Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the first question from Paula in last week’s episode was
My father has a tracheostomy and the ICU doctors are planning LTAC! How can I keep him in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s two-part episode of “YOUR QUESTIONS ANSWERED“, I want to answer the questions from one my clients PAULA as part of my 1:1 consulting and advocacy service!
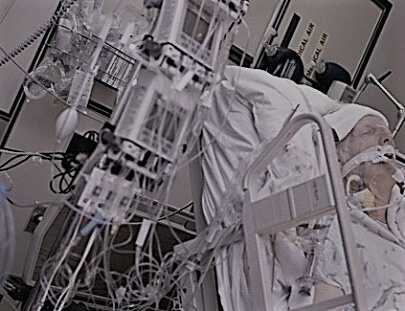
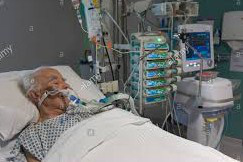
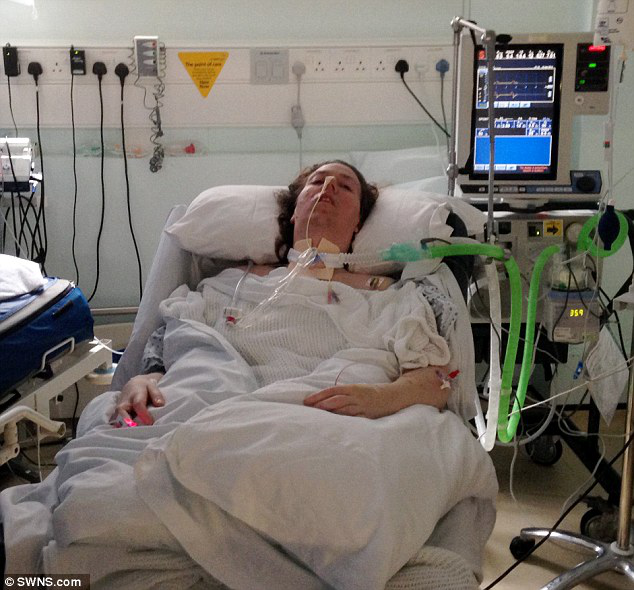
Paula has her father transferred in the Intensive Care due to a torn aorta. In the end, her father had undergone an emergency tracheostomy and open heart surgery, a growing concern is that her father is unable to come-off sedation due to behavioural changes during waking moments.
I think the ICU is keeping my father sedated for too long, how should I help him!?
Paula: Right.
Patrik: When was the last time when you felt your dad is acknowledging you, and your dad can see you, and your dad is basically aware of what’s going on? When was the last time you would say that was the case?
Paula: Well, we just had this big hurricane here, so we weren’t able to go to the hospital for the weekend, but I would feel Wednesday night. I could swear that when I was there, he was semi-awake and I was talking to him, and I could swear that he was kind of following my voice with his eyes. It could be in my imagination, but I swear he blew me a kiss.
Patrik: Okay. Good. Good.
Paula: It could have been my imagination.
Patrik: No, no, no, no. I don’t think … you should trust your gut and your intuition. You know your dad. You should trust all of that. You definitely should. You need to trust all of that. That’s your heart connection to your dad. That’s very important. You should never ignore that … never. That’s …
Paula: I know. That’s why I feel like there’s something else that they’re not telling us, they’re not doing, or … I mean they haven’t really told us anything. They’ve just been doing. That’s another thing. I was flipping out in the hospital last week when they said they want to move him. I’m like, “How can you move us? You haven’t even told us anything about his care, or his health, or what to expect, and you just want to slough him off on the next person.”
Recommended link and information:
Patrik: They know that waking up after an aortic rupture can be delayed, especially with increasing age. They know that. They’ve seen that before. Often, there are no time lines around this. Patients wake up in their own time.
What I don’t like is that they keep giving the propofol. I don’t like that at all. They should probably take the propofol off and introduce medications like maybe quetiapine, or Seroquel. I don’t know if you’ve heard of that. Or maybe-
Paula: That’s what I thought, too, something for his anxiety.
Patrik: Absolutely. Absolutely. That, or a little bit of diazepam or Valium, just a little bit. That could help. Get rid of that propofol. Get rid of that propofol as quickly as they can. Propofol has its time and its place, but not for long-term weaning.
That’s one thing. The next thing is, before they should be even considering LTAC (Long-Term Acute Care), any ICU is much better equipped, much better skilled, to wean patients off the ventilator, than any LTAC.
Recommended:
Paula: Right. I would think so, too.
Patrik: Absolutely. The whole idea about LTAC is long-term. Nobody wants to be on a ventilator long-term. That’s a whole lot of crap. That’s a whole lot of crap.
Paula: That’s what I think, too.
Patrik: Any ICU is much better equipped, and skilled, and experienced to wean patients off ventilators and tracheostomies. As long as your dad is sedated, he’s not going to LTAC (Long-Term Acute Care), so that’s not even on the cards for them. The other thing that’s important for you to know is, ICU beds are in high demand. If they think they can’t manage the weaning process off the ventilator in a time frame that’s convenient to them, they will try and send your dad off to LTAC.
So, your challenge at the moment is to direct his care, so he can have the best chance to get off the ventilator in this ICU, so he can avoid LTAC.
Recommended:
Paula: That’s what I thought, too. Me and my brothers, both say the same thing.
Patrik: Absolutely. You’re on the right track. You’re on the right track, okay?
Paula: Okay.
Patrik: The question is; how do you want to go about this? There’s a series of questions that you can ask, and you can definitely start with “Why is he still on the propofol? Why are they not dealing with his anxiety?” Maybe they do, and they just haven’t told you, but it doesn’t look to me like they do. Otherwise, they would be trying to stop the propofol. I’m very concerned that if … he had the tracheostomy on Friday did you say?
Paula: Yes. No, they did it last week, so it’s almost a week now.
Patrik: Okay. Let’s just say, for simplicity, it’s been a week, and he’s still on the propofol. That’s a big concern. That’s a big concern.
Paula: That’s how I feel. They’re giving him a diuretic now, too, because he’s kind of filling up with a little fluid, because he isn’t moving. That’s another reason why they say … you know this is all stuff that happens from sitting in that bed.
Patrik: It does, but if they are giving him a diuretic, there is still a chance that he might have mild kidney failure … mild.
Paula: It’s possible. He has one kidney.
Find more information about Dialysis:
Patrik: I tell you … an aortic rupture … I tell you two things that stand out to me. There’s two things that I’ve seen in front of me. I worked in ICU for nearly 20 years. There’s two things that stand out to me after emergency surgery for an aortic rupture. Number one, delay in waking up, especially with increasing age. That’s number one. That’s the first thing I see right in front of me.
The second thing I see is kidney failure. Those are the two things that stand out to me for somebody who has gone through that surgery. There are other things that stand out, too, but they’re more on the medical side … like with medications. We can talk about that later if you like. Those two things really stand out to me. I’ve seen it over and over again. Delay in waking up-
Paula: Now, if they did dialysis on his kidney, that would be too much trauma at this time, wouldn’t it?
Patrik: No, not necessarily. Not necessarily. If his kidneys are failing, he needs dialysis. That wouldn’t be a concern for me. That wouldn’t be a concern for me. That is what an ICU is doing. ICUs are very good at life support. Dialysis is life support. I’m not worried about that at all. That would be the least of my concerns. I’m way more concerned about how they’re managing the waking up process.
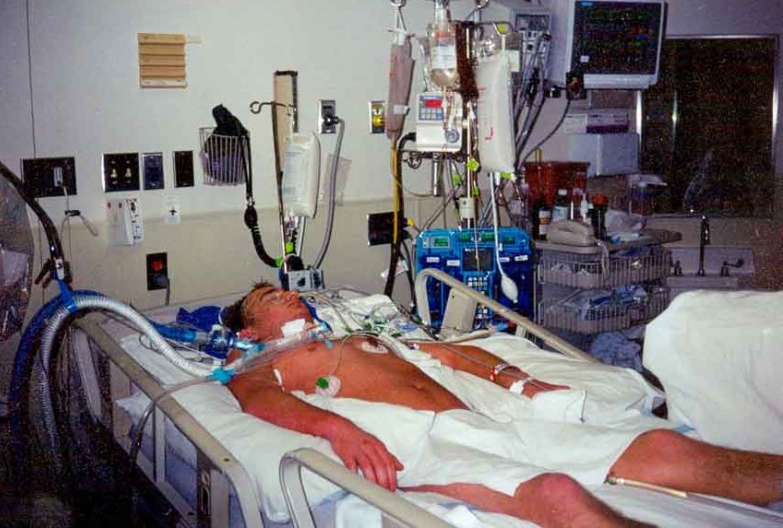
Paula: Since the beginning, they haven’t really, been really pushing him to wake up. They’re keeping him sedated. They keep saying, “He gets apprehensive.” I’ve been there when he’s been kind of not very sedated. He’s been asleep for how long, and they’re trying to wake him up. Then they say he gets apprehensive and his heart rate goes, and they put him back to sleep, they say.
I’ve never been there when they’ve totally woken him up. But, I’ve been there when he’s kind of been not so sedated. I don’t see that happening. Do you know what I mean? His heart rate is going, but like the nurse said, “Oh, he acknowledged … he hears you.” His blood pressure would be going, but nothing that’s out of hand.
Recommendations:
Patrik: Do you know whether he’s on any inotropes or vasopressors? Have you heard of those terms before?
Paula: No.
Patrik: No. That’s okay. Then we don’t worry about that. That’s okay. Do you know what ventilation settings he’s on? Do you know whether he’s breathing by himself, do you know whether he’s getting a lot of support from the ventilator? Do you know any of that?
Paula: I don’t know any of that.
Patrik: That’s okay. That’s okay. I tell you what I believe the steps forward could be for you.
Paula: Okay.
Patrik: I can definitely help you with that. It would be a matter of trying to find out what are they exactly doing? What medications is he on? How are they trying to manage the waking up process? But also, where is he at, in terms of ventilation, and guiding that if we can.
That includes me talking to doctors and nurses directly, if you want me to. If you want to set up a meeting with the doctors and you want me to be there, over the phone, I can do all of that.
If you don’t want that, there’s hundreds of questions on our website from people in similar situations. All the information is there for you, if you can spend the time on the website to look for that information. The shortcut is to talk to me directly, of course. Then I can guide you.
Recommended:
Paula: Can I ask one question? With his age and the one kidney, if we could properly get him to wake up, is there a way that he could survive?
Patrik: Oh, absolutely. Your dad will most likely survive. I’ll tell you why. I’ll tell you why. 90 to 94% of patients in Intensive Care leave Intensive Care alive. That’s about 6 to 10% mortality rate.
Paula: Right. Okay.
Patrik: Those are the statistics. It sounds to me like, irrespective of the challenges your dad is facing, it sounds to me like his heart is strong. If he hasn’t gone into kidney failure, those are all a good sign. Those are all good signs.
Paula: Right.
Recommended:
Patrik: The recovery process in Intensive Care is a lengthy one. It’s often a marathon. It’s not a sprint. If he survived with major blood loss, which he would have … he would have had major blood loss. He survived all of that. He’s only got one kidney and he hasn’t gone into kidney failure. That to me are all good signs. He’s acknowledged you last week. That’s a good sign.
It’s just a matter of moving things along. The challenge in Intensive Care often is, we all want to speed up the process. You, as a family, want to speed up the process of recovery. The ICU wants to speed up the process of recovery because they need the bed. All of that.
But the reality is, people will recover in their own time. It’s been a major, major surgery for your dad … major life event.
Paula: Oh yeah. And his age … he’s made it this far. The man is amazingly strong.
Patrik: Absolutely.
Paula: His surgeon couldn’t believe it. Even the pulmonologist told me, “Most people, especially your father’s age, they die on the table.”
Patrik: Absolutely.
Paula: They don’t make it that far.
Patrik: Correct. Correct. This is highly risky surgery your dad had … highly risky. From that perspective … because I’ve seen this before … he’s not doing too badly at all. But, he is facing some challenges, of course.
Paula: Of course, yeah.
Patrik: What I might do is, I might send you some information around if you wanted to engage me. You’re onto our free email newsletter. There’s good information there. As I said to you, all the information that you’re after. On our website there’s hundreds of articles … people in similar situations where we answer the questions.
Find more information:
Paula: Okay. Okay.
Patrik: I will send you some information around that and then we can talk again tomorrow
Paula: Okay. Alright. Perfect. Perfect.
Patrik: Does that help for now?
Paula: Yes, that helps a lot. I know a lot of this is tied to the healthcare and different things, but my dad is a strong man, and I know that he wouldn’t give up on himself or give up on us. I know that. I know that for sure.
Patrik: Right. That’s what you need to pay attention to. You need to pay attention to what would your dad want? Yeah. That’s what you need to pay attention to.
Paula: Okay. Perfect. Yeah. I’d love you to send me that information, and then I will definitely be talking to you again, and probably buy the package. Yes, definitely.
Patrik: Sure. Okay. Okay.
Paula: Perfect.
Patrik: Thank you very much. Have a good night.
Paula: Thank you, you too.
Patrik: Take care. Bye-bye.
Paula: Thank you.
Patrik: Your welcome. Bye-bye.
“Thank you very much for being a part of the previous series of 1:1 consulting and advocacy sessions. We hope you will find these new upcoming episodes informative and empowering.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!