Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM , where we instantly improve the lives of Families of critically ill Patients in Intensive Care, so that you can have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from one of our readers and the question was
“Will my 19 year old son ever come off the ventilator after he aspirated during a seizure?”
You can check out the answer to that question here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I answer another one of our most FREQUENTLY ASKED QUESTIONS and in this week I answer
”HOW LONG DOES IT TAKE TO WAKE UP AFTER BEING VENTILATED?”
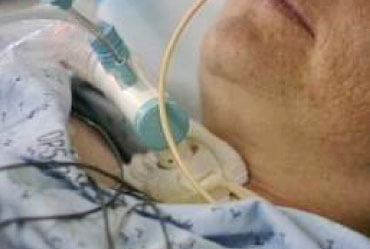
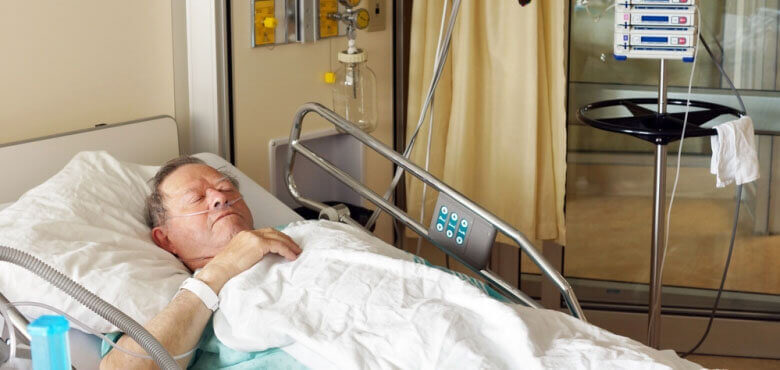
Mechanical ventilation and the breathing tube are big unknowns for Families of critically ill Patients. It often comes as a shock for Families of critically ill Patients in Intensive Care to see their loved one with a breathing tube attached to a ventilator.
It can be quite scary for you and here’s what you need to know
It can be quite scary because you haven’t seen your loved one with all those tubes attached before and maybe you didn’t expect to see your loved one critically ill in Intensive Care. Maybe your critically ill loved one was healthy just a few hours or days before coming to Intensive Care. So, in essence it can be a bit of a shock to find that your loved one is ventilated with a breathing tube in Intensive Care for critical illness.
But the big question remains, ”HOW LONG DOES IT TAKE TO WAKE UP AFTER BEING VENTILATED?”
The answer to that question is that it depends. It depends on the length of time your critically ill loved one is ventilated for and it depends on how long your loved one is in a medically induced coma for.
Mechanical ventilation, the breathing tube and the induced coma always go hand in hand
Mechanical ventilation, the breathing tube and the medically induced coma always go hand in hand. They always go together, because a breathing tube and mechanical ventilation cannot be tolerated without a medically induced coma. It’s too uncomfortable without putting your loved one to sleep.
Imagine somebody is inserting a breathing tube through your mouth into your throat and then starts to put air and oxygen into your lungs with high pressure, that’s going to be very uncomfortable right?
Therefore, the medically induced coma is absolutely necessary for your critically ill loved one to be able to tolerate the ventilation and the breathing tube.
Even after the decision has been made to take your critically ill loved one out of the induced coma and even after the sedative and opiate drugs have been weaned off to “wake” your loved one, the length of time to come out of the medically induced coma and to “wake up” can still vary.
“Waking up” sometimes takes longer than you think
The length of time for your loved one to “wake up” is dependent on a number of things such as
- The length of time ventilated and in an induced coma
- The amount of sedative drugs and opiate drugs(pain killers) used for the medically induced coma
- The nature of the sedative drugs and the opiate drugs(pain killers) used for the medically induced coma
- Other medical issues such as a stroke, seizures or head or brain injuries that often delay “waking up”. Those injuries generally speaking don’t make “waking up” linear or straight forward
- “waking up” is more of a process and not an event
- Your critically ill loved one’s age. Generally speaking the older your loved one is, there can be a delay in “waking up”
- Other medical issues such as kidney or liver failure. If the kidneys or the liver are not working properly, sedative drugs and opiate drugs can stay in the body system longer, as they can’t be metabolised and/or excreted by those organs and therefore stay around longer in the body and delay “waking up”
- The other issue some critically ill Patients encounter when coming out of the induced coma is that they can be confused, agitated and/or non- cooperative at times due to disorientation
Related articles
- After weaning off a ventilator is it normal to be confused?
- The 5 things you need to know if your loved one is confused, agitated and delirious in Intensive Care
Length of time of ventilation and the nature of drugs given are a major factor
Other issues that need to be considered are what type of sedative drugs are given, whether they’d be short- acting or long- acting and obviously the length of time your critically ill loved one has been ventilated for and how long they have been in a medically induced coma for.
The length of time for mechanical ventilation and induced coma can generally be divided in three categories or time frames. The three categories are
1) Short term ventilation for up to 72 hours
2) Medium term ventilation lasting from 72 hours up to 7 days
3) Long(er) term ventilation> 7 days
Short acting vs long acting sedation
Short acting sedatives are sedatives such as Propofol(Diprivan) and normally, what happens is that as soon as Propofol is switched off a critically ill Patient should wake up immediately and if they have shown to breathe by themselves and if they can follow simple instructions such as squeezing fingers, they can be taken off the ventilator or extubated(=removal of the breathing tube).
Long acting sedatives such as Midazolam(Dormicum or Hypnovel) are generally used if sedation and the induced coma is required for more than 72 hours. Midazolam is also a Benzodiazepine and can make critically ill Patients addicted to it and they can experience withdrawal symptoms when being “woken up” or when being weaned off the ventilator.
The same applies for opiate drugs(pain killers) given during the medically induced coma, they can be addictive, as usually Fentanyl and/or Morphine are used as drugs of choice and the longer those drugs are used, the higher the risk that your critically ill loved one is experiencing a withdrawal from those drugs and make “waking up” more difficult.
Withdrawal symptoms such as hallucinations and agitation are also sometimes contributing to a delay in “waking up”.
Also “waking up” is more of a process and not an event. “Waking up” and coming out of an induced coma can be compared to switching on a light with a dimmer, rather than with a switch. It’s slow and delayed.
Other time frames that you and your Family need to be aware of when your loved one is on a ventilator are
- If your loved one is ventilated for up to 3 days or 72 hours, waking should be relatively quick and uneventful if there are no other issues such as head or brain injuries, stroke and or seizures
- If your loved one is ventilated for more than 72 hours for up to 7 days, you can expect a bigger delay in “waking up” as generally speaking the longer sedation and opiates are being used, the more those drugs have accumulated in the body system and those drugs generally speaking make your critically ill loved one more drowsy
- If your loved one is ventilated for more than 7 days, then you and your Family can expect an even bigger delay in your loved one “waking up”. Again, as a rule of thumb, the longer sedation and opiates are being used for a medically induced coma, the longer the delay in “waking up”
- Furthermore, if your loved one requires a medically induced coma for critical illness for more than 7 days, keep in mind that they are critically ill after all. Whilst mechanical ventilation, the breathing tube and a medically induced coma should not be applied for longer than necessary, a longer recovery time may sometimes be necessary just simply because of the nature of the illness or injuries your critically ill loved one is suffering from
Your job is to be patient, to support your critically ill loved one and to ask the Intensive Care team the right questions. Your job is also to have PEACE OF MIND, power, control and influence whilst your loved one is critically ill in Intensive Care, especially if your loved one is in a very difficult situation such as
- very unstable and in a very critical condition
- in a life threatening situation
Then it’s even more important to have PEACE OF MIND, control, power and influence. After all you, your Family and your critically ill loved one don’t want to be at the mercy of the Intensive Care team.
How can you have PEACE OF MIND, control, power and influence whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below! In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE reports you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 “killer” tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial “behind the scenes” insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Thank you for tuning into this week’s episode of “YOUR QUESTIONS ANSWRED” and I’ll see you again in another update next week!
Make sure you also check out our ”blog” section where we answer your questions or send me an email to [email protected] with your questions!
Also check out our Products section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 consulting!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
Sincerely, your Friend
Patrik Hutzel