Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM , where we INSTANTLY improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, get PEACE OF MIND, real power, real control and so that you can influence decision making FAST, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question that our readers ask quite frequently and the question was
“How long can a critically ill Patient be on a ventilator with a Tracheostomy in Intensive Care?”
You can check out last week’s episode here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I answer another question that many of our readers want to know about, if their loved one is critically ill in Intensive Care and in this week I want to answer
”HOW LONG DOES IT TAKE TO WAKE UP AFTER AN INDUCED COMA?”
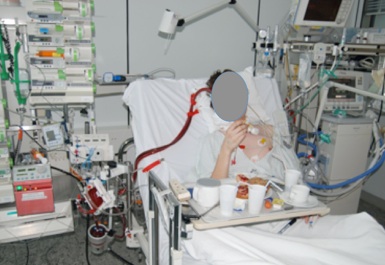
If your critically ill loved one has been admitted to Intensive Care and if your critically ill loved one is or has been in an induced coma, you have of course been wondering “How long does it take to wake up after an induced coma?”
It’s a great question to ask and after all it’s a question you would want to know the answer to, especially since you are feeling rather helpless in such a stressful, difficult, challenging and overwhelming situation such as having a loved one critically ill in Intensive Care!
Related articles/videos:
So let’s get to the meat of the question and let’s get to look at the answers.
If your critically ill loved one is or has been in an induced coma and has been ventilated with a breathing tube, it can be rather normal that your critically ill loved one isn’t waking up straight away. There sometimes can be a delay in waking up because of
- The amount of drugs given for sedation and opiates(pain medication such as Morphine and Fentanyl) whilst your critically ill loved one is in the induced coma in order to tolerate mechanical ventilation and the breathing tube. An induced coma is necessary for your loved one in order to tolerate mechanical ventilation and the breathing tube/endotracheal tube.
- The reason why your critically ill loved one has been in an induced coma; i.e. an induced coma for head or brain injuries is generally speaking more difficult to come out of, compared to an induced coma for “straight forward” surgery or for less acute and/or “softer” admissions into Intensive Care
- The length of the induced coma- generally speaking, the longer the induced coma the more likely it is to have a delay in “waking up”
- “waking up” is generally speaking a process and not an event that you can compare to switching on a light with a dimmer rather than switching on a light with a switch
- Your critically ill loved one’s age might be a factor, generally speaking, with increasing age, the higher the risk of going through a “delay” when “waking up” and coming out of the induced coma fully functioning
- Another risk factor is severe or heavy drug and alcohol abuse. If your critically ill loved one is using drugs and/or alcohol it’s more likely that when induced into a coma that a lot more sedative and opiate drugs are being used compared to a Patient who doesn’t use drugs and/or drinks alcohol. When “waking up” and coming out of the induced coma, your critically ill loved one has a higher chance of being confused and agitated, sometimes they may even be aggressive
Let’s break it even further down and look at time frames.
1. Your critically ill loved one is a “Straight forward” and/or “soft” admission to Intensive Care
If your critically ill loved one is a “straight forward” admission to Intensive Care after elective or planned surgery or is a “soft” admission to Intensive Care for a medical emergency on a ward etc… your critically ill loved one should come off the ventilator/ respirator and out of the induced coma relatively quickly within 12- 72 hours!
In those circumstances, your critically ill loved one should be on short acting sedatives, such as Propofol(Diprivan). Propofol(Diprivan) is a sedative that is widely used in Intensive Care to put Patients asleep and it is used as a short acting sedative, meaning that when switched off, your critically ill loved one should “wake up” relatively quickly sometimes within minutes or hours.
That can still mean that your critically ill loved one can be confused after the induced coma.
2. Your critically ill loved one has been in an induced coma and ventilated for 3- 7 days
If your critically ill loved one is a more complicated admission to Intensive Care and is more unstable, such as after a car accident or after major surgery where complications occurred or if your critically ill loved one sustained a head or brain injury or had a heart attack or cardiac arrest, then the breathing tube/endotracheal tube, the ventilator/ respirator and the induced coma might be required for more than 72 hours and if your loved one is stable and progressing, breathing up on the ventilator/ respirator with the support from the ventilator/ respirator being reduced, then again, your critically ill loved one should be able to come off the ventilator/ respirator after the sedation and the opiates(pain medication) have been removed and minimized.
By removing, weaning and minimizing the drugs that keep your critically ill loved one in the induced coma, your critically ill loved one should slowly but surely waking up. This at times can take time, because just as I have explained in number one, where your critically ill loved one may be sedated with short acting sedatives such as Propofol, the longer sedation for the induced coma is required, the more likely it is that a longer acting sedative such as Midazolam/Versed(Dormicum/Hypnovel)) is used. Midazolam/Versed is a Benzodiazepine and the longer a Benzodiazepine is used, the higher the risk and the likelihood that your critically ill loved one is getting addicted to it. Therefore, getting your critically ill loved one out of the induced coma, might have some challenges, such as withdrawal symptoms and therefore a gradual weaning off the Midazolam/Versed might delay “waking up”.
With Midazolam/Versed being a longer acting sedative, chances are that the longer the medication is being given, the longer it takes to “wake up” after an induced coma.
The same applies to the opiates(pain medication) that are given during an induced coma such as Morphine, Fentanyl or sometimes Ketamine. Those drugs can be addictive as well and just like with Midazolam/Versed, the longer your critically ill loved one has been receiving those drugs, the higher the chance to go through a withdrawal and also a “prolonged” waking up period.
Related:
-
The 5 Mistakes you are unconsciously making if your critically ill loved one is in an induced coma and is not “waking up”!
-
The 10 answers to the 10 most frequently asked questions when your loved one isn’t “waking up “ after an induced coma!
Again, coming out of the induced coma and off the ventilator/ respirator after more than 72 hours of ventilation and an induced coma might be a little bit more difficult, because as a rule of thumb, the longer ventilation and the induced coma is required, the higher the risk that complications and/or delays occur of course.
So, once again, if your critically ill loved one is stable, can open their eyes, can follow commands, is waking up and has shown strength to breathe by themselves there should be no reason that they can’t be taken off the ventilator after 3-7 days, generally speaking, even if your critically ill loved one is still a little confused, agitated and/or aggressive.
3. Induced coma and ventilated for more than 7 days
If your critically ill loved one has been in Intensive Care for more than one week now and has been in an induced coma and has been ventilated for more than one week by now, you’re probably wondering and you are more importantly worried when your loved one will finally come out of the induced coma and can come off the ventilator and the breathing tube/endotracheal tube.
Just like in number 2. the longer your critically ill loved one has been in an induced coma, the higher the risk of your critically ill loved one going
- Through a delay in “waking up”
- Through a phase of confusion, agitation and sometimes even aggression due to the side effects of the sedatives and opiates and due to possible or likely withdrawal from the sedatives and opiates
As a general rule of thumb, you need to be patient. Even if your critically ill loved one has finally come out of the induced coma, you might experience that your critically ill loved one is confused, agitated, drowsy or aggressive. And you’re probably shocked and maybe even embarrassed by what you see.
It’s OK. Know that it’s nothing unusual and it happens all the time in Intensive Care. Also know that many Patients can leave Intensive Care whilst they are still confused as long as they are stable.
What you also need to know is that most critically ill Patients don’t remember their time in Intensive Care, so don’t worry too much about the confusion and agitation if that’s what your critically ill loved one experiences.
Now, if after one week of ventilation and an induced coma the Intensive Care team still doesn’t feel confident to take out the breathing tube, they may suggest to insert a Tracheostomy. Before they actually suggest a Tracheostomy they should try and get your loved one out of the induced coma first and if your loved one is “waking up” and is cooperative and can breathe, the Intensive Care team should remove the breathing tube and give your critically ill loved one “a fair go” first to find out whether your loved one can breathe without a breathing tube and without the ventilator/ respirator.
If that fails, then the Intensive Care team would have a fair point to suggest a Tracheostomy, but once again that shouldn’t be brought up before or after at least 7-10 days of ventilation. And again it shouldn’t be done until the Intensive Care team is certain that there is no other alternative.
Other important issues to consider when your loved one is not “waking up” after an induced coma
- If for example liver function and kidney function is impaired it might take longer for sedation and opiates to be metabolised and excreted, hence “waking up” might take longer because the liver and the kidneys are not working at full capacity
- Sometimes even when sedatives such as Propfol(Diprivan) and/or Midazolam/Versed have been ceased, your loved one might still be on opiates(=pain killers) such as Morphine or Fentanyl for pain relief and the main side effect of opiates is respiratory depression, hence “waking up” can be delayed until Fentanyl or Morphine are ceased and out of the body system
- Also, another sedative that has been used in ICU in recent years is Precedex/ Dexmedetomidine. Precedex/ Dexmedetomidine is a substitute for commonly used sedation and opiates.Precedex among others, is an anxiety reducing, sedative, and pain medication. Dexmedetomidine is notable for its ability to provide sedation without risk of respiratory depression (unlike other commonly used sedatives such as propofol, fentanyl, and midazolam) and can provide cooperative or semi-arousable sedation.Similar to clonidine, it is an agonist of alpha2-adrenergic receptors in certain parts of the brain.
- Clonidine is sometimes also being used for light sedation, some pain management and also to manage withdrawal from mainly opioids like Morphine or Fentanyl
- A further delay in “waking up” after an induced coma can also occur when during the induced coma muscle relaxants(Paralysing agents) such as Rocuronium, Vecuronium, Cysatracurium etc… are given to manage extreme agitation, high Intracranial pressures or to facilitate mechanical ventilation in patients with acute lung injury (ALI) or acute respiratory distress syndrome (ARDS), and to prevent and treat shivering in patients undergoing therapeutic hypothermia
And if you still feel like you and your Family have little to no PEACE OF MIND, no power, control and influence and if you still feel like the Intensive Care team is keeping you at arm’s length, you need a quick in depth education that gives you PEACE OF MIND, control, power and influence!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
For more information regarding Tracheostomy, ventilation and induced coma check out our related Articles here
- The 5 things you need to know if your loved one is confused, agitated and delirious in Intensive Care
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?