Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question in this series of questions from our client Sue and the question last week was PART 2 of
My Dad has end-stage HIV and is on ECMO in Intensive Care! Can he have a lung transplant? (PART 2)
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another question from one of my clients, Sue, which are excerpts from phone and email counselling and consulting sessions with me and the question this week is
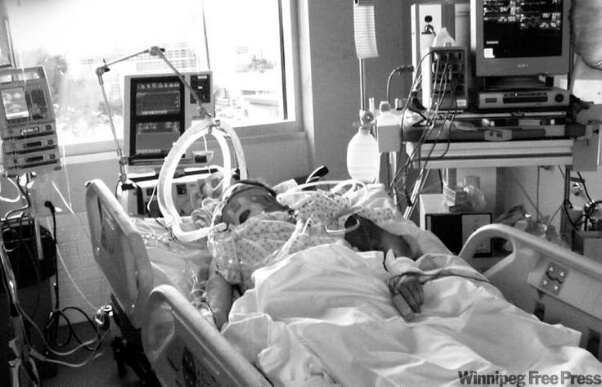
My Dad has end-stage HIV and is on ECMO in Intensive Care! Can he have a lung transplant? (PART 3)
Sue continues to describe her and her Dad’s situation as follows
Hi Patrik,
the doctors just called my family in and have advised the lung to my dad is irreversible and there’s nothing more they can do.
They said they initially thought there would be hope but his lungs are so affected by the PCP Pneumonia although it has cleared he simply cannot breathe by himself.
Is a Tracheostomy still possible in your opinion?
They said he is sleeping for longer and no not believe he is comfortable when one of the sedatives is taken off so they give it back to him.
I am still at the hospital waiting for my brother and sister to be informed of the same thing by them.
They acknowledged he has late stage HIV and that there will be an investigation into the other hospital but now they are saying next steps would be to take away treatment and ECMO once we are ready.
Can you advise if there are any alternatives or trust is this is the best for my dad?
Can you also please advise if their decision making of not putting my Dad on a lung transplant list is within line of their policy for the selection of lung transplant Patients?
May I ask you to also call xxxxxx xxxxxxx. He is an ICU consultant looking after dad.
If you can call him within the next hour that would be great. He is expecting your call.
Nurse Christine will forward you to XXXXXXX.
He asked questions if you were practising and if you were based here and I said you were previously based here and you are practicing ICU nurse.
He said he will send me the policies about withdrawal of treatment now but that they were not at liberty to get out agreement to stop treatment but they prefer agreement! They said they need us as a family to come in the next 24 hours!
Here are also some comments from the ICU consultant regarding lung transplant for my Dad
Attached is a list of inclusion criteria.
International data show that lung transplantation on patients on ECMO who were not on the transplant list prior to ECMO support is universally fatal. Couple this with your Dad’s weight and other issues, I can say with confidence that he would not be a transplant candidate.
I hope this helps and look forward to speaking to you later.
Many thanks
Sue
Recommended:
Hi Sue,
Thank you for sending through your questions and your email.
I have been talking to the ICU consultant who’s looking after your Dad, thank you for getting this organised.
I was very pleased to talk to him and have found him to be very openly answering my questions.
I didn’t feel he was trying to hide and we had a mature conversation between two health professionals.
He appreciated you and your family seeking external advise and external guidance in such a highly emotionally charged situation.
He understands and appreciates that you don’t want to rush such a “life” or “death” decision and again he feels like they are at the end of what they are able to provide in terms of treatment for your Dad.
I do believe they have done everything they could in terms of treating your Dad’s PCP Pneumonia.
The only thing that I would criticise is that they should have informed you much earlier about the possibility of
- A tracheostomy and therefore the advantages and also drawbacks of such a tracheostomy
- The potential/possibility of ECMO being used as a bridge to a lung transplant
Both, a tracheostomy as well as the listing for a lung transplant would not have been guarantees for your Dad’s survival, but could have stacked the odds in his favour and I do believe they have failed their duty of care to you and your Dad by not explaining those options to you and your Dad in the first place.
Related articles/videos:
For now, I do believe with all the information the ICU consultant has given me and with all the questions that I asked, the length of time your Dad has been on VV-ECMO with multiple failed weaning attempts, there is probably not much more they can do.
He’s still on sedation with Midazolam and he’s still on Fentanyl for pain relief. Therefore the ICU consultant assured me your Dad is not suffering and I trust in his skill and assessment there.
He’s also still on inotropes/vasopressors Noradrenaline on top of the ventilation and the breathing tube.
If VV-ECMO can’t be weaned off, your Dad will inevitable pass away as soon as they will remove ECMO support.
Your Dad from that perspective is in a “real” and not a “perceived” end of life situation.
This distinction is a rather important distinction to be made before such an important “life” or “death” decision can be made with confidence.
Related article/video
I can assure you that I would be the first person to point out and question the ICU consultant if I was under the impression that they haven’t done everything they should have done.
Again, besides not being transparent about the potential for a tracheostomy as well as the potential for a lung transplant, I do feel they have done whatever they could have done.
I’m also pleased to see that they are cooperating with you in this inevitable and also “ONCE IN A LIFETIME” end of life situation that you need to brace yourself for now!
Furthermore, I have looked at the lung transplant policy and I have looked at the relevant sections.
Please note the following.
- PCP Pneumonia is not listed as one of the factors that could lead to a listing for a lung transplant.
- It’s mainly chronic lung conditions leading to the eligibility for the listing to a lung transplant
- Patients being considered for lung transplant also need to meet the following criteria
- Be on maximal medical therapy
- Have a potential survival benefit from transplantation or a potential significant improvement in their quality of life as a result of transplantation
- Have projected post-operative survival >5 years with a quality of life acceptable to the recipient
- These are the key criteria which are required and none of these criteria is applicable in your Dad’s situation
The best outcomes you get when Patients are eligible for a lung transplant is to make a decision and selection early on in a disease process.
That’s where I believe the ICU didn’t follow their duty of care in the beginning, they didn’t transparently educate you on the possibility of a lung transplant, the pros and cons and also the pre-determining factors.
Next, in the policy it also says
“Mechanical ventilation – carefully selected candidates on mechanical ventilation/extracorporeal support without other acute or chronic organ dysfunction, who are able to actively participate in a meaningful rehabilitation program, may be successfully transplanted”
Again, this is what your Dad’s situation might have looked like in the beginning, however their concern would have been that with such a drastic weight loss from 100kg to ~69kg in recent months, your Dad might not have been able to “participate in a meaningful rehabilitation” down the line because he presented in a severely weakened condition with the significant weight loss and the end-stage HIV.
I also do believe that at this point in time the policies around withdrawal of treatment or “no-CPR” policies are irrelevant because the focus is now on end of life care.
Even if they attempt continuing ECMO for a few more days, this potentially life sustaining treatment might not be sufficient and your Dad may pass away anyway.
With the ECMO and the inotrope/vasopressor therapy, it only takes one form of life support to be taken away and your Dad would not be able to sustain life.
This is why I feel confident that they have maximised all therapies and life support for now and there is nowhere to go from here.
At least they have been open and transparent in sharing their policies with you and there is nothing in the policies that they are not adhering to.
I think the next step is to prepare for the passing of your Dad and we can discuss this in our next phone call.
Warm Regards & Best wishes
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!