Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM , where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can have peace of mind, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “your questions answered” and in last week’s episode I answered another question from our readers and the question last week was Part 3 of
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “your questions answered” I want to answer the next question from Heather, as part of her consulting sessions with me.
Previous questions(Part 1, Part 2 and Part3) from Heather you can find answered by clicking on the link here and here.
Today, Heather asks
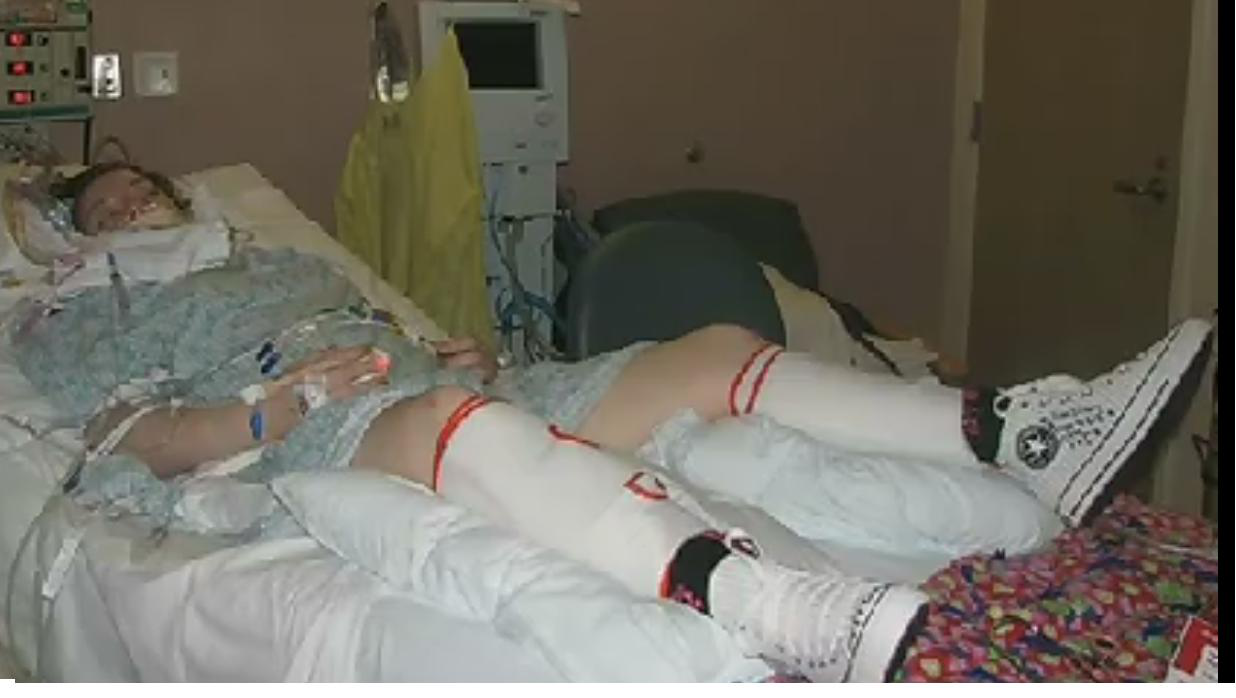
MY PARTNER IS IN INTENSIVE CARE ON A VENTILATOR! THE INTENSIVE CARE TEAM WANTS TO DO A TRACHEOSTOMY AND I WANT TO HAVE HIM EXTUBATED! WHAT DO I DO? (PART4)
Heather asks
Hi Patrik,
They extubated him again and then they had to re-intubate him.
They want to know if we wants a DNR(Do not resuscitate order) or to do the tracheostomy.
They say he will NEVER be able to have the tracheostomy removed or be out of the bed and they say that he will never be strong enough to cough up his secretions.
They say that my partner is too weak for physical therapy as he can’t move his lower extremities. That he will have no quality of life.
Unless they did something to him I know they are simply wrong.
He’s been in Intensive Care for about four weeks at this hospital.
In seven weeks since he’s been hospitalized he’s had physical therapy two times. Once while intubated and once the day after extubated him.
At no other times did they do or offer him Physiotherapy and I don’t know, but I think they are plain wrong about him not being strong enough. He has been here 4 weeks and they are ready to send him off.
Anyway his parents showed up today. They want to know if we want to do the tracheostomy or a DNR(Do not resuscitate order).
His Physiotherapist keeps saying that he is just to weak. He can’t respond with his lower extremities. They say they don’t think he’ll ever be strong enough to cough up his secretions and that he’ll have a poor quality of life.
They say he’ll be susceptible to more pneumonia. He has not been out of bed since December 5th.
They have done physical therapy with him three times that’s IF he really had physical therapy yesterday. That means he had it twice while intubated and once the day after they extubated him.
The doctor says they have more documentation than that and they are also a little more scientific than that. Though he didn’t offer up the scientific information.
Also why did they even try to extubate him earlier if they thought that he would NEVER be strong enough to maintain his airways. I think he is scared and I think he has anxiety.
I think until the sedation wears off and the meds get out of his system and until the Physiotherapy gets going they won’t know that. His dad is giving consent for the tracheostomy. Do you think he’ll never recover from this really?
Many thanks
Heather
Hi Heather,
I am again, very sorry to hear what you are currently experiencing.
I know that this must feel like a nightmare to you that will never end!
It’s typical that the Intensive Care team is quick in painting a negative and “doom and gloom” picture!
There is from what I can see absolutely no reason why he can’t have the Tracheostomy removed after it’s been inserted.
It’s also not overly surprising that the Intensive Care team is saying that your partner won’t have any “Quality of life” and I will explain more about “Quality of life” later and what it really means.
You need to, once again, dig really deep and ask yourself what the positioning of the Intensive Care team and more importantly, the positioning of your loved one’s diagnosis and prognosis by the Intensive Care team really means!
Does it mean that they are not prepared to try hard and give your partner the best care and treatment to get him the Tracheostomy and then go and wean him off the ventilator?
If they say so, they need to be very specific and explain to you in detail why they think that they can’t wean him off!
Recommended:
Do the Intensive Care team even have a limited mindset and don’t they believe that they can help your partner?
Also, why do they suggest a “DNR” (Do not resuscitate order)? Is it because they don’t want to invest the resources, including their emotional resources to “do whatever it takes” to get your partner out of Intensive Care alive?
Is it because they don’t view your partner as a “good business case” and they are worried that if your partner will be in ICU for a prolonged period that they won’t meet their budget targets?
Recommended:
Also, are they currently experiencing a high demand on their precious and ”in-demand” Intensive Care beds?
For example, if they have other Patients awaiting admission to Intensive Care that the Intensive Care team views as more interesting, more viable and if they perceive other Patients to be “in and out” of Intensive Care quicker, it tends to give them more revenue and short stay Patients are often more interesting to deal with from an Intensive Care team’s perspective, rather than dealing with a long-term ventilated Tracheostomy Patient, who has a Partner who is “difficult and demanding”!
Do not underestimate the Intensive Care team’s agenda, it often goes way beyond your critically ill loved one’s diagnosis and prognosis
Recommended
Next, as I have mentioned to you before, the Intensive Care team tends to have massive interests in medical research and if they think that there are other, “more interesting” Patients that they can enrol into a medical research study, which often attracts hundreds of thousands if not Millions of Dollars $$$ per year in funding, they want to focus on other Patients that they can enrol into a medical research study.
Related article:
Now, let’s look at “Quality of life”.
“Quality of life” is a term that is being overused by Intensive Care teams without them actually really knowing what “Quality of life” really means.
Let’s put things in perspective here.
Intensive Care teams are the expert in Intensive Care. They are the expert of saving people’s lives, curing them and get them out of Intensive Care in a better condition than they have been before they came to Intensive Care!
In some instances (around 6-10% of all ICU admissions) the Intensive Care team has the role to accompany a Patient when they are approaching their end of their life.
That’s what Intensive Care teams do. Again, Intensive Care teams are the experts in Intensive Care when it comes to critical illness.
They are not the experts when it comes to “Quality of life”.
Why do I say this? I say this, because as soon as a Patient has left Intensive Care, the Intensive Care team has absolutely no clue what’s happening with this Patient.
There is no follow up. They have absolutely no idea how a Patient and/or their families after Intensive Care experience “Quality of life”.
Whenever the Intensive Care team is referring to “Quality of life”, they are talking about their perception after a Patient has been discharged from Intensive Care. But they are talking about their perception of “Quality of life” and not reality!
Intensive Care teams are standing on this pedestal of “we know what’s best”, that’s been “granted” to them by society, by universities etc…
After all they are academics and scientists and they often miss the reality of life outside of Intensive Care!
Their view and perception about “Quality of life” outside of Intensive Care is blurred by their academic and scientific view and perceptions about life.
What are your thoughts and views about “Quality of life”? What are your partner’s thoughts and views about “Quality of life”?
What are your deeply held beliefs, cultural values, religious values/ beliefs, family traditions etc…?
The Intensive Care team always thinks it’s about them and their beliefs and values, but it’s not.
This is a very sacred time for you and your partner. You need to make up your own mind, you need to be strong and you can’t have anyone dictate you of what you want and what you believe in.
Related article:
Now, let’s look at the Physiotherapy or the lack thereof.
I can’t believe your loved one hasn’t been out of bed since 5th of December. That’s extremely poor care.
Especially since he has been extubated, he could have gone out of bed, there are no two ways about it.
After he’s had the tracheostomy, he should be able to get out of bed. Again, if they don’t get him out of bed they are making excuses. ICU’s where I worked in, we got Patients out of bed on a ventilator! There is no reason why you can’t do that.
Unless they have made serious attempts to get him out of bed, they can’t say that he won’t recover. Everything else is BS.
Also, as a side note, here in Australia as well as in European countries such as Germany, long-term ventilated Patients with Tracheostomy are able to go home if they can’t be weaned off the ventilator and continue their treatment at home. This is a win-win situation as it frees up expensive Intensive Care beds and it improves Quality of life and in some instances Quality of end of life. Check out www.intensivecareathome.com.au for more information.
You should also check out these articles here about DNR
Related articles:
Heather, to sum things up, it sounds to me like things are not working out currently, but I would imagine your partner is by far too young to be given up upon, since you have been referring to his parents.
Even though I don’t firmly believe in a Patient’s age as the main determinant for continuing treatment or not, it sounds to me like all avenues haven’t been explored and you shouldn’t buy into the “doom and gloom” and the negativity of the Intensive Care team.
Continue to be “difficult and demanding” and see where it leads you.
If you think your partner is suffering too much and best and full treatment and care isn’t leading anywhere, than you can re-evaluate.
Until then, get the tracheostomy done, get Physiotherapy going and see what happens. Be patient. Intensive Care is often two steps forward and one step back. Sometimes it can even be two steps forward and two steps back.
Take care.
Let me know what other questions you have and we can go on Skype or on the phone again or simply send another email.
Thank you& Kind Regards
Patrik
How can you have PEACE OF MIND, control, power and influence whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below! In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 “killer” tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Thank you for tuning into this week’s “YOUR QUESTIONS ANSWERED” and I’ll see you again in another update next week! Make sure you also check out our BLOG section for more tips and strategies or send me an email to [email protected] with your questions!
Also check out our Products section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 consulting!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
Related Articles