What is an Intravenous Catheter or IV cannula?
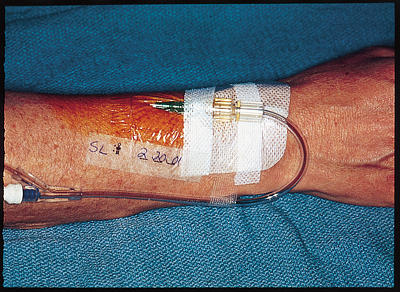
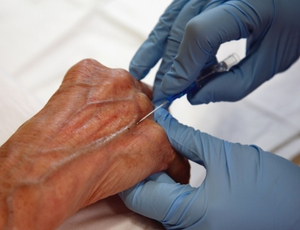
An Intravenous Catheter(IV cannula or peripheral venous catheter) is a catheter (small, flexible tube) placed into a peripheral vein(usually in a Patient’s arm or leg) in order to administer medication or fluids. Upon insertion, the line can be used to draw blood.
A tourniquet is applied to a Patient’s arm or leg so that the return blood flow of the veins is reduced and the veins are easier to see. The skin is cleaned with an antiseptic agent, the doctor is wearing sterile gloves and the catheter is then introduced into the vein by a needle (similar to blood drawing), which is subsequently removed while the small tube of the cannula remains in place. The catheter is then fixed by taping it to the Patient’s skin (unless there is allergy to adhesives). Newer catheters have been equipped with additional safety features to avoid needle stick injuries. Modern catheters consist of synthetic polymers such as teflon (hence the often used term ‘Venflon’ or ‘Cathlon’ for these venous catheters).
A peripheral venous catheter is the most commonly used vascular access in medicine. It is given to most emergency room and surgical patients, and before some radiological imaging techniques using radiocontrast, for example. In the United States, more than 25 million patients get a peripheral venous line each year.
A peripheral venous catheter is usually placed in a vein on the hand or arm. It should be distinguished from a central venous catheter(Central Venous Lines) which is inserted in a central vein (usually in the internal jugular vein of the neck or the subclavian vein of the chest), or an Arterial Catheter which can be placed in a peripheral as well as a central artery. In children, a local anaesthetic gel (such as lidocaine) is applied to the insertion site to facilitate placement.
Why is it done?
In Intensive Care, he purpose of IV cannulation is to give your loved one fluids and/or medication. Directly administering fluids and medications into the vein, means that your loved one will receive the effects of the treatment much more quickly than by any other route. Your loved one may also need a cannula in case of an emergency.
Does it hurt?
The only pain endured is generally at insertion point of the needle for a brief period.
Care of
- The sterile dressing should be kept clean and dry and therefore must be covered when showering or bathing
- The cannula should be changed every three days and most hospitals have a policy regarding how often the cannula should be changed
What are the risks?
Infection, phlebitis(inflammation of a vein), extravasation(leaking fluids into the tissues) leading to infiltration, air embolism(air bubbles), hemorrhage (bleeding) and formation of a hematoma (bruise) may occur.
Because of the risk of insertion-site infection recommendations are that the catheter needs to be replaced every 72 hours.
Any questions?
If you have any more questions about catheterisation, you can ask one of the many doctors and nurses looking after your friend or relative.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related articles:
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- Be more selfish if your loved one is critically ill in Intensive Care
- How to stay positive if your loved one is critically ill in Intensive Care
- 4 ways on how to be more persuasive if your loved one is critically ill in Intensive Care
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


