Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How To Avoid A DNR Or How To Revoke A DNR! Livestream!
You can check out last week’s question by clicking on the link here.
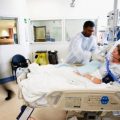
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Mikaela, as part of my 1:1 consulting and advocacy service! Mikaela’s sister is ventilated in the ICU and she is asking why the ICU doctor can’t provide their hospital policy for DNR (Do Not Resuscitate).
My Sister is Critically ill In the ICU and We are Worried Why the ICU Doctor Can’t Provide their Hospital Policy for DNR (Do Not Resuscitate)? Are They Hiding Anything from Us?
Mikaela: Hi, this is Mikaela. Are you the primary care provider of my sister?
Dr. Min: Yes, how can I help you?
Mikaela: It was just about the DNR.
Dr. Min: I’m on her records at the moment.
Mikaela: Okay.
Dr. Min: There is no DNA CPR (Do not attempt cardiopulmonary resuscitation) documented on her records. There isn’t one, just like you asked. Your concerns about the DNA CPR have been documented in the documentation of the discussions you’ve had with my colleagues.
Mikaela: Yeah. All right. That’s what I thought I heard. Sorry, it was just breaking up in between.
Dr. Min: So yeah. So your concerns about it are documented and there isn’t a DNA CPR on the system. The only thing that I would say to that is, in the event of another cardiac arrest, we would do treatments that we thought would be appropriate. Resuscitation attempts that we thought are appropriate. But I can’t guarantee that they would be successful.
Mikaela: Yeah. That’s fine.
RECOMMENDED:
Dr. Min: Yeah. Sorry go on.
Mikaela: We were just checking on the heart and the cardiology. Is there any possibility that we can speak with the cardiologist that’s directly looking after Tina?
Dr. Min: You can. Yes. You could certainly… When I speak to them, I can certainly ask them to-
Mikaela: Can you just ask them to reach out maybe?
Dr. Min: To speak to you. But what specific questions do you have for them?
Mikaela: Something that I just rather have speak to them on an individual basis? About, to be honest. There’s nothing against you guys. It’s just to get a bit more of an understanding of how the heart’s functioning and a bit of more layman’s terms, if it were.
Dr. Min: Yep. I will certainly ask them to give you a ring when they reviewed. Yeah, no problem with that.
Mikaela: Thanks, cheers for that. Thanks for that.
Recommended:
Joseph: Is that her… Sorry. Can I ask, is that her cardiologist?
Dr. Min: The cardiology registrar who covers during the day, when they come round, I can ask. If you want to speak to a specific cardiologist, your best thing to do is actually ring up and speak to her secretary and make an appointment. That’s probably a better way.
Joseph: Okay.
Dr. Min: Because what tends to happen is the registrar visits each day. And we have a discussion about where we are from an ICU and a cardiology point of view together. And she will then liaise back with her consultant. So I can certainly ask her to give you a ring when she gets the chance, or I can ask her to pass on your request to her consultant. But if there is a specific consultant that you would like to speak to, your best bet is to go through switchboard and speak to her secretary, and then you might be able to arrange a specific time for a conversation.
Joseph: Okay. So I’d like to speak to Dr. Marie … What’s her name?
Mikaela: Yes, Dr. Marie.
Joseph: Because I’ve never spoken to her. I’ve never spoken to this woman. I’m speaking to different consultants since I’ve been here. It’s like Tom, Dick and Harry. I’m speaking to different people all the time. I don’t know who I’m speaking to. So I like to speak to the horse… From the horse’s mouth. I like to speak to the main person, please.
Dr. Min: Okay. If you have a specific name in mind, you are welcome to try and speak to them through the secretary. But the team that are doing the predominance of the care at the moment are the intensive care team.
Joseph: I know, but I like to speak to the person that’s actually looking after her heart. And that’s what she’s come in for. Initially. So the cardiologist I understand was Dr. Marie. So I have not spoken to her once.
Dr. Min: So while people are on intensive care, they are looked after by the cardiology consultant of the week. They don’t come in usually under a specific cardiologist.
Mikaela: Yeah. Sorry. It’s just that obviously when she came in, it was Dr. Marie and still on her bedside.
Dr. Min: It was Dr. Marie, wasn’t it?
Joseph: Yes it was.
Mikaela: Yeah. And on her bedside, it still states that, that is her cardiologist or the cardiologist in charged for her condition. But yeah, if we could arrange for that, I mean..
Dr. Min: Yeah. What you need to do is if you go through the hospital switchboard and ask to speak to Dr. Marie’s secretary-
Mikaela: Yeah.
Dr. Min: … And she will tell you the process for arranging a telephone call with her.
Mikaela: Yeah.
Dr. Min: … And about what it’s about.
Mikaela: Okay. And then is that the same for the neurological department as well? Who’s the actual neurologist that’s come to the… Was it Dr. Toni?
Dr. Min: So, the neurologist who came to visit was Dr. Toni, who was one of the rehab neurologists.
Joseph: Okay. I’d like to speak to her as well please.
Dr.Min: By all means. Yep, same process. Speak to her secretary to try and arrange a suitable time to speak to her.
Recommended:
Mikaela: Yeah, that’d be great. Okay, cool. It’s just… We just need to get a bit more clarity on the situation in terms of neurological and cardiology standpoint, just to see where we stand essentially. Because with all due respect, we hear it from all different people in terms of her recovery and such, but from consultants wise, like example you. However, we just haven’t spoke to the main people in charge on the predominantly… In terms of the actual organs and were they’re working. Just to get a little more in-depth look at it. So yeah, that’s fine. We can work on that.
Mikaela: In terms of the paperwork and such. So is there a hospital policy on anything for DNRs and whether we agree to it, whether we don’t, et cetera? Is there a link that I can go to?
Dr. Min: In terms of DNA CPR, the management of the clinical care of a patient in terms of the delivery of actual care, it is at the remit of the doctors looking after them at the time. But in terms of planning, things like DNA CPRs, or withdrawal of treatment and things like that, they are done in discussion with family, where the family are there to give the perspective of the patient, if the patient cannot discuss it themselves, for reasons such as sedation or neurological injury.
Mikaela: Yeah.
Dr. Min: So-
Mikaela: Where this is the case with my sister at the moment.
Dr. Min: I beg your pardon?
Mikaela: That is the case with Tina at the moment. Where she hasn’t got any mental capacity to make a decision on her own behalf.
Dr. Min: That’s right. So you’re speaking as her advocates.
Mikaela: Correct.
Recommended:
Dr. Min: Yeah. So that’s the state of play. And what that means is, if there are treatment decisions that are of uncertain benefits, then there is a requirement to consider the patient’s best interests and the patient’s wishes of which part of that is discussing with advocates if they haven’t got capacity themselves.
Mikaela: Yeah.
Dr. Min: But in the event of treatments that have no benefit, then I’m afraid they can’t be requested. If there is a treatment that you want, that the medical teams do not feel poses any benefit to the patient, then that’s not something that can be forced through.
Dr. Min: However, in the event of a situation like this, where there is disagreement on outcome, then in a DNA CPR form, if you are concerned about the form being put in, I’m happy for it to not to be put in. But the more important aspect is that the lines of communication between the medical team and the family stay open. So it’s important for me that you have the opportunity to express your concerns and feel that they’re listened to which I’m more than happy to listen to. And I’m happy to discuss it as you see it.
Mikaela: Yeah. Thank you for that, Doctor. We appreciate that. So in terms of how she’s looking at the moment, obviously not much has changed. We kind of expect that. In terms of her ventilation process, how’s the weaning going?
Dr. Min: So the weaning as you… I think at the end of last week, the plan was to try and wean her down onto CPAP and then onto a slightly different ventilator.
Mikaela: Yeah.
Dr. Min: But she had a little bit of a setback and went back onto what’s called pressure support over the weekend.
Mikaela: Yes.
Suggested links:
Dr. Min: On Saturday, an alternative weaning plan, which is called sprint weaning, which is where rather than dropping the pressure support by one every day until you’re on none at all. What you do is you drop the pressure support to zero for five minutes in every hour, for example, and you increase the period of time in every hour where the patient has no pressure support.
Mikaela: Okay.
Dr.Min: That’s what’s called the sprint wean.
Mikaela: Yeah.
Dr.Min: She did 10 minutes in every hour without pressure support yesterday, quite successfully.
Mikaela: Yeah.
Dr. Min: And so far today she’s managed 10 minutes… Sorry, 20 minutes in every hour without pressure support.
Mikaela: So this is the sprint weaning… So it’s like in an interval process.
Dr. Min: Say that again?
Mikaela: It’s like an interval process that you’re working on at the moment. So she’s doing it in short intervals.
Dr. Min: It’s just another way of weaning people.
Mikaela: Yeah.
Dr. Min: There are infinite different ways of weaning people. And the process that she was following last week was to gradually reduce the pressure support by a fixed amount each day until it’s off and that led to a bit of a setback. So this time we’re leaving the pressure support at its particular level, but dropping it to zero for a fixed period of time each hour.
Mikaela: So when you said setback, what sort of setback did you come across?
Dr. Min: That her oxygen levels went up and her tidal volumes went down. So she needed a bit more pressure support to get… Which was put back on.
Recommended:
Mikaela: Yeah. Oh, that’s fine. Sorry, just one second. Was there anything more that you wanted to ask? Sorry, I just got, I’ve got my father here as well and..
Dr. Min: Yeah no problem.
Joseph: Now, okay. I’m Tina’s dad. Can I just check her blood pressure levels? And what’s her blood pressure like? Is that okay?
Dr. Min: It’s fine.
Joseph: And her urine levels? I think-
Mikaela: Kidney.
Joseph: What was that?
Mikaela: Kidney.
Joseph: Kidney function. There was a concern about kidney function-
Mikaela: She is on fluids.
Joseph: … And fluids.
Dr. Min: So, she’s still passing urine. Her kidney function is stable.
Joseph: Right. There was another one … Glasgow Coma Scale, I think the nurse said this morning that she opened her eyes, although be it that she didn’t look directly at her.
Mikaela: Not purposeful.
Joseph: … Purposely, but she did open her eyes.
Dr. Min: Okay.
Joseph: Did you know that?
Dr. Min: I did.
Suggested links:
Joseph: Okay. The other thing I was… In terms of her stimulation, again-
Dr. Min: Her what, sorry?
Joseph: Stimulation.
Mikaela: Stimuli.
Dr. Min: Yeah.
Joseph: Stimuli. I was wondering, is she able… Is there a way that she can be seated upright in a chair? Is there any possibility?
Dr. Min: The beds that she is in allow the back to sit upright. So, she is in a sort of semi-upright position at about somewhere between 30 and 45 degrees.
Joseph: Right.
Dr. Min: But because she has no body tone or… Not tone, that’s the wrong thing. Because she doesn’t control her body position. If we sit her up too much, then her head will sort of lull in an uncomfortable position. So, we can’t sit fully upright because it’ll actually worsen her position rather than improve it.
Joseph: Right.
Dr. Min: But in terms of the stimulation that you said, when I came round this morning, she had the headphones on and was receiving the music and the stimulation as requested.
Joseph: Could you keep that on please Dr. Min? Because that will actually…
Mikaela: Resonate.
Joseph: Yeah, she does like that music.
Mikaela: It resonates.
Joseph: It does resonates with them, that sort of music. Okay, I think that’s it for me. Okay. I’ll just pass you back onto my daughter. Thank you.
Dr. Min: Okay.
Joseph: Thank you.
Recommended:
Mikaela: Hi Dr. Min.
Dr. Min: Hi there.
Mikaela: I’m sorry. It was just one more thing really on this. It was just more on the neurological side again. Do we have access still to any reports in terms of neurological reports? Because we did request for them, but there’s still no talk about getting them sent it to us.
Dr. Min: Have you written and requested them?
Joseph: Yes.
Mikaela: We’ve done it.
Dr. Min: I’m afraid you have to wait for that process to come through. There is no way of sending you written copies of the report. It has to be requested through writing. The team responsible for it then go through the process and they will send it to you in due course.
Mikaela: Okay.
Dr. Min: That process is deliberately separate from me.
Mikaela: Yeah.
Dr. Min: … So that the correct procedure is followed.
Mikaela: Yeah. No, that’s fine. That’s fine. Okay. I guess there’s not really much else to add to that.
Joseph: Yeah. Sorry, Dr. Min. Sorry. So I’m just filling this insurance form for Tina, because obviously I don’t know what her… How long she’s going to be poorly for..
Dr. Min: Okay.
Joseph: So on this form, it’s asking for the consultant’s name. I don’t know which consultant’s name to put on, really. Because I’m speaking to many consultants, I don’t know who her main consultant is.
Recommended:
Dr. Min: And I think if you put Dr. Marie, cardiology. That’s probably the best thing. As I mentioned, the person who’s looking after her in actuality, is the ICU consultant and the on-call cardiologist. The people looking after them do change, but they do update each other extensively.
Dr. Min: However, it is recorded as the person who was the on-call consultant on the day that she came in. So that would make sense to keep everything in the… The names correct all the way.
Joseph: Okay. Thank you for that. Thank you. All right. Anything else? None. Okay. That’s lovely. Thank you for your help.
Dr. Min: No problem. Is there anything else that you’d like to discuss at this stage?
Joseph: No, I think you’ve covered everything. Thank you for that. I think we’ll make a video call in about… When you thinking?
Mikaela: We’ll discuss with the nurse.
Joseph: Well, yeah. We’ll just ring the nurse in about half an hour, I think. And we’ll do the video call. Yeah.
Dr. Min: Okay. And I’m on today, tomorrow and Thursday, and I’m happy to catch up with you each day, if you think that would be helpful.
Joseph: Oh, that would be wonderful. So you’re consistent for two days then.
Dr. Min: For three days.
Joseph: Three days.
Dr. Min: Three days and I’m on call on Friday nights as well.
Joseph: That’s fantastic.
Dr. Min: So a four day run, I’d be happy to speak to you if you would find that helpful.
Joseph: That would be great. No, that would be good, having that consistency. That’s great. Thank you. All right.
Dr. Min: Okay, no problem.
Joseph: Take care.
Dr. Min: Thanks very much.
Joseph: Thank you.
Mikaela: Cheers bye.
RECOMMENDED:
Hi Mikaela,
It’s Patrik here. Thank you for sending that recording through. I think the quickest way is to just summarize from what I am hearing from this recording. I’m very happy to talk to you tomorrow. Its midnight here. But just quickly summarizing from what I’ve heard in this recording, and then very happy to get on a call with you tomorrow.
The first thing, Mikaela, is the DNR. Whilst he says there is no DNR form on file, my concern is that he says that it’s then up to the consultant on shift to make the decision to resuscitate or not, which from my experience says, whilst there is nothing documented, the consultant on shift might decide, well, we don’t resuscitate, or we don’t go to heroic efforts. A bit wary there, but yes, whilst they’re not doing the paperwork, but in their mind, they might still not resuscitate her properly if it was to happen. I do believe that leads me directly to the cardiologist. I do believe you need to talk to her. I do believe what Dr. Min said, you need to go through reception, and just call them, and try and track her down that way.
He did not answer your question about where’s the policy. He was sort of waffling around the DNR policy or withdrawal of treatment policy. He was waffling around, sort of saying that, yes, ideally, they would talk to you and consent you whilst sort of also saying, well, it is our decision at the end of the day and we always have the best interest of a patient in mind. Again, I would pin him down and say, okay, you’re telling me something that you’ve already said before. Where is the evidence? Show me the policy. Ask for the evidence, because other than that, they will just be waffling around.
Then, he talked about ventilation. Obviously, if she’s in breathing in CPAP already, that’s good. If they’re still fiddling around with the pressure support, I mean, it looks like at least she’s on her way. Yeah, there’s often setbacks when weaning someone off the ventilator. What you may want to ask for is PEEP pressure support. He mentioned that tidal volumes went down, which was probably a direct result of the pressure support being reduced. Nothing that I haven’t seen before, but I don’t buy his argument that she can’t be sat out of bed. I don’t buy that argument at all. I’d say there is a way of getting her mobilized. There is a way of simulating. I just think they’ve given up, to a degree. They’re too complacent. It’s a lot of work mobilizing people, but it can be done. I don’t believe that it’s not possible to mobilize her. I think it is possible.
The other thing that I found, a little bit, where he was contradicting himself, is you asked about the insurance form and initially he says, oh yeah, when people are in ICU, they’re looked after by the critical care team. Then, you ask him about the insurance form and then he points right back to the cardiologist. On the one hand, he says the cardiologist is not directly responsible. Then, when it’s convenient for him to delegate paperwork, he says the cardiologist is responsible. Just goes to show, they will use them as they see fit or not use them as they see fit. Just something to be mindful of.
Then, you did mention about the Glasgow Coma Scale again, and you did mention that she opened her eyes, and I know that Dr.Min more or less dismissed that, but keep looking for the things that give you hope and that you think will help Tina to improve. I know you’re nowhere near from giving up.
I think those are my thoughts. I am very happy to talk to you tomorrow. Sorry, again, it is a bit late. I really hope that you can visit Tina, or at least have a video call, and go from there. Any questions, just shoot me a message back and I’ll respond to that. Take care for now.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!