Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question last week was
You can check out last week’s episode by clicking on the link here
Other parts of this series of questions you can look up her PART 2, PART 3, PART 4, PART 5 and PART 6
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another the next question from one of our clients which are excerpts from email counselling and consulting sessions with me and the question this week is
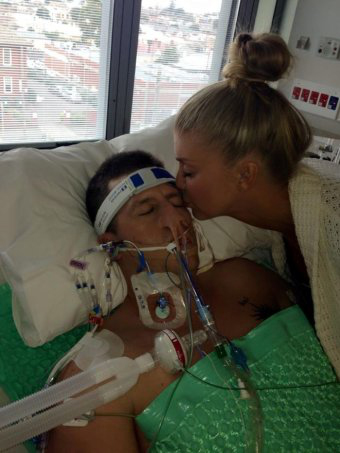
My husband had open heart surgery with complications! He’s not “waking up”, he needs 100% of oxygen and now he’s bleeding from the stomach, I’m so scared, help! (PART 2)
This was another great series of questions where I was able to “hand-hold” a very anxious and distressed client through a very stressful and complex situation.
Katie writes
Hi Patrik,
thanks so much for your response, my husband had aortic valve surgery on Thursday and today , due to this hole in his heart (=Ventricular septal defect or VSD) he had a second surgery to repair the hole.
They did not know he had the hole until a procedure showed it and my husband didn’t tell them about it prior to the surgery.
The docs determined the hole was preventing the blood from going to the lungs to give the lungs oxygen but instead were just going from one chamber of the heart to the other so he has been on 100% of oxygen on the ventilator since Thursday.
Yes, they did give him Nitric Oxide(NO) with the ventilator before the VSD surgery. Since the surgery (completed by 4:30 this afternoon and it is now about 9:30), there has been no change …still on 100% ventilator, though we were all hoping this 2nd surgery would provide more Oxygen to his lungs.
Now what? My husband is totally sedated again. Is there anything you can suggest? It means so much to get your outside thoughts and opinions.
How can I thank you for the hope you are giving us…I am so grateful for your prompt and detailed explanations…I am so very afraid and am trying to be strong and stay positive.
He is also bleeding what looks to be “old” blood from his stomach…they could give no explanation for that. His blood count is low but not enough to give him blood. Any ideas about that? The surgery itself seems not to be causing any bleeding problems.
I am sorry to be asking so many questions. I have read about intra-abdominal haemorrhage and there is a correlation with open heart surgery where the spleen and liver can bleed. They say it is OLD blood…darker in color. I am so upset…and it is not good. I am so scared …please help me respond to his care givers…they just say it is common. I don’t think so, please respond.
Many thanks!
Katie
Recommended:
Hi Katie,
there is definitely a correlation between any type of surgery, as well as ICU admissions in general and stomach bleeding, also called GI bleed/ Gastrointestinal bleed, but I wouldn’t say it’s common.
It’s something to be mindful of and it’s something that needs to prevented in the first place.
It’s often a stress response. The stress of being critically ill causes the stomach to produce more acid, this may have also already happened leading up to surgery with your husband feeling uneasy about going for surgery. More acid in the stomach can cause bleeding because the PH is trending more towards the acidosis side and it basically erodes the stomach cells causing a bleed.
This has been well documented over the years in Intensive Care. The risk for stomach ulcers and sub- consequent bleeding in Intensive Care Patients is huge because of the reasons I mentioned above.
Normally in order to prevent bleeding to occur, Patients in an induced coma and on a ventilator should be receiving Nasogastric tube feeds as early as possible to maintain a healthy and physiological stomach and PH environment.
Other preventative measures include giving Pantoprazole (Somac), Esomeprazole (Nexium) or Ranitidine (Zantac). Those drugs all reduce the acid production in the stomach and are almost always standard ICU treatment, as the stomach ulcers are a well-known and well documented side effect of ICU admissions with often dramatic consequences. That’s why it’s so important to try and prevent those ulcers and GI bleeds in the first place.
Common treatment for GI bleed includes giving units of donor blood, Fresh frozen plasma and/or Platelets. Also, if stomach/ GI bleed is ongoing, a Pantoprazole infusion should be commenced as well as Nasogastric tube feeding should be continued as early as possible to again, maintain a healthy, normal and physiological stomach flora and PH.
Other medical treatment includes giving Somac (Pantoprazole) intravenously, often as an infusion. Furthermore, starting to feed your husband through a Nasogastric feeding tube will reduce the risk of bleeding as well.
In some instances a Gastroscopy (=putting a video camera in the stomach) is also necessary in order to find the exact source of bleeding.
The next issues around bleeding is simply that during the AVR replacement as well as the VSD closure your husband would have been on a Bypass machine and during that time he would have been given some Heparin, which is a blood thinning medicine.
This increases the risk of bleeding significantly, however a GI(Gastrointestinal) or stomach bleed is often a result of a stress response and results in acid production in the stomach and the bleed.
Now, as far as your husband’s induced coma goes, they will need to make sure that he’s stable first and foremost before they will take him out of the induced coma.
Related article/video
The complications that I mentioned in my previous email like pulmonary hypertension, low blood pressure will most likely persist for now and the pulmonary hypertension in particular may stabilize once the Nitric Oxide (NO) can be weaned down as the pulmonary hypertension will be reduced.
Again, pulmonary hypertension is high pressures in the blood vessels that supply the lungs with oxygen. Those blood vessels are connecting the right side and the left side of the heart.
Furthermore, your husband is most likely still having a critically low blood pressure as a side effect of the bleeding as well as a side effect of being sedated and in the induced coma.
Because of this critically low blood pressure he will need another form of life support called vasopressors or Inotropes.
Vasopressors or Inotropes are intravenous drugs to increase blood pressure to a level so that life is sustainable.
Common drugs being used for vasopressors/ inotropes are Adrenaline (Epinephrine), also Noradrenaline (Norepinephrine). Also, for Patients in heart failure Dobutamine or Milrinone are being given to increase the cardiac function of the heart.
Overall, your husband remains in a critical condition, especially with having been through two major open heart surgeries within 48 hours.
On top of that he’s dealing with the bleeding from the stomach, therefore he most likely will need to stay in the induced coma until he is more stable and until they are certain that there is no more bleeding.
They will also need to wean down the oxygen to less than 50% on the ventilator, the nitric oxide (NO) as well as the vasopressors/inotropes before they can take your husband out of the induced coma.
Please also keep in mind that your husband would have had even more sedatives and pain killers in the last 48 hours than many other Patients because of the surgery, therefore it might take a while until he will be awake.
Here is another link to how long people can stay in an induced coma for
I know how frightening this experience must be for you and your family Katie, but being patient is your biggest asset in all of this.
Wait another 24 hours, keep close communication with the doctors, the nurses and myself and I can keep “hand-holding” you through this challenge.
I hope that helps.
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



