Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer a question we get quite frequently from our readers here at INTENSIVECAREHOTLINE.COM and the question this week is
When to give TPN (Total parenteral nutrition) in Intensive Care?
Now first off, let’s clarify what TPN is and what it stands for.
TPN stands for Total parenteral nutrition and is in essence IV or intravenous nutrition in infusion form.
Now if your loved one is in Intensive Care and is ventilated and sedated in in induced coma, you may have already asked yourself how feeding or nutrition is taken care of.
The short answer to this question is that most of the time your critically ill loved one will have a nasogastric feeding tube (NG tube) in their nose and will get fed through it.
Or if your loved one isn’t on a ventilator and is awake in Intensive Care they may either
- Eat orally
- Get nutrition via a nasogastric tube (NG tube), I.e. if they can’t swallow. This is also known as enteral feeding
- Get IV/intravenous TPN if they can’t eat orally or if they can’t tolerate NG tube feeding
The preferred method of nutritional management in Intensive Care or critical care is always to let a Patient eat orally or to have NG feeds. It’s easy, it’s effective and the stomach gets some nutrition and is maintaining a healthy gut flora if the feeds are getting absorbed appropriately.
In some circumstances in Intensive Care your critically ill loved one will not be able to either tolerate or digest the nasogastric feeds via the nasogastric tube or will be unable to take food orally.
Those are the situations when TPN is required.
Indications for TPN are
- Malnourishment
- Loss of gastrointestinal function, I.e. the gastrointestinal tract cannot be accessed, is not functional because it is either obstructed, inflamed, fistulated or leaking, and your loved one cannot achieve adequate nutrition by oral or enteral means. Less commonly, where there is irreversible loss of alimentary function (e.g. short gut syndrome), TPN can be life saving and may be considered long term (including the delivery of home TPN)
- Peri-operative nutritional support. I.e. 7-10 days before surgery to improve post-surgery outcomes and recovery
- Patients with high risk of post-operative bowel obstruction (ileus)
- Pancreatitis and pancreatic fistula
- Palliative care situations, in order to maintain quality of life and/or quality of end of life
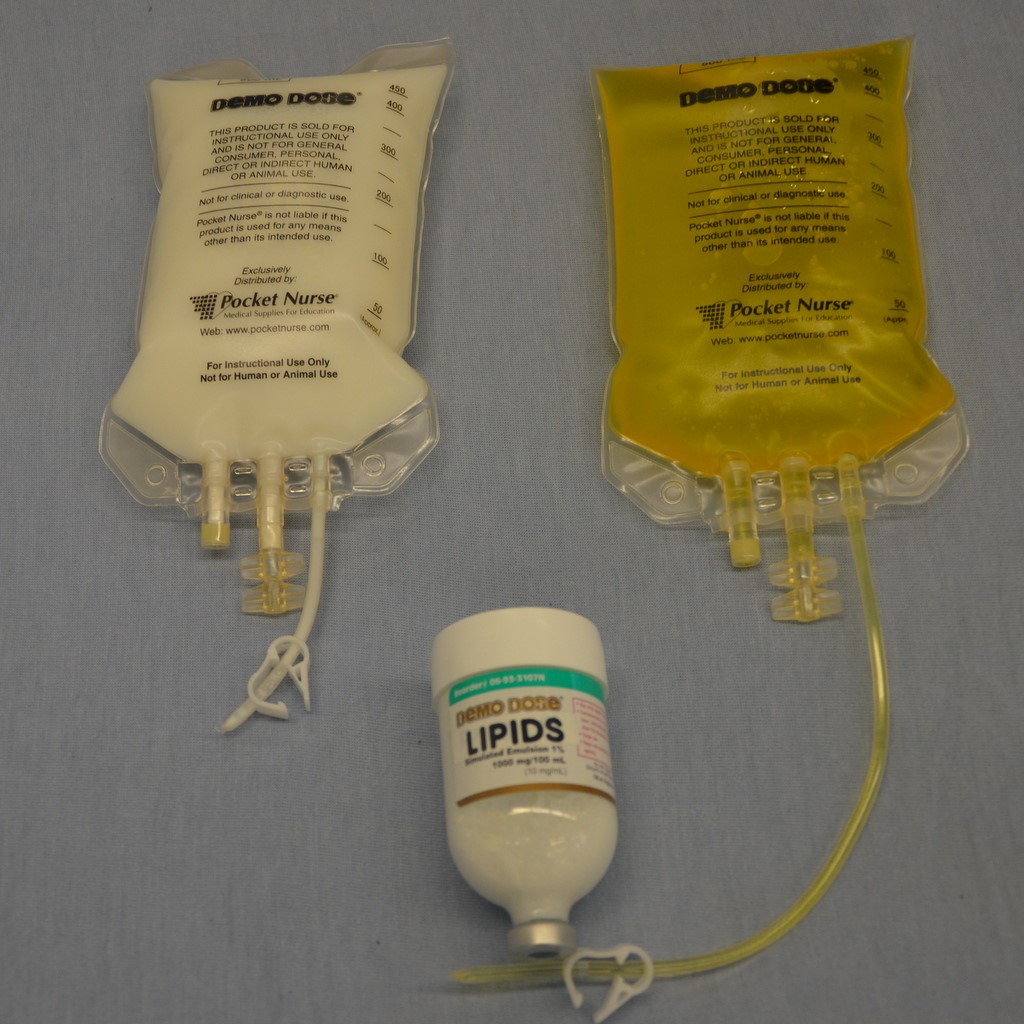
TPN (Total parenteral nutrition) can only be given via central venous line (CVC) or PICC line (PICC= peripherally inserted central catheter).
A central venous catheter or CVC poses an infection risk as the CVC needs to be changed every 7 days for infection control reasons.
Assessment for TPN (Total parenteral nutrition) should include an assessment of individual nutritional risks and requirements, including the risk of refeeding syndrome.
Given that Patients in Intensive Care/critical care can lose weight rapidly, adequate nutritional support needs to be administered.
It’s better to ask early in your loved one’s ICU admission how the Intensive Care team is managing your loved one’s nutrition.
Whilst your critically ill loved one is receiving TPN, regular checks of Blood glucose levels should take place, as well as regular blood checks and electrolyte checks, such as Sodium, Potassium, Phosphate, Magnesium and Calcium.
The advantages of TPN include easy access and accurate and speedy delivery whenever a central venous catheter (CVC) or PICC line is present.
Disadvantages are things like infection risk and potentially cost, as TPN can cost up to $500-$600 per day.
Historically speaking, enteral feeds such as PEG and nasogastric feeds as first line nutrition management for critically ill Patients are relatively new. Therefore, intravenous nutrition in the early days of critical care/Intensive Care was how Patients were fed.
This kept the stomach empty, which came with its own set of problems and complications, such as increased acid production due to the stomach flora including the stomach PH being out of balance and getting more acidity.
This imbalance of the PH has often led to stomach ulcers and therefore gastro-intestinal bleeding (I.e. GI bleed), also known as a “stomach bleed”.
Therefore, the shift has been to move from “IV nutrition” to enteral feeds such as Nasogastric (NG) feeds or PEG feeds to in essence “normalise” gut flora and not have an empty stomach and therefore also reduce the risk of stomach ulcers and reduce the risk of a GI or stomach bleed.
Therefore, since the shift from TPN to a more naturalised version of nutrition management in ICU such as Nasogastric and PEG feeds, the risk of ulcers and GI bleeds has also been reduced.
Therefore, survival rates have increased which is certainly a good thing!
Furthermore, stress levels in Intensive Care for critically ill Patients are pretty high, therefore the stomach naturally is producing more acid, again bringing the PH level out of balance and making the development of stomach/gastric ulcers and a “stomach bleed” more likely.
Again, enteral feeding is minimising this risk and is reducing acid production in the stomach, keeping the PH more neutral.
To summarise quickly. Enteral feeds such as nasogastric or PEG feeds for ventilated and sedated Patients in an induced coma should always be priority.
Oral intake for awake Patients is also a preference.
For any complications as I mentioned above TPN should be considered!
If you or your loved one need TPN at home, have a look at the link here.
TPN (Total Parenteral Nutrition) administration and PICC Line/ Central line Care in the community
Your friend
Patrik Hutzel
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!