Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to feature another case study with one of our clients and the case study this week is
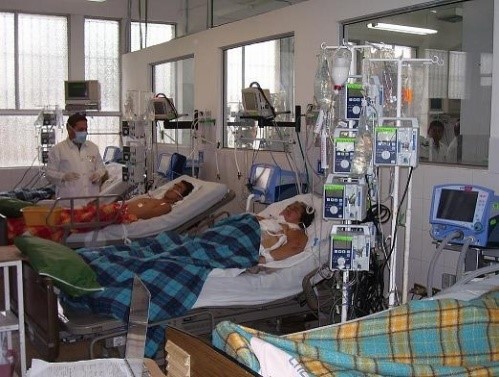
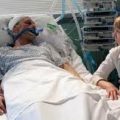
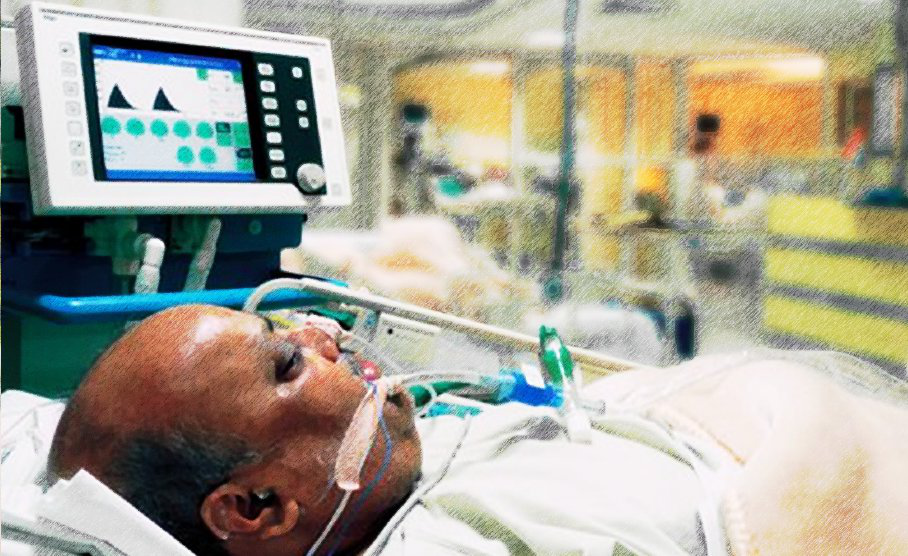
CASE STUDY: My 87 year old Dad has been in ICU two weeks after cardiac arrest, he’s slowly “waking up” will he need a tracheostomy?
This is another great case study with one of our clients and an excerpt from a 1:1 phone counselling and consulting session with me and it just goes to show once again that families in Intensive Care don’t know what they don’t know.
Intensive Care teams don’t take the time to explain things and issues in details and as you can see in the case study, one of Lauren’s complaints is that she’s dealing with junior doctors who don’t seem to have all the necessary experience dealing with this complex situation.
Lauren: Hello?
Patrik: Oh, hi Lauren. It’s Patrik from Intensive Care Hotline. How are you?
Lauren: Oh. All right, I guess. I’m just here … having a lot of questions about this hospital. It’s mainly interns that have seem him. ICU doctors but they’re all young.
Patrik: Mm-hmm (affirmative). Yeah. That’s a concern. That’s a concern.
Lauren: Everyone we meet with has a different story to tell us. It’s kind of like … whenever I’m meeting with the hospital’s supervisor tomorrow … trying to get him-
Patrik: Right. Why do you meet with the hospital supervisor?
Lauren: Sorry?
Patrik: Why are you meeting with the hospital supervisor? Are you making a complaint?
Lauren: Because we talked to one of the doctors yesterday and every doctor we speak with has a different … we’re not getting the same stories is what I’m saying. The first doctor told us … They tried to wean him three days ago, because they said he was breathing over the machines but then when they tried to wean him off, they said he panicked. So, they had to put him back on Propofol and keep him on the machines. The first doctor told us, “Even though he does well …” Telling us pretty much the stomach’s still not working. He might just starve to death. I mean, really negative. This woman doctor I spoke with last night said we’re gonna have come to a decision if we want to put him on the trach or keep him on the ventilator, which she said, “You don’t want to keep him on that long …” I don’t know. I really … That’s why we’ve spoken to the supervisor.
Patrik: Yep. Okay. So, it’s nothing unusual that patients panic when they come out of an induced coma and it’s nothing unusual that the first attempt to get somebody off the ventilator don’t work. Nothing unusual, right? I think-
Lauren: Okay.
Patrik: … it often takes a few attempts. You said that your dad is 87. Now, you can sort of say-
Lauren: But even though he’s 87, he was like a 60-year-old.
Patrik: Yep. Yeah. I get that.
Lauren: He started getting depressed but nothing wrong with him. Nothing.
Patrik: No, no. I get that. I get that. But there is … what I will say … and I agree with you. Age is not a big factor. If your dad has previously been fit and well. What age is doing, however … let’s just say a similar situation for a 25-year-old, they come out of the induced coma easier. With increasing age, it takes a bit longer to get out of the induced coma and that’s important to know because getting out of induced coma can be challenging but it’s definitely something that can be overcome with a bit of patience.
Related article/video:
Lauren: But you see, whenever … okay …
Patrik: With some-
Lauren: He’s still communicating with them.
Patrik: Oh, well, that’s good.
Lauren: Whenever-
Patrik: That’s even better.
Lauren: Right.
Patrik: That’s even better.
Lauren: Right. He tells them whether or not he’s hurting.
Patrik: Yeah, yeah. That’s even better. So, from that perspective, he’s doing all the right things and you’re saying that most staff that you’ve come in contact with seem to be quite young. Now, I can tell you … I’m not a doctor. I’m an intensive care nurse. I worked in intensive care for 20 years. I’m not sort of wanting to go overboard, but most of the doctors who just start in ICU, they know everything from the textbook but they haven’t got that hands on experience to get somebody out of an induced coma. Right?
Lauren: Right.
Patrik: And if he’s communicating that’s a sign that he can’t be far away from getting off the ventilator. And now the, the good news about Propofol is … Propofol is short-acting. That means as soon as they stop Propofol, your dad is meant to wake up. That’s good because there are other medications that are long-acting and it takes a lot longer for patients to wake up. So, that-
Lauren: Right. Well, today, they were supposed to start weaning him off the Propofol.
Related article/video:
Patrik: Yeah, good. Good. And do you know whether he … he must be getting something for pain relief. Do you know what he’s getting? Do you know what that-
Lauren: Morphine.
Patrik: Morphine. Okay.
Lauren: They were given him Morphine every two hours but yesterday, when I went, he had not gotten it … I got there at seven o’clock that night. He hadn’t gotten it … and six o’clock in the morning. He had gone all day into the night without it.
Patrik: Yep. Good. Good. Because what you need to know about morphine is … morphine is … that the main side effect is Morphine is respiratory depression. Basically, respiratory depression means it’s suppressing efforts to breathe. Morphine is a wonderful drug for pain but the main side effect is not conducive to trying to wean somebody off the ventilator. Okay? So, by sort of minimising the Morphine … that’s certainly something they need to aim for, okay?
Lauren: Okay.
Patrik: To answer your original question with the tracheostomy … a tracheostomy is good for patients who can’t … if your dad has been ventilated for two weeks and he can’t come off the ventilator after several failed attempts, right? Then I would say, “Yes, do a tracheostomy because he had several attempts to get off the ventilator. You’ve tried. It didn’t work. Let’s do a tracheostomy.” Now, a week on a ventilator is not a long time in intensive care terms. Now, I know it probably feels like an eternity for you, right?
Lauren: No. You see … my daughter … I have a daughter that’s in Oregon and she came last night to see him and she said the same thing you’re saying. She was like, “I don’t understand what’s the hurry. A week is not a long time. He has his mind. I don’t understand what they’re rushing y’all for.”
Patrik: Yep. Well, I can tell you what they’re rushing for. I can tell you what they’re rushing for. They’re rushing for two things. Number one, getting him off the ventilator, then they can probably send him to a ward in the next few days. That’s one thing. One reason why they’re trying to rush. The reason why they’re trying to rush towards the tracheostomy is simply once he’s got a tracheostomy he can be moved to long-term acute care.
Lauren: Oh.
Patrik: So, that’s the rush and that’s why it’s so important that before somebody considers the tracheostomy, you’ve gotta think about, “Okay, what are the benefits? What are the drawbacks of a tracheostomy?” You need to understand the hospital system. Basically, saying what I’ve just said now, their goal is to get that ICU bed freed up. That’s their goal. Right?
Lauren: Okay.
Patrik: Because ICU beds are in demand. They’re in huge demand.
Lauren: Yes.
Patrik: So, their goal is to free up the ICU bed. So, therefore, a tracheostomy, yep, they’ll do that and he’ll get shipped off to a long-term acute care facility, which is not desirable, as far as I’m concerned. So-
Lauren: Oh, no, no, no.
Patrik: So, from my perspective, what needs to happen is they need to maximise their efforts to get your dad off the ventilator and not just saying, after the first or after the second failed attempt, “Oh, he needs the tracheostomy.” As I said, if after two weeks, he still can’t be weaned off the ventilator, fair enough, then I’d say, “Okay, well, maybe he needs the tracheostomy.” I tell you what I can do. I’ll send you some links to some articles and videos that talk about when to do tracheostomy. Okay? That’s one thing that I’ll do. The other thing that needs to happen, from my perspective, is they need to start some physiotherapy or Physical therapy. They need to minimise the morphine, if they can. They need to sit him up. They need to stimulate him and I don’t know whether they’re doing that or not.
Related articles/videos
Lauren: Well, they started sitting him up and they started feeding him … trying to see if he’ll take protein … trying to feed him a little bit to see if his stomach will take it. And they had him sitting straight up to try to stop him from having another … a like he … I can’t think of the name, but you know what I’m talking about.
Patrik: Yep. Yep.
Lauren: Aspirate again.
Patrik: Yeah, of course.
Lauren: And that too, I want to ask you about because my daughter was questioning me too about that. Okay. He was … after his surgery in the ICU, okay, they pulled him out of ICU too quick, I find. He was just in a few days after the surgery. I don’t remember because like I said … we’re an hour away from the hospital. We don’t know the-
Patrik: Oh, I see. I see.
Lauren: Okay. So, anyway, they brought him to a room, which I was shocked that they brought him to a room that quick, then, okay, that week every day I went, he was talking. He was fine. He was upset about what happened and he said to me, “Oh, God. I have a long way to go after what happened.” And I said, “Yes, Daddy, you do. But you strong enough and you can do it.” And he was encouraged. He’d get aggravated sometimes when the pain would start, but he was encouraged and then the Friday, my sister went earlier and she fed him a couple of spoons of pudding and then that night I went and they said they were taking him in for a … a CT, a test, to see about the intestines and then they found that there was like a little part of the intestines that was still dead, but they were going to try to wake it up. Fine. Then the Friday, they were taking him … and Monday, he had started complaining that it hurt … The only real pain was between his shoulder blades and I said to the nurse, “I hope pneumonia’s not setting in. That sounds like pleurisy or pneumonia.”
Well, then he had a little cough and Thursday, my mom … he coughed into a napkin and she showed the nurse it was green. She said, “That looks like pneumonia.” So, then Friday they took him in for another test to see about pneumonia. Well, then Saturday morning, they never called us at six o’clock in the morning. We called at eight and they said, “He aspirated and went into cardiac arrest,” and they … So, we rushed over there and the nurse said, “They pulled two and half litres of faeces and blood.” Now, how … can you … tell me how can you, running these tests, how can you not see that much fluid getting into his lungs?
Patrik: That … look … I was exactly thinking the same one I read your message. I was exactly thinking the same, “How can they not?” Right? I can’t answer you that question. It almost sounds negligent to me, right?
Lauren: Right. And that’s why the doctor had said, “If y’all want a meeting with the supervisor …” Because I said to her, “I had never met this doctor that I talked to last night.” It’s a new doctor every night. Well, they say it’s the ICU group that we have to see and I told him, “I don’t have a compliant. The nurses are wonderful to him. But the doctors are so cold and none of them …” Like she wasn’t even familiar with his chart when I questioning her. “Oh, well, I didn’t read this and I didn’t read that.” I said, “That’s what I’m talking about. Y’all don’t even know him.” You’re reading a paragraph and still coming in and telling the nurse …
Patrik: Yep. For the doctors, your dad is just a number.
Lauren: Right. Right.
Patrik: Okay. So, here is what we could do. As I said to you, I will send you a link to some articles and videos, “When to do a tracheostomy.” Again, from my perspective, this is way too early … they haven’t even maximised the efforts to get your dad off the ventilator. As I said to you, you’ve gotta keep the system, the hospital system, in mind. Their goal is to free up this ICU bed. Now, here is what we could do as well. We would be very happy to talk to doctors directly and find out what they’re doing, what they’re not doing, how are they treating the cardiac arrest, what are chest X-rays showing, because chest X-rays … or his chest X-rays would be another indicator on how far away he would be to get off the ventilator, right?
Lauren: Okay.
Patrik: Also, if we knew whether he is on any medication for his heart. If he had the cardiac arrest a few days ago, there is a fairly good chance that he’s getting medication to support his heart at the moment. So, let’s just say his heart has been severely weakened from the cardiac arrest. That might also be another challenge to get him off the ventilator but, again, I would have to speak to one of the doctors or the nurses to figure what’s been happening-
Lauren: Right. Now, we haven’t anything about damage to the heart, at all.
Patrik: Of course. But you’re also probably … the challenge, as a family member in intensive care, is you don’t know what questions you need to ask. They’re not … they don’t tell you the full story. They pick bits and pieces. They don’t tell you the full story because they assume you don’t understand or you don’t know. They’re trying to hide behind medical language … blah, blah, blah. We know all of that. What we could do is we could speak to the doctors directly or if you, for example, had a meeting with them, we could call into the meeting. That’s the sort of service we can offer as part of your 24/7 unlimited 1:1 phone counselling, consulting and advocacy package. But as a starting point, I would definitely like to send you some links to some articles you can read and there’s also some videos-
Lauren: That would be good too.
Patrik: Absolutely. Absolutely. Sorry, what was-
Lauren: Now-
Patrik: Yep.
Lauren: I wanted to know this question too. If he does end up with a trach, can you take … if he gets strong enough, can they remove it?
Patrik: Oh, yeah, absolutely. A trach should always be a temporary thing. A trach should be-
Lauren: That’s what I wanted to know.
Patrik: Yeah, a trach should be a temporary thing. At the same time, again, with increasing age, it gets-
Lauren: Right. It gets more challenging.
Patrik: … it gets more difficult, but … and that’s why I’m saying. That’s why I’m so adamant about they need to maximise their efforts to get out this breathing tube in the first place without doing the tracheostomy.
Lauren: Right.
Patrik: Right?
Lauren: Well, listen … can you send me material and I … my brother might want to call you too and talk to you.
Patrik: Yeah.
Lauren: That’s good. That’s good.
Patrik: So, there’s great information there and, as I said to you, I would be very happy to talk to you again or to other family members.
Lauren: Okay. All right.
Patrik: You’re most welcome. All the best.
Lauren: I appreciate it.
Patrik: You’re most welcome. Take care.
Lauren: You too.
Patrik: Bye-bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!