Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have peace of mind, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
In the last week’s podcast interview I featured Penny from the UK with PART 1 of
You can check out last week’s interview by clicking on the link here.
In this week’s podcast interview we want to continue the conversation with Penny and you can listen to Part 2 of
My husband died on a hospital ward after a stay in Intensive Care! He should have been readmitted back to Intensive Care and the Hospital let him die without trying to save his life! (PART 2)
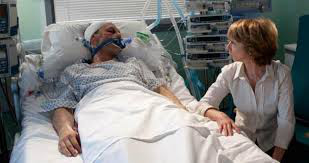
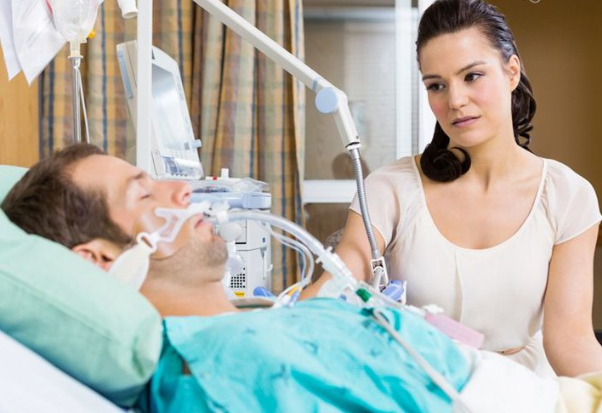
Penny has lost her 67 year old husband Terry last year after a stay in Intensive Care when he died on a Hospital ward when he should have been readmitted back to Intensive Care.
Penny’s husband Terry died in front of her very eyes without the hospital trying to save his life and without trying to resuscitate him!
Listen to Penny’s breathtaking story!
We split the interview into a two part series and you can listen to Part 2 today where Penny talks about her husband’s last few days before his death and Penny reveals the details in how the hospital has let her and her husband down, ultimately resulting in the death of her beloved husband!
Listen to the interview here
Penny: Hello?
Patrik: Hello, and welcome to the Intensive Care Hotline.com Podcast. Intensive Care Hotline.com helps families of critically ill patients in intensive care to instantly improve their lives so that they can make informed decision, get peace of mind, control, power, and influence, even if you’re not a doctor or nurse in intensive care. In today’s episode, I’ve got a very special guest. For the second time, I want to welcome Penny in the UK. Hi, Penny, how are you?
Penny: Hi, Patrik. I’m certainly fine, yes. Good to be back with you and your listeners!
Patrik: Yes, thank you so much for coming back for part two of the interview. Last week, we spoke about your husband’s premedical history, what led him to go into a care facility, and then we pretty much stopped where he was about to go in intensive care, so I told them we have to leave our listeners with a cliff-hanger to make it have a little bit of tension so they come back for the second episode which I’m sure they do. And we want to continue, basically, where we stopped last time, where your husband went into ICU.
Penny: That’s great, yes. I have some repeated scenario that has affected me and my acceptance of what was going on, and my judgement and my intuition, because the few months before when Terry actually did have the exact same type of grand mal seizures, and he went into intensive care in the same hospital. He was in two days given antibiotics but he was fine, he had good heart palpitations with hundred-and-twenty-something a minute on the monitor. And then he was moved up to the high dependency unit, treated well, into the ward for a few days, treated well, and then he went back to care.
Now, I assumed that that would be the same thing that happened last year, last April 27th, when I had the phone call they said it was a grand mal seizure and he’s back in intensive care. So, the difference between the year before was that the “Do Not Resuscitate” had been reversed, so he wanted to live. I went in to visit and saw him exactly the same as before, with the tubing, very well-nursed; can’t fault the way the doctors there and there’s one doctor-nurse to each patient, I’ve always been very impressed with the gadgetry and the monitoring, it’s incredible.
And this is a whole thing that– what I didn’t know was, and I’ll just remind you how I have power of attorney for Terry because he had problems with head injury in that site and the Co-Codamol given a lot of deterioration of his brain. On good days, it was brilliant and we had some really good chat, and on poor days he wasn’t making decisions, so I had the power of attorney.
That was in the record and that would happen in 2014, so, two years before, I had the power of attorney. And what I didn’t know was, that a consultant actually misdiagnosed him when he had the head injury, having some type of seizure and fell down the stairs. So he’d never had a seizure before. It was really the same…
Patrik: Yes, we talked about this last time, that he was misdiagnosed.
Penny: Well, it’s controlled, and it’s funny, you know, I’ve been a school teacher for 27 years, so, I used to try and see things from some another perspective, because when you’re teaching children, you have to do that. And what he actually did was see Terry in a very, very weakened state, you know, Patrik, you’ve seen seen so many in intensive care, and the very few I’ve seem.
It just pulls your heartstrings, and when it’s his training, I feel– and I haven’t contacted the guy yet because I’m going to wait and see what happens to the ombudsman and so on, but he thought he was helping Terry by tripling his anticonvulsant drug straight away without doing it gradually. I have not gotten to the bottom of that, I did ask during the meeting for this to be looked at and it wasn’t.
And in fact this consultant wasn’t invited to the meeting, and now, with Terry had a history of being extremely sensitive to chemicals. I remember saying last interview time that “one size does not fit all”. And, I mean, that was in his records, they knew that.
Patrik: I’ve really got to throw in there, Penny, that you say that one size does not fit all and I agree with that, the problem in hospitals and in intensive care as well is this “one size fits all” approach. So, they would have looked at your husband, and said “Oh, he’s got seizures. So, we’ve got this protocol for seizure management, and we will be giving him the same drugs that we give the next ten patients that have seizures, and the previous ten patients”, right? And that is this “one size fits all”, that is not necessarily appropriate for the individual.
Penny: No, certainly not at all. I’ve never met anyone so sensitive, really to only have organic food and so on. Anyway, I didn’t know this, so he went up to the high dependency unit, and that was when things started to take on a turn– all right let me just get back to intensive care, because I was very impressed when they gave him a feed through the nasogastric tube and he was only semiconscious, he didn’t like that then or the last time that he was in.
I think they did that two or three times in the high dependency unit, and he pulled the tube out– It can’t feel very good, can it? Think about it. But, as you know from your experience, which you told me quite a bit this morning having that little chat before we came on the recorded interview, that it’s important to get some food into the stomach to protect it because of the acid, and I really was pleased.
But then when I found out that there were some things, some ingredients in the liquid made by a company called Nutricia, which is global, so I’ve taken to do some more investigation, I was learning things, and I didn’t know they had sodium fluoride which I don’t think you’re too familiar with, Patrik, but perhaps some of your listeners might- well, it’s a gateway to do a lot of investigation, I can tell you.
So, sodium fluoride being adopted for supposed peace, you know, helping — it’s based on a lot of lies, but if it was calcium fluoride, a natural mineral from the Earth, I wouldn’t have had any problem at all, but I was very surprised at that ingredient as well as the salt, that is the sodium chloride again, which can cause side effects, which, again, there are many side effects from any of the drugs Terry in the past when he was more stressed, suffered from.
So, anyway, we went up to HDU and I was just visiting, I didn’t really feel– I think that’s quite important to stress, that I had to talk to the doctor when he came out of the high dependency unit and the intensive care, because obviously doctors are around a lot there, you know, again, very impressed with the whole setup. I was expecting the same to happen as last year, so when I went in to visit, I think it was just before he went up to the ward, I was so surprised after he was sit, literally, he sat up in bed for the first time. He was joking with his nurses– I must tell you this because it’s just– his sense of humor was amazing, we used to have many laughs.
One of the nurses came to his bed and knelt down and Terry looked down at her and said, “What are you doing?” and she said, “Oh, it’s all right, sir, just tidying up”, and he looked at her with a nudge that I was guarding them up, and we laughed. And that was, again, a false sense of security on my part. So, imagine how I felt when I went through it next time, and he was nearly sitting up, and he was clutching his stomach, groaning, moaning, calling out with pain. “What’s happening?” I’ve no idea, I go and fetch the nurse but they’re busy it’s a busy ward, very busy. She came over and, “Oh, we’ll give him some paracetamol.” And I was really really worried, now that I think is worth highlighting when I did look at the records in the ward note and obviously the report that came back from the trust after I’d written might about my concerns and this is very strange to see that the report of that and those symptoms very dreadful symptoms that Terry had this horrible pain was described as some discomfort and then serious stomach ache, there was two different types of descriptions which is strange, anyway —
Patrik: And that was let me just clarify the opinion that was in HDU?
Penny: Yes, just before he went in up to the ward.
Patrik: Okay and just to clarify for our America listeners or for our listeners in North America HDU stands for high dependency unit —
Penny: Competency yes.
Patrik: It’s mainly UK thing I think some ICUs in America have HDUs as well but it’s mainly a UK the step down from ICU that’s just for American.
Penny: Yes ready for patients going to a ward which ready for discharge which–
Patrik: Pretty much.
Penny: — and still so it would happen and in my way of thinking I knew how sensitive he and I thought I wonder he’s having a little reaction to the sodium fluoride in the feed it just crossed my mind so again I didn’t make a huge fuss but listen that knowing what I know now having done my research on me that was absolutely would take a lot of money on this but that’s when he starts to experience the gastrointestinal haemorrhage.
Patrik: Yes and I can honour really want to explain to our listeners very briefly that about 20 or 30 years ago in ICU most patients even get nutrition early on, they were giving intravenous nutrition rather than nasogastric feeds which is feeds into their stomach which is what’s happening nowadays because 20 or 30 years back by patients not having nasogastric feeds a lot of them were ending up with ulcers in their stomach and they end up bleeding and it’s the mortality patients dying was much higher than now. So but in your husband’s case it still didn’t stop him from bleeding?
Penny: Not really he was on a blood can you say that something else —
Patrik: I see.
Penny: — same for drugs but he was in the care home and then I stepped back and I didn’t have much input on that because I think I’m saying last time when he went in the care home he was aside- maybe this was going to be a way- actually make to go by having the drugs but he got used to them and they weren’t very high on dosage and I know one reason one’s an anticonvulsan, one’s a depressant, and I think also one went to stomach but then when I looked at the ward notes and records, he was on seven, and that’s paracetamol that’s not paracetamol, Keppra, ciprofloxacin.
Patrik: Ciprofloxacin yes.
Penny: — explaining to antibiotics knocks a poem I’m going to do. Now, Terry, that would be an absolute disaster I didn’t even know this and I didn’t think to inquire I was caught up with a lot of things happening at home here as well as those other things, my sister actually passed away two weeks before Terry so she wasn’t able to go to hospital she was very coping with all that as well and yes she was only two years older than me my sister but — yes life is good [chuckles]. And so when I thought taking a blood thinner how on earth will the bleeding stop it wouldn’t.
Patrik: I need to ask that question then so he was getting the blood thinner which is pretty much standard for any patient in ICU/HDU unless they have a bleeding condition but he didn’t have it up to this point so then my next question did they stop the Clexane saying when he started bleeding, do you know?
Penny: They never knew stomach was bleeding nobody ever knew not after days had passed which then I was witness to severe deterioration which started to really worry me and all that was written in the notes as so flat today and then no concern that this is what I really feel I’m highlighting its what on earth that these doctors and nurses what did they see , a lot of them agree and I like all of them I’ve liked everyone to be high suspicions of.
Patrik: And do you think that especially in an environment like HDU which is a step down from ICU where you still should have trained ICU nurses you would think that people would pick up on early signs you would hope that.
Penny: It wasn’t just that though Patrik it was the all day symptoms that Terry started to experience on what the mainland was so difficult following which again in the report they tried to make out that it happened in the community, difficulty swallowing, he never did have. So this is what so sad really when they’re desperate to protect themselves, “I’m not going for any suing,” if we have the remedies and that will come a bit later, so you’re telling lies, he never did. Now this difficulties in swallowing and that he wasn’t getting any more nutrition, and they didn’t do a peg — I didn’t even know what that was till I looked in the records after he’d died, Peg feeds what’s that? But they didn’t know that’s not being addressed as to why they didn’t do it and that was a few days into meal by mouth they kept trying to give him little swallowing tests, which didn’t work. And maybe I know of this drug set of four or five of the drugs used including stomach pain, bleeding in the stomach, I could go on —
Patrik: Why was he fed by mouth?
Penny: Because of his swallowing, yes that’s why it’s very soon you see after the tripling I think that was the tripling of that dose and diagnosis straight away instead of gradually was a trigger and things like he’s crying I went in the next day he was crying, he got diarrhea, he got a fewer but now I’m just lifting this often kept for adverse effects of that I’ve got in front of me they got eighty or a hundred listed. But I didn’t look out until on the Friday before he passed away when I knew something was seriously wrong and I thought I’ve got dig up some investigation here of my own all of these without printing out that something like crying diary see but which made then the doctors think that he’s got a infection which needed another antibiotic do you see that’s where the pure antibiotic you came in. Anti means against biotic life and the adverse effects and I said this in the meeting in front of their staff, their consultant what have you I said I have never read I hadn’t had been close to the most jaw-dropping appalling adverse effects from this what’s supposed to be helping again it’s a classic case of inversions isn’t it where there’s mental, political or mental depression, and heat, unusual drowsiness, vomiting, feeling sad or empty, mood or mental changes, this is actually one, bloating now that’s so tough to have the pain in the stomach. The following day I went in well then paracetamol, what painkiller had to help with the pain. His abdomen was nearly bloated and that was strange.
Patrik: And that’s something that the nurse should have picked up that is something that doctor or nurse should have picked up.
Penny: He was on the ward by this time Patrik we’ve gone up on the ward.
Patrik: So just to clarify so he had stomach pains in HDU he was still discharged to the ward without any investigation?
Penny: Yes knowing that of a need probably to check the dates and so on I’m not really good on numbers [chuckles] art teacher known to do a lot of English but maybe the pain that I witnessed it was really bad could have been just on the ward and let me check that is that okay?
Patrik: Very if you’ve got it here we’ve got to continue the conversation.
Penny: Yes, I’ll come back to you on that but she can put it anywhere besides and wherever doctors and nurses said they’re still just trying now I don’t see they’re trying to see adverse effects at all.
Patrik: Well that what they should be I’m really concerned about this.
Penny: This has been happening time and time and time again since 1990 and Terry had an operation between 1995 he had his gallbladder operation and there were problems there that they didn’t see. 1998, he had a mental breakdown after my daughter took her own life and the adverse effects of the antidepressant. Not one, two or three at a time, about a high 19 then, I’m going back quite a few years on there I did not know I had a computer before, I was still trying to work, you know, my living and nobody noticed and that was but the good thing about it, it prompted me to do my research. I have about 16 books, few of… just a couple of you know the titles and I learned a lot. My God did I learn and I hadn’t a clue about. When I saw in one or two of the antidepressant side effects could cause suicidal thoughts and seizures and on and even if, and I’m thinking, and I said in the meeting what is in these drugs something is wrong, because something is desperately wrong, so anyway–
Patrik: What happened on the ward? Once your husband was on the ward, what happened?
Penny: Right. On the ward yes, he — they put him in a side room more flatter he got, and the more sort of ill and in a really terrible state means one to five down his own room and still nil by mouth, nothing — I noticed he’s got a big white-coated tongue and they kept listing, when I was starting to take more interest and they told me I could come in outside visiting hours. That night I had a chat with the prescribing doctor because I was so upset about everything and he ended up not even having the strength to hold my hand, and he look terrible. and then I had a chat with- I said I’m worried about — he said I am have been looking over notes now, I said he is on a lot more drugs in him than before. I did not know then the caps had been tripled the dose. you know, trying to take in everything and it was just basically too full on, too much. He supported everything he was quite a nice guy and everything that he done and we had a long chat because I know a lot of background about the medical profession and he was a pleasant guy to talk to but he did — I said I got power of attorney and that was when he agreed to take off one of the antibiotics —
Patrik: right
Penny: -and one of them but that was a few days in now probably he can–
Patrik: In light of everything that happened at that point there was no consideration for your husband to go back into intensive care?
Penny: No.
Patrik: And why was that?
Penny: I do not know. Now that the question I’ll ask-
Patrik: That is the big question.
Penny: -I think actually– Can I just say if you have heard of the Liverpool care pathway?
Patrik: Oh yes.
Penny: Right. Well that apparently had been stopped a while back.
Patrik: Yes.
Penny: so looking at what actually happened, you know, I mean quite a lot of friends and so on and when I related the stories, sounds on that care pathway and that is what I said when i went in to pick up the death certificate took about two to three days after he passed away and I refused it because it have not got the- you know, what I thought he passed away of you know, something good reactions in it said pneumonia and now I said he sure this Liverpool care pathway? Oh no, he said. But they still seem to come and making- say making comfortable with me it was just absolutely not speaking flat out almost semi-conscious but then we saw- sorry.
Patrik: Given that he was so ill at that point in time and you you are now referring to the Liverpool pathway, people who are not- our listeners, people who are not familiar with a Liverpool care pathway basically end-of-life pathway that can been rolled out by the NHS in the UK a few years back but now they stop using it again. But I do know from other clients —
Penny: They tell us.
Patrik: They tell us, but it still being used. But coming along century also would suggest that if they use the Liverpool Care Pathway that they made your husband DNR do not resuscitate, have you got any any information around that what is your- what is your fear?
Penny: does, no. you know the actual Terry actually said on the day, he really did want he was concerning the DNR first. I wrote the letter there was not a DNR in place but i think they assume there was and that now, let me get bit which when I just lifted up the covers of Terry because obviously he was being nervous I was being nurse up. He was slack out he was not really with me and all I could see under the covers were black tarry excrement. I was absolutely got mad. I called the nurse quickly. What is– you know, and when I am looking at the drug adverse effects after all this happened, after he died and I went into it in a lot more detail black tarry stools but and then they started giving him drugs next– well let us go back to the black tarry I am looking at for sure I never understand before in my life. and I called the nurse, this is a Saturday before he died, he died on a Sunday. They passed clean him up, you know, I went up there, and clean him up and put out all the stuff. Do you see it was a weekend, have you heard about weekend problems in hospitals
Patrik: Staffing tends to be minimized on weekend for a number of reasons and other I mean that is not — nothing new to me having worked in IC for 20 years nothing is new to me and that’s not only — after hours and after hours
Penny: That is why there is a lot of deaths on weekends —
Penny: Well anyway, I had to ask, are you not going to do anything send something off for sample and all I got was sort of little blank looks. Nobody really you know, responded after I see it a lot but all I kept thinking of touch it what caused that. I didn’t know they had been average and then nothing. And when I run in the next morning, He is giving blow I said what is going on here I knew then that the sodium chloride caused swallowing difficulties in fever and I was upset about that because you have taken having a lot of intravenous saline which you think would be lethal old Kelsey salt is not and I knew that then and I just have to you know what’s really go through quite a lot of such as total poor alterian I just felt like I did not know what to do I want to help him but they were giving — all of them seems to give him blow
Patrik: Yes, It would have been. Yes.
Penny: Yes. I will answer it then. And then she bought the blood, you know, the bag empty bag when it cannot come out with the unit. Doc asked me to go out the room and tripped and see and she saw drips on the floor, blood, She left it. I had an apology from that but I cleared it up with two weeks from them
Patrik: And your husband, was he conscious at that point in time still?
Penny: Not really, but he — ah, now this is interesting but he had chronic ongoing one time notice that he had a white-coated tongue, this is all coming up towards the last few days. I was concerned and I had a tip-off from a friend who is a complementary health practitioner and he said, “That means it is a problem in his stomach, it is gastric problems.” I said, “Oh,” now all I did Patrik, I went and got a jar of manuka honey on the way to the hospital, I took it in and I took my own spring water, I cannot put tap water with chlorine and chemicals in it on the patient. I took my own spring water, I put a little bit of honey in the spring water. Now nothing on meal by mouth because of the swallowing, so I gave him a teaspoon of this honey and his mouth opened and he had it and the last words I heard him say to me was when I said, “How do you feel?” He said, “Terrible,” but then when he opened his mouth he said, before he opened his mouth, “Honey,” and that’s the last words I heard. Now, overnight his tongue went pink from giving him the honey. The staff, the nurse said when I saw, I went in early, I phoned at five in the morning to get them to stop these drugs. They still wouldn’t stop. You know, because that is all I thought was causing these side effects. I did not know about the haemorrhage. Really, even if the drugs would have been stopped, Patrik, I think at that stage I don’t think he could have been saved because the investigation I did on gastric intestinal haemorrhage can lead to respiratory distress and immobility, I didn’t know that.
Patrik: Oh absolutely, Penny, I am very conscious of time, what shall we do, we really want to continue, for now we really want to condense this so that people get to those, you know the moral of the story which I’m sure they get by now but we really got to sort of condensed this because we’re conscious of time and I’m surprised– I cannot believe that your husband that nobody send him back to ICU, I can’t believe that. With that with him conscious, with him getting blood transfusion, I can’t believe nobody send him back to ICU. I just can’t.
Penny: He was only 67 and nothing — was really an elderly patient and gentle lovely guy. But what happened right at the end when I went in the Sunday morning, Terry’s asleep, I had an appointment to see the on-call doctor I took a 16 –, no not quite. I’ve got 16 but until about six of my books, Your Drug May Be Your Problem, What Doctors Don’t Tell You, How to Survive Medical Treatment, good quality books. Something very good, well. I’ve got more positive and then I talk to his doctor for an hour, she would not budge with the drugs, she would not budge and I had to pack up and I felt so upset that I had to go out the hospital for an hour. When I came back Terry gone into into a spiritual distress their cordoning, I didn’t know that and I saw him till his last breath and do you know what they said? They couldn’t today — They’re standing around his bed, looking at him. Nobody’s got a knock on that door, no tube and you know what they said in the report and also in the meeting, “We let him die peacefully because we thought that any intervention would be more stressful”. I am not making this up.
Patrik: Well which is another indicator to me that they might have issued DNR do-not-resuscitate order without your or your husband’s consent. Have you found any evidence in the note of that?
Penny: No, I haven’t but I haven’t been back you see. What I what I need to do is go back to hospital because I’m — we’re talking quite a few months now. The actual NHS meeting was on the 14th of December and I was on my own, I couldn’t tell a friend that she wasn’t well and I’ve done a lot of research natural fat, and wrote down the agenda. I did the agenda they let me cover — apparently, the meeting’s good. Now, this is a good point and also the remedies I really want to try and get a remedies and how long have we got to go now–
Patrik: I’ve got another five minutes where we can go for —
Penny: Oh then, five minutes. This is what I’m confident now the agenda and I got here, please leave it all out, you’re essentially all that where email and six staff with funding from the NHS including the consultant — respiratory consultant but they did not invite any of the prescribing doctors. I didn’t have a say in that and I do because you’d probably get from talking to me or question things, because the informed consent Montgomery’s Law, that’s something. Let’s put that out, do have a look, this was about Montgomery’s Law it came in 2015. This patient consent even higher or their advocate, some quite evidence. Right, well I’ve got here pointed concern to be addressed: a) informed consent Montgomery’s Law, b) DNR cancellation. There was a report in, that the doctor that was the on-call doctor referred to me overturning it during our tour. She accused me of overturning that and I thought, totally untrue. C) my power of attorney comes in hospital records, d) safety of Terry’s prescribed drugs. I wanted confirmation they’re tested in combination and not only singly on a fit human and I wanted confirmation that the sudden increase was a safe and I didn’t get it, e) documented adverse reactions to drugs, f) presumed infections antibiotic side effects, g) severe stomach pain, abdominal bloating, pathologists report of haemorrhage and documented evidence of importance of the diagnosis and early treatment… the pathologist
Patrik: And I think there is one point that should be on that list as well from my perspective, just by looking to his story now in detail. The last point that should probably should be one of the first points even on this list should be why was he not readmitted back to intensive care and that is the big question to me that might prevented his passing.
Penny: Actual fact, they might have had no beds. They may have been absolutely full…bursting…
Patrik: They should have sent him somewhere else.
Penny: Yes, you’re right.
Patrik: I mean that’s not an excuse in a first-world country.
Penny: I’ll just write it on my own with all this, I didn’t really get any help and obviously leaving all the stuff that was putting no concern on his ward notes. What are they looking at? Anyway it goes on with nutrition, meal-by-mouthful and difficulties, incidences of Melena is it —
Patrik: Yes, Melena.
Penny: Yes, another concern. Then it went on and white-coated tongues, they just denied the gastric — the nurses in that says there was no knowledge that white-coated tongue had any link with those gastric problems. They didn’t know and in the final hours of Terry’s life, when I went to the nurse called me as I came back in hospital. “Quick, quick” she says. “He’s going.” I said “What?” and I saw a chest x-ray machine being wheeled out of his room and the spiritual consultant in the report said that was probably the doing of a doctor. The chest x-ray.
Patrik: Within that time that based on the chest x-ray they could have readmitted him back into intensive care.
Penny: They could have achieved them. Why didn’t they achieve them?
Patrik: So, you’ve got a lot of questions to ask to the NHS and I think the the moral of the story is — [crosstalk].
Penny: [crosstalk] — fob me off saying a lot of it was this helpful really on the heart and joy. I want to just try and find out where they’re coming from and I think it’s one, they’re very busy and two, the doctors are trained solidly to ignore adverse drug effects because I think in a way if they admit to that then that would allow medical negligence. Well, I mean it’s a minefield isn’t it, Patrik?
Patrik: It is a minefield but I believe medical negligence is a strong word but I think in this case, it’s at the right place. I mean if they’d let your husband die without escalating treatment if there is an no DNR in place then I believe, the term medical negligence is appropriate.
Penny: Well it’s like a scenario that you couldn’t make it up. I’ve never read anything like this. So the plans of remedies it’s very very — right at the end of the meeting they said that I could be involved in some of the meetings that they have the mobility major concern I’ve not heard anything.
Patrik: I hope they’re genuine.
Penny: Well, yes. This plans of remedies.
Patrik: Alright, Penny, I’m very conscious of time here. We’ve got to sort of summarize the hour two parts, very quickly.
Penny: Right. Very quickly. Hang on to your hat. One, Educating your medical staff including– that’s doctors and nurses about Montgomery’s Law and importance of informed consent plus checking for power of attorney and DNR cancellations with your patient’s medical —
Patrik: Yes. Very important.
Penny: Two, educating all staffed and recognizing documented AVIs, educating medical staff to the fact that that drugs are tested singly on fit humans and drug companies do not always publish accurate test results. Essential books are Bad Farmer by Dr. Ben Goldacre, Confessions of a Medical Heretic by Dr. Robert Mendelssohn that’s MD, Your Drug May Be Your Problem by Peter Breggin MD book, booklet on patients’ rights published by What Doctors Don’t Tell You. Quote from one of the books, “A drug that suppresses symptoms does not always cure the underlying problem and is able to cause more symptoms and the deterioration of the patient sometimes leading to death.” Four, give your medical staff information about the Oath of Geneva, especially as many medical herbalists have to take Hippocratic oath which states, “First, do no harm,” make plans to remedy the situation. Five, after adequate research insists on the replacement of refined denatured sodium chloride into their own solutions which has documented adverse effects of health on sea salt, six, insist that harmful sodium fluoride have to take another liquid food supplied by a nutritionist. Book, Fluoride Deception by Chris Brightly, an investigative journalist who published up at five years of sound research. There’s also aspartame that’s shown here, but that didn’t apply when Terry was in intensive care. Seven, educate and bring into practice to prescribing of good quality honey as a natural probiotic. Anti- means against the biotic life. This is the mission, that antibiotics have documented adverse affects that are life-threatening, also use honey to help gastric problems which were often linked to a white-coated tongue. eight, begin to practice true integrative medicine which has been advocated by Prince Charles in brackets the royal family takes herbal and homeopathic medicines and live healthily to a very old age. There is evidence that they have no toxic dentistry or vaccination, that’s it. Eight remedies. What are the chances [laughs] I can calculate.
Patrik: Look, Penny. I am very grateful for that you can say it, that you share your story with all of us. I mean it’s a very, very sad story but you’ve been kind enough to spend all this time on the interview and share your story. That’s not long along, really. It’s not even 12 months so thank you. You are probably, still going through the motions and I really appreciate you coming on and sharing this with our listeners and hopefully —
Penny: Thank you
Patrik: Thank you. Giving them an example for them. What to pay attention to, if they’re in a similar situation if they are concerned about treatment if they are concerned about how they ‘re dealt with. You know? If they have questions. No to wait, bring it out in the open. Do their research before it’s too late.
Penny: Absolutely. I think the thing is to get the informed consent and it’s a questioning with a friendly level. You know? Not to — It is difficult when you’re very worried obviously and I always tried to be as– I’ve said to doctors quite a few times look I know you’re doing the best you can with the skills you have. I said that there are certain– when apply to carrying things that are worrying but it was– when I started to get involved in that level. It was basically looking back and it’s too late. The only thing is that I have learnt an awful lot. Terry’s been my teacher and I really want this step not to be in vain. Did some good came from it.
Patrik: That’s fantastic. Penny —
Penny: You are doing a good job as well.
Patrik: Thank you. I think we are all trying to do our best to educate people. Penny thank you once again for coming on to this two part series. If you want to listen to the first part of the interview and you haven’t done that please go back. Is in our podcast series and Penny thank you once again. Now for out listeners check out intensivecarehotline.com Check out the, your questions answered section. Where we answer all of your questions. You can also get one-on-one counselling and consulting with me over the the phone, via email or via Skype. Check out that and if you have any questions. Just send out an email to [email protected] Penny once again thank you so much for sharing the story and we will speak soon.
Penny: Really, my pleasure and I’m hoping that some of these remedies were coming. I think you will inform partially?
Patrik: Pleased. That would be correct.
Speaker 1: Obviously, if the remedies come in. It will affect a family. So much harm is done with the best of intentions to help people buy this multi– it’s good polypharmacy. Iatrogenic illness is the second or third leading cause of death in the states. I don’t know what it is over here. It seems to be more dynamic. I want to talk basically, I’ve given them many meetings to make an illusion to the fact that lots have kickback firms from the drug companies. All they had to say was “Oh, just shut up.”
Patrik: I wouldn’t be surprised for that. We could go on for next two thousand to talk to you–
Penny: Yes I know. [laughs]
Patrik: Thank you so, much babe. Take care
Penny: Bye.
Patrik: Bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get PEACE OF MIND, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s PODCAST and I’ll see you again in another update next week!
Make sure you also check out our “YOUR QUESTIONS ANSWERED” section where I answer your questions or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling with me via Skype or over the phone and via email by clicking on the email and phone counselling tabs on the top of the website!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!