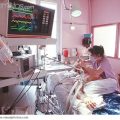
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question last week was
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer question from one of our readers and the question this week is
My 76 year old Dad has been in ICU for one month! He can’t be weaned off the ventilator and his tracheostomy, what are the alternatives? Help!
This question from Felix formed part of an email counselling/consulting session with me.
Felix writes
Hi Patrik,
first of all I want to thank you for your kind and generous service for many caregivers who have their loved ones in Intensive Care.
My dad is 76 he has been in the ICU ward here in North Carolina since May 17th and his stay in ICU has now been for about a month!
He has had complications with MRSA & CRE Pneumonia.
He was given 3 types of antibiotics, Metronidazole(Flagyl), Polycimin-B & Tetracycline.
His lungs to say the least have taken a beating. In the fourth week he was taken off the antibiotics.
His lungs are much clearer now according to the last chest X-Ray.
The blood cultures have come back negative.
They have been trying to wean him off the ventilator and they had not much success.
They tried him on the tracheostomy collar for a couple of days to wean him off the ventilator, at first he lasted for 12 hours, then 8 hours and now he has gone backwards to only be tolerating between 1-3 hours off the ventilator.
His heart rate will go up to 130 beats per minute when he’s off the ventilator and on the trache collar. He is on Coreg(Carvedilol) to keep his HR between 70-80 beats/min.
He does have CHF(Chronic heart failure) with 40%-LVF(left ventricular failure). His blood pressure fluctuates between 120/75 to 89/45.
His RR(Respiratory rate) on the ventilator is between 14-17 per minute. When he’s going on the trachea collar his RR(Respiratory rate) is going up to 40/minute. His ventilator machine oxygen (O2) will be set between 45% in the day and 60% at night. Generally his SO2(Oxygen saturation) is at 100%.
The therapists also keep his bed propped at 45% to strengthen his lungs. The doctors don’t want to keep trying to wean him off the ventilator in the ICU and that he would be a candidate for a Long Term facility to be weaned off. The doctors say that because of the severe pneumonia his body and lungs had to endure, he is weak and it therefore will take him longer than what they can keep him in ICU for.
How long can someone in my dad’s circumstances be able to be weaned off the vent? Thanks for your valuable time! God Bless! Felix
Hi Felix,
thank you for your inquiry and for using my email counselling/ consulting service!
I have also received your phone message!
I appreciate your kind words and I’m sorry to hear the difficult circumstances that your Dad is finding himself in.
There is no straight forward answer to your question, because critically ill Patients on ventilators with tracheostomies are different and therefore the time frames differ in how long it’ll take them to be weaned off a ventilator and the tracheostomy!
However I have a number of suggestions from my experience and I’m sure you’ll find some useful advice after having worked with hundreds of ventilated Patients with tracheostomies in Intensive Care as well as in a home care environment!
My best advice is to start with this article/ video here (click on the link)
TRACHEOSTOMY AND WEANING OFF THE VENTILATOR IN INTENSIVE CARE, HOW LONG CAN IT TAKE?
This article/video will give you a good overview.
There are a lot of things that you as a family member can influence if you find the right information and if you get the right advice!
You also need to be prepared to do what the 99% of the families in Intensive Care who make no informed decisions, who don’t get peace of mind, control, power and influence are not prepared to do!
If you are prepared to go against the grain, take my advice you will see results, period!
To start off with, your Dad will need to get into a proper day and night rhythm whilst he’s in Intensive Care. Most long-term Patients in Intensive Care have a disturbed day and night rhythm and this is simply because Intensive Care is a 24 hour environment with all sorts of disturbances going on 24/7 including care needs, especially whilst being on a ventilator with tracheostomy!
Next, you’ve mentioned that your Dad has chronic heart failure and therefore weaning him off the ventilator might take longer or at the very least it might be more challenging as a weak heart usually impacts on the lungs as well!
Furthermore, starting your Dad off on 12 hours a day on the tracheostomy collar, especially with a weak heart might not be the right thing to do. Usually a slower weaning process is a gentler and also wiser approach and it has a better chance to succeed in the long run.
You’ve also mentioned that your Dad still needs 40-60% of oxygen whilst on the ventilator. That’s still a fair amount of oxygen and it doesn’t surprise me that your Dad is only lasting for 1-3 hours on the trachea collar. Usually oxygen requirements on the ventilator should be less than 40% before starting the weaning process on a tracheostomy collar/ mask.
Combining this with a weak heart and you have a recipe for making it a slow wean off the ventilator.
Starting off with two hours off the ventilator and two hours on the ventilator during the day and then increasing the frequency to stay off the ventilator might be a more successful approach.
Again, your Dad might be frightened when he spends too much time off the ventilator, especially since it’s been four weeks now that he’s been in ICU and on the ventilator!
Once your Dad can tolerate more time off the ventilator as his strength increases, he can hopefully get into a routine where he stays off the ventilator during the day and get back on the ventilator over night!
This would also get him back into a normal day and night rhythm! Getting him a good night’s sleep is vitally important, so he can feel rested for the day and have strength to have time off the ventilator!
Good nursing care is also extremely important and is often highly underrated! Your Dad needs to get good mouth care, eye care, regular washes and showers to make him feel comfortable and well looked after!
You also mentioned that they keep his bed at a 45% ankle to strengthen his lungs! That can be important and it might contribute and it’s not enough! Your Dad needs to get out of bed at least twice a day at a bare minimum! The Physiotherapists and also the nurses need to mobilise your Dad into a chair!
That’s absolutely vital and it needs to happen full stop!
This will help and it will build up your Dad’s strength!
Most importantly, you need to think outside of the box! The Intensive Care team wants to send your Dad to long-term acute care and they probably want to do so because the ICU team doesn’t want to continue weaning your Dad in ICU most likely for bed management reasons and also for financial reasons.
That’s most likely what’s happening, however before your Dad is going into long-term care, you should consider a much better alternative.
In this day and age Intensive Home Care is a genuine alternative to a long term stay in Intensive Care and for example a service like INTENSIVE CARE AT HOME can wean long-term ventilated Patients with tracheostomies off the ventilator at home.
You may want to consider this and you can fund more information here INTENSIVE CARE AT HOME
Furthermore your Dad has been in ICU for one month, therefore it now might be the right time to get the ball rolling to get your Dad home with specialised Intensive Home Care.
More specific help that I can offer you now is to check out the following Ebooks/ Videos (click on the links)
Both Ebooks and Videos will give you specific insights into long-term ventilation and tracheostomy and will help you to make informed decisions, get PEACE OF MIND, control, power and influence, irrespective of the challenges.
Both Ebooks and Videos will help you to get a handle on things and will give you insights of what’s really happening and the information is cutting through all the myths and the BS and it’ll help you to get your desired results.
Another option is to talk to me personally over the phone or Skype and get ONE on ONE counselling and consulting and there I can go into even more detail.
You can also check out our “your questions answered” section where you’ll find a ton of questions about the issue as well.
Please let me know if you get stuck or if you have any other questions.
Thank you& Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
Your Friend
Patrik Hutzel
Related Articles