it was maybe complications from the pacemaker.
Recommended:
Patrik: Look, I can tell you that if they shocked him after he had the pacemaker it makes me very nervous, and I do believe they’re not telling you the full story there. I really do believe that they’re not telling you the full story there. Going back to the beginning, to sort of put this in perspective for you, so there have been complications, and complications mean he was probably in an irregular heart rhythm, which is why they probably put the pacemaker in while they shocked him. That’s one of the issues.
I can’t talk about the alcohol withdrawal. I mean, even though he may only drink three times a week he may still go through alcohol withdrawal. You know? People are very different. I wouldn’t rule that out even though you might think three times a week is not a lot. He may still feel like he needs a drink. Right? You couldn’t rule that out either.
Going forward, if I was you the first thing that I would want to find out if I was you is why did they shock him. You haven’t got a clear answer on that. If I was you, I would seek a very clear answer to that question because he could have had … Especially if he had a CT scan followed up after he had the shock. I would not rule out that he had a cardiac arrest, and they haven’t told you. You may have asked them, and they may have denied it. That doesn’t mean he didn’t have a cardiac arrest. They may just brush it off, and they don’t want to tell you.
Rachel: Okay.
Patrik: I would seek very clear answers to that question. If you think they are hiding something, just ask for the medical records. Are you the medical power of attorney for your husband?
Rachel: Yes.
Recommended:
Patrik: Okay, that’s good. That’s good. Does he still have his drains in his chest? After cardiac surgery patients come back with chest drains. Does he still have-
Rachel: He still has the drains. It is still draining blood, not blood, but you know, now sort of like an orange in colour.
Patrik: Yeah. Does he only have one drain or two drains or three drains? Do you know?
Rachel: He has the one drain and then he has Foley catheter.
Patrik: Okay. What’s your biggest concern at the moment? Your biggest concern at the moment is that he’s not waking up. Is that correct?
Rachel: The thing about it is he’s waking up in the sense when they’re suctioning him he’s making faces, and you can see that he’s agitated. Then last night they’ve been taking him on vacations from the propofol. The vacations are kind of where they’re seeing if he’s able to respond in time because they’re saying when they’re off of their propofol they should respond within 15 minutes.
Patrik: Yeah, that’s correct.
Rachel: I did not know until today that they had him on some withdrawal program.
Patrik: Yeah, yeah.
Rachel: It was the Librium. When I read about Librium, it said in elderly patients, you know, they get 5 mg a day two to four times, and she said that he’s had that for like three days unbeknownst to me. When I looked up that drug it said that you could have … You know, you could be sedated, you can have confusion, all these other things. When I walked into the room earlier his eyes just barely opened, but it was just like he’s not doing anything other than when you touch him he is moving his neck.
Patrik: Yeah. That’s all relevant what you’re sharing there. The reality is, yes, propofol is short acting. That means if you switch it off, patients should wake up within 15 minutes. At the same time the Librium, for example, is more like a long-term drug, and it takes longer to get out of the system, and it takes longer for patients to wake up.
Here’s another thing that’s important for you to know. Let me just finish that thought so you understand why it’s important. When your husband came out of surgery for the first few days he would have been on strong painkillers like morphine, Fentanyl, oxycodone or something like that, and he’s probably still on some of them. Those pain medications like morphine, Fentanyl, or oxycodone would make him very sleepy as well, and it would stop him from waking up quickly as well.
There is a very good chance your husband is still on morphine or Fentanyl especially if he has the chest drain in situ, especially if he has the chest drain in place still. Those pain killers will make him very sleepy as well.
Now, here’s another thing that is very important to know. Waking up after an induced coma is like switching on a light with a dimmer. Okay? I’ll repeat that because it’s very important. Waking up after an induced coma is like switching on a light with a dimmer, not like with a switch. Does that make sense?
Rachel: I see what you’re saying. So you’re saying if it happens out of the blue or it happens gradually or it should happen instantly.
Patrik: Very gradually. Very gradually. Sometimes over days and sometimes over weeks. What you are describing there is very … It’s very abnormal from your perspective. Now, what you’re describing to me having worked in intensive care for 20 years you’re describing something that I’ve seen hundreds and thousands of times. Okay? For you, this is all very unnatural whereas what you are describing to me I’ve seen hundreds or thousands of times. You’re describing a “normal process” in intensive care.
What you need now is you need to find out why did they shock your husband. That’s really important to find out. I would really dig very deep there. You need to find the answer to that question. The next thing that you need is being really patient so that he can come out of the induced coma. We have a number of articles on our website how people come out of an induced coma, how long it takes, what to look for, all of that.
What I would like to do in the next step … Is this the first time you’ve come across our website?
Recommended and information about Induced Coma:
Rachel: Yes.
Patrik: Okay. There’s a number of things to move forward. Number one, I would really encourage you to subscribe to our free email newsletter, and I can do that in a moment. I’ll just grab your email. In our free emails newsletter, we answer all of those questions, how long does it take to wake up after an induced coma, but I will send you specific information around that. Right?
Rachel: I’m a little curious about alcohol withdrawal mixed with the procedure. You know?
Patrik: Bad combination. It’s a bad combination, but it’s just something that will take time. Right? What you need to do at this stage is you need to wait. By that, it could be another week. It could be another two weeks. Don’t throw in the towel just because it looks awful. I know it looks awful, but as I said to you are describing something that I’ve seen hundreds if not thousands of times. Your biggest asset at the moment is waiting.
Rachel: people wake up after two weeks, and their brain is still fully functioning?
Patrik: Absolutely. It just takes times. They will be confused most of the time. Right? A recovery after such an event will take time. It’s massive surgery your husband had. It’s massive.
Rachel: Okay. I do think I want you to talk with the nurses and get like a clear snapshot of what’s going on because they told me that they shocked him because of like I said they said when they were giving him suctioning his blood pressure went up to 130 or 160.
Patrik: Keep in mind-
Rachel: His heart palpitations was the word unfortunately.
Patrik: Right. Keep in mind when you suction someone their blood pressure almost always goes up because it’s so uncomfortable. Again, what you are describing there I have seen hundreds if not thousands of times. For you, this is all new and this is terrible.
Rachel: I think for the nurses it was new too, and I think when the cardiologist came in in the morning he brushed it off like it was kind of not a big deal.
Recommended:
Patrik: Yeah, I think it is. I really think it is. I can tell you that if it was my family member and I would know that they shocked him … because I know way too much. Right?
Rachel: Right.
Patrik: If they shocked him with a pacemaker in, I have huge concerns. The worst thing that could have happened is he had a cardiac arrest and they shocked him, and it probably worked right away, which is great, or number two, the pacemaker didn’t work, and he went back into atrial fibrillation and they shocked him. One way or another that is a warning sign to me especially if they brushed it off. Well, they don’t have to brush it off if they can just explain it to you. Every time they brush you off I have huge concerns.
Rachel: Yeah. That’s kind of why I started to look around on the Internet for options because to me I know it was Christmas time, but my husband is also a physician. He’s been a doctor for 41 years. I understand that medicine is not an exact science. It’s kind of based off of what they’ve seen in the past. To me, the two doctors that are there are pretty young.
Patrik: Exactly.
Rachel: The one doctor that I had seen was trying to figure out things, and he asked me again about the drinking and was trying to figure out why he isn’t waking up. He’s the one that took him off propofol to have him take a sedation vacation. When I went in today he was back on the propofol.
Recommended:
Patrik: Right. Right. That’s good because you have to do that to see whether patients wake up or not. I like that they’re doing that, but at the same time I don’t expect any miracles after a week in a coma. It’s not like if people are in a coma for a week and you take them off sedation, it’s not like they wake up and all of a sudden they move everything. That’s why I keep saying waking up after an induced coma is like switching on a light with a dimmer. I keep coming back to that. It’s a slow process.
What I’ll do Rachel is I will send you some information around how long it takes to wake up after an induced coma, what to look for. You can have a look. If you have any questions, get back to me. I will subscribe you to our free email newsletter. As I said, just by you reading that you will get a lot of good information because families come to us with similar questions. One of those questions is why is my family member not waking up.
Rachel: That was on the website. Yeah, I listened to your video.
Patrik: Right.
Rachel: I’ll look at the email.
Patrik: I’ve got to go for now, Rachel, but you’re on the right track. Keep asking them, and dig deeper. I would definitely want to find out if I was you why they shocked him. That would be your number one question. I would ask for a very detailed answer there.
Rachel: Okay. All right, hopefully maybe you can talk to the nurses and the doctors tomorrow.
Patrik: Very happy to do that. Very happy to do that. What I’ll do is I’ll send you all the options for consulting. You can just click on the links, and you can just enter your email then and use your credit card, but I will send you all of that in a moment. You will get that in an email in the next ten minutes.
Rachel: Okay.
Patrik: Okay.
Rachel: Do you know if … Okay, yes.
Patrik: Okay, thank you so much for your call, Rachel.
Rachel: Thank you. I appreciate it.
Patrik: You’re very welcome. Take care. Bye-bye.
“Thank you very much for being a part of this episode of 1:1 consulting and advocacy sessions. We hope you will find these new upcoming episodes informative and empowering.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!