Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have peace of mind, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
In the last BLOG I talked about PART 1 of
The 9 myths of being a critically ill Patient in Intensive Care revealed! (PART 1)
You can check out last week’s BLOG by clicking on the link here.
In this week’s blog I want to share with you
The 9 myths of being a critically ill Patient in Intensive Care revealed! (PART 2)
- Myth#5- Visiting hours are limited in most Intensive Care Units and the staff usually try and send Family members outside when they do procedures or ‘hands-on’ nursing care, like washing or turning
Intensive Care Units have gone a long way in the last 10-15 years when it comes to visiting hours and the time allowed at the bedside of your critically ill loved one.
Whilst during the 1990’s there was still a restricted mindset or paradigm about visiting hours, it has changed in many units, where there are often no or very limited restrictions during the daytime.
And rightly so, in this day and age, the consumer should be the focus and Intensive Care Units should operate from a point of view that they have nothing to hide and they should operate from a customer service mindset.
This is a critical mindset to adopt, because your high expectations of care and treatment being provided, including having access to your critically ill loved one are very important!
You should expect and you deserve the best, period! Don’t lower your expectations because 99% of families of critically ill Patients in Intensive Care are intimidated by the Intensive Care team and therefore have low expectations!
In order to get what you want, you need to have high self esteem!
If you feel like you are not getting enough visiting time with your critically ill loved one, you should talk to the doctors and the nurses in ICU.
Don’t be afraid to speak up! Some doctors or nurses also don’t feel overly comfortable, having relatives at the bedside when they do the ward round or when they perform medical or nursing procedures.
If that’s the case, your alarm bells need to start ringing and you immediately need to start asking “does the Intensive Care team have anything to hide?”
Just by you asking this question to the doctors and the nurses will show them that you are not a push over and that you are not like 99% of the families of critically ill Patients in Intensive Care! It shows them that you are different and that you are not intimidated by their “perceived power” and their “perceived authority”.
Again, in this day and age, where transparency should be paramount, you should ask yourself of whether the Intensive Care team has anything to hide from you. Some doctors and nurses do feel comfortable having Family at the bedside, whenever they are performing tasks. In some Intensive Care Units, the nursing staff might even get the Family involved in the nursing care if the Family wants to engage in such activities.
In any case, should you feel like you are not getting enough time with your loved one, you should ask and you shouldn’t be hesitant to ask for more time if you feel like you aren’t getting any!
Furthermore, the more you engage with the Intensive Care team, the more insight you get about what is really happening!
Related article/video:
- Myth#6- Children are not allowed in ICU
Once again, everything is negotiable. If you feel like your child or your children should come to Intensive Care, to see your loved one and if you feel like your loved one wants to see their Children or grandchildren or nieces and nephews, you should go for it.
Of course you should check with the Intensive Care staff and if your child or your children don’t want to go, you shouldn’t force them. Furthermore, make sure that your child or your children are healthy as there are a fair number of unhealthy ‘bugs’ flying around in Intensive Care and if your child is in good health it shouldn’t be a problem for them to visit.
Most children tend to be very good and understanding when it comes to one of their loved ones being sick in Intensive Care! Children are smart and can often cope with changing circumstances!
The worst thing you can do is to withhold any information from your children and not tell them the truth.
Whilst you may want to go slow and at your children’s pace in revealing the truth about a significant family member being critically ill or even dying, I have seen over the years and after working with thousands of critically ill Patients and their families that not including your children in what’s happening with your critically ill loved one can have devastating consequences for your relationships and the trust you build with them long-term.
I have seen too many parents trying to hide the fact that their mother/father or grandparents were actually approaching their end of life in Intensive Care until they had no other choice but to tell them. This is not a good strategy and not a trust builder.
If you think your child can’t cope with the news, get professional help from a counsellor or consultant in how to breach the news.
Do not withhold any information from your children they are entitled to know and help them to cope with the situation.
You’ll be surprised how resilient they are and how they adapt to change.
If you brake bad news too late, your kids will most likely say something along the lines of “Mommy/Daddy why didn’t you tell me?”
You don’t want to come in such a position, ever!
It’s ok to be vulnerable with your children.
Here is a quick “real-world” example so you can understand what I’m talking about.
A while back I was looking after a 45 year old man who was dying after a cardiac arrest in Intensive Care. He had two young children, a 9 year old son and a 5 year old daughter.
Their mother and wife of the Patient told their children that their Dad was on a business trip for a few days and that he would be back soon. The wife very much was in denial of the situation and she thought her husband would survive and everything would be fine.
Nothing was further from the truth, her husband was in a real end of life situation.
Related article/video:
When she finally had no other choice but to break the news to her children that their father was dying, this traumatised the children as you can imagine.
Unfortunately this is not an isolated case and I have witnessed many similar situations where parents withheld and excluded their children from the truth.
No matter how difficult the situation, honesty is the best policy with your children!
- Myth#7- Doctors and nurses working in Intensive Care must be of higher status than I am and they must be “smart”
As you know, I have said this one before in some of my other reports if you have read them. So I admit that I am repeating myself here. Why do I keep repeating myself? I keep repeating myself because I want to help you and also because I see this behaviour in Intensive Care over and over again and it’s holding you and your Family back and it doesn’t give you what you want and what you need, which is making informed decisions, get peace of mind, control, power and influence!
The minute you think the people in Intensive Care, mainly the doctors and the nurses that you are dealing with, are of higher status or smarter than you are, you are giving away your power and you are handing over whatever level of control you thought you’ve had. You’ve just given it away, hand delivered on a silver platter!
It doesn’t matter where in life you have come from and where in life you are going to. Just because the people you are dealing with happen to be doctors and nurses in Intensive Care doesn’t make them smarter or of higher status.
It is your perception and your perception only, that puts them on a pedestal and it’s your perception that makes them look “smarter” in your eyes. It is not even real and you are harming yourself if you continue doing that.
I am not saying that you should be disrespectful towards doctors and nurses, but you certainly shouldn’t be thinking that they are smarter than you are or that they are of higher status than you are.
Read my “Instant Impact” report again and if you haven’t done so go and check it out here http://intensivecarehotline.com/instant-impact-report-2016/ , there is even more about this topic, but for now, just remember, do not put doctors and nurses on a pedestal and do not think that they are smarter than you are, because chances are that they are not.
Your positive mindset and you having high self esteem is critical. And it doesn’t even finish there. Your body language, your tone of voice and you staying composed and determined are all critical aspects if you want to make informed decisions, get peace of mind, control, power and influence!
Related article/video:
- Myth#8- Because my loved one is mechanically ventilated means that they are very unwell and it’s therefore likely that they will die
If I had a dollar for every enquiry we get along the lines of
“My loved one is in Intensive Care on a ventilator and in an induced coma, will he/she make it?”
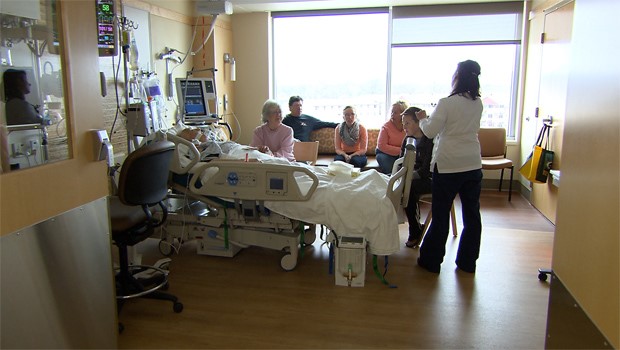
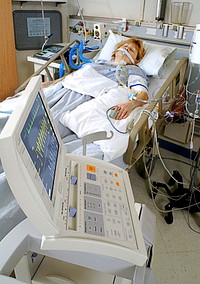
I know that when you walk into the Intensive Care Unit and you see your critically ill loved one for the first time, connected to a bedside monitor and connected to a ventilator you probably swallow. You don’t like the look of it. Your loved one looks very different to what they looked like before and you think to yourself
“what are the chances of my loved one surviving this?”.
As I pointed out in myth 1, the vast majority of Patients in Intensive Care are leaving Intensive Care alive!
Let me say that again because it’s so important to understand.
The vast majority of critically ill Patients in Intensive Care will survive their stay in ICU and leave Intensive Care alive!
But also, the answer to the question “what are the chances of my loved one surviving this?”, is not a black and white “yes” or “no” answer.
It all depends. There are so many variables and so many nuances when your loved one is critically ill in Intensive Care that it takes someone like me to look at the situation from many different ankles including knowing all the diagnostics, x-ray and blood results, medications your loved one is getting etc… in order to get to the most pressing answer of this question.
Recommended:
I know just by you looking at all the cables, wires and tubes everywhere, especially if your loved one is connected to a ventilator or respirator and the tube is coming out of your critically ill loved one’s nose or mouth. If your loved one is ventilated with a breathing tube, they are also on sedation and in an induced coma most likely. It’s usually not a very nice look or feel.
Related article/video:
A lot of relatives and Families panic, when they first see their critically ill loved one in this particular condition and they often associate ventilators, cables, equipment and tubes with serious life threatening issues for your critically ill loved one.
And that may well be the case, as in some instances your critically ill loved one may well be in a life threatening situation.
But for the majority of ventilated Patients in Intensive Care it is a short term measure and the average time of being ventilated is usually around 2 days or 48 hours. That means that on average a Patient doesn’t stay on a ventilator or on respirator for much longer than 48 hours. It is very often a short term measure post surgery or post admission to Intensive Care for loss of consciousness.
So, just because your critically ill loved one is currently on a ventilator or respiratory, the chances are that he or she will be off ventilation/ respiration very soon and therefore there is no need to think that just because your loved one is currently ventilated that he or she is about to die.
Once again, ask the doctors and the nurses and you will find that they will answer your questions regarding the ventilation of your loved one.
If you happen to be a Family member who has a critically ill loved one in Intensive Care who has been ventilated for more than 7 days and also has a Tracheostomy, things are different and we have more reports and blog posts about (long-term) ventilation with Tracheostomy. You’ll find links to resources to when to do a tracheostomy here
Also keep in mind that more and more countries have Intensive home care services available for long-term ventilated Adults& Children with Tracheostomy as a genuine alternative to a long-term stay in Intensive Care! Check out INTENSIVE CARE AT HOME for more information!
- Myth#9- The doctors and nurses have told me that I can’t stay overnight with my critically ill loved one in Intensive Care
As I have touched on in myth# 5, Intensive Care Units have become more tolerant in the last 10-15 years about their visiting times and their visiting hours.
After all, Intensive Care is not a prison.
The general consensus in most Intensive Care Units is that Family members shouldn’t be encouraged to stay overnight for a number of reasons. Please keep in mind that most Intensive Care Units are busy, noisy and stressful places that run 24hours a day, 7days a week, 365 days per year.
In order to maximise quiet times and rest periods for Patients, especially overnight, less visitors is usually a good thing to maintain those quiet periods.
There are however, periods where critically ill Patients in Intensive Care are in dire, difficult and unique circumstances such as
- They have been admitted to Intensive Care in the middle of the night
- They are extremely unstable and critical and the prognosis of their survival is poor and therefore it is unknown and uncertain whether the Patient is going to survive
- The Patient is approaching their end of life
Those are the three most common scenarios where Families of critically ill Patients are usually allowed and even encouraged to come and visit even overnight.
Furthermore, I have also seen Families staying overnight regardless of the rest and quiet period, just because they wanted to be with their loved one during times of crisis. Most hospitals usually do not encourage overnight stays, but at the end of the day, if you feel like you want to be there, you should make your wishes known and proceed accordingly.
I hope that you and your Family are on your way to making informed decisions, control, power and influence, whilst your loved one is critically ill in Intensive Care.
Your friend
Patrik Hutzel
How can you become the best advocate for your critically ill loved one, make informed decisions, get PEACE OF MIND, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s BLOG and I’ll see you again in another update next week!
Make sure you also check out our “YOUR QUESTIONS ANSWERED” section where I answer your questions or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling with me via Skype or over the phone and via email by clicking on the email and phone counselling tabs on the top of the website!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update