Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question last week was
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer the next question from Belinda one of our readers and the question this week is
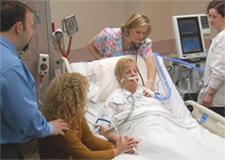
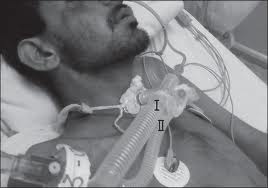
My 84 year old Dad has been in ICU for three months! He’s ventilated with a tracheostomy, the doctors want to let him die and turn off the ventilator! We want to take him home instead, what are our options? (PART 2)
You can also check out PART 3 of this series by clicking on the link.
This series of questions are excerpts from a 1:1 phone/Skype counselling session and a series of email counselling and consulting
Belinda describes her father’s situation in Intensive Care as follows
Hi Patrik,
thank you Patrik for your time on the phone on Tuesday!
Since we last spoke my father got low blood pressure and as soon as he gets moved only by the slightest bit he de-saturates(=low oxygenation).
So for now he is too fragile to be moved…since then they move him very carefully…
So I hope they don’t start again tomorrow with trying to move him too much.
Yesterday they started talking about taking my Dad to a hospice and he is “suffering” what we are waiting for, because we still want him at home.
He is very weak but he doesn’t look like he’s suffering and he’s not in any pain….they try to talk to all of us in a different form of taking him off the ventilator.
He’s still on 70% of oxygen on the ventilator…
We don’t believe in that at all and we could not live with it…so we are hanging in there that
his health turns around and improves.
We really feel pressured to agree to something that we believe will kill our father and we are not ready for it.
They are now talking about sending him to a Hospice after they have taken off ventilator and the tracheostomy. It sounds very cruel to us and we don’t want it.
They basically want to get rid of us and our goal is still home care with continued treatment.
But they say he is too fragile what I believe.
They put him on another set of antibiotic as they believe he’s got sepsis again, but my Dad is now getting weaker and we’ll see if the Antibiotics work.
But we don’t believe in turning off the Ventilator, he is still fighting.
I guess no other long term facility will take him and we want to stay in the ICU, he needs
ICU care, either he’ll improve and we take him home or….
He only has a chance with ICU treatment to get over it, at any Long term Facility he won’t survive.
What do you think what are his chances in ICU to survive whilst he remains that fragile with sepsis and low blood pressure?
Thanks
Belinda
Hi Belinda,
thanks for clarifying your father’s situation and thanks for the update.
If he has low blood pressure and if he de-saturates he certainly needs ICU care and treatment.
Also with your Dad’s high oxygen requirements of 70% it doesn’t surprise me that he de-saturates quickly when being moved.
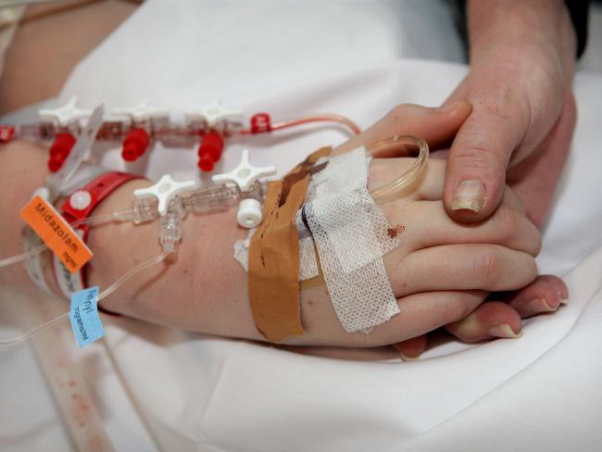
With his low blood pressure(=hypotension) they would have started him on Inotropes or Vasopressors to manage his low blood pressure.
With low blood pressure(=hypotension) during Sepsis he might also get an increased amount of IV fluids such as Albumin 5% or Gelofusin(=colloid fluids) to improve his fluid status and also increase his blood pressure.
If they haven’t, you may want to find out rather sooner than later whether they are planning to actively manage your Dad’s low blood pressure or not. If they don’t actively manage your Dad’s low blood pressure with Inotropes or Vasopressors as well as IV fluids, it could be part of their (documented) plan to “withdraw treatment” that they still haven’t formally discussed with you.
It’s nothing uncommon that they continue to try and talk you into taking your father off life support. They have their “hidden agenda” and we have spoken about this a couple of days ago and thankfully you are very clear in what you want. Don’t retreat from that.
Again, you should continue objecting a “withdrawal of treatment” if this is what you feel is the right thing to do. If they actively manage your Dad’s low blood pressure with medications they are being pro-active and they are doing the right thing.
Related:
By giving Antibiotics they are actively treating him at least for an infection/ Sepsis. The infection/Sepsis is most likely also leading to your Dad’s low blood pressure.
They would also need to look at finding a source of the infection and they need to send a sputum sample of his chest, they need to culture his blood as well as taking a Urine sample. By doing that there is a chance that they may find a source of the Sepsis.
There is a good chance that your Dad has a chest infection/Pneumonia if he’s still requiring 70% of oxygen on the ventilator.
Of course no long-term care facility will be taking your Dad if he is fragile and in need of ICU care and treatment. Long-term care facilities are usually for medically stable ICU Patients with ventilator/ Tracheostomy needs. Your Dad is not medically stable at present, not with low blood pressure(=hypotension), Inotropes/Vasopressors ,sepsis and 70% oxygen on the ventilator.
As long as he’s as fragile as you describe he certainly needs ICU treatment. As soon as he’s over the Sepsis and he’s off Inotropes and the Vasopressors he could go home with a service like INTENSIVE CARE AT HOME.
The question you may want to ask yourself, your family and your Dad in the next few days might be that if your Dad isn’t improving if you want to take him home for palliative care.
Check out
Have you had chance to look into taking your Dad home as well and if so are there any services available in your area and/or are you prepared to take this step?
I know it can be overwhelming into making all these decisions, however you have been remarkably brave and strong so far and I’m sure you continue to do so.
But it definitely sounds to me like you are not prepared to give up lightly. As long as your father is not unduly suffering you need to continue to fight for what you believe in.
Please let me know if you have anymore questions and you can always give me a call.
Take care
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!