Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from intensivecarehotline.com with another quick tip and questions answered for families in intensive care.
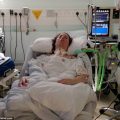
So Betty writes, my five-year-old granddaughter has a large VSD which stands for ventricular septal defect and pulmonary hypertension. She was admitted to ICU unresponsive after a seizure, she wasn’t breathing.
She was ventilated after heavy paralyzing sedation with Rocuronium, diagnosed with pneumonia, positive rhinovirus and UTI. After two weeks she had surgery for a tracheostomy and she’s now still sedated with Precedex, clonidine and Fentanyl.
They have tried weaning her off the ventilator several times in the past few days without success but he’s negative now for pneumonia and they are talking about moving her out of ICU slowly. They never resolve the seizure issues. She has an episode each time they reduce her sedative medications. She recently started on Valproic acid for the seizures.
My question is would she be able to come off the ventilator? How long is it safe to remain on the ventilator? Will this mean she must remain sedated? They are presently doing an EEG for the past 48 hours so far. They’re trying to rule out the seizure activities. She’s also fed with the PEG tube at a slower concentration rate. Any suggestions please. Thank you. From Betty.
Betty, I am very sorry to hear about your granddaughter. Let’s look at the issues in particular. So you’re asking if she can come off the ventilator. So there’s a number of issues there Betty as far as I can see. If she has a large VSD. They may have to close that VSD with surgery, she may need surgery for that because what basically happens in a VSD, deoxygenated blood moves over to the oxygenated side and is really decreasing oxygen levels in the blood that could be one issue why your granddaughter can’t come off the ventilator, but it may not be the only issue.
She has pulmonary hypertension and in order to treat pulmonary hypertension, she may also need to be started on medications like Sildenafil maybe a little bit of nitric oxide, maybe a Prostacyclin nebulizer or Epoprostenol nebulizer that could help with weaning off of the ventilator.
But I believe one of the biggest issues as well is that if your granddaughter has ongoing seizures and she’s still sedated with the Fentanyl and the clonidine and the Precedex because they can’t control the seizures that will potentially also keep her on the ventilator and the tracheostomy, I guess the combination of the seizures and the pulmonary hypertension and the VSD could potentially hinder your granddaughter to come off the ventilator, but it would also be important for you to share what ventilation settings she’s on and I can have a closer look and give you my estimation of how long she, how far away your granddaughter is from coming off the ventilator.
What needs to happen going forward I believe is a need to optimize anti-seizure medications. You talked about the Valproic acid, but maybe they need to add in some Keppra or some phenytoin as well to give her a good baseline so the seizures can be controlled. And then wean off the clonidine the Fentanyl and the Precedex. Also for seizure management often there are benzodiazepines in both to manage seizures at least in the acute onset such as Midazolam or diazepam, you haven’t actually mentioned that.
You’re also asking how long is it safe to remain on the ventilator. Look there are many adults and children that can be on a ventilator for a long time to come. In fact a lot of children, you know and adults as well live at home on ventilation with tracheostomy with services like intensive care at home and you can check out intensivecareathome.com for more information about those services.
So you’re asking does it mean that she must remain sedated. Now, the issue is Betty that your granddaughter probably will need to remain sedated until they got the seizures under control. And again, what I’m suggesting here is that they have to probably add-in, you know, you mentioned the valproic acid, but potentially some Keppra and some phenytoin as well to control the seizures and then it’s going to be a fine line between how sedated is your granddaughter with those anti-seizure meds and can they, on the one hand, control the seizures but on the other hand is your granddaughter awake enough to breathe by herself and then come off the ventilator.
So it’s a very fine line. Yeah. So the EEG that they’re doing might give you some answers you talking about the PEG feeds another issue that often happens with seizures and PEG feeds is your granddaughter might be at risk of vomiting and aspiration during a seizure. So that would be the last thing your granddaughter needs, an aspiration pneumonia because she’s vomiting, so maybe one way forward is to reduce the rate you already talking about a slower rate because of high concentration. Another option is potentially to have a fundoplication so that reflux can be prevented.
So I hope that answers your question for today. This is Patrik Hutzel from intensivecarehotline.com and If you have a question, please send me an email to [email protected] or simply call me on one of the numbers on the top of our website at intensivecarehotline.com, and I’ll talk to you in a few days.
Take care for now.