What is an Epidural Catheter?
An Epidural Catheter is a thin plastic catheter that is inserted into the epidural space(space inside the bony spinal canal but just outside the dura mater). The epidural route is frequently employed by anesthetists to administer diagnostic (e.g. radio-contrast agents) and therapeutic (e.g. steroids) chemical substances, as well as certain analgesic(pain relief) and local anaesthetic agents to alleviate pain. Epidural techniques frequently involve injection of drugs through a catheter placed into the epidural space. The injection can result in a loss of sensation—including the sensation of pain—by blocking the transmission of signals through nerves in or near the spinal cord.Therefore, lumbar epidural injections carry a low risk of injuring the spinal cord. Insertion of an epidural needle involves threading a needle between the bones, through the ligaments and into the epidural potential space taking great care to avoid puncturing the layer immediately below containing CSF.

When is it used?
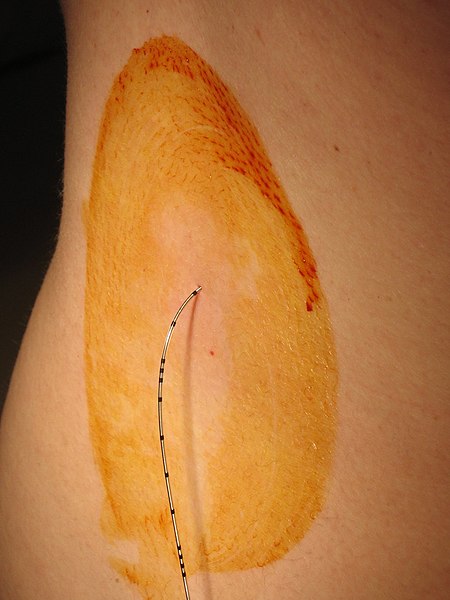
Injecting medication into the epidural space is primarily performed for analgesia(pain relief). When a catheter is placed into the epidural space(see image below) a continuous infusion can be maintained for several days, if needed. Epidural analgesia(pain relief) may be used:
- For analgesia alone, where surgery is not contemplated. An epidural injection or infusion for pain relief (e.g. in childbirth, rib fractures, back fractures) is less likely to cause loss of muscle power, but is not usually sufficient for major surgery
- As an adjunct to general anaesthesia. The anaesthetist may use epidural analgesia(pain relief) in addition to general anaesthesia. This may reduce the subject’s requirement for opioid analgesics such as Morphine or Fentanyl. This is suitable for a wide variety of surgery, for example gynaecological surgery (e.g. hysterectomy), orthopaedic surgery (e.g. hip replacement), general surgery (e.g. laparotomy) and vascular surgery (e.g. open Abdominal Aortic Aneurysm repair).
- As a sole technique for surgical anaesthesia. In Intensive Care Lung Transplantation may have an Epidural Catheter for pain relief. Some operations, most frequently Cesarean section, may be performed using an epidural anaesthetic as the sole technique. Typically the subject would remain awake during the operation. The dose required for anaesthesia(sedation) is much higher than that required for analgesia(pain relief).
- For post-operative analgesia(pain relief), after an operation where the epidural technique was used as either the sole anaesthetic, or was used in combination with general anaesthesia. Analgesics(pain relief) are given into the epidural space for a few days after surgery, provided a catheter has been inserted. Through the use of a patient-controlled epidural analgesia (PCA) infusion pump, a person has the ability to give himself an occasional dose of pain medication(i.e. Morphine, Fentanyl, Oxycodone or Pethidine) through an epidural catheter.
- For the treatment of back pain. Injection of analgesics(pain relief) and steroids into the epidural space may improve some forms of back pain.
- For the treatment of chronic pain or palliation of symptoms in terminal care, usually in the short- or medium-term.
The epidural is easily removed by the nurse when it is no longer required.
When is it not used?
There are circumstances where the risks of an epidural injection are higher than usual. These circumstances include:
- Anatomical abnormalities, such as spina bifida or scoliosis
- Previous spinal surgery (where scar tissue may hamper the spread of medication, or may cause an acquired tethered spinal cord)
- Certain problems of the central nervous system, including multiple sclerosis or syringomyelia
- Certain heart-valve problems (such as aortic stenosis, where the vasodilation induced by the anaesthetic may impair blood supply to the thickened heart muscle.)
- Bleeding disorder (coagulopathy) or anticoagulant medication (e.g. warfarin) – risk of spinal cord-compressing hematoma
- Infection near the point of intended insertion
- Infection in the bloodstream which may “seed” via the catheter into the central nervous system
- Uncorrected hypovolemia (low circulating blood volume)
- Allergy to the anaesthetic
Are There Any Complications?
- failure to achieve analgesia or anaesthesia occurs in about 5% of cases, while another 15% experience only partial analgesia or anaesthesia
- Accidental dural puncture with headache (common, about 1 in 100 insertions). The epidural space in the adult lumbar spine is only 3-5mm deep, which means it is comparatively easy to cross it and accidentally puncture the dura (and arachnoid) with the needle. This may cause cerebrospinal fluid (CSF) to leak out into the epidural space, which may in turn cause a post dural puncture headache (PDPH). This can be severe and last several days, and in some rare cases weeks or months
- Blood in the Epidural catheter. It is easy to injure an epidural vein with the needle. In people who have normal blood clotting, it is extremely rare (e.g. 1 in 100,000) for problems to develop. However, people who have a coagulopathy may be at risk of epidural bleeding or bruise
- Catheter misplaced into a vein (uncommon, less than 1 in 300). Occasionally the catheter may be misplaced into an epidural vein, which results in all the anaesthetic being injected intravenously, where it can cause seizures or cardiac arrest
- Catheter misplaced into the subarachnoid space (rare, less than 1 in 1000). If the catheter is accidentally misplaced into the subarachnoid space (e.g. after an unrecognised accidental dural puncture), normally cerebrospinal fluid can be freely aspirated from the catheter (which would usually prompt the anaesthetist to withdraw the catheter and re-site it elsewhere). If, however, this is not recognised, large doses of anaesthetic may be delivered directly into the cerebrospinal fluid. This may result in a high block, or, more rarely, a total spinal, where anaesthetic is delivered directly to the brain stem, causing unconsciousness and sometimes seizures
- Epidural abscess formation (very rare, about 1 in 145,000). Infection risk increases with the duration catheters are left in place, although infection was still uncommon after an average of 3 to 5 days’ duration
- Paraplegia (1 in 250,000)
- Death (extremely rare, less than 1 in 100,000)
Any Further Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation.It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related Articles:
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


