Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another frequently asked question from our readers and the question last week was
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer another question from one of our readers and the questions this week is
My 79 year old sister has had seizures and she’s now in ICU! She’s not waking up and she’s having a tracheostomy! Can she improve?
This question from Tam is an excerpt from a 1:1 phone counselling and consulting session.
Tam describes her sister’s situation as follows.
Hi Patrik,
my sister had seizures two weeks ago and has been on the ventilator since then.
The ICU doctor said her condition is not improving and we have to decide whether to remove the ventilator and let her go or put in the tracheostomy.
They have done a CT scan of her brain and it shows some mild damage.
They said my sister is not responding to commands yet even though she has been out of the induced coma for a few days now.
My sister is 79 years old and has dementia.
We had to also think about her quality of live with the trachea on.
After we had to think about the options for a couple of days we wanted to give our sister a tracheostomy so that she can have the best chance of recovery.
Regarding her quality of life, at least my sister was alert and physically healthy before the seizures and ICU admission.
That’s what I hope she will be able to do again with the tracheostomy. I hope that’s the best option for her.
Even though we are happy that we made some decisions now we still feel we don’t know what’s yet to come, therefore I would appreciate if you can give some advice on this.
Regards,
Tam
Hi Tam,
thank you for clarifying your sister’s situation and thank you for your questions!
Also thank you for signing up for my 1:1 phone counselling and consulting service.
First, it’s nothing unusual for elderly people to take their time when “waking up” after when faced with challenges such as an induced coma as well as seizures.
Seizures fall into the category of head and brain issues and usually a further delay in “waking up” can be expected.
On top of the drugs being used for an induced coma, there would have been medications given for seizure activities that would have further dampened your sister’s brain responses and brain activity.
Therefore your sister needs time to “wake up” in a time frame that reflects her own needs for her own recovery.
The dementia that your sister has been battling certainly doesn’t help the situation.
However I do believe that you and your family have done the right decision to let your sister have the tracheostomy and take everything from there.
I also believe that you would have made the right decision if you were opting against the tracheostomy.
I would imagine you and your family have made the decision based on what your sister would have done if she was able to decide for herself.
Therefore, no matter your decision you have acted in her best interest.
With the tracheostomy, your sister is now having the ability to have time for coming off the ventilator and she will have time to “wake up” in her own time.
But where to from here?
It really depends.
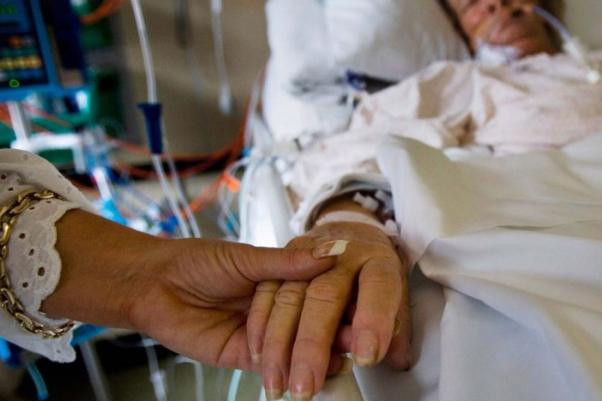
Tracheostomy and weaning off the ventilator can be a challenge and it’s often hard to put a time frame on it.
I have highlighted and explained this in this article/ video (click on the link to read the article and/or watch the video)
Furthermore, “waking up” after an induced coma after seizures can be delayed and as I have said, I have seen over and over again that injuries to the brain can put a further delay on “waking up”.
Again, I have highlighted and explained this in the following articles/ videos(click on the links to read the articles and/or watch the videos)
People in Intensive Care whether Families, Doctors or nurses often get time frames wrong and they mistakenly think that recoveries must happen quickly.
Nothing is often further from the truth and if anything it’s quite the opposite.
“Waking up” after an induced coma and “waking up” after seizures takes time, therefore two weeks into an Intensive Care stay probably feels like an eternity for you and your family and yet it is nothing in the bigger scheme of things.
Intensive Care and critical illness is often a marathon and not a sprint.
If the Intensive Care team says that your sister’s not “waking up” and that she’s not “obeying commands” it doesn’t really mean anything unless given much more time.
Time really is irrelevant in Intensive Care from a Patient recovery perspective.
You also need to be mindful that time is everything from an Intensive Care team perspective, because of the perception of scarce and limited resources.
Because of the perception of scarce and limited resources, Intensive Care teams can be fairly negative early on in painting a “doom and gloom” picture for Patients and their families.
Again you have made a good decision by giving your sister the opportunity to have a tracheostomy and you have given her the best shot at life.
Even though the CT scan of her brain is showing “mild damage” it doesn’t mean much, especially since it’s only been one CT scan.
They probably have to do another CT scan or MRI scan of the brain, as well as potentially an EEG of the brain, including a Neurology consult.
It may also depend on issues like if any medications need to be given longer term to prevent seizures such as Phenytoin(Dilantin), Keppra(Levetiracetam) and/or Epilim(Sodium Valproate) as they may interact with your sister’s Dementia.
Especially when “waking up” from an induced coma after seizures it just simply takes time and it also takes time for the brain to recover and heal.
I understand that despite your sister’s mild dementia, she was able to live independently before the seizures and the ICU admission.
Nobody knows if she can get back to that level of quality of life and level of functionality after her Intensive Care stay and again the tracheostomy will enable your sister to have time to recover and enable your sister to “wake up”.
Please also please keep in mind that if your sister needs much longer to “wake up” and also needs much longer to get off the ventilator and the tracheostomy than anticipated, you may want to start thinking about alternatives such as INTENSIVE CARE AT HOME.
A service like INTENSIVE CARE AT HOME can provide care and treatment for long-term ventilated adults& children with tracheostomies in the home as a genuine alternative to a long-term stay in Intensive Care.
INTENSIVE CARE AT HOME is also way more Patient and family friendly compared to an Intensive Care stay. And it’s also by way more cost effective compared to an Intensive Care stay.
Therefore everybody is winning!
I hope this gives you some insights and clarifications about what to expect and also what options you might have to look at when making crucial decisions for your sister and your family.
And for now, stay positive and hope that your sister will “wake up”, obeys commands and also gets off the ventilator and the tracheostomy.
Give her time, love and nurturing for that.
She has the best of families around her to enable her to have the best of recoveries!
Please let me know if you have any other questions and challenges.
Wishing you and your family all the very best!
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



